Abstract
This study investigates factors contributing to teenage pregnancy in South Africa and their impact on maternal mortality. Twenty participants were purposively sampled for one-on-one interviews using a mixed-methods and descriptive study design. SPSS software analysed the data, revealing reduced risk factors through educational policies. Teenage mortality rates from pregnancy and maternal health issues are lower than the rates in adults, with high blood pressure, abortion and injuries being the leading causes of adolescent death. The study emphasises a significant public health concern in South Africa, influencing women’s life expectancy due to socioeconomic barriers and insufficient awareness of danger signs, urging prioritised policies and programmes.
Introduction
Maternal deaths are an indicator of maternal health around the world. As part of the Millennium Development Goals, it is an important health indicator that must be addressed (World Health Organization, 2010). According to the Millennium Development Goals, Number 5, the maternal mortality ratio worldwide should be reduced by three quarters between 1990 and 2015 (World Health Organization, 2015). The World Health Organization (2015) reported similar findings that women in sub-Saharan Africa have a 1 in 16 chance of dying in pregnancy or childbirth.
According to the World Health Organization (2010), there were approximately 358,000 maternal deaths worldwide in 2008, with 57% occurring in sub-Saharan Africa and 99% occurring in developing countries. The maternal mortality ratio for sub-Saharan Africa is estimated to be 640 deaths per 100,000 live births, which is 40 times the maternal mortality ratio for 16 deaths per 100,000 live births in Europe and 28 times the maternal mortality ratio for 23 deaths per 100,000 live births in North America (World Health Organization, 2010). In sub-Saharan Africa, Guinea-Bissau and Chad have maternal mortality ratios of 1000 and 1200 per 100,000 live births, respectively (World Health Organization, 2010). There was also a high maternal mortality ratio in Southern Africa, including Angola and Tanzania, with 610 and 790 deaths per 100,000 live births, respectively (World Health Organization, 2010). It was the highest rate of mortality recorded in South Africa, with 176 for every 100,000 live births and 430 for every 100,000 live births, respectively (Burton et al., 2015).
The South African Government offers a confidential investigation system for maternal deaths, one of the few in the world (Gebhardt et al., 2015). The National Committee on Confidential Enquiries into Maternal Deaths (NCCEMD, 2009) defines the system as ‘a systematic multidisciplinary anonymous investigation of all or a representative sample of maternal deaths occurring in a region, area or national level to identify the number, causes, preventable or remediable factors associated with them’ (Moodley et al., 2014). In South Africa, maternal deaths were reported to the NCCEMD for the country as well as for its provinces (Moodley et al., 2014; NCCEMD, 2009). It is evident from NCCEMD reports that maternal deaths differ from province to province in the country (Moodley et al., 2014; NCCEMD, 2009). Health districts and care levels in provinces may differ in terms of the causes of maternal deaths and the avoidable factors.
The South African Government, like any other developing country, joined the international development goal of reducing maternal mortality, which was adopted by the United Nations and South Africa as member states at the Millennium Summit in 2014. A woman dies every minute from complications related to pregnancy and childbirth somewhere in the world. It is undeniable that over half a million women die from the same mysterious circumstances every year, meaning 1600 women die somewhere every day (World Health Organization, 2023).
Especially in developing countries, abortion is a major health issue among young females. Woldesenbet et al. (2021) report that 75% of unplanned pregnancies occur in sub-Saharan Africa, along with 25% of unsafe abortions. Almost all the 43.8 million induced abortions performed in 2008 occurred in developing countries, with 41% occurring among women between 15 and 24 years of age (Statistics South Africa, 2016).
Physical complications resulting from unsafe abortions are well documented. Physical complications are more likely to occur in younger women, which can have a serious effect on their health (Girgis et al., 2013). The consequences of safe abortion are detrimental to the individual as well as to the healthcare system as a whole, with complications consuming considerable resources (Frederico et al., 2018).
Various factors can influence the decision to terminate a pregnancy (Alhassan et al., 2016). Several factors determine individual risks, such as marital status, economic independence, rape history and so on (Gbagbo et al., 2015). A partner’s and parents’ support are one of the interpersonal factors (Jaffee et al., 2013). Premarital norms, social determinants, premarital stigma, extramarital sex and religion all play a role (Kabiru et al., 2016).
Women’s health has received considerable attention over the past two decades, particularly the mortality rate among women of reproductive age (Lehohla, 2013). Women of reproductive age are particularly susceptible to the dangers of unplanned pregnancies (Lehohla, 2013). The World Health Organization (2014) estimates that 22 million unsafe abortions are performed globally each year, most of them in developing countries. The number of women hospitalised each year because of unsafe abortions is estimated at 5 million (World Health Organization, 2014). The World Health Organization (2014) reports that 13% of all maternal deaths are caused by unsafe abortions in Africa, with more than two thirds of those deaths occurring there (World Health Organization, 2014). A major part of the Millennium Development Goals is to promote maternal health; therefore, women’s health cannot be ignored.
In South Africa, teenage pregnancy is seen as a social problem with implications for the development and empowerment of women (Macleod, 2014). According to Kaphagawani and Kalipeni (2017), teenage pregnancy is not merely a matter of reproductive health and young women’s bodies but is also linked to the gendered social environment in which teenage girls live. Teenage girls in South Africa are less likely to finish high school if they become pregnant, which seems to be one of the major obstacles to their educational development (Nkosi and Pretorius, 2019). Only about a 30 of teenage girls in South Africa re-enter school after pregnancy despite progressive legislation allowing them to do so (Modisaotsile, 2012).
Ethical considerations
The research emphasises the importance of upholding ethical standards, particularly in the dissemination of data and the protection of individuals’ dignity. De Vos et al. (2011) define ethics as a system of moral principles guiding behaviour towards experimental subjects, sponsors, employers, researchers, assistants and students. Ethical procedures, including the submission of the proposal form, ethical clearance application form, consent form and interview guide to the University of the Western Cape Ethics Committee, were followed up in this study involving 20 adolescents. The informed consent form provided a clear description of the study’s purpose, ensuring participants’ comprehensive understanding. Participants had the freedom to choose to participate or withdraw at any time, with no harm or advantages resulting from participation. Anonymity and confidentiality were prioritised, with participants’ identities kept private. Only the researcher and participants had access to the information. The study, approved by the ethics committee, assured participants that their data would be used for a report, and they could request access at any time. Publication plans were disclosed, along with contact information for further inquiries.
Data and methods
The maternal mortality rate represents the number of women who die while pregnant within 42 days of termination of their pregnancy. In addition to being an important indicator of the functioning of the health system, maternal mortality is a significant public health problem globally. There is a high maternal mortality rate in South Africa, as in any other country. In health facilities, pregnancy and childbirth are the most common causes of death. During the postpartum period, most women in public hospitals and clinics are discharged about 6 hours after delivery. Consequently, most problems are not detected, so complications like thromboembolism or sepsis cannot be detected. Maternal mortality factors were studied to develop relevant policies and programmes.
The study was conducted in Johannesburg, South Africa (2023), where teenage pregnancies are high and young females generally have higher odds of mortality. To conduct a study, a sample is selected from a group of people, behaviours, events or other elements (Burns and Grove, 2010). Random or non-random sampling can be used. Purposive sampling was used in this study. Researchers use purposive sampling as a non-probability method of selecting cases based on their judgement about information-rich participants based on their firsthand knowledge and ability to describe their experiences, challenges and coping strategies in a given situation. According to Creswell (2013), qualitative research aims at developing an in-depth understanding of the phenomenon of interest, not to generalise to a population. To gain in-depth, rich information about the phenomenon of interest under investigation, a non-random sample of 20 young females who met the criteria were selected to participate in the study.
In this study, in-depth interviews were conducted with a purposively selected sample of potential participants based on the inclusion criteria, and SPSS software was used to analyse data. The data analysis utilised the SPSS Version 23.0 computer programme, with descriptive statistics presented through frequencies and percentages for data representation. A comprehensive discussion of the topic was provided. As a result, the researcher was able to ensure that the gathered data supported the provision of thick descriptions. As a former maternity care worker, the researcher bracketed his personal experiences with the topic and avoided expressing personal prejudices or thoughts about it.
Self-administered structured questionnaires were used to collect data from 20 October 2022 until 09 December 2022. Participants in the study were recruited from a health facility after the researcher had explained the purpose of the study to them. Prior to consenting to participate, the women were given detailed information about the study in English. When completing the questionnaire, participants were required to provide both verbal and written consent. The researcher invited each participant who was capable of reading and writing well into a private room so that they could complete the questionnaire. The researcher set aside an already prepared private room for participants to fill out their self-administered questionnaire. In the afternoon, data were collected. To analyse and interpret the findings, the researcher used frequency tables and graphs.
The researcher conducted interviews with participants per interview guide to test the feasibility of the data instruments. It was a way of determining if participants understood the questions. Therefore, the participants correctly answered all questions. Self-administered questionnaires were answered with understanding by all participants, indicating that the data collection instruments were feasible. With the prepared questions in hand, the authors resumed the research.
English was the language used in the questionnaire. For those who could not understand, the questionnaire included questions formulated in the native languages of the researcher, who is proficient in four languages: Xitsonga, IsiZulu, Sepedi and IsiXhosa – commonly spoken in Johannesburg. This approach aimed to ensure consistency and improve confidentiality and anonymity for participants whose mother languages were Xitsonga, IsiZulu, Sepedi and IsiXhosa, predominant in the communities under study. In addition, this approach avoided the need for interpreters, especially for those who might not comprehend English. Participants had an opportunity to ask questions regarding the research during each session of filling out the questionnaire. The researcher thanked each participant for participating in the study. About 25–30 minutes were spent filling out each questionnaire.
To ensure credibility, semi-structured interviews were conducted. Participants were free to express their views during the interviews, which were conversational in nature. In addition, to enhance credibility, the researcher avoided double barrel questions, expressed statements clearly, avoided framing the questions negatively, reframed and repeated the questions and asked questions related to the study and participants to ensure that the participants understood them.
Results
The researcher interviewed 20 young females. The primary topic of the interviews was abortion related to maternal mortality. Participants’ background characteristics are presented in the first section of the results. The results are presented according to the stated objectives of this study. Using pseudonyms, verbatim quotes from participants’ responses are used to support the results presented (refer to Table 1).
Social demographic characteristics of the study sample.
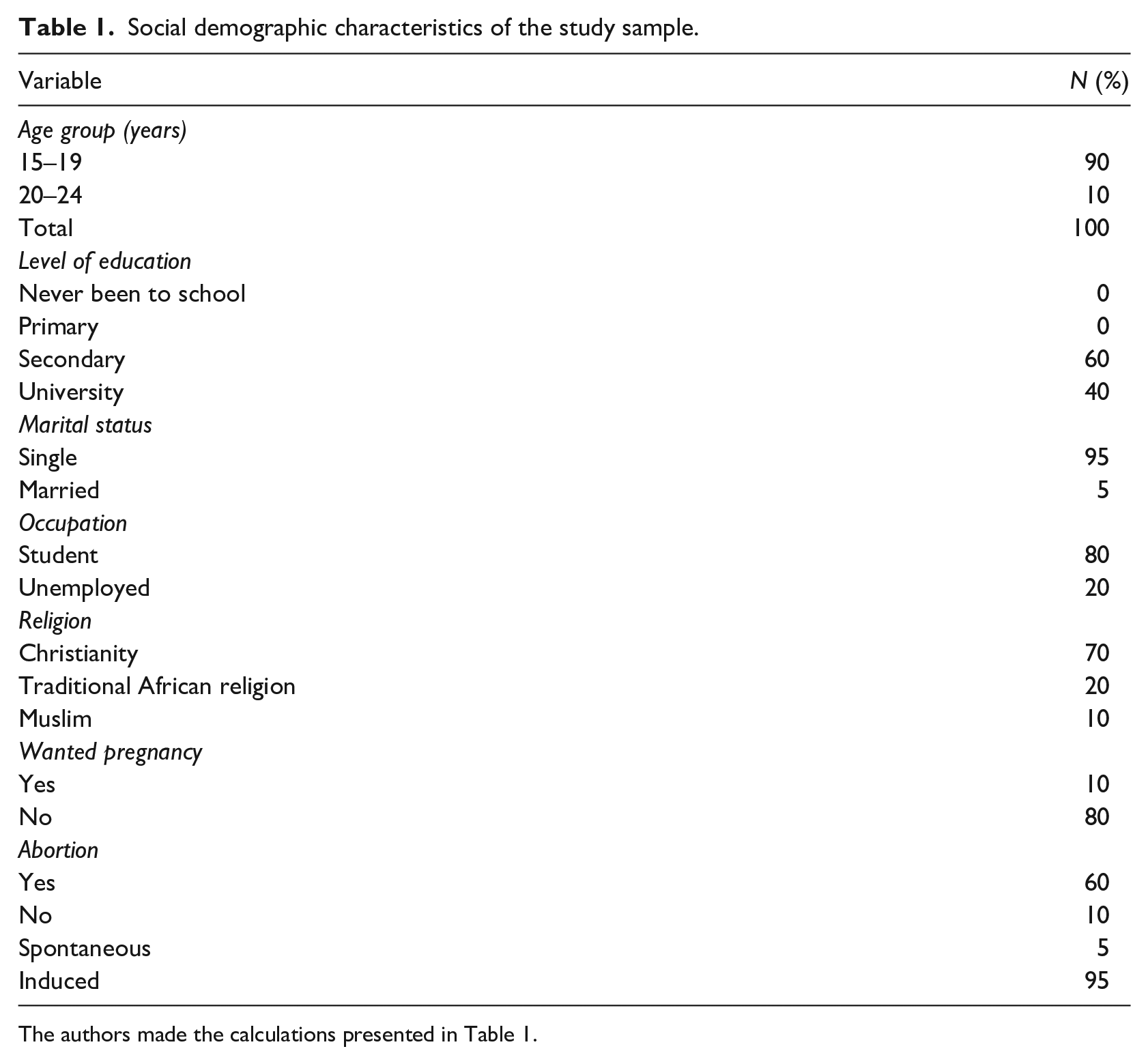

The authors made the calculations presented in Table 1.
Participants characteristics
As shown in Table 1, the study used 20 young females aged 15–24 years. There was also a majority of single participants. Most of them had a secondary education as their highest educational level. A higher percentage of participants identified black as their ethnic group. Most of the participants were unemployed and single.
Reasons for seeking abortion
An individual’s life is affected by a decision to terminate pregnancy. Women consider various factors when making decisions about reproductive health, especially regarding pregnancy and termination of pregnancy, including their physical, financial, social and spiritual well-being. Palomino et al. (2011: 74) wrote that ‘a pregnancy that is unplanned or unwanted does not take place in a vacuum, but rather takes place within a partner and family relationship as well as the broader social, political and cultural context’. According to Chetty (2012), participants cited various reasons for seeking an abortion. Among them were financial difficulties, the desire to complete their studies and conflict with the baby’s father.
According to participants in this study, the lack of interest their partners showed in them after they had told them they were pregnant influenced their abortion decision. A woman’s partner may have difficulty supporting her during an unplanned/unwanted pregnancy, as other studies have shown. Consequently, some women find it hard to continue the pregnancy without their partner’s support. In their study, Gresh and Maharaj (2014) found that women ended pregnancies if their partners did not support them.
Women sometimes separate from their partners because they deny paternity or refuse to take responsibility for their children. Participants confirmed this by saying, ‘As soon as I told him who the baby’s father was (which is him), he told me I should go talk to the baby’s father because he was not . . .’.
Men sometimes question the paternity of their children or claim they only slept with the girl once, according to Mkhwanazi (2010). Many young women have to make the great decision about their unplanned pregnancy on their own because of conflict with their partners. It is possible that the fact that all young women in this study were single and that some were abandoned or rejected by their baby’s father might have contributed to their decision to have an abortion.
Use of contraception
It was determined in this study that the participants did not use contraceptives or that they did so inconsistently, leading to unintended pregnancies. Although all the young women said they did not intend to have children, approximately 60% reported not using any form of contraception. In a study by MacPhail et al. (2007), fewer than half of young girls who were sexually active before the age of 24 years used some form of contraception to prevent unintended pregnancies.
One of the participants who was using the pill mentioned:
The fact that I became pregnant occurred because I was taking pills.
Other participants were using the injection:
The injection was used by me. My periods were irregular when I was taking the Depo injection, so when I stopped it. I began getting spotting, so I wanted to try something else so I could have my regular periods again. For the first three to four months after I stopped taking it, I did not get periods, and then I got them every day for two months. For 3 months, I bled daily. The bleeding would stop for a day, then resume. As a result, I had complications.
Three others used condoms. One reported that it burst, and the other two were inconsistent in using condoms.
My condom burst when I used it. The day we did not use a condom, yes I use one on a regular basis. The contraceptives I had been using – condoms, for example – sometimes I would not use them.
The findings of Selebalo (2010) support these responses, which found that inconsistency and low contraceptive use were apparent among sexually active teenagers. Unintended pregnancies are a significant cause of abortion, which, in some instances, is illegal, due to limited or inconsistent use of contraceptives. However, research shows that contraceptive methods do not always prevent unintended pregnancies, even when they are effective.
According to Ngene’s (2011) study, 75% of South Africans requesting termination of pregnancy services at the Durban Hospital used contraception when pregnant. In some instances, condoms break, and pregnancy occurs despite their effectiveness in preventing unplanned pregnancies. An emergency contraceptive would be most effective in this situation. It is difficult for women to access emergency contraceptives due to a lack of knowledge and lack of access to this service.
The reasons participants visit health facilities
The participants indicated different reasons for visiting health facilities when asked why they visited. The participants indicated that they visited health facilities to receive advice, reassurance, counselling or education on pregnancy when they had problems or complications. Twenty women filled out the questionnaire explaining that they were seeking advice, reassurance, counselling or education on pregnancy. According to some young female interviewees, they went to the public healthcare facility for treatment, while others stated that they would not recommend other pregnant women to go to the facility because of negligence of nurses.
As soon as you walk into the clinic, they will shout, ‘You are also pregnant, so what is your problem?’ You just step in, you are still asking for directions, on how to get a card, then you hear, ‘You are pregnant’; everyone at the clinic knows about you. Maybe you are pregnant because you were raped, and they have not heard your story. The moment you walk into the pharmacy, maybe you were sent there by your father or aunt, they shout, ‘Pill holders on this side, ARV users on the other. Have you coughed? The coughing you are doing is a sign of TB, so I want to check for it with your sputum’. Your child is at such a young age and look how you skipped school to make it here, you do not feel well when you consider taking them to the clinic. Your fear of being shouted at the clinic will cause you to miss clinic appointments. It has been my experience that when girls go to clinics, the sisters sometimes shout, ‘So, you are having sex too at your age!’
A minority of the participants were satisfied with the level of service provided at the clinics/hospitals where they received assistance, while most of them were dissatisfied for various reasons, including rude nurses, a lack of respect, unprofessional behaviour, unfriendliness and hostility. A healthcare worker is expected to display a welcoming attitude towards patients, to be friendly, to offer their patients seats, to listen to them, to speak to them in a way that is understandable to them and to provide general and pregnancy-related information to patients. This is outlined in the South African Health Rights Charter (2004).
A study conducted between 2012 and 2014 reported that poor interaction existed between clients and healthcare providers based on findings from the Confidential Enquiries into Maternal Deaths in South Africa. According to Mashao et al. (2015), mothers do not utilise maternity services because of the negative attitudes of health workers. Women’s confidence and compliance to medical care is bolstered by positive interactions between them and healthcare providers (Budhwani et al., 2022).
The maternal mortality ratio in South Africa is decreasing, as shown in Figure 1. There were 144.9 deaths per 100,000 live births in 2012, but the ratio has since fallen to 88.0 deaths per 100,000 in 2020. Compared to 2019, the decline in 2020 appears to be steeper (see Figure 1).
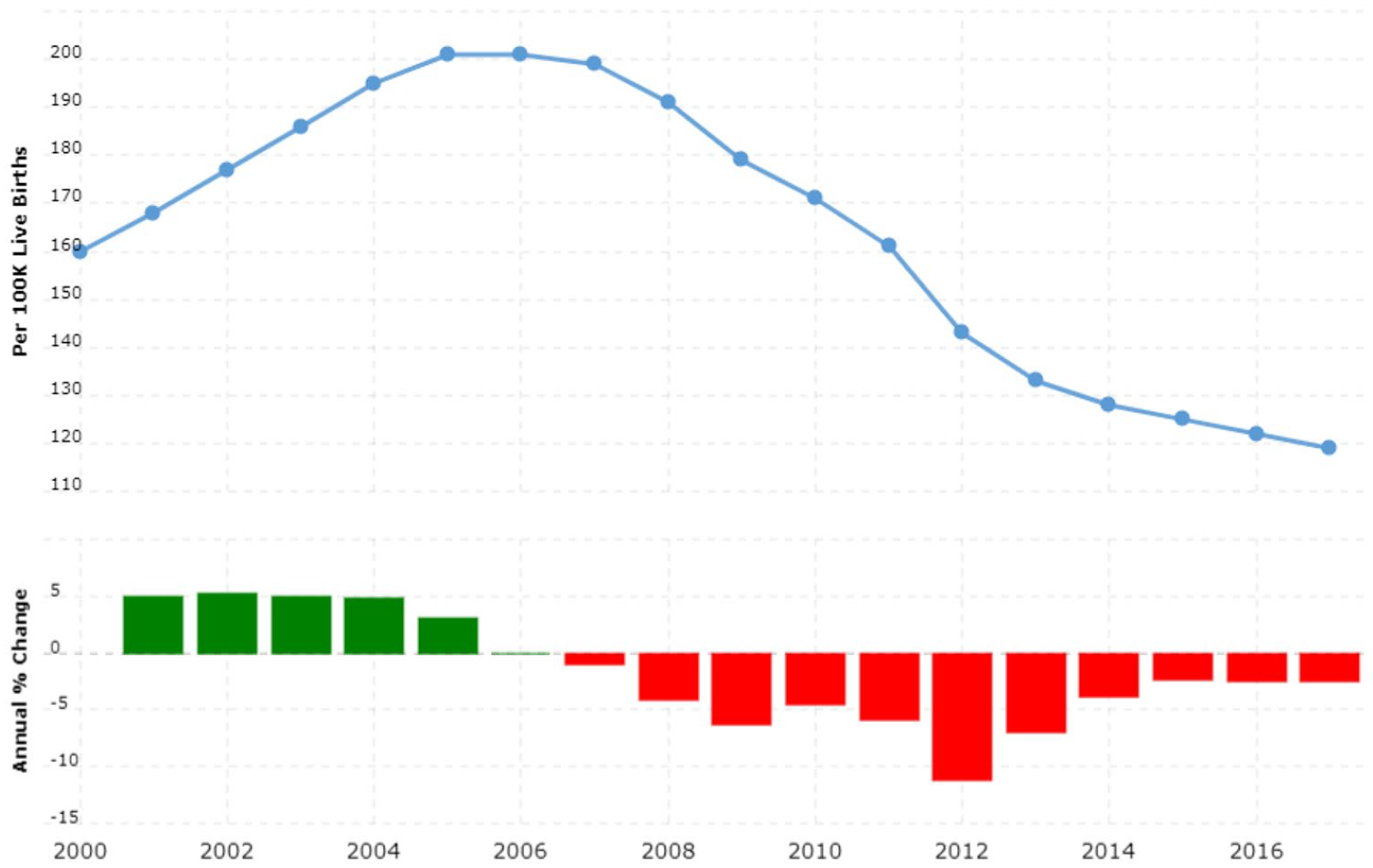
Maternal mortality in facility ratio.
Using the pregnant female’s age and the 1,047,886 live births to teenagers during the study period, a maternal mortality ratio was approximated using a proportion of all live births during the study period (n = 7,320,968) divided by all pregnant females’ ages. There were 2.03 maternal deaths per 100,000 live births among adults. The maternal mortality rate of teenagers was consistently lower than that of adult females throughout the period (Figure 1). There has been a consistent decline in adolescent and adult maternal mortality rates since 2009, when they peaked (Figure 2).
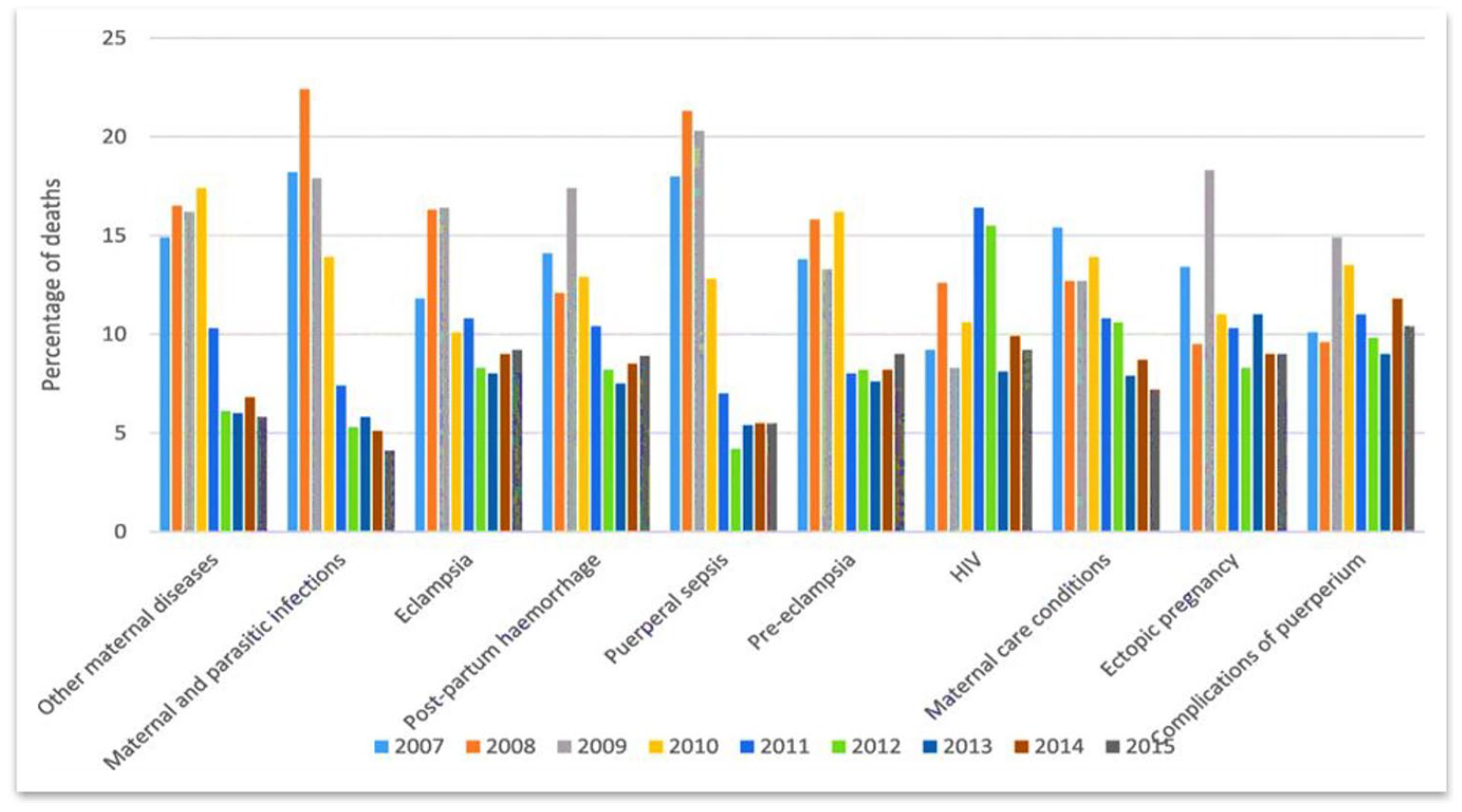
Causes of maternal mortality.
The highest rates of HIV and related causes (30%), viral diseases (29.4%), immune system disorders (28.2%) and other ill-defined causes (22.9%) were in the 25–29 years age group. Among indirect causes, HIV and related causes (23%) accounted for most maternal deaths (excluding miscellaneous indirect causes, 31.3%). Most accidents (23.2%) and events of unknown intent (28.4%) occurred among 20- to 24-year-olds. Among those older than 40 years, the highest rates of tuberculosis (24%) and miscellaneous indirect causes (26.7%) were observed. Women in KwaZulu-Natal died of four indirect causes and miscellaneous indirect causes most frequently, while women in Gauteng died of three indirect causes most frequently. Four indirect causes of death were most common in healthcare facilities.
It was difficult to analyse the occupation variable because it included occupations that could not be classified elsewhere. The number of deaths among non-professional women from all seven indirect causes and miscellaneous indirect causes was high. A similar trend was observed for deaths from indirect causes and miscellaneous indirect causes among those who had an unspecified educational status. With regard to all indirect and miscellaneous indirect causes, unmarried women had the highest death rate.
The direct causes of death also varied depending on age group, similar to the indirect causes. Indirect causes of death included other ill-defined diseases (23%), maternal infectious and parasitic diseases (17%) and hypertensive disorders (17%). Twenty- to 24-year-olds were most likely to suffer from hypertensive disorders (23.4%), puerperium complications (25%) and miscellaneous direct complications (23.5%). However, abortions (25.9%), other maternal disorders (26.1%), complications during delivery (27.8%), sepsis (26.7%), maternal infectious diseases (30.1%) and other ill-defined diseases (26.2%) mostly occurred among 25- to 29-year-olds. Haemorrhage (24.8%) and maternal care conditions (24.6%) caused the most deaths.
Discussion
This paper aims to provide insights into the mortality rate of young females of childbearing age in South Africa due to abortion. The purpose of this paper is to illustrate how young females in South Africa understand factors that influence maternal mortality and teenage pregnancy mortality rates. Individuals’ entire lives are affected by decisions to terminate pregnancy. Physical, social, financial and spiritual factors are considered when women make decisions regarding their reproductive health, especially pregnancy and termination. Young women’s decisions to seek abortions from illegal providers secretly seem to have been influenced by their fear of parents and their lack of support. Consequently, the young females may have been influenced to use illegal termination of pregnancy providers by their peers, who may not have been aware of legal termination of pregnancy services. Illegal abortions, including incomplete abortions, have many negative consequences that affect not only the abortion seeker but also her family and society as a whole. During the treatment of women who present to health facilities with post-abortion complications, the public health system of South Africa loses millions of rands (Banerjee et al. 2012).
Fear and confusion often accompany abortion decisions. Strong support structures can assist young females in making informed decisions when they make life-changing decisions like abortion. Unfortunately, women are forced to undergo abortion alone because of the stigma surrounding this life-changing decision and fears they will be mistreated and judged by their communities and loved ones. According to this study, young people in general have difficulty discussing their reproductive needs with their parents. However, it can also be assumed that parents make it difficult for young people to approach them about their reproductive and sexual problems.
Young females felt more comfortable confiding in their peers than in family members, especially parents. There is a communication barrier between parents and children, which is one of the most important concerns arising from this study. There appears to be a communication problem between children and parents, since none of the young females considered talking to their parents about the pregnancy. She is disappointed when her parents discover that she has unintentionally fallen pregnant. Young females secretly resort to abortion to maintain a good daughter identity and avoid disappointing their parents.
According to Mkhwanazi (2010), some parents punish their children when they learn they are pregnant, scream at them and, in some cases, banish them. Young females often worry about their parents’ reactions when they discover they are pregnant. The young females’ decisions to seek abortion from illegal providers seem to have been influenced by fear of their parents and their lack of support. It is also possible that young females were influenced by their peers to seek illegal termination of pregnancy services because they did not know of legal termination of pregnancy services.
Similar findings were found in other studies on teenage pregnancy and abortion in terms of contraceptive use among the youth. MacPhail et al. (2007) found that fewer than half of young girls use contraception to prevent unwanted pregnancy, despite two thirds of them engaging in sexual activity before the age of 24 years. The findings of this study show that many young females are not financially, psychologically, emotionally or socially ready to have children, but their use of contraceptives is limited or inconsistent, resulting in an increasing number of unplanned teenage pregnancies.
There were three methods of contraception: pills, injections every three months and condoms. A young female reported that her condom burst during intercourse, leading to an unintended pregnancy while condoms are believed to prevent sexually transmitted infections and unplanned pregnancies. Emergency contraceptives would be the most effective method in such a situation. This service is underutilised and difficult to access because of little knowledge of it. Approximately 5% of the participants in Ngene’s study (2011) were unaware of emergency contraceptives.
Many unwanted pregnancies among young females are caused by contraceptive methods failing to prevent unintended pregnancies, resulting in abortions. According to Deschner and Cohen (2003: 7), ‘women who wish to limit their family size and time of childbearing will use any means available to them to achieve this; if contraception is not an option, women will seek abortion even if it is illegal’. In view of these findings, it is imperative not only to make contraception information accessible to the youth but also to improve contraceptive methods to prevent unintended pregnancies.
The low life expectancy of women in South Africa is largely due to maternal mortality, which is a serious public health problem in any developing country. As part of the study, four objectives were met:
Perceived factors contributing to maternal mortality among women in health facilities were identified and described.
The knowledge of women regarding reproductive health services available in public health facilities that would reduce maternal mortality was described.
The socioeconomic, cultural and knowledge factors that affected women’s attendance at antenatal care services were analysed.
Policy changes that would improve women’s access to early antenatal care were suggested.
Over time, maternal mortality in South Africa has decreased. Over the past 20 years, healthcare facilities in South Africa have undergone major reforms that have increased accessibility and affordability (Burger and Christian, 2020). According to a Johannesburg study of 208 adult females, 97% reported seeking antenatal care early in their pregnancy in the area of obstetric care (Solarin and Black, 2013). It is also possible that South Africa’s declining fertility rate may be contributing to reduced maternal mortality (Swartz, 2009).
Conclusions
Maternal mortality remains a serious public health concern in South Africa and contributes to women’s low life expectancy. The study identified several factors that contributed to maternal mortality in the study area. An in-depth interview with 20 young females was conducted as part of this mixed-methods study to gain a better understanding of teenage pregnancy mortality rates in South Africa. Maternal risks during pregnancy were well known to more women. However, socioeconomic factors and inadequate knowledge of danger signs were among the factors that prevented women from using health facilities. In addition, long distances, lack of transport and the high cost of healthcare contributed to them delivering at home. Furthermore, most women complained of sudden onset of labour due to a lack of knowledge about key elements of birth preparation. One of the factors that contributed to women not using health facilities was the poor quality of healthcare services.
Footnotes
Acknowledgements
The authors would like to acknowledge participants for their willingness to contribute to the study.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Availability of data and materials
The primary data collected for this study, as part of the Ph.D. programme, remain unpublished. We are willing to provide the data upon requests based on the specific requirements of interested parties.
