Abstract
Globally, migrant workers often take ‘3-D jobs’ – dirty, dangerous, and demanding. In Norway, they mainly work in construction, manufacturing, and healthcare, often in low-wage positions. However, little is known on the occupational health outcomes of migrant workers. This study utilizes Statistics Norway’s (SSB) Living Conditions and Work Environment Panel Survey 2022, which includes 35,000 respondents, to explore how migrant status affects health. Results show that psychosocial work exposure has a stronger association with mental health symptoms among non-Norwegian workers, while mechanical work hazards are more strongly associated with musculoskeletal symptoms among non-Norwegian workers.
Background
The United Nations Sustainable Development Goal 8 (SDG 8) aims to promote decent work and economic growth, with a specific focus on ‘protecting labor rights and promoting safe and secure working environments for all workers, including migrant workers’ (target 8.8) (United Nations, 2016). Migrant workers are a critical focus because employment opportunities are a primary driver of cross-border migration (Hargreaves et al., 2019). According to the International Labour Organization (ILO), in 2019, there were 169 million international migrant workers, constituting 4.9 percent of the labor force in destination countries (International Labour Organization, 2021). In the European Union (EU) alone, labor migrants comprise 17 percent of the workforce, with 33 million migrants contributing significantly to various sectors (Sterud et al., 2018). In addition, approximately 17 million European citizens live or work in other EU Member States. The European Pillar of Social Rights emphasizes the importance of safeguarding workers’ rights, aiming to build a fair, inclusive, and opportunity-filled social Europe (European Commission, 2022). Despite these efforts, work-related illnesses and accidents remain prevalent, contributing to significant mortality and economic loss across the EU. In 2017, work-related illnesses accounted for approximately 200,000 deaths annually in the EU, alongside 3300 fatal and 3.2 million non-fatal workplace accidents resulting in at least 4 days of absence from work (EuroStat, 2021). The economic cost of these workplace accidents and illnesses is estimated to account for 3.4 percent of the EU’s gross domestic product (GDP) each year (Tompa et al., 2021).
Globally, a significant proportion of migrant workers are employed in the service sector (66.2%), followed by industry (26.2%) and agriculture (7.1%) (Moyce and Schenker, 2018). Within these sectors, migrant workers are often relegated to ‘3-D jobs’ – dirty, dangerous, and demanding – which are frequently overlooked by policymakers and the public (Takala et al., 2014). These jobs expose migrants to various occupational hazards, resulting in poor health outcomes, workplace injuries, and fatalities (Sterud et al., 2018; Takala et al., 2014; Yanar et al., 2018). In 2014, it was estimated that there were 2.3 million occupational fatalities worldwide, with 2 million attributed to work-related diseases and 0.3 million to occupational injuries, with higher rates observed among migrant workers (Takala et al., 2014). Migrant workers often lack proper training, work without adequate protective equipment, and are less likely to report unsafe working conditions, increasing their risk of occupational injuries and fatalities compared with native-born workers, even when performing the same jobs in the same industries (Moyce and Schenker, 2018). This situation underscores the importance of studying musculoskeletal and mental health symptoms, key indicators of occupational health and safety, given their global prevalence as leading causes of disability and poor health (James et al., 2018).
Mechanical work hazards and musculoskeletal symptoms
Numerous studies have established a link between work-related mechanical risk factors and musculoskeletal problems, such as lower back pain, pain in the elbow, forearm, hands, hips, legs, and knees (Farioli et al., 2014; Govaerts et al., 2021; Madsen et al., 2018). For example, healthcare workers exposed to high levels of mechanical work hazards, such as lifting and transferring patients, are strongly associated with musculoskeletal pain (Mirmohammadi et al., 2015). Similar findings have been observed in other studies, linking long working hours to increased musculoskeletal symptoms (Lee et al., 2018).
Psychosocial work hazards and mental health symptoms
Psychosocial work factors refer to social characteristics of the work environment that interact with individual psychological factors (Havermans et al., 2018). High psychological demands at work are associated with an increased risk of mental health problems, such as anxiety and depression (Havermans et al., 2018; Plaisier et al., 2007; Virtanen et al., 2007). For instance, low job autonomy and poor decision-making procedures have been linked to mental health issues among hospital employees (Elovainio et al., 2004). Similarly, dissatisfaction with leadership and co-worker relationships has been found to significantly increase the odds of experiencing mental health problems (Gamperiene et al., 2006).
Occupational health and safety programs and policies in Norway
In 1992, Norway introduced the Internal Control (IC) Regulation in response to the tragic oil rig disaster in March 1980 when the ‘Alexander Kielland’ platform collapsed, resulting in the loss of 123 workers’ lives (Saksvik and Quinlan, 2003). The IC Regulation aimed to create a comprehensive national system for occupational health and safety (Saksvik and Quinlan, 2003). Further strengthening these efforts, the Working Environment Act was introduced in 1997 to ensure a healthy and meaningful working environment, safeguarding against harmful physical and mental influences (Arbeidstilsynet, 2020). Despite these measures, Norway has not ratified several key ILO conventions crucial for promoting occupational safety and health, particularly for vulnerable groups such as migrants, raising concerns about the adequacy of protections for these workers.
Theoretical perspective
Othering theory and immigration
Othering theory helps explain how immigrants are marginalized in host societies due to perceptions that they are fundamentally different from the dominant population (Viruell-Fuentes, 2007). This process creates social, cultural, and economic boundaries, leading to exclusion and discrimination (Grove and Zwi, 2006). Immigrants are often seen as outsiders, which reinforces negative stereotypes and limits their access to opportunities, including education, employment, and social services. As a result, they are placed on the margins of society, facing challenges in integration and social mobility (Udah and Singh, 2019). Research highlights that this marginalization happens across many host countries, further entrenching the notion of immigrants as ‘others’ who do not fully belong in the dominant social fabric (Reidpath and Allotey, 2019).
This othering process impacts immigrants in numerous ways, mainly in how they access labor markets and navigate social structures. Studies have shown that immigrants often face significant barriers, including discrimination and xenophobia, which restrict their upward mobility and force them into more precarious employment positions (Hossin, 2020; Kosny et al., 2016). As immigrants are treated as ‘outsiders’, they are frequently funneled into jobs stigmatized or seen as undesirable by the native population (Reidpath and Allotey, 2019). The result is that immigrants become overrepresented in specific sectors of the labor market, such as manual labor and low-wage service jobs (Duncan and Trejo, 2009).
Othering and workplace-related health outcomes
The exclusion that immigrants experience in the workplace has significant consequences for their mental and physical health. Immigrants often endure workplace discrimination, such as being passed over for promotions or receiving lower wages than their native-born counterparts, microaggressions like being the subject of derogatory jokes or comments, and unequal treatment, which leads to chronic stress (Shenoy-Packer, 2014). This stress is associated with a range of health problems, including depression, anxiety, hypertension, and other cardiovascular issues (Elshahat et al., 2022). Chronic stress is a known risk factor for many health conditions, and the hostile work environments that result from othering amplify these risks for immigrant populations (Rosemberg et al., 2022). In addition to mental health concerns, the physical toll of being othered in the workplace can be profound. Immigrants often face unsafe working conditions and a lack of access to healthcare, compounding their physical health challenges (Sally and Marc, 2018). Barriers such as language difficulties, inadequate healthcare provisions, and fear of deportation further prevent many immigrants from seeking the care they need (Elshahat et al., 2022; Reidpath and Allotey, 2019). The Healthy Immigrant Effect is a phenomenon where immigrants initially arrive in better health than their native-born counterparts, but this health advantage diminishes over time as these stressors take a toll on their wellbeing (Elshahat et al., 2022; Hossin, 2020; Markides and Rote, 2018).
Othering and physically strenuous jobs
Othering provides a useful framework for understanding why immigrants are disproportionately represented in physically demanding, low-wage jobs. Systemic discrimination and barriers often push immigrants into labor-intensive industries such as agriculture, construction, and manufacturing (Elshahat et al., 2022). These sectors typically involve tasks characterized by repetitive movements, heavy lifting, and unsafe working conditions, contributing to an increased prevalence of musculoskeletal disorders, including chronic back pain, joint strain, and other related health issues (Sally and Marc, 2018). The lack of proper safety measures and training further elevates the risk of workplace injuries for immigrant workers, as protections like ergonomic support are often inadequate (Reidpath and Allotey, 2019; Sally and Marc, 2018).
Research indicates that immigrant workers in such physically demanding roles frequently endure long hours under harsh conditions, with inadequate safety protocols (Mondragón, 2011). In addition, due to their vulnerable socioeconomic and legal status, many immigrants underreport injuries, fearing job loss or deportation (Mondragón, 2011). This, in turn, leads to untreated musculoskeletal conditions that worsen over time (Reidpath and Allotey, 2019). Compounding these challenges is the fact that immigrants are less likely to be unionized or have access to health insurance, which further exacerbates their physical health issues and financial hardships (Thomas et al., 2014).
In conclusion, othering theory is instrumental in explaining why immigrants face higher rates of physical and mental health challenges in the workplace. Their marginalization restricts their access to safer, better-paid jobs and pushes them into physically demanding roles, increasing their susceptibility to both workplace injuries and mental health difficulties (Elshahat et al., 2022).
Given these factors, immigrant workers are particularly vulnerable. Reducing occupational health and safety (OHS) risks for critical and vulnerable groups is essential to building a fairer and more equal society. In 2018, immigrants made up approximately 17 percent of Norway’s population (i.e. 920,000 people). Since 1990, about 34 percent of immigrants have come to Norway for work (Statistics Norway, 2021). Following the EU enlargement in 2004, Norway experienced a significant influx of labor migrants, particularly in sectors like construction, manufacturing, and healthcare (Ødegård, 2020; Slettebak, 2020). These sectors are associated with exposure to hazards that result in adverse health outcomes, but there are limited data on the occupational health outcomes of migrant workers in Norway. This gap in knowledge hampers policymakers’ ability to address and improve the occupational health and safety of migrants. This study aims to fill this gap by exploring the associations between occupational hazards, immigration status, and health outcomes among migrant workers in Norway.
Hypothesis
Based on the discussion above, this study expects to find associations among indicators of occupational health exposure, immigration status, and health outcomes:
H1: People with a higher level of exposure to mechanical work hazards have a higher degree of musculoskeletal symptoms.
H1a: The relationship between exposure to mechanical work hazards and musculoskeletal symptoms will be stronger for non-Norwegians than Norwegians.
H2: People with a higher level of exposure to psychosocial work hazards have a higher degree of mental health symptoms.
H2b: The relationship between exposure to psychosocial work hazards and mental health symptoms will be stronger for non-Norwegians than Norwegians.
Method
Study design
This study adopted a quantitative research design to explore the impact of various occupational health hazards and migrant status on occupational health outcomes. Data were drawn from the Living Conditions and Work Environment Panel Survey 2022, conducted by Statistics Norway (SSB) between August 15, 2022 and April 10, 2023. This survey sampled 35,000 individuals aged 17–67 years, with a random sample of 20,000 drawn from the target population 2023 (Statistics Norway, With ML and Bye, 2024). An additional selection of 15,000 individuals was then drawn from the employed group, with an emphasis on those without higher education. The Living Conditions and Work Environment Survey is a longitudinal panel survey that collects data every 3 years from the same participants on key areas such as employment status, working conditions, physical and mental health, and work environment characteristics 2023 (Statistics Norway, With ML and Bye, 2024).
Measures
Exposures
Mechanical work hazards
Mechanical work hazards were measured through self-reported exposure to six specific mechanical risk factors: (1) neck flexion, (2) squatting/kneeling, (3) forward bending, (4) awkward lifting, (5) heavy physical work, and (6) standing/walking. These measures, developed by an expert group as part of a Nordic cooperative project, have been utilized in the Living Conditions Survey since 1989 (Lindström et al., 2000; Orhede, 1994). Respondents indicated their exposure on a binary scale (‘Yes’ or ‘No’) and further categorized the duration of exposure into one of five categories ranging from ‘almost all the time’ to ‘a very small part of the time’. An index score for mechanical work hazards was calculated by summing the exposure values across all six items, with lower scores indicating greater exposure. The internal consistency of this scale was confirmed with a Cronbach’s Alpha coefficient of 0.75.
Psychosocial work hazards
Psychosocial work hazards were assessed using self-reported data on three key dimensions: quantitative demands, role conflict, and emotional demands. These dimensions were derived from the General Nordic Questionnaire for Psychological and Social Factors at Work (QPS Nordic). Quantitative demands were evaluated with a single item on workload, role conflict was assessed with three items, and emotional demands were captured with one item. Respondents rated their experiences on a five-point Likert-type scale ranging from ‘to a very high degree’ to ‘not at all’. An index score for psychosocial work hazards was computed by summing the scores across these dimensions, with lower values indicating higher exposure to psychosocial risks. The reliability of this measure was supported by a Cronbach’s Alpha coefficient of 0.61.
Outcomes
Musculoskeletal symptoms
Musculoskeletal symptoms were self-reported and included pain in the neck and shoulders, lower back, elbows, forearms, hands, hips, legs, knees, and feet. Respondents rated the severity of their symptoms on a four-point scale ranging from ‘Very bothered’ to ‘Not bothered’. An index score was created by summing the responses across the four symptom categories, with lower scores indicating higher musculoskeletal symptoms. The internal consistency of the musculoskeletal symptom scale was verified with a Cronbach’s Alpha of 0.69.
Mental health symptoms
Mental health symptoms were assessed using self-reported data on depression, nervousness/anxiety, and difficulty sleeping. These symptoms were also rated on a four-point scale, similar to the musculoskeletal symptoms. An index score was generated by summing the values of these three symptoms, with lower scores indicating greater mental health difficulties. The reliability of this measure was confirmed with a Cronbach’s Alpha coefficient of 0.71.
Covariate
Gender was included as a covariate in the analysis due to its known association with both mechanical work hazards and musculoskeletal symptoms, as well as with psychosocial work hazards and mental health outcomes. For example, Nordander et al. (2008) found that females are at a higher risk for musculoskeletal disorders and are more physically exposed than males. In addition, psychosocial working conditions are significant predictors of musculoskeletal pain, as evidenced by studies linking work-related psychosocial factors to low back pain in the general Norwegian working population (Sterud and Tynes, 2013). Thus, gender was statistically controlled for in both moderation models, and psychosocial work hazards were controlled for in the second moderation model.
Analytical strategy
Prior to conducting any statistical analyses, primary data screening and normality tests were performed on all variables to ensure data accuracy and integrity. Descriptive statistics, including frequency, mean, standard deviation, and percentage of respondents, were reported for all variables used in the study. Two separate moderation models, depicted in Figures 1 and 2, were employed to evaluate the associations between mechanical work hazards and musculoskeletal symptoms, as well as psychosocial work hazards and mental health symptoms. Multiple regression analysis was then utilized to assess the impact of immigrant status on health outcomes, following the methodology outlined by Aiken and West (Aiken et al., 1991). This approach involved calculating an interaction term by multiplying exposure to occupational hazards by worker status, and then using exposure, worker status, and the interaction term as predictors in the regression model.
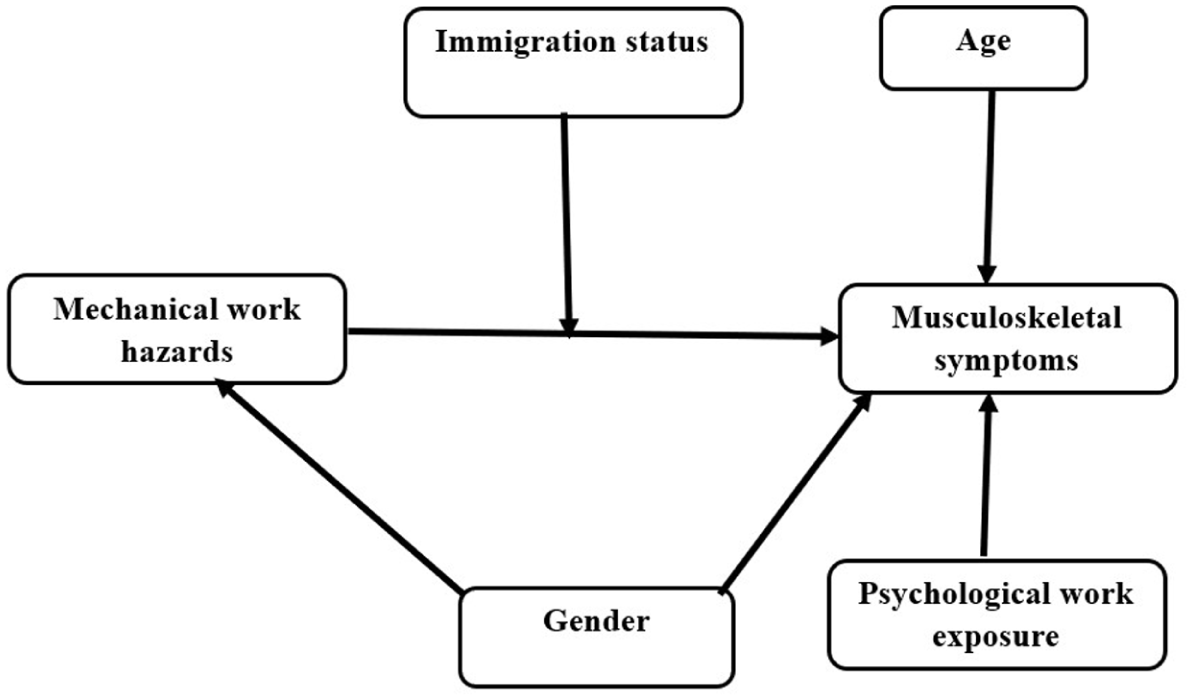
Moderation model illustrating the interaction between mechanical work hazards and immigration status on musculoskeletal symptoms among respondents (N = 17,971), based on the Living Conditions and Work Environment Panel Survey 2022, conducted by Statistics Norway (SSB), August 15, 2022–April 10, 2023.
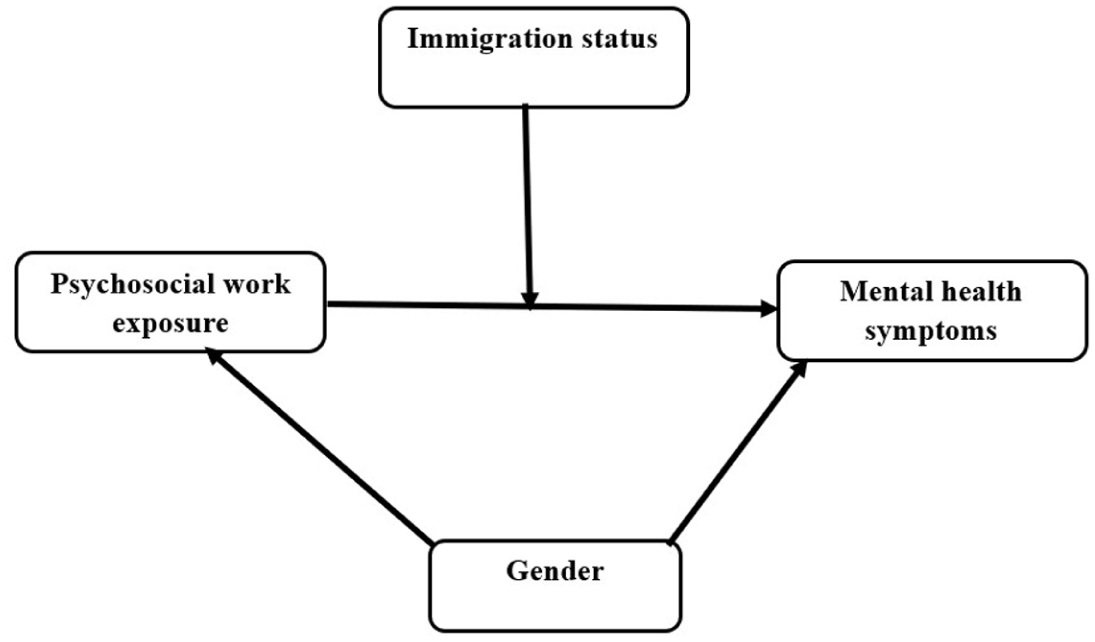
Moderation model illustrating the interaction between psychosocial work hazards and immigration status on mental health symptoms among respondents (N = 17,971), based on the Living Conditions and Work Environment Panel Survey 2022, conducted by Statistics Norway (SSB), August 15, 2022–April 10, 2023).
Furthermore, we adopted stratified sensitivity analysis to assess the robustness of the main findings across work types (permanent and temporary). We conducted separate multiple linear regression analyses for each group using mental health symptoms as the dependent variable and psychosocial work exposures as the independent variable. All models controlled for age, gender, and birth country and included an interaction term between psychosocial work exposures and birth country. Similarly, we performed multiple linear regression analyses for each group with Mechanical work hazards as the dependent variable and Musculoskeletal symptoms as the independent variable. These models controlled for age, gender, and birth country, and included an interaction term between Mechanical work hazards and birth country.
Results
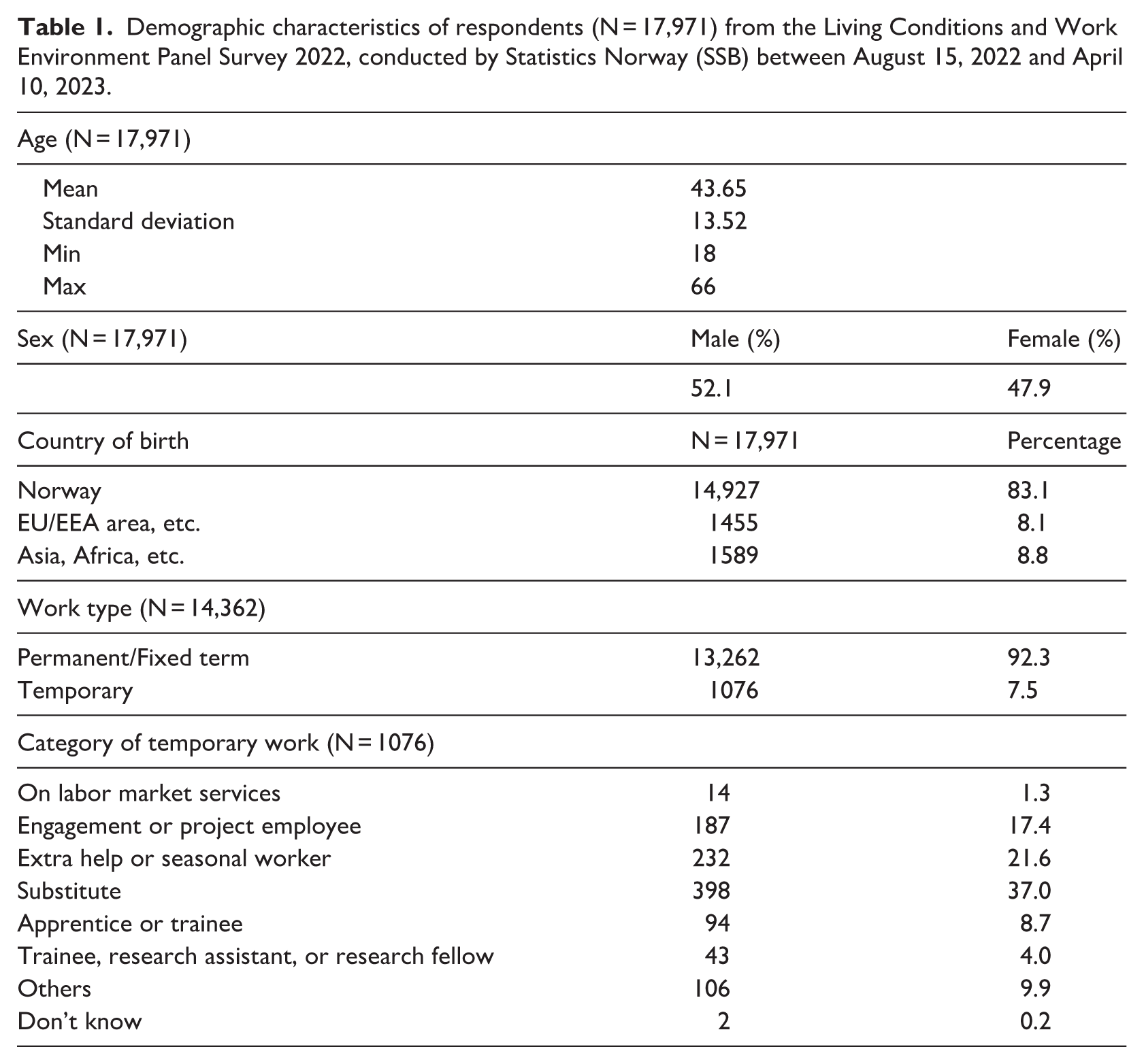
In this study, 17,971 respondents were included in the final analysis. Of these respondents, 52.10 percent were male, while 47.90 percent were female. The mean age of the respondents was 43.65 years. The majority of respondents (83.1%) were Norwegian citizens, while immigrants comprised 16.9 percent of the sample, as shown in Table 1.
Demographic characteristics of respondents (N = 17,971) from the Living Conditions and Work Environment Panel Survey 2022, conducted by Statistics Norway (SSB) between August 15, 2022 and April 10, 2023.
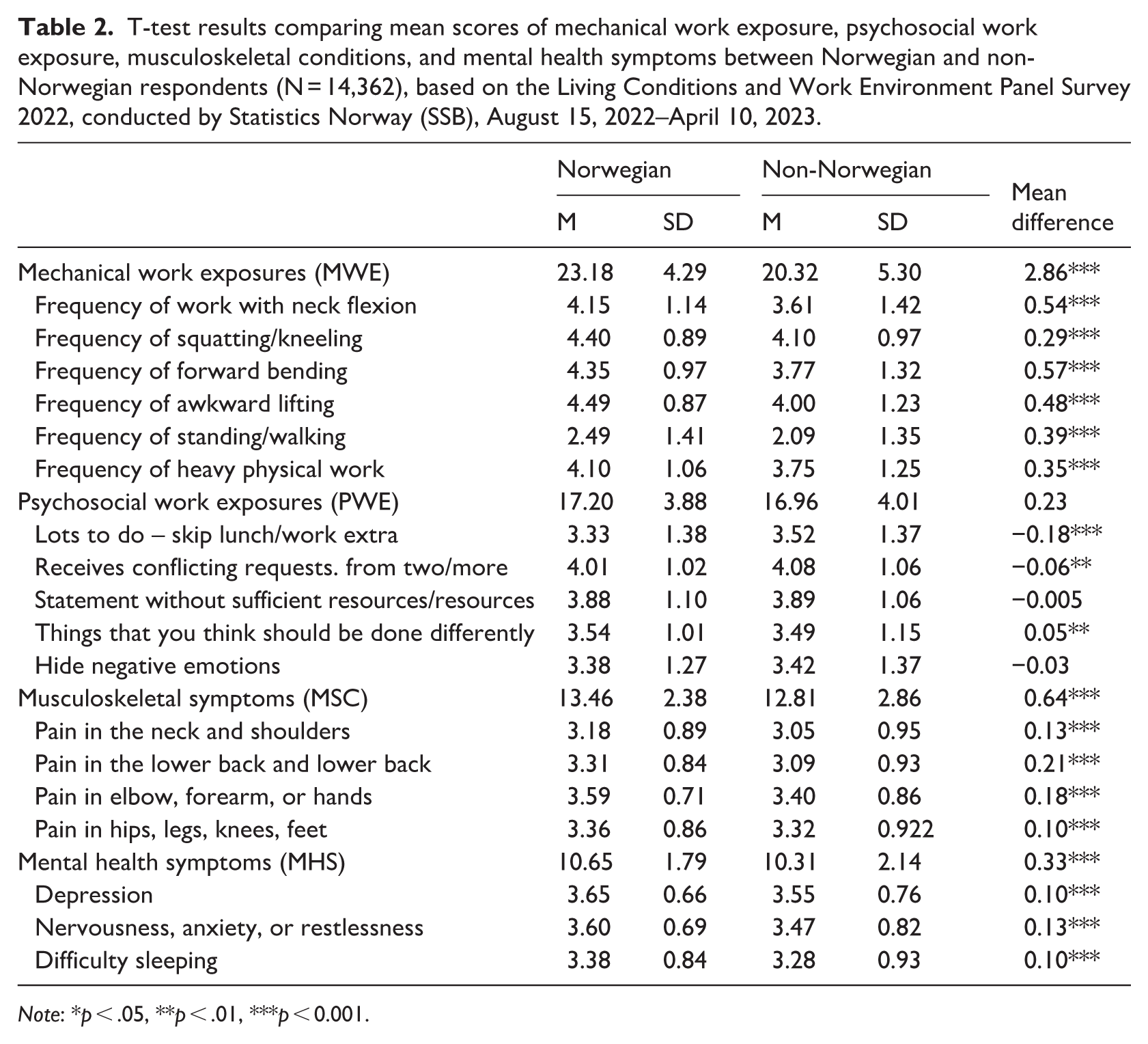
An independent t-test was conducted to compare the mean differences between Norwegian and non-Norwegian respondents across various outcome and exposure variables, as shown in Table 2. The mean score for mechanical work exposure was 23.18 for Norwegians and 20.32 for non-Norwegians. In terms of psychosocial work exposure, the mean score for Norwegians was 17.20, while for non-Norwegians, it was slightly lower at 16.96. When examining musculoskeletal symptoms, Norwegians had a mean score of 13.46 compared with 12.81 for non-Norwegians. For mental health symptoms, Norwegians had a mean score of 10.65, whereas non-Norwegians had a considerably lower mean score of 10.31. This means that non-Norwegians have a high exposure to both mechanical work hazards and psychosocial work hazards, musculoskeletal symptoms, and mental health symptoms.
T-test results comparing mean scores of mechanical work exposure, psychosocial work exposure, musculoskeletal conditions, and mental health symptoms between Norwegian and non-Norwegian respondents (N = 14,362), based on the Living Conditions and Work Environment Panel Survey 2022, conducted by Statistics Norway (SSB), August 15, 2022–April 10, 2023.
Note: *p < .05, **p < .01, ***p < 0.001.
Table 3 presents the results of a moderation model examining how respondents’ birth country influences the relationship between mechanical work hazards and musculoskeletal symptoms. After controlling age, gender, and psychosocial work exposure, it was found that musculoskeletal symptoms increased by an average of 0.27 units for each one-unit increase in exposure to mechanical work hazards. This relationship was statistically significant (p < 0.001). However, when birth country status (i.e. Norwegian vs immigrant) was added as a predictor in the model, musculoskeletal symptoms were 3.54 units. The interaction term (−0.12) was significant (p > 0.01), indicating that mechanical work hazards are more strongly associated with musculoskeletal symptoms among non-Norwegians.
Model summary for moderation analysis examining the interaction between mechanical work exposure and birth country on musculoskeletal conditions among respondents (N = 14,362), Living Conditions and Work Environment Panel Survey 2022, conducted by Statistics Norway (SSB), August 15, 2022–April 10, 2023.
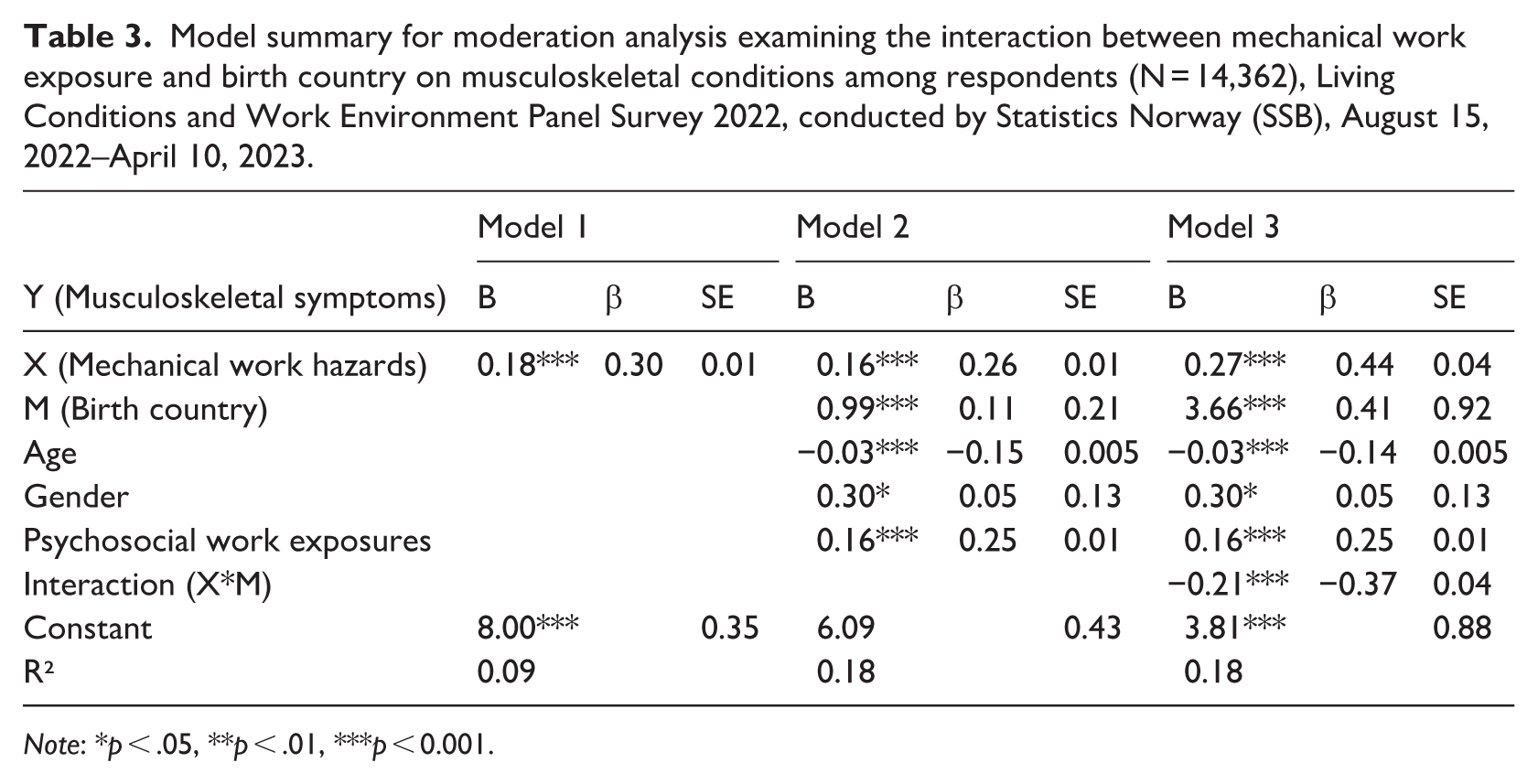
Note: *p < .05, **p < .01, ***p < 0.001.
This suggests that being an immigrant increases the risk of experiencing musculoskeletal symptoms in relation to mechanical work exposures.
Table 4 details the results of another moderation model exploring the influence of birth country status on the association between psychosocial work exposure and mental health symptoms. Controlling for age and gender, a one-unit increase in psychosocial work exposure was associated with a 0.21-unit increase in mental health score, indicating better mental health. This relationship was statistically significant (p < 0.001). Furthermore, the interaction term (−0.06) was significant (p > 0.01), indicating that psychosocial work exposures have a stronger association with mental health symptoms among non-Norwegians.
Model summary for moderation analysis examining the interaction between psychosocial work exposure and citizenship on mental health symptoms among respondents (N = 14,362), Living Conditions and Work Environment Panel Survey 2022, conducted by Statistics Norway (SSB), August 15, 2022–April 10, 2023.
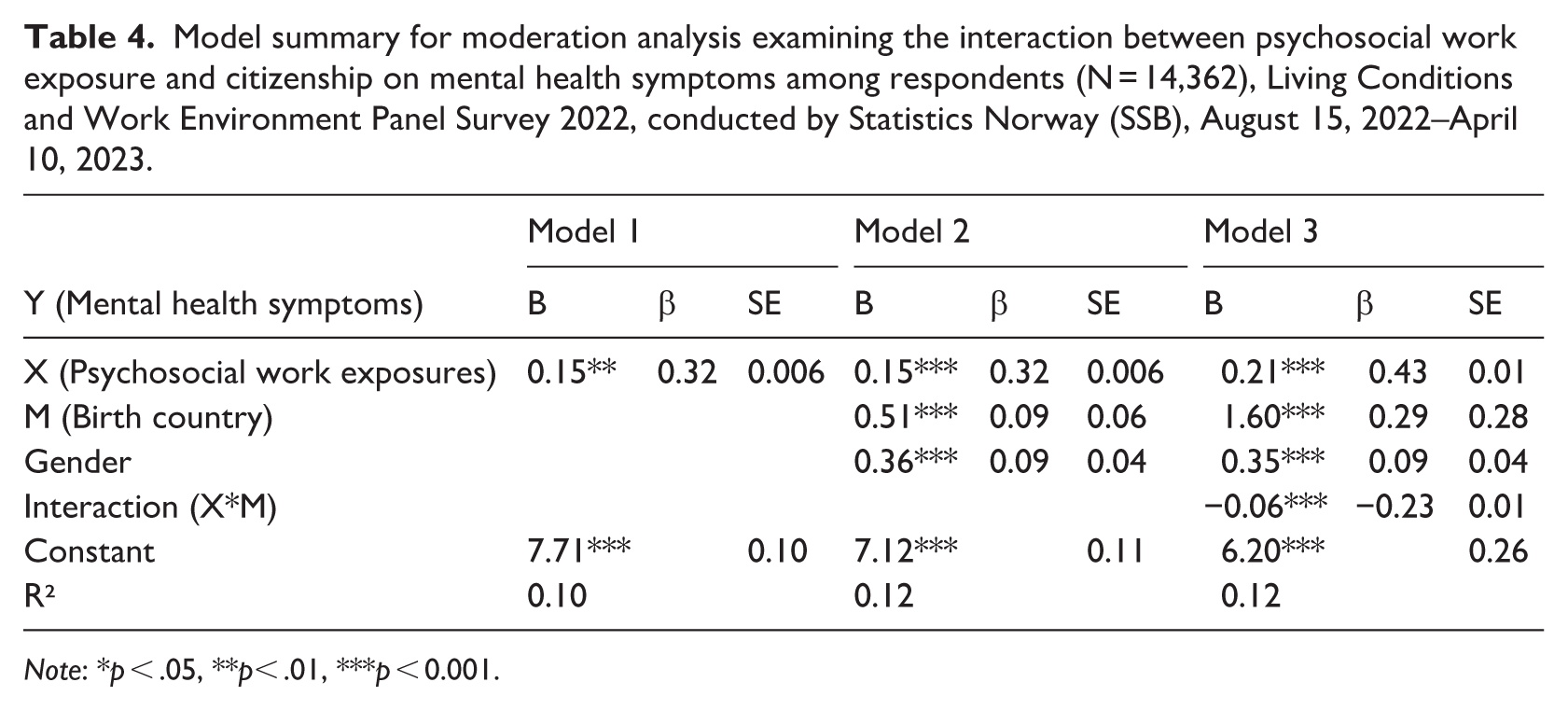
Note: *p < .05, **p< .01, ***p < 0.001.
Sensitivity analysis
Table 5 presents stratified sensitivity analyses by work type, indicating that the association between psychosocial work exposures and mental health symptoms was significant in both groups but differed in strength. Among permanent workers, higher psychosocial work exposures were associated with higher mental health scores (B = 0.20, β = 0.42, p < 0.001) after accounting for age, gender, and birth country. For temporary workers, the association was somewhat stronger (B = 0.29, β = 0.50, p < 0.001). The interaction between psychosocial work exposures and birth country remained significant in the permanent worker group (B = −0.06, p < 0.001), indicating that the impact of psychosocial hazards was weaker for workers born in Norway than for non-Norwegians. The overall pattern was consistent with the primary analysis, reflecting the robustness of the findings across employment groups.
Stratified analysis of musculoskeletal conditions and mechanical work exposure by birth country among respondents (N = 14,362), Living Conditions and Work Environment Panel Survey 2022, conducted by Statistics Norway (SSB), August 15, 2022–April 10, 2023.
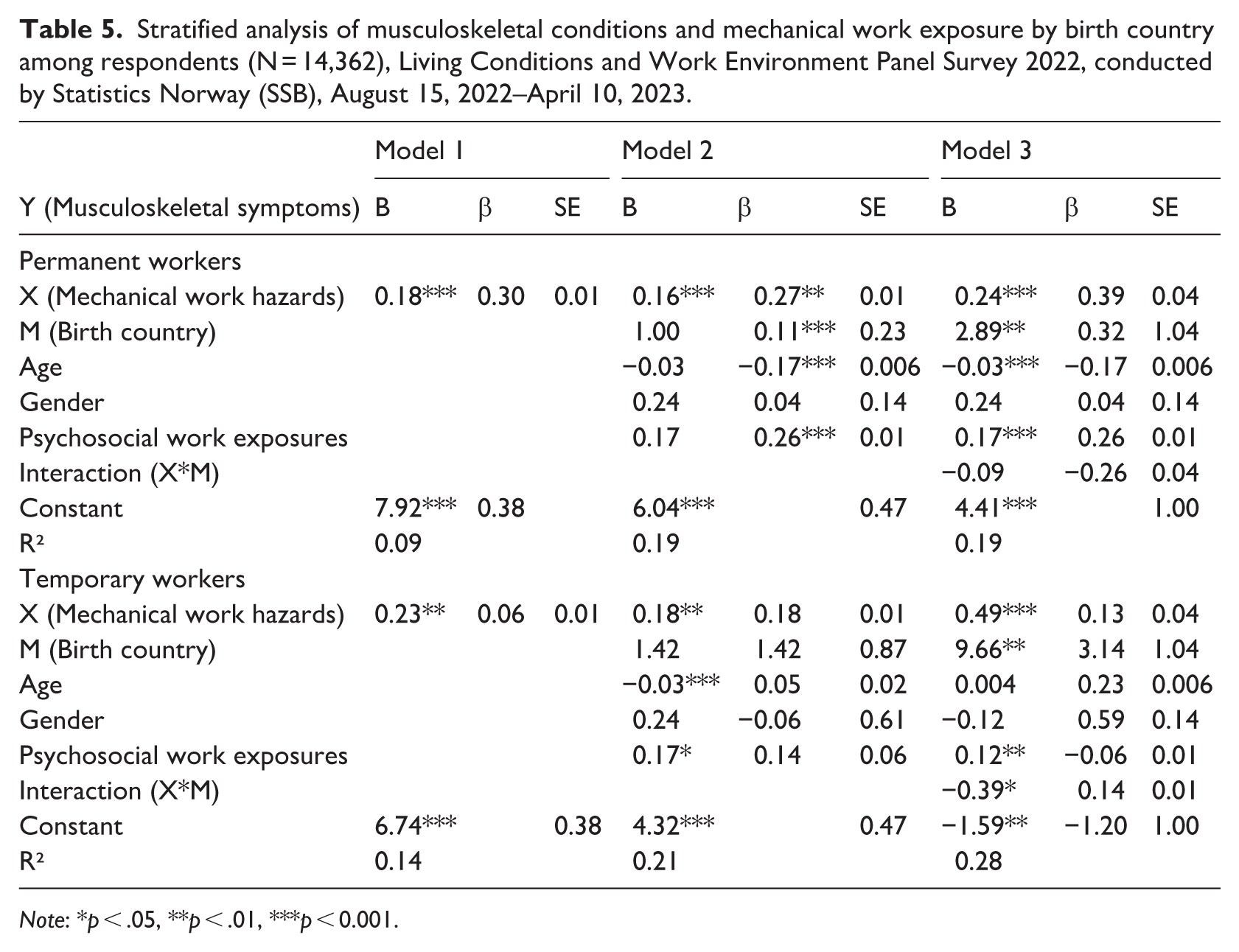
Note: *p < .05, **p < .01, ***p < 0.001.
The stratified sensitivity analyses by work type, presented in Table 6, among permanent workers showed that higher mechanical work hazards were significantly associated with higher levels of musculoskeletal symptoms (B = 0.24, β = 0.39, p < 0.001) after adjusting for age, gender, and birth country. Birth country also remained a significant predictor (B = 2.89, p < 0.01). The interaction between mechanical work hazards and birth country was not statistically significant, suggesting that this relationship did not differ between Norwegians and non-Norwegians. Among temporary workers, the association between mechanical work hazards and musculoskeletal symptoms was stronger (B = 0.49, β = 0.53, p < 0.001). Birth country was again significant (B = 5.66, SE = 1.34, p < 0.001), and a significant negative interaction term (B = –0.35, p < 0.001) indicated that the relationship between work hazards and musculoskeletal symptoms was weaker among Norwegian workers than among non-Norwegian workers. The overall pattern of results was consistent with the primary analysis, indicating that higher mechanical work hazards were associated with greater musculoskeletal symptoms across both employment types, with a more substantial effect observed among temporary workers.
Stratified analysis of mental health symptoms and psychosocial work exposure by birth country among respondents (N = 14,362), Living Conditions and Work Environment Panel Survey 2022, conducted by Statistics Norway (SSB), August 15, 2022–April 10, 2023.
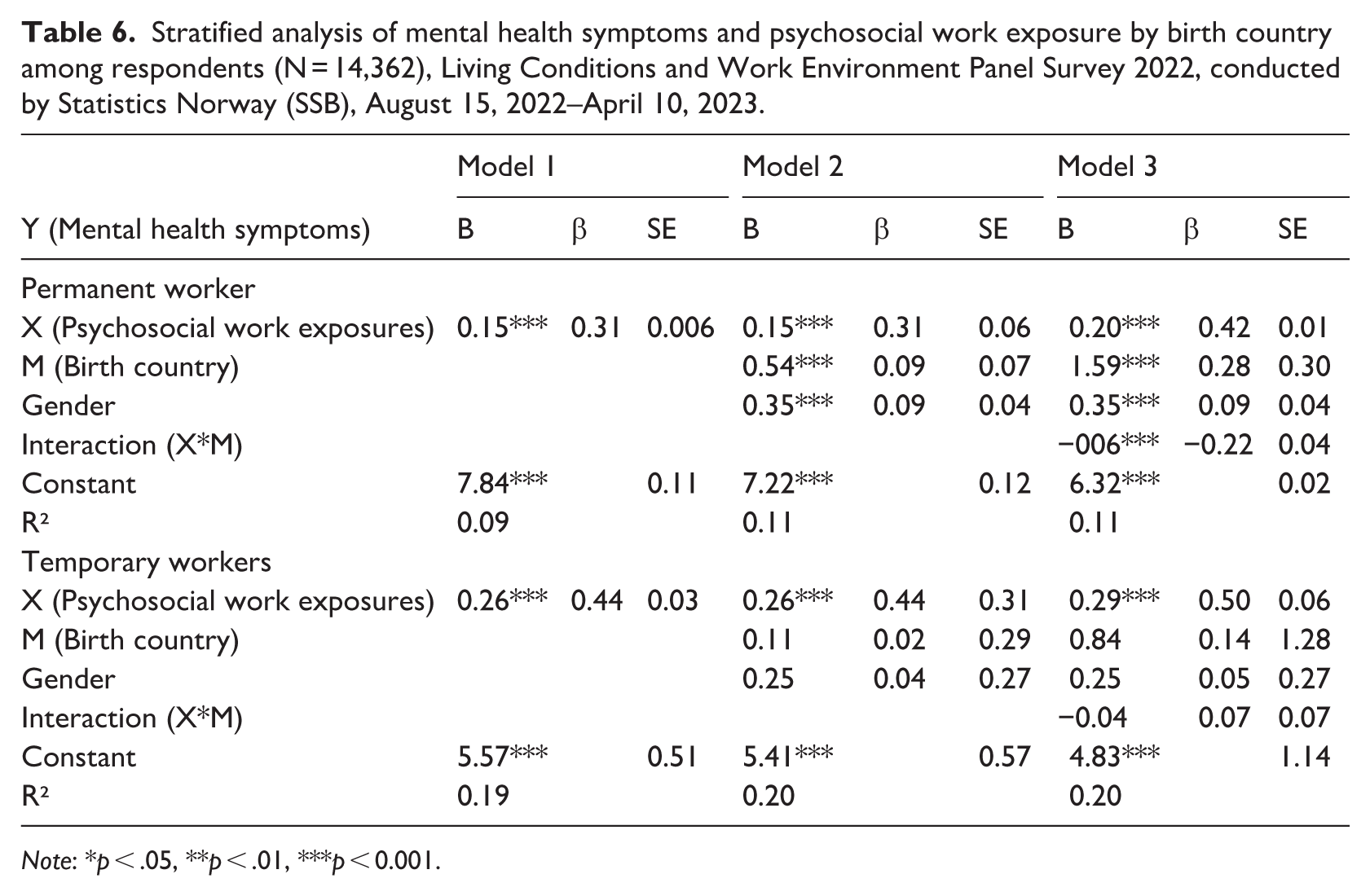
Note: *p < .05, **p < .01, ***p < 0.001.
Discussion
This study examined how exposure to mechanical and psychosocial work hazards is associated with musculoskeletal and mental health symptoms among workers in Norway, and whether these associations differ between Norwegian and non-Norwegian workers. Our results indicate that occupational exposures are important determinants of health and that immigrant workers carry a disproportionate share of work-related risks and outcomes. This study’s results support the hypotheses that higher levels of mechanical and psychosocial work hazards are linked to poorer health outcomes (H1 and H2). Across the full sample, greater exposure to mechanical work hazards was significantly associated with more musculoskeletal symptoms, even after adjusting for age, gender, and psychosocial work exposures. Likewise, higher psychosocial work exposures were associated with more mental health symptoms. These findings are consistent with earlier studies showing that repetitive movements, awkward postures, and heavy physical work increase the risk of musculoskeletal disorders (Farioli et al., 2014; Govaerts et al., 2021; Madsen et al., 2018), while high job demands, role conflict, and emotional strain are linked to anxiety, depression, and sleep problems (Havermans et al., 2018; Plaisier et al., 2007; Virtanen et al., 2007).
Furthermore, the descriptive results show that non-Norwegian workers have lower mean scores on indices of mechanical work exposures and health outcomes than Norwegian workers, indicating greater exposure and worse health, as lower scores indicate greater exposure and more symptoms. Non-Norwegians reported more mechanical hazards, more musculoskeletal complaints, and poorer mental health. This pattern aligns with the broader literature, which documents that migrant workers are more likely to be concentrated in physically demanding jobs and to experience adverse occupational health outcomes (Hargreaves et al., 2019; Moyce and Schenker, 2018; Sterud et al., 2018).
The moderation models indicate that birth country plays a crucial role in shaping the health impact of work hazards. For musculoskeletal health, the interaction between mechanical work hazards and birth country was statistically significant, demonstrating that mechanical exposures are more strongly associated with musculoskeletal symptoms among non-Norwegian workers than among Norwegian workers. After controlling for age, gender, and psychosocial exposures, each unit increase in mechanical hazards was linked to a steeper increase in musculoskeletal symptoms for immigrants, confirming H1a. A similar pattern was observed for mental health. Psychosocial work exposures were linked to more mental health symptoms overall, but the significant interaction term indicated that non-Norwegian workers experience a stronger deterioration in mental health in response to psychosocial stressors than Norwegian workers, supporting H2b. These results are consistent with ‘othering theory’, which emphasizes how discrimination, marginalization, and perceived outsider status can intensify the mental health consequences of workplace stress (Elshahat et al., 2022; Grove and Zwi, 2006; Viruell-Fuentes, 2007).
Our findings suggest that migrant workers experience ‘othering’ as a structural condition of their employment rather than as isolated individual experiences. Norwegian labor regulations emphasize equality, participation, and a safe working environment for all; everyday practices and informal norms in workplaces often position migrants at the margins by treating Norwegian language skills, cultural codes, and social networks as the implicit standard for desirable jobs, advancement, and being heard (Andersson and Rye, 2023). This contributes to migrants being disproportionately channeled into more hazardous, lower-status, and often temporary positions, with less autonomy over work organization and fewer opportunities to raise concerns about risk or unfair treatment (Andersson and Rye, 2023), effectively marking them as ‘outsiders’ in the Norwegian workplace. Our empirical results reflect this process of othering through both exposure and outcome variables: non-Norwegian workers are more frequently exposed to mechanical work hazards and adverse psychosocial work exposures, and the associations between these exposures and musculoskeletal symptoms and mental health symptoms are stronger for migrants than for Norwegian workers, particularly among those in temporary employment. In other words, migrant workers not only encounter more physically and psychosocially demanding working conditions, but these conditions more directly translate into musculoskeletal and mental health problems. These patterns suggest that othering in the Norwegian work context is not only a social or symbolic experience of exclusion but also materially rooted in unequal distributions of mechanical and psychosocial work hazards and in the disproportionate burden of musculoskeletal and mental health symptoms borne by migrant workers.
We further conducted stratified sensitivity analyses by employment type (permanent vs. temporary) to provide additional insight into how labor-market position interacts with birth country. This shows that among permanent workers, mechanical hazards were significantly associated with musculoskeletal symptoms, but the interaction with birth country was not statistically significant. Among temporary workers, however, mechanical hazards were more strongly related to musculoskeletal symptoms, and the interaction term indicated that this relationship was particularly pronounced among non-Norwegian temporary workers. This suggests that precarious employment amplifies the physical health risks associated with mechanical exposures, especially for immigrants, echoing research on the vulnerability of migrant workers in insecure, labor-intensive jobs (Mondragón, 2011; Ronda Pérez et al., 2012). For mental health, psychosocial work exposures were significantly associated with mental health symptoms in both permanent and temporary employment groups. The coefficients were higher among temporary workers, indicating that psychosocial hazards are especially consequential in precarious jobs. In the permanent worker group, the interaction between psychosocial exposures and birth country remained significant, whereas it was not among temporary workers. One interpretation is that permanent immigrant workers, who are embedded more deeply within organizational structures, may accumulate psychosocial strain related to organizational injustice, limited career opportunities, and everyday microaggressions (Elovainio et al., 2004; Shenoy-Packer, 2014). For temporary workers, the general insecurity and instability of contract work may produce such high levels of stress that differences by birth country become less visible.
The overall pattern of findings from the most recent survey data aligns well with ‘othering theory’. Immigrant workers’ concentration in physically demanding, low-status, and often temporary jobs, combined with limited control over working conditions and fewer opportunities to influence decisions, reflects structural processes that categorize them as ‘others’ in the labor market (Johnson et al., 2004; Reidpath and Allotey, 2019). The stronger health impact of mechanical and psychosocial exposures among non-Norwegians suggests that these workers not only encounter hazards more frequently but also have fewer material and social resources – such as job security, social support, and institutional protection – to buffer their effects (Hossin, 2020; Tallarek et al., 2020). Over time, this may erode the ‘healthy immigrant effect’ and contribute to the higher levels of musculoskeletal and mental health symptoms observed in this study (Elshahat et al., 2022; Markides and Rote, 2018).
A key strength of this study is the use of national-level panel survey data, which includes a wide range of occupations across Norway and enables a robust analysis of the causal relationships between occupational health hazards and health outcomes. However, studying is not without limitations. One notable limitation is that the Living Conditions and Work Environment Panel Survey is cross-sectional, making it difficult to establish the temporal order of the causal association between migrants’ status and occupational health outcomes.
Conclusion
This study highlights that the Norwegian workplace is not as equitable as expected, with migrants being disproportionately exposed to both mechanical and psychosocial work hazards. Migrant workers are more frequently engaged in physically demanding tasks, such as neck flexion, forward bending, squatting/kneeling, and awkward lifting, than their Norwegian counterparts. In addition, migrants face greater exposure to heavy physical work and prolonged standing or walking. Similarly, immigrants are more vulnerable to psychosocial work hazards, such as receiving conflicting demands from different individuals and being tasked with work without adequate resources. The findings reveal a significant disparity in work-related mental health outcomes, with immigrants showing greater susceptibility to mental health problems compared with native workers. In conclusion, the study underscores the urgent need for more inclusive occupational health and safety policies in Norway, particularly those that address the unique challenges faced by migrant workers. Despite Norway’s reputation as an egalitarian society, the findings suggest that more effort is needed to ensure fair and equal treatment for all workers, regardless of their immigration status.
Footnotes
Ethical considerations
Approval to use the Living Conditions and Work Environment Panel Survey 2022 was obtained from Statistics Norway (SSB) on November 6, 2025, under Approval Order No. 3668.
Author contributions
Nabaraj Adhikari contributed to the study’s conception and design and to the acquisition, analysis, or interpretation of data. Nabaraj Adhikari wrote the first draft of the manuscript, and Shahad Uddin contributed to the critical review of its intellectual content.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the student grant in Sustainability and Health (SHE; Center for Sustainable Healthcare Education), University of Oslo.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
The data are publicly available from the Norwegian Agency for Shared Services in Education and Research (Sikt) on request.
Statement on AI
The Grammarly AI tool was used to correct grammatical errors in the manuscript across all sections.
