Abstract
Background:
The long history of the Palestinian-Israeli conflict has resulted in a public and mental health crisis. Despite the significant mental health burdens facing the Palestinian population in the Occupied Palestinian Territories (OPT) and refugee camps, this issue remains comprehensively unexplored.
Aims:
This scoping review identified mental health interventions and assessed their effectiveness among populations in the OPT and Palestinian refugee camps, while addressing delivery challenges.
Method:
A scoping review was conducted using 14 databases to include relevant studies published through March 2024 using PRISMA guidelines for scoping reviews.
Results:
Analyzing 31 intervention studies meeting the inclusion/exclusion criteria, revealed varied outcomes in interventions targeting post-traumatic stress disorder, depression, and overall mental well-being.
Conclusions:
While some interventions showed potential, others had limited effectiveness, underscoring the complexity of mental health needs in conflict zones. Gender- and risk-specific effectiveness was observed, emphasizing the need for tailored approaches. Challenges like low attendance rates and systemic barriers hindered intervention success. The profound impact of war on children stresses the urgency for targeted interventions. Empowerment and community connectedness are vital for resilience, along with the importance of family and community involvement and research that balances the need for strong evaluation designs with the need for ongoing mental health services. Advocacy for systemic changes is crucial to implement the complex sustainable interventions necessary to assure mental health in any population. This review highlights the importance of holistic, contextually relevant approaches for mental health intervention in OPT and refugee camps, emphasizing rigorous evaluations and community-driven approaches.
Introduction
The long history of the Palestinian-Israeli conflict has created and precipitated a pronounced public health and mental health crisis, exposing Palestinians to pervasive instability, insecurity, and deprivation (Jamal et al., 2022; Qato, 2020; Sarraj & Qouta, 2004). The persistent conflict between the two countries has subjected Palestinians to a litany of adversities including displacement from their homes, the loss of family members and kin, destruction of infrastructure, complete breakdown of basic needs, fragmentation of health services, and the overpowering disruption of any life amenities (World Health Organization Regional Office for the Eastern Mediterranean, 2024a). These dramatic successive upheavals have profoundly impacted the mental well-being across various demographic strata of Palestinian populace manifesting in heightened prevalence rates of mental health disorders (World Bank, 2022). A spectrum of psychological issue such as post-traumatic stress disorders (PTSD), anxiety, and stress have been documented (Bdier et al., 2023; Wagner et al., 2020), with PTSD exhibiting a particularly elevated incidence (World Health Organization Regional Office for the Eastern Mediterranean, 2024c).
The World Health Organization (WHO) in its comprehensive review of conflict-induced mental health dynamics across 39 nations, has underscored a heightened susceptibility to mental health afflictions among conflict-exposed populations, revealing that one in five individuals may suffer from depression, anxiety, PTSD, bipolar disorder, or schizophrenia (World Health Organization, 2022). A systematic review by Dimitry (2012) on the mental health of children in areas of armed conflict in the Middle East reveals the profound impact of exposure to traumatic events on the mental and behavioral well-being of adolescents. Similarly, Sullivan and Simonson (2016) underscore the high prevalence of mental health issues among these populations, with a particular emphasis on school-based interventions. Thompson et al. (2018) and Tyrer and Fazel (2014) both explore the efficacy of psychological interventions, with Thompson specifically delving into the treatment of PTSD. van Wyk and Schweitzer (2014) and Tribe et al. (2019) both emphasize the necessity for more rigorous research methods and recognize the potential benefits of narrative exposure therapy. While Williams and Thompson (2011) highlight the effectiveness of community-based interventions, Vossoughi et al. (2018) advocates for further research in this area.
Despite struggling with significant mental health burdens that place the Palestinian population in the Occupied Palestinian Territories (OPT) and refugee camps among the most vulnerable globally, the issue remains largely unaddressed (World Bank, 2022). The WHO has identified the imperative of addressing the mental health needs of Palestinians in OPT and refugee camps as a paramount public health concern (World Health Organization Regional Office for the Eastern Mediterranean, 2024a, 2024c). This imperative has been supported by the development of national mental health policy by the Ministry of Health in Palestine, prioritizing the integration of mental health services into primary and secondary health care settings, and transitioning away from a reliance on hospital-based management (Giacaman et al., 2011). However, the provision of mental health services contends with overwhelming demands for such services coupled with deficits in trained personnel and financial resources (Marie et al., 2016). WHO has begun to address the gap and facilitated the training of non-specialist health workers to help in supporting people with mental disorders (World Health Organization Regional Office for the Eastern Mediterranean, 2024c) The WHO has also assumed a pivotal role in advocating for and bolstering the development of interventions tailored to community mental health services (Abo-Rass & Abu-Kaf, 2023; Abo-Rass et al., 2023; Al-Krenawi et al., 2004; Ben-Zeev et al., 2017; Giacaman et al., 2011; Marie et al., 2016, 2020; Shawahin & Çiftçi, 2012; Tsacoyianis, 2021).
Other studies have highlighted the significant mental health needs of Palestinians, particularly in the OPT, due to the impact of political violence, displacement, and limited resources (Ben-Zeev et al., 2017; Giacaman et al., 2011; Marie et al., 2016). These studies have emphasized the potential of mental health interventions, such as smartphone applications and web-based interventions, to address these needs (Ben-Zeev et al., 2017). However, they have underscored the necessity of increasing the availability and quality of mental health care, as well as the need for a sustainable system of public mental health services (Giacaman et al., 2011; Marie et al., 2016). The challenges and opportunities in the community mental health field for Palestinians have also been explored (Tsacoyianis, 2021). Despite these efforts, the complex barriers to improving the quality of life for patients with schizophrenia in Palestine and the fragmented mental health system remain a significant concern (Marie et al., 2020).
Despite efforts to integrate mental health services into primary and secondary healthcare settings, challenges persist due to an overload of demands coupled with deficits in trained personnel and a dearth of pharmacological and financial resources. This context underscores the urgent need for effective interventions to support mental health for Palestinian people in the OPT and surrounding Palestinian refugee camps. Yet a comprehensive evaluation of such interventions remains lacking.
Aim
This scoping review aims to examine the effectiveness of existing interventions, contributing to the enhancement of mental health outcomes for Palestinians living in conflict-affected areas.
Methods
Literature search
A scoping review of the literature was conducted using 14 databases, employing the PRISMA Extension for Scoping Reviews (Tricco et al., 2018; Figure 1). These databases were selected for their medical and biomedical focus and rigorous standards. A combination of search terms and phrases (Table 1) was employed. The comprehensive electronic search aimed to identify all available studies on mental health intervention conducted within the OPT and among Palestinian refugees. Inclusion and exclusion criteria were structured around the ‘Population, Intervention, Control, Outcome’ (PICO) framework (Table 2). Additionally, reference lists from retrieved studies underwent manual searches to identify any additional relevant publications. All retrieved articles were screened against eligibility criteria to endure relevance to the topic and the objectives of this review. Given the nature of this review, no ethical oversight or approval was deemed unnecessary and therefore not acquired.
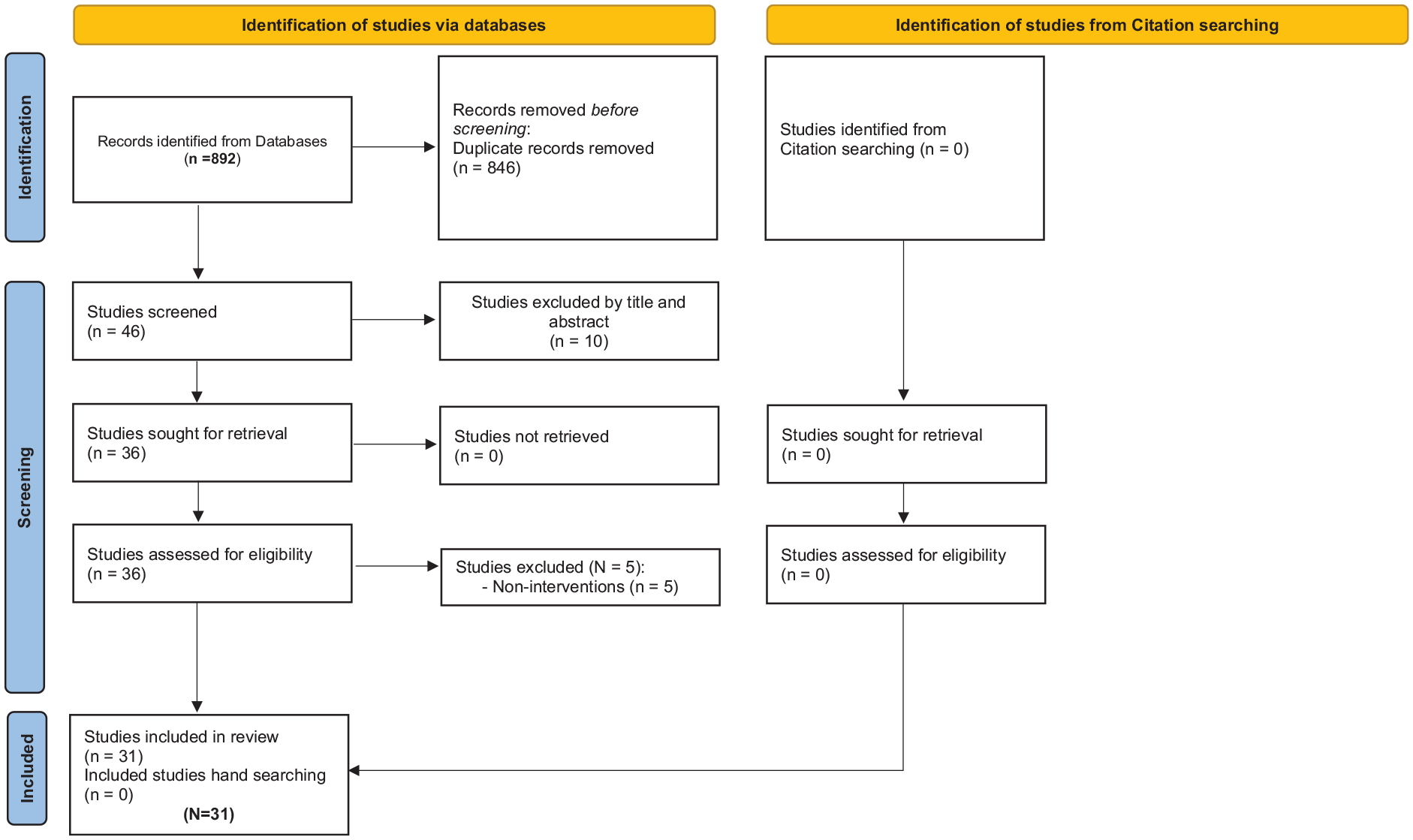
Flow diagram.
Electronic databases used with relevant search period and terms.
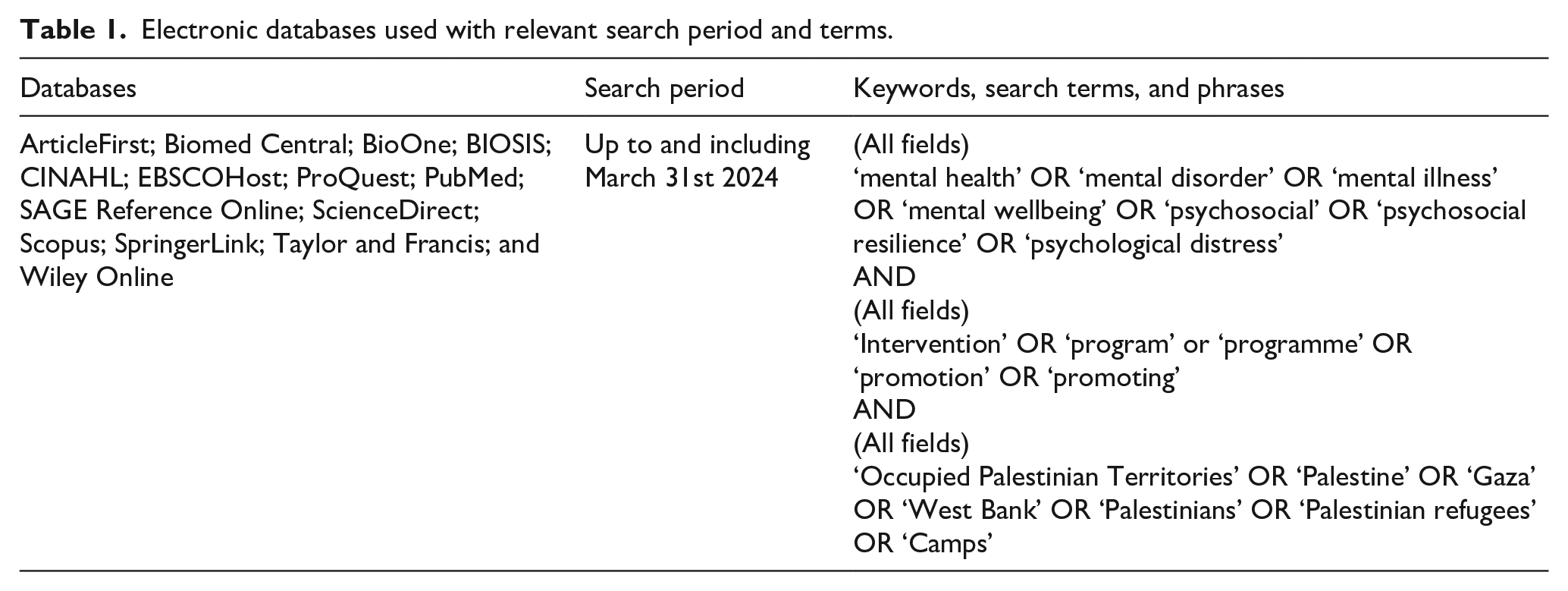

Criteria for inclusion and exclusion of studies.
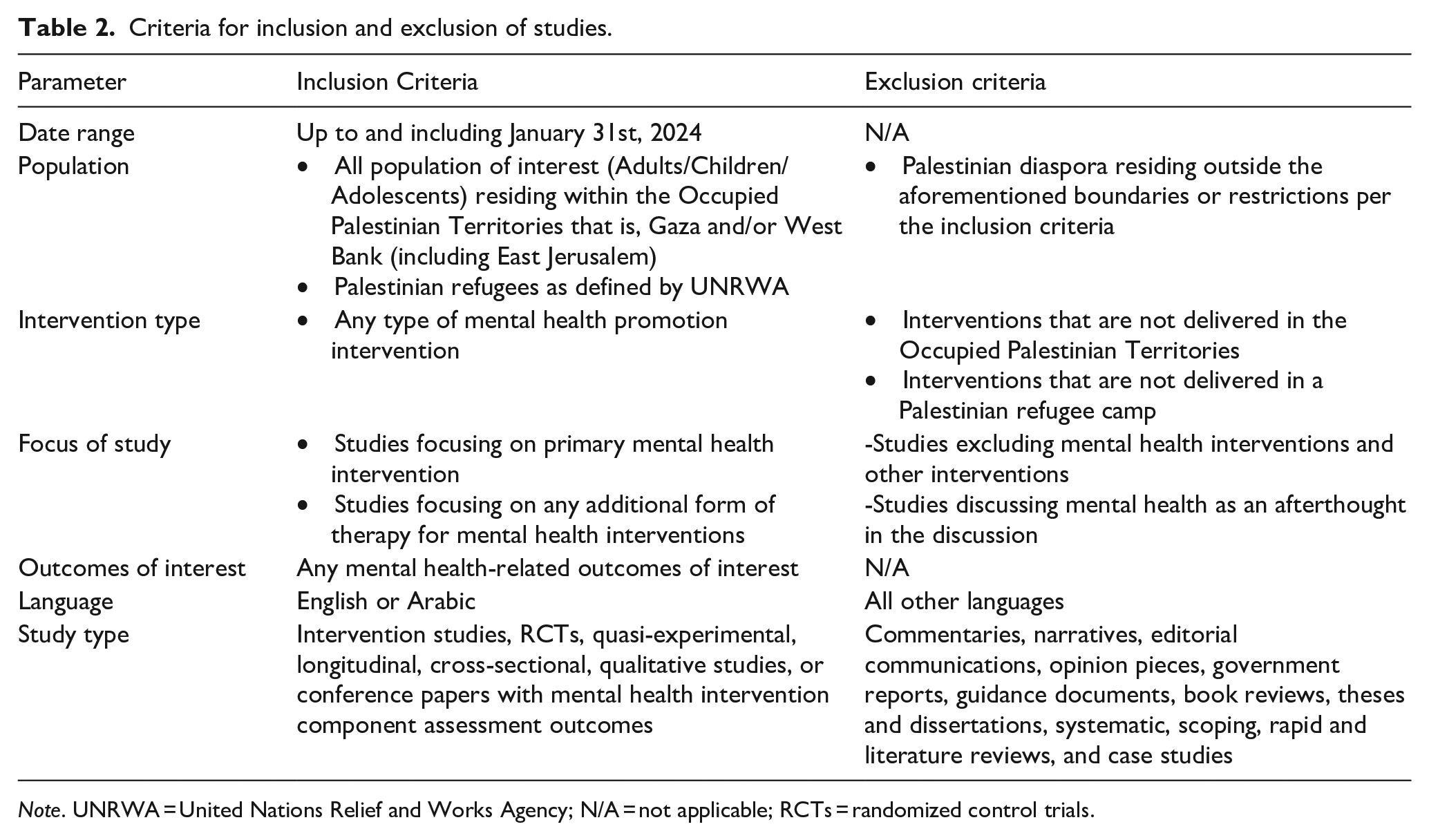
Note. UNRWA = United Nations Relief and Works Agency; N/A = not applicable; RCTs = randomized control trials.
Eligibility criteria
The search was restricted to studies published in the English or Arabic languages in peer-reviewed journals. The search was conducted in Spring 2024 and the results encompassed literature published up to and including March 2024. Only articles focusing on mental health intervention were considered, involving the application of mental health-based interventions, promotions, or program either as the primary intervention or as a part of a multi-behavioral intervention. Protocol studies were also included in the review. Excluded from consideration were publications in other than English or Arabic, brief communications, grey literature, qualitative studies, and interventions reported outside of traditional peer-reviewed articles (Table 2).
Study selection and data extraction
BAE, WAR, and PK conducted the literature search independently and collaborated to select studies for inclusion in the scoping review. The search strategy was adjusted to align with the indexing systems of each respective database. Rayyan QCRI software (Ouzzani et al., 2016) facilitated the screening process and study selection. Titles and abstracts underwent initial screening for relevancy, followed by a thorough review of potentially relevant journal abstracts by HB, FA, BAE, and WAR. Each author independently evaluated potential studies for relevance and adherence to inclusion/exclusion criteria (refer to Table 2). Any discrepancies in selection were discussed to reach a consensus, with FA, BAE, and WAR resolving discrepancies if necessary. All selected articles were subsequently reviewed with the primary author before a final decision on inclusion was made (refer to Figure 1). Once the list of selected studies was finalized, BAE, WAR, and PK extracted the relevant data, which was cross-checked by FA, BAE, and WAR. Data extracted for each study included author, date, target population, country, study type, sample size, intervention details, measured parameters, main results, and recommendations (refer to Table 3). Any discrepancies in extracted data were resolved through discussion to reach a consensus and tabulated accordingly. Given that methodological quality assessment is not obligatory for scoping reviews, the included studies were not appraised (Peters et al., 2020).
Summary of findings (N = 31).
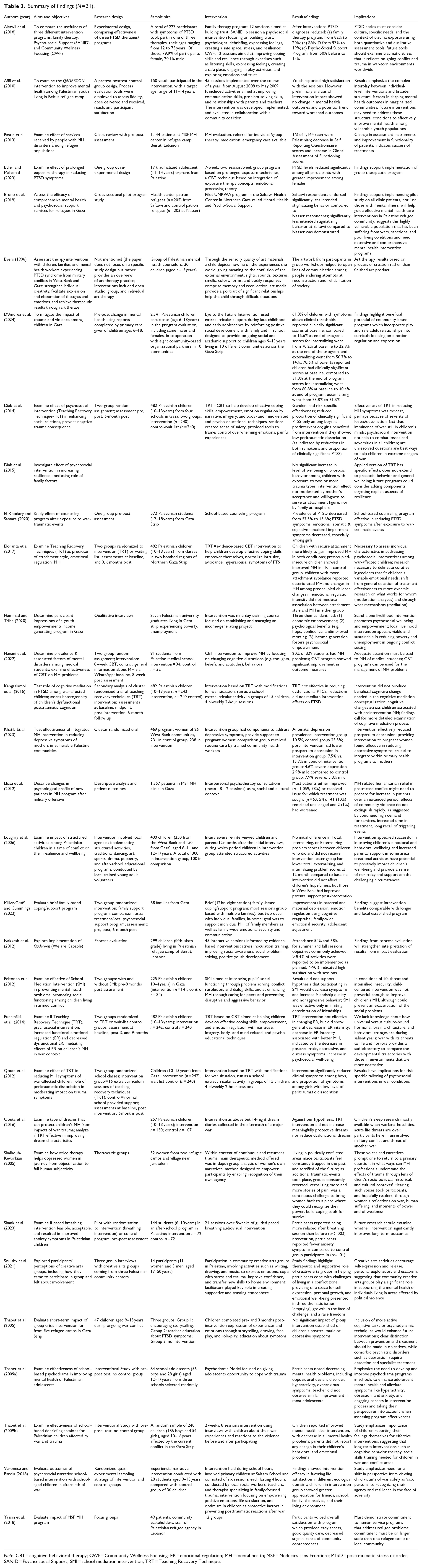
Note. CBT = cognitive-behavioral therapy; CWF = Community Wellness Focusing; ER = emotional regulation; MH = mental health; MSF = Medecins sans Frontiere; PTSD = posttraumatic stress disorder; SANID = Psycho-social Support; SMI = school mediation intervention; TRT = Teaching Recovery Technique.
Results
Thirty-one articles were identified. While all had Palestinians as their population, three were conducted with samples of Palestinian refugees in Lebanon (Bastin et al., 2013; Nakkash et al., 2012; Yassin et al., 2018). Twenty one studies focused on adolescents and children in the OPT (Afifi et al., 2010; Altawil et al., 2018; Bdier & Mahamid, 2023; Byers, 1996; D’Andrea et al., 2024; Diab et al., 2014, 2015; El-Khodary & Samara, 2020; Eloranta et al., 2017; Kangaslampi et al., 2016; Loughry et al., 2006; Nakkash et al., 2012; Peltonen et al., 2012; Punamäki et al., 2014; Qouta et al., 2012, 2016; Shank et al., 2023; Thabet et al., 2005, 2009a, 2009b; Veronese & Barola, 2018) and two on adults in primary care settings (Bruno et al., 2019; Llosa et al., 2012). Twelve were school-based or conducted with samples of either school or university students (Diab et al., 2014, 2015; El-Khodary & Samara, 2020; Eloranta et al., 2017; Hammad & Tribe, 2020; Hanani et al., 2022; Kangaslampi et al., 2016; Peltonen et al., 2012; Qouta et al., 2012, 2016; Shank et al., 2023; Thabet et al., 2009a, 2009b; Veronese & Barola, 2018) and two focused on university students or graduates (Hammad & Tribe, 2020; Hanani et al., 2022). Three were conducted with patients at mental health clinics (Bastin et al., 2013; Llosa et al., 2012; Yassin et al., 2018). Two studies worked exclusively with women (Bruno et al., 2019; Llosa et al., 2012) and two with families (Altawil et al., 2018; Miller-Graff & Cummings, 2022).
The research methods employed in the identified studies varied, ranging from qualitative assessments (Hammad & Tribe, 2020; Shalhoub-Kevorkian, 2005) to chart reviews (Bastin et al., 2013; Llosa et al., 2012) and process evaluations (Nakkash et al., 2012) to one-group interventions with pre-post assessments (Bdier & Mahamid, 2023; El-Khodary & Samara, 2020). Twelve of the articles described research methods that used two randomized groups or clusters with pre-post assessment (Diab et al., 2014, 2015; Eloranta et al., 2017; Hanani et al., 2022; Kangaslampi et al., 2016; Miller-Graff & Cummings, 2022; Peltonen et al., 2012; Punamäki et al., 2014; Qouta et al., 2012, 2016; Shank et al., 2023; Yassin et al., 2018). All studies except one (Shank et al., 2023) aimed to assess long-term outcomes, conducing post intervention assessments at some point distant from the end of the intervention. Cognitive behavioral therapy (CBT) and teaching recovery techniques emerged as the most prevalent approaches (Bdier & Mahamid, 2023; Diab et al., 2014, 2015; Eloranta et al., 2017; Hanani et al., 2022; Kangaslampi et al., 2016; Punamäki et al., 2014; Qouta et al., 2012, 2016), encompassing regular CBT applications, Prolonged Exposure Techniques, and Teaching Recovery Techniques. Beyond CBT, the studies explored a variety of other intervention strategies, including economic empowerment (Hammad & Tribe, 2020), community-based participatory research methods within an ecological framework (Altawil et al., 2018; Nakkash et al., 2012), family-based coping/support programs (Miller-Graff & Cummings, 2022), and school mediation interventions (Peltonen et al., 2012). Additionally, school-based counseling programs were developed by the Ministry of Education in the Gaza Strip to address mental health needs (El-Khodary & Samara, 2020), along with paced breathing interventions (Shank et al., 2023), voice therapy for oppressed women (Shalhoub-Kevorkian, 2005), traditional counseling or psychotherapy (Bastin et al., 2013; Llosa et al., 2012; Yassin et al., 2018), art therapy and creative activities (Byers, 1996; Soulsby et al., 2021), experiential narrative intervention (Veronese & Barola, 2018), and group crisis and psychodrama (Thabet et al., 2005, 2009b).
The results of the interventions investigated across the 31 articles revealed diverse and nuanced outcomes. Bdier and Mahamid (2023) demonstrated a reduction in PTSD symptoms through prolonged exposure therapy, a CBT technique. Byers (1996) art therapy intervention facilitated communication among individuals navigating the challenges of reconstructing and rehabilitating their society. Similarly, Loughry et al. (2006) highlighted the therapeutic role of creative arts groups in fostering self-expression, personal growth, and emotional well-being. The work of D’Andrea et al. (2024) showed improvements in children’s and parents’ symptoms, moving from an initial 61.3% of children and 78.6% of parents with clinically significant problematic total scores, to 15.6% and 31.3%, respectively, by the program’s end. Internalizing symptoms decreased from 70.2% to 22.9% for children and from 80.8% to 40.4% for parents. Externalizing symptoms also decreased from 50.7% to 14% for children and from 73.8% to 31.3% for parents. Khatib et al. (2023) found antenatal depression decreased reduced post-intervention when comparing intervention and control groups (7.5% vs. 13.7%). Hanani et al. (2022) observed significant improvement in mental health problems among medical students following a CBT program. Miller-Graff and Cummings (2022) reported enhancement in depression, emotion regulation, and family-wide emotional security through a family-based support program and Shank et al. (2023) illustrated that paced breathing interventions reduced anxiety symptoms in Palestinian children. Traditional counseling and psychotherapy were explored by Bastin et al. (2013) and Llosa et al. (2012), revealing improvements in psychological profiles and functioning scores. Nakkash et al. (2012) underscored the success of community-based participatory methods in achieving high satisfaction and objectives. Punamäki et al. (2014) noted a general decrease in emotional regulation intensity, associated with better mental health outcomes. Shalhoub-Kevorkian (2005) found that voice therapy empowered oppressed women by acknowledging their agency and Thabet et al. (2009b) results showed that there was statistically significant decrease in total scores of child mental health problems and hyperactivity symptoms after psychodrama program. Yassin et al. (2018) reported overall satisfaction with a mental health program that offered accessible, quality care, decreasing stigma, and enhancing community connectedness. Hammad and Tribe (2020) evaluated an income generating program in the Gaza Strip, identifying benefits such as economic empowerment, psychological well-being including hope and confidence, and psychosocial empowerment.
Some of the studies described more nuanced results, with minor pre-post changes or changes observed only among specific subgroups. For example, Diab et al. (2014) and El-Khodary and Samara (2020) identified gender- and risk-specific effectiveness in their interventions, particularly observing reduced PTSD symptoms in girls. In Loughry et al. (2006) children in the intervention group displayed lower externalizing and internalizing mental health problem scores at follow-up (Time 2) compared to baseline (Time 1). However, while this intervention did not affect children’s hopefulness, those in the West Bank reported improved parental support post intervention. Similarly, both studies by Thabet et al. (2009a, 2009b) showed improvements in children’s mental health following interventions, with reductions in various mental health problems such as oppositional deviant disorder, hyperactivity, and overanxious symptoms. However, teachers did not consistently observe similar improvements in adolescents. Additionally, while children reported improved mental health after the intervention, parents did not report any change in their children’s behavioral and emotional problems.
On the other hand, some studies did not substantiate their main hypotheses or found the interventions not to be effective. For example, Eloranta et al. (2017) explored the role of attachment style in the effectiveness of teaching recovery techniques but did not observe the expected outcomes. Peltonen et al. (2012) assessed the School Mediation Intervention but found the program to be only marginally effective in preventing the deterioration of friendships rather than improving mental health outcomes. Qouta et al. (2016) scrutinized the impact of teaching recovery techniques on dream characteristics and found no significant change, challenging the initial hypothesis. Kangaslampi et al. (2016), who examined the role of cognitive mediation in PTSD among war-affected children, characterized the heterogeneity of children’s dysfunctional posttraumatic cognition and found that the intervention did not effectively reduce such cognition, and that reductions did not mediate intervention effects on posttraumatic stress symptoms. Additionally, Diab et al. (2015) investigated the effect of a psychosocial intervention on increasing resilience and the mediating role of family factors, but found no significant improvements in well-being or prosocial behavior among highly traumatized children.
Discussion
This scoping review synthesized findings from 31 studies aimed to exploring the effect of mental health interventions among Palestinian in the OPT and refugee communities. The review also identified challenges to delivering effective mental health services in the context of armed conflict, war, or adverse social conditions. While several interventions showed promising outcomes, particularly in reducing PTSD symptoms, improving mental health among medical students, and empowering marginalized groups such as children and women, there were also instances where interventions did not yield significant improvements or had limited effectiveness.
The results across the adult population studies uniformly demonstrated positive outcomes, indicating the effectiveness of interventions in reducing or improving mental health-related issues, such as depression, emotional regulation, and overall psychological well-being.
Conversely, the results focused on samples of children were more varied, with the majority of studies showing limited to no improvement with the interventions. The studies with children that did stand out for their positive outcomes shed light on potential avenues for success (Bdier & Mahamid, 2023; Khatib et al., 2023; Loughry et al., 2006; Nakkash et al., 2012; Shank et al., 2023). However, challenges such as low attendance rates and lack of parental support underscore the complexities of implementing interventions for children in conflict-affected regions (Nakkash et al., 2012). The prevalence of PTSD, depression, and anxiety among Palestinian youth in the Gaza strip underscores the urgent need for effective interventions tailored to their unique circumstances. The impact of such trauma and adversity on the developing minds and personalities of children and adolescents is profound, with mental health issues escalating among individuals in these territories. Despite this imperative and the efforts to address these challenges, questions remain regarding the most effective strategies for supporting children in extreme war-related dangers (Diab et al., 2014). There remains a dearth of evidence guiding prevention and management strategies for mental health issues, particularly within the complex ecological, political, and societal contexts of the OPT.
One notable finding is the gender- and risk-specific effectiveness observed in some interventions, such as the reduction of PTSD symptoms among girls, underscoring the importance of considering group differences and contextual factors when designing and implementing mental health programs. The challenges encountered in studies where outcomes did not meet expectations suggest that factors such as cultural norms, socio-economic conditions, and the specific nature of trauma can influence the participation in and effectiveness of interventions. The heterogeneity of responses to interventions underscores the importance of tailoring approaches to the specific needs and circumstances of the target population. Additionally, the marginal effectiveness of certain interventions, such as the school mediation intervention, highlights the need for continuous evaluation and refinement of intervention strategies to ensure optimal outcomes.
Many of the interventions documented in the reviewed studies focused on individual-level interventions, reflecting the training and expertise of the researchers involved. Indeed, the concepts of empowerment and agency emphasized by Shalhoub-Kevorkian (2005) and the community connectedness reported by Yassin et al. (2018) underscore the critical role of mental health interventions in enhancing individual resilience and social cohesion. These aspects are pivotal for developing policies and programs that not only address mental health symptoms but also foster environments conducive to mental well-being.
However, the literature had a minimal focus on family and community-based approaches; neglecting the role of these structures in building resilience among children may overlook crucial support systems. Betancourt et al. (2013) advocates for a broader, ecological approach to addressing the needs of children affected by war, recognizing the interconnectedness of individual, family, and community well-being. Implementing such approaches in conflict zones like Gaza, where families face ongoing threats to their safety and basic needs, presents formidable challenges.
The success of community-based and family-support interventions highlighted by Miller-Graff and Cummings (2022) and Shank et al. (2023) also points to the critical role of community engagement and familial support in mental health promotion and intervention efforts. Their findings underscore the need for mental health practitioners to collaborate closely with local community leaders, organizations, and families to develop and implement culturally sensitive and contextually appropriate interventions.
Only a few studies have assessed multilevel or stepped-care packages, highlighting the need for a comprehensive mental health management approach that addresses individuals across various settings (Miller-Graff & Cummings, 2022; Shank et al., 2023). Commitment to human service programs that address refugee problems is crucial, necessitating efforts that extend beyond individual communities or refugee camps (Yassin et al., 2018). The nuanced findings of studies such as Diab et al. (2014) and El-Khodary and Samara (2020), alongside the challenges identified in studies such as Eloranta et al. (2017) and Peltonen et al. (2012) underscore the need for ongoing research to refine intervention strategies and understand the contexts under which they are most effective. The imperative to address post-traumatic stress disorder (PTSD) and other trauma-induced illnesses in culturally appropriate manners within marginalized communities necessitates a theoretical framework to develop comprehensive, effective, and sustainable solutions that comprehensively address and treat trauma on both collective and individual levels, distinct from Western medicine.
Additionally, insights from studies such as Bastin et al. (2013) and Llosa et al. (2012) regarding traditional counseling and psychotherapy highlight the importance of a balanced approach to mental health care that integrates both modern and traditional healing modalities. Mental health practitioners should acknowledge and respect the cultural beliefs, values, and practices of Palestinian communities, incorporating traditional healing methods alongside evidence-based interventions. This holistic approach can improve treatment engagement, enhance therapeutic rapport, and foster a sense of trust and mutual understanding between mental health providers and service users. Collectively, these implications underscore the necessity for holistic, contextually relevant approaches to mental health intervention in conflict-affected regions like Palestine. Efforts to address mental health needs in Palestine must be comprehensive, inclusive, and grounded in the principles of cultural humility, social justice, and human rights. By adopting a multidimensional approach that addresses clinical, community, and policy-level factors, stakeholders can work toward building resilient, thriving communities that prioritize mental health and well-being amidst ongoing conflict and adversity.
Facilitators to mental health interventions, such as culturally appropriate designs and caregiver involvement, are noted, yet systemic challenges, such as lack of political will and financial resources, persist. Advocacy for macro-level changes, including policy reforms and sustained humanitarian support, is crucial for addressing the complex mental health needs of conflict-affected populations (Yassin et al., 2018). The ongoing conflict between Palestine and Israel exacerbates trauma-related symptoms, further straining already limited resources and healthcare systems. As the demand for mental health services continues to rise, humanitarian relief efforts must adapt to the long-term impacts of community violence and prioritize sustainable interventions to meet the evolving needs of affected populations (Hanani et al., 2022; Llosa et al., 2012; Shalhoub-Kevorkian, 2005).
The ongoing Palestinian-Israeli conflict and the most current humanitarian crisis in Gaza has perpetuated a cycle of continuous and recurrent trauma, presenting significant challenges for implementing effective and sustainable mental health interventions in the region. The limited healthcare system capacity further exacerbates these challenges, as evidenced by the insufficient number of qualified healthcare workers and the strain on existing resources (Abudayya et al., 2023; Alduraidi et al., 2021; Jabr & Berger, 2024; Marie et al., 2016; Shukri et al., 2023; Vossoughi et al., 2018). Mental health-related humanitarian relief efforts in protracted conflict settings must anticipate a sustained increase in patients over an extended period, as the effects of community violence do not dissipate rapidly.
Overall, the evidence suggests that existing mental health interventions have the potential to alleviate mental health disorders, improve individual functionality, and enhance overall societal productivity. Despite the enduring conflict between Palestine and Israel, there is hope that targeted interventions can make meaningful strides toward improving the mental health and well-being of Palestinians living in the OPT. However, addressing the multifaceted challenges of mental health in conflict-affected regions requires ongoing research, collaboration, and a commitment to holistic, community-driven approaches.
Localized community-based mental health interventions tailored to local cultural and geopolitical contexts, like those in Palestine, offer more effective, sustainable, and adaptable solutions than broad-based Western approaches. Localized community-based interventions not only enhance access to care, reduce stigma, and promote long-term community resilience and well-being but also improve acceptance and increase the utilization of mental health services, leading to better health outcomes (Yudkin et al., 2022). By integrating mental health care into familiar community settings and utilizing culturally resonant practices, these interventions address major barriers such as mental health stigma, which often prevents individuals from seeking help. Tailoring interventions to fit the socio-cultural fabric of the community not only enhances s.
Community-based models in mental health care respect and leverage cultural nuances, thereby enhancing the sustainability of interventions. By fostering community ownership and ongoing local engagement, these models build on existing social structures and resources, which is crucial in regions with limited resources. Such an approach not only makes mental health care more accessible and less stigmatized but also promotes long-term resilience and well-being by empowering communities to take charge of their mental health needs.
Furthermore, the flexibility of community interventions allows them to adapt to changing circumstances and needs, a feature of immense value in conflict-affected areas like Palestine. The political and social landscape in such regions can change rapidly, and mental health programs need to be adaptable and responsive to remain effective (Hillel, 2023). Building mental health programs that are adaptable and can quickly respond to external conditions ensures that they continue to serve the community effectively, even as situations evolve.
The implications of the studies in this review are multifaceted, encompassing clinical practices, community interventions, and policy-level considerations. The evidence from studies such as Bdier and Mahamid (2023) and Hanani et al. (2022) reinforces the value of cognitive-behavioral therapy techniques in reducing PTSD symptoms and improving overall mental health, advocating for their integration into clinical practice. Similarly, the successes of community-based and family-support interventions highlighted by Shank et al. (2023) and Miller-Graff and Cummings (2022) underscore the importance of accessible, culturally sensitive approaches that engage community resources, and family systems in mental health care. These results underscore the importance of integrating evidence-based interventions like CBT into the standard repertoire of mental health care providers operating in conflict-affected regions. Clinicians and mental health professionals working in Palestine should receive training and support to effectively implement CBT techniques and tailor them to the unique cultural and contextual factors present in the region.
Despite the mixed findings in this review, it is essential to acknowledge the significance of conducting rigorous evaluations of mental health interventions in conflict-affected areas, particularly in OPT. These evaluations provide valuable insights into the strengths and limitations of different approaches, informing future program development and implementation. Moreover, they contribute to the growing body of evidence on effective strategies for promoting mental health and well-being in vulnerable populations.
However, the challenges inherent in conducting research and providing mental health services in conflict-affected areas, such as the OPT, cannot be understated. Limited resources, including trained staff, finances, and infrastructure, present significant barriers to delivering even basic medical care, let alone conducting and publishing studies. Study designs must take such limitations into account, while at the same time acknowledging the enormity of the problem. While scientific evidence is necessary for assuring that intervention content is effective, conducting randomized control trials with one arm receiving only monitoring cannot be ethically permitted. Alternatives such as testing different interventions against each other or sequential multiple assignments randomized trial (SMART) designs must be considered to assure that all participants receive attention (Lorenzoni et al., 2023). Attention should not be diverted from scaling up whatever mental health and psychosocial services might be available (World Health Organization Regional Office for the Eastern Mediterranean, 2024b), and indeed the available literature may not fully capture the scope of mental health services provided in the region. This balancing of research integrity with clinical needs will challenge even the most seasoned researchers.
Conclusion
The literature reviewed in this study presents a comprehensive overview of the mental health interventions implemented among Palestinian populations, particularly in the context of protracted conflict and occupation. The findings underscore the complex challenges faced by individuals, families, and communities in Palestine, as well as the resilience and resourcefulness demonstrated in the face of adversity. While some interventions showed promising results, particularly in adult populations, nuanced findings and mixed outcomes highlight the need for ongoing research, refinement of intervention strategies, and a holistic, contextually relevant approach to mental health care.
Moving forward, it is imperative to prioritize the integration of evidence-based practices, such as cognitive-behavioral therapy, into clinical settings while also recognizing the importance of community-based and family-support interventions in promoting mental health and resilience. Additionally, efforts to address mental health needs in Palestine must be guided by principles of cultural humility, social justice, and human rights, ensuring that interventions are sensitive to the unique cultural, social, and political context of the region. Moreover, the findings underscore the urgent need for increased investment in mental health services, capacity-building initiatives, and policy reforms to address the systemic barriers to mental health care access and delivery in Palestine. By fostering collaboration among stakeholders, including local communities, policymakers, and international organizations, it is possible to create a more inclusive, equitable, and effective mental healthcare system to co-design and implement culturally responsive interventions that meet the diverse needs of Palestinian populations. Additionally, efforts to strengthen mental health systems and build local capacity for delivering evidence-based interventions will be crucial in promoting long-term mental health resilience in conflict-affected contexts. Ultimately, addressing mental health challenges in Palestine requires a multifaceted approach that encompasses clinical, community, and policy-level interventions. By prioritizing the well-being of individuals, families, and communities, stakeholders can work toward building a more resilient and thriving society, even amidst ongoing conflict and adversity. In conclusion, adopting community-based models in mental health care offers a robust solution that is both culturally appropriate and sustainable, particularly in complex settings like Palestine. These models provide a framework for addressing immediate mental health needs while also building long-term capacity within the community to manage and overcome mental health challenges. A focused investment in strengthening and rigorously evaluating such models is essential for achieving lasting impacts in global mental health, ensuring interventions are not only effective in the short term but also sustainable and resilient in the face of future challenges.
Footnotes
Acknowledgements
None.
Author contributions
BAE conceptualized the study and BAE, WAR, and FA contributed to the study design. HMB and DA carried out data preparation and FA, HMB, DA, and WAR did the data analysis. BAE, FA, HMB, DA, PJK, and WAR wrote the first draft and all authors contributed to interpretation of findings and review and editing of the manuscript. BAE had final responsibility for the decision to submit the manuscript.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Compliance with ethical standards
Given the nature of this review, no ethical oversight was found to be necessary and, therefore, no institutional review board was acquired.
