Abstract
Background:
Whole-school approaches (WSAs) to mental health aim to promote collaborative, system-wide action by school communities to reduce stigma, raise awareness and embed mental health as ‘everyone’s business’. Although investment in such approaches has increased in England, implementation remains challenging due to variation in interpretation and the complexity of engaging diverse stakeholders.
Objectives:
The NHS Trailblazer programme introduced Mental Health Support Teams in schools to enhance support for children and young people’s mental health. This exploratory qualitative study examined stakeholder perspectives on the factors influencing the successful implementation of WSAs to mental health, using the Trailblazer programme as a real-world exemplar.
Methods:
Interviews with senior practitioners (n = 19) and 12 focus groups with mental health practitioners, school staff, parents/carers and children and young people (n = 29) were conducted across four educational settings in three areas of the North East of England. Data were analysed thematically using the Framework Approach and mapped post hoc onto the COM-B (Capability, Opportunity, Motivation) model of behaviour and Theoretical Domains Framework (TDF) to inform policy and practice.
Results:
Using the COM-B model as the organising framework (with TDF domains mapped within each component): ‘Capability’ encompassed knowledge, skills and behaviour regulation; ‘Opportunity’ captured environmental context and resources and social influences and ‘Motivation’ included social/professional role and identity, beliefs about consequences, optimism/pessimism, emotions, goals, intentions and reinforcing behaviour.
Conclusions:
While WSAs to promote mental health in schools show promise, their success depends on sustained investment, professional development and clarity around implementation roles and expectations. This study contributes to the literature by providing real-world insights into the implementation of such approaches, extending understanding of how national policies can translate into local school practices.
Introduction
Mental health disorders in children and young people are rising (Deng et al., 2023), with 1 in 5 (20%) aged between 8 and 16 years in England having a probable disorder (NHS England, 2022) and half of adult disorders beginning in adolescence (Kessler et al., 2007). Growing risk factors and reduced stigma have increased strain on specialist services, making reactive approaches insufficient; preventive approaches can reduce symptoms and improve future outcomes (Neil and Christensen, 2009).
Schools are key settings for mental health education and promotion. Many children and young people spend much of their time in school, families can easily engage with schools and schools link to support services (Spencer et al., 2025). Schools can foster belonging, shared values and positive staff-student relationships, linking school climate to better academic, behavioural and psychosocial outcomes; however, not all schools do this consistently (Turan Bora and Akbaba Altun, 2025). Rather than interventions targeting individuals, there is emerging evidence that mental health programmes and interventions that consider the whole-school context are more effective in improving mental health outcomes (Goldberg et al., 2019). Whole-school approaches (WSAs) strengthen relational, social and emotional factors across school life by viewing mental health as ‘everyone’s business’ (Weare, 2013), by requiring partnership working between a range of stakeholders including senior leadership, teaching and non-teaching staff as well as parents/carers and the wider community (Critchley et al., 2018).
The 2017 Green Paper Transforming Children and Young People’s Mental Health Provision (UK Government, 2017) proposed enhancing mental health support for mild-to-moderate needs in schools. These proposals were implemented via a large-scale phased rollout of Mental Health Support Teams (MHSTs) and the training of Educational Mental Health Practitioners (EMHPs) to support children and young people’s mental health across England. MHSTs work with clusters of schools to deliver early intervention for mild-to-moderate mental health needs, train staff in mental health awareness and promote a WSA. EMHPs complete a 1-year postgraduate training programme covering cognitive-behavioural and systemic approaches, engagement with families and liaison with statutory services.
In 2019–20, the first wave of rollout established 25 Trailblazer sites, and subsequent waves expanded the programme (NHS England, 2019), working with education settings to support a WSA to mental health and wellbeing (Ellins et al., 2021). In the North East and North Cumbria (NENC), three Trailblazer sites (three areas participating in the pilot, encompassing multiple schools within different localities) were selected as pilots in April 2020. In the NENC, it is estimated that 50% of children are living in a household with an income below acceptable standards of living (Adjei et al., 2024), with 3.2% of school pupils having social, emotional and mental health (SEMH) needs (significantly higher than the England average) and hospital admissions for children and young people self-harm being the second highest in the country (Public Health England, 2021). Comparable initiatives internationally, such as ‘Positive Behavioral Interventions and Supports’ (Pinkelman and Horner, 2019) and frameworks like Advancing Comprehensive School Mental Health Systems (Hoover et al., 2019), have demonstrated the value of coordinated, multi-tiered models that integrate mental health promotion into school culture.
While there has been recent large-scale investment in WSAs, there remains a need for research to better understand the components necessary to achieve success (Goldberg et al., 2019). While numerous studies have explored school-based mental health frameworks internationally, limited evidence exists on how England’s nationally-funded Trailblazer programme operationalised WSAs in practice. Given the relatively new and complex definition of WSAs, we used the Trailblazer programme as a real-world case study with which to explore factors affecting WSA implementation in the NENC region, ensuring participants reflected on lived rather than hypothetical experiences, thereby addressing a critical evidence gap and potentially informing future larger-scale evaluation.
Methods
Study design
The study protocol (Spencer et al., 2022) for this study adhered to Consolidated Critera for Reporting Qualitative Research (COREQ) guidelines and guidelines for the publication of qualitative research studies (Tong et al., 2007). Qualitative research is recognised as enabling an in-depth analysis of socially situated experiences and can provide insight into behaviours or concepts that are not yet well understood, ensuring better-informed public health policy decision-making (Maher and Dertadian, 2018).
Recruitment and sample
To ensure relevance to real-world implementation challenges, three different NENC Trailblazer sites were chosen, each with an Index of Multiple Deprivation (IMD) score that were above the average (21.7) for England (Ministry of Housing Communities and Local Government, 2019): Site 1 (IMD = 22.1); Site 2 (IMD = 31.5) and Site 3 (IMD = 29.1). We worked closely with regional Trailblazer contacts and site-level gatekeepers (including school senior leaders, designated mental health leads and EMHPs) to recruit participating schools and colleges. A purposive sampling strategy was employed to ensure varied representation from within these education settings, with individual participants being invited to join the study via site-level gatekeepers, who disseminated study information through routine school communication channels. The researchers did not make direct contact with parents/carers or children and young people until consent or assent had been secured. Across the three geographical sites, four types of educational establishment were recruited in line with the main types of education settings included in the Trailblazer programme nationally, based on estimated average school sizes: a primary school; a secondary school; a further education college and a specialist school. Sample size for data collection was guided by the principle of information power, which posits that sample size should be guided by factors relevant to the study aims, the specificity of the research question asked, the quality of dialogue between participants and researchers and the researchers’ theoretical and analytical skills, with sampling continuing until further data collection was judged unlikely to yield new insights (Malterud et al., 2016).
Data collection
Semi-structured interviews and focus groups (FGs) served as methods for data collection. Work was undertaken in two phases: (1) online one-to-one exploratory interviews with key practitioner stakeholders (head teachers, Special Educational Needs Co-Ordinators [SENCOs], EMHPs and Clinical Commissioning Group [CCG] leads); and (2) in-person FGs, homogeneous by role (separate for staff, parent/carers and children and young people) to encourage openness. Children and young people participated in three FGs conducted in a mainstream primary school (ages from 8 to 10 years), a specialist school (ages from 7 to 9 years) and a mainstream secondary school (ages from 14 to 16 years). Semi-structured schedules were developed collaboratively by the research team and were informed by the existing literature on WSAs and implementation factors, as well as the research team’s prior work in this area (Flynn et al., 2020). Key domains explored included: stakeholders’ understanding of WSAs, perceived enablers and barriers to implementation, experiences of the Trailblazer support initiative and suggestions for improvement. Questions asked included: ‘How are mental health issues discussed in school currently’; ‘What things help to facilitate a WSA to mental health?’ and ‘What gets in the way of meeting these goals?’. Written informed consent (or assent accompanied by parental consent for children and young people under 16) was obtained from all participants prior to data collection. Interviews and FGs were conducted by two researchers (LPS and NP).
Data analysis
Data were transcribed verbatim, anonymised and imported into NVivo to facilitate analysis. The initial phase of data analysis was an iterative and progressive process using the Framework Approach, following a five-step process: (1) familiarization, (2) developing a thematic framework, (3) indexing, (4) charting and (5) mapping and interpretation (Pope et al., 2000). The development of the analytic framework was informed by a comprehensive review of relevant literature (Spencer et al., 2022). Interview and FG data were coded within a shared framework. The primary analytic focus of this study was on factors influencing the implementation of WSAs from practitioners’ perspectives, and data from parents/carers and children and young people were included to provide contextual insights that enriched the practitioner-focused analysis, rather than to be of equal focus or of direct comparison. Data analysis was led by two researchers (LPS and NP), and emergent themes were discussed within the research team.
In order to provide practical recommendations for implementing WSAs to mental health, themes from the first phase of analysis were mapped post hoc onto the domains of the Theoretical Domains Framework (TDF). The TDF was developed to identify influences on professional behaviour related to the implementation of evidence-based recommendations (Atkins et al., 2017), making it well-suited to examining barriers and facilitators to WSA implementation. Post hoc mapping, rather than using TDF-specific topic guides, ensured that only unprompted and salient domains identified by participants were captured. The TDF domains were mapped onto of the COM-B (Capability, Opportunity, Motivation) model of behaviour change (Atkins et al., 2017; Cane et al., 2012) (see Figure 1), providing a pragmatic organisational and translational framework with which to structure findings for policy and practice stakeholders, rather than to develop or test theory.
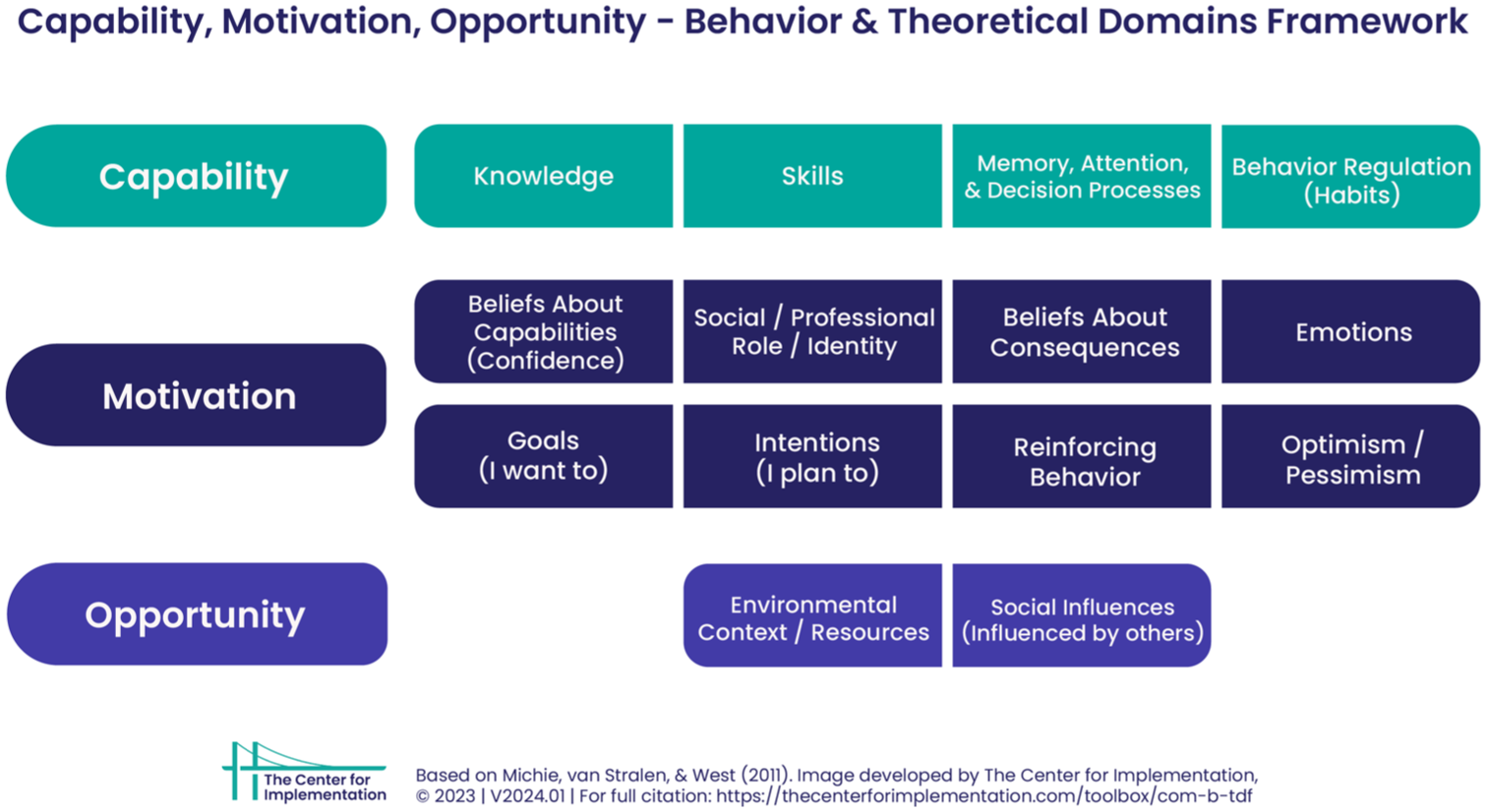
Combination of the COM-B and TDF (The Center for Implementation, 2023).
Ethical approval
Ethical approval for the research was provided by Northumbria University Research Ethics Committee in June 2021 (Reference: 32926)
Results
Data collection took place between July 2021 and December 2022. Nineteen interviews were undertaken with senior practitioner stakeholders (n = 8 from site 1, n = 6 from site 2 and n = 5 from site 3). Twelve FGs were conducted: four practitioner FGs with n = 12 participants; two parent/carer FGs with n = 5 participants and three children and young people FGs with n = 12 participants. Informed by the COM-B framework, our findings are structured under the following three headings: (1) Capability, (2) Opportunity and (3) Motivation, which are then sub-categorised according to relevant domains from the TDF.
Capability
Knowledge
Participants highlighted the importance of enhancing the knowledge base of school staff to effectively address escalating mental health challenges among children and young people. This was seen as pivotal in fostering a supportive and responsive educational environment.
Participants frequently highlighted gaps in knowledge about how mental health services operate, including eligibility, referral processes and what WSAs entail. Both staff and parents emphasised that without clear, consistent knowledge, schools struggle to set realistic expectations for what support can be delivered. For successful implementation, it is crucial for school staff to possess a realistic and comprehensive understanding of mental health services and what defines an effective WSA. Awareness should extend beyond the existence of statutory NHS services such as Child & Adolescent Mental Health Services (CAMHS), to include details on their processes, expected outcomes and limitations, such as long waiting lists and managing expectations among children and young people and parents/carers.
It’s almost like some kind of magical elixir that if we can just get to CAMHS and you know, everything will be sorted, and in reality, that isn’t what happens at all. (INT_07, School Head Teacher) There has to be a collective approach. The acceptance, the compassion, the willingness to understand that every child is different. And I think it’s not just down to the pastoral team or the SENCO team, each member of staff should have a basic understanding of children’s mental health. (FG_2, Parent/Carer, Specialist School)
Skills
Consistent, structured training to equip staff with skills was perceived as essential to meet children and young people’s mental health needs. Participants emphasised the need for staff to develop skills in identifying early signs of distress, responding appropriately in real time and communicating with children and young people about their mental health. These were described as skills requiring structured training rather than one-off sessions. Training should be ongoing and adaptable to ensure that staff can address emerging issues and identify changes in best practice.
They [MHSTs] came in to give us a bit of training last term, but because of the COVID situation it was a little bit sporadic [. . .] there was no sort of cohesive kind of way forward. (FG_9, Staff, Secondary School)
Participants also reflected on how mental health support required not only practical and interpersonal skills but also the ability to build trusting relationships and respond compassionately and flexibly to children and young people’s needs within everyday interactions. Help-seeking was seen as being shaped less by professional role or specialist training than by the quality of relationships and whether staff are perceived as approachable and willing to listen.
I think they should be told [. . .] if you’re feeling [sad or frustrated], don’t just go to youse, go to a dinner nanny, go to the caretaker. And I think then that people also need to have some understanding of how to deal with them, when they’re in that situation. (FG_4, Parent/Carer, Primary School) If you don’t get along, you’re not going to go and speak to them about something that’s quite serious. You’re more likely to go to someone who you feel will listen. (FG_8, Student, Secondary School)
Effective mental health support therefore relies on both interpersonal and procedural competence. Participants articulated frustration with current systems and processes, suggesting that schools and mental health support services should collaborate on the implementation of more efficient administrative mechanisms to reduce burden on staff and provide clarity on the status of referrals and support.
I often get letters with extra paperwork to fill in, for an assessment and that kind of thing. But otherwise, I don’t know where they are in the process. So, even if there was an online tracking or something, so you could see how long they are on the waiting list. (FG_6, Staff, Primary School)
Behaviour regulation
Establishing and maintaining consistent practices is essential for proactively addressing mental health issues. Participants described how structured routines, such as regular emotional check-ins, predictable responses to distress and early intervention strategies, were key for proactively supporting children and young people’s mental health.
Participants also highlighted the need for routines and strategies providing stability, especially during transitions such as moving from primary to secondary school. This could include regular check-ins with students, mindfulness sessions, peer support groups and establishing consistent communication with parents. In addition, data-collection practices and habits need to be shifted towards supporting WSAs, rather than just individual outcomes.
Behaviour changes coming up to holidays ‘cos they know their safe space is not there . . . you can predict it coming. You know there’s certain ones where you know the week or two before a holiday, the behaviour will change and it’ll- they’ll just be not settled at all’. (FG_6, Staff, Primary School) [The] . . . mental health data set. It doesn’t reflect what the breadth of the team is meant to do, even now when they have refined their data collection, in a way it is getting more focused on individual outcomes rather than looking at the development of whole school approaches. (FG_3, Staff, Specialist School)
Opportunity
Environmental context and resources
Adequate resourcing was seen as a critical factor for the effective implementation of mental health initiatives, with concerns about insufficiency voiced by all participant groups. Limited staff capacity and long waiting times for services were seen to restrict the timely delivery of support, leaving students without access to help when most needed. Participants emphasised that without sustained investment in staffing and infrastructure, schools would struggle to embed these initiatives within a WSA. The short-term nature of many funding streams was also identified as a key barrier to sustainability, making it difficult to maintain progress once initial financial support concluded.
All these challenges were evident across different levels of the school system: staff described the strain of operating under budgetary and staffing constraints; students highlighted the limited availability of immediate support and mental health professionals reflected on the instability of external funding and its implications for service continuity.
It’s budgetary constraints. That’s the issue. So, we try our best to prioritise it. But then staff absences and cover and all the rest of it, especially with COVID, has been very, very challenging. (FG_6, Staff, Primary School) I was involved [with] the family intervention projects, and the amount of money that was thrown at them, fantastic ideas, but then I think we were funded for two years and then it all stopped [. . .] reduced pressure on CAMHS and shortening waiting times will come, but it won’t come for a few years. (INT_03, Primary Mental Health Team Service Manager)
The importance of allocating time and resources to mental health leadership roles like SENCOs and Designated Mental Health Leads was highlighted. Participants shared that it was important to ensure that staff have the capacity to focus on mental health initiatives without being overburdened by competing responsibilities.
If I’d been a full-time, class-based teacher, given the role as a Senior Mental Health Lead, I could not have done any of what I’ve done. Even the idea of communicating with people and building those relationships; you wouldn’t have the time. (FG_3, Staff, Specialist School)
Local school contexts and needs also emerged as crucial factors in establishing WSAs to mental health. Participants emphasised the importance of being able to use a flexible approach; tailored to accommodate the unique characteristics and requirements of individual school communities, rather than a one-size-fits-all approach.
Whether it be local drivers, mechanisms, it has allowed some basic principles to be considered across England whilst allowing local interpretation of that, the flexibility from a provider’s perspective. (FG_3, Staff, Specialist School)
Social influences
The importance of co-production and social influence in developing mental health strategies in schools was repeatedly emphasised. Participants highlighted how relationships within schools and between schools and families shaped the success of mental health initiatives. Parents noted the importance of family-school collaboration, recognising that children’s mental health needs cannot be addressed in isolation. Relationship-building and network development within schools and with external services can therefore support more collaborative and sustainable WSAs.
Relationship-building’s been key; inviting people in from all these different services, unpicking their roles as to what they do, and how they can make an impact on our children, our families. (FG_3, Staff, Specialist School) I think the approach with the [school] it’s very much about the family as a whole and they know that if they’re not working, and the child is not functioning then that’s pretty much going to have a knock-on effect for everyone. (FG_2, Parent/Carer, Specialist School)
Motivation
Social/professional role and identity
Providing clarity regarding roles and responsibilities related to mental health support can enhance the effectiveness of school-based initiatives. Participants expressed uncertainty about their professional role in supporting mental health, particularly in relation to how their responsibilities intersected with MHSTs and specialist practitioners. This lack of clarity often left staff unsure about when and how to intervene, reflecting a gap between role expectations and operational reality. Participants also highlighted the importance of ensuring that all staff clearly understand their own and others’ roles within the mental health support system, and it was suggested that this could be achieved through clear documentation, regular refresher training and open communication channels between professional groups.
When it comes to senior leads, obviously, there’s a level of authority that comes along with that into leadership. But in terms of the MHST versus the mental health, the EMHP, I think that would be less equally definable . . . I think it would be more difficult, just reading this for a teacher, for example, to know what the difference is. (FG_9, Secondary School, Staff) Everybody is on the same playing field I would say. All the staff know what they’re looking for, or everybody knows what approach they’ve got to children that they have. (FG_2, Parent/Carer, Specialist School)
Beliefs about consequences
Understanding the long-term impact of mental health initiatives is key to sustaining efforts in the development of a WSA to mental health. Participants recognised that WSAs were expected to have long-term benefits, such as reducing CAMHS demand, but believed that these outcomes could take years to materialise. This perception influenced their motivation to fully engage, as some doubted whether immediate impacts would be seen. Schools should communicate the long-term benefits of these initiatives to staff, children and young people and parents/carers and manage expectations regarding timeframes for change. This can help ensure buy-in, build motivation and maintain commitment over time.
Reducing the pressure on CAMHS and shortening the waiting times is one of the outcomes [. . .] but I think it’s a long-term outcome. It could be years before that is actually delivered and like lots of things, you know, this has come from a political perspective, the politics need to be taken out of it. (INT_19, School CEO) I am sure everyone agrees that yes, mental health should be everyone’s business but how does that translate to on the ground practice when you have got the conflicting agendas of no, we must follow the school behaviour policy [. . .] I think it is very difficult with lots of things coming at teachers. (FG_3, Staff, Specialist School)
Optimism/pessimism
Perceptions of the relative success of mental health initiatives were seen as influencing engagement and motivation. Experiences of inconsistent communication across school settings shaped parents’ optimism or pessimism about mental health support. Positive experiences in primary school settings increased confidence in the system, while negative experiences in secondary school settings dampened expectations and engagement. Creating a positive, supportive environment and maintaining open lines of communication was seen as helping build optimism and confidence in mental health initiatives. One parent/carer clearly articulated the different experiences of communication across primary and secondary school settings. However, some parents/carers shared contrasting experiences, particularly between primary and secondary schools.
I could come in here [the primary school] and I know I could speak to the . . . teacher, I could speak to the TA’s [Teaching Assistant’s] in his class . . . I could speak to anybody in school about [their son] and what they thought and how things were and if they’d seen anything . . . but if it was my eldest, [in secondary school] I’d be lucky if I got a phone call off his tutor. (FG_2, Parent/Carer, Specialist School)
Emotions
Increased empathy and reduced stigma associated with mental health developed during the COVID-19 pandemic, and emotional responses to mental health initiatives can influence their success. Participants described how emotional experiences, particularly empathy and reduced stigma following the pandemic, had motivated more open conversations about mental health. Encouraging more open conversations about mental health among staff, children and young people and parents/carers can help support a more positive mental health culture in schools and reinforce the importance of associated initiatives.
I think that’s probably the best thing to come out of COVID, that everybody’s been a bit more understanding and the stigma around mental health I feel has sort of diminished because of everybody dealt with something during COVID. (FG_6, Staff, Primary School) I think the whole school approach is just treat every child kind. And not that I’m saying the teachers don’t, but just don’t assume, well, that one hasn’t got mental health issues. Because you could with adults. I’m sitting here and I have. [. . .] underlying, no one really knows what goes on. (FG_5, Parent/Carer, Primary School)
Goals
Aligning personal and organisational goals with mental health priorities can encourage engagement and commitment from children and young people specifically. Students articulated clear goals about wanting accessible and confidential mental health support, reflecting the desire to feel safe and in control when seeking help. These goals underpinned their preferences for flexible and anonymous routes to care.
To engage with these concerns, schools could provide multiple channels for children and young people to seek and access support, including anonymous options like e-mail or online forms, to accommodate different comfort levels and encourage more children and young people to reach out for support recognising that there is not a one-size-fits-all approach to treatment.
People don’t like to talk about their mental health . . . so, I think having an email address that they can just email and just vent everything to that email and still get help, rather than talking face-to-face. (FG_8, Student, Secondary School)
Intentions
Concrete plans and commitments are necessary for the effective implementation of WSAs. Schools should engage in continuous consultation with all stakeholders, including children and young people, parents/carers and staff, to ensure that mental health strategies are co-produced, relevant and effective. Importantly, there should be clear communication about the specific goals and limitations of WSAs, as there is often confusion about what these approaches are expected to achieve. For example, the needs of children and young people who may require specialised support differ significantly from the needs of children and young people who can be addressed within the scope of a WSA.
Clarifying these distinctions and managing expectations with young people and parents about what is achievable in schools is crucial to avoid misunderstandings. Participants highlighted their intention to build on early consultation processes and co-produce strategies with children and young people and families, signalling a conscious commitment to embedding mental health approaches beyond initial pilots. Staff provided examples of intent and planning by supportive leadership in implementing initiatives, and this was seen as a powerful facilitating factor.
I think the leadership is very supportive, you know what I mean? We have had great support from the head and the senior leaders and the deputy, but it’s important to everybody. It is something that needs to be happening and it is important. We haven’t really had any obstacles like that. (FG_3, Staff, Specialist School) We’ve done a little bit of consultation with a tiny little group of young people and a couple of SENCOs. We recognise that we need to probably move forward in our next wave, really need the whole co-production process after a little lip service at the beginning of the project. Tell us what you need. So again, it’s lessons learned. (FG_3, Staff, Specialist School)
Reinforcing behaviour
Positive reinforcement can sustain positive mental health practices, cultures and help to facilitate the development of a WSA, as well as overcome distinct challenges, such as generational stigma, whereby parents/carers may not openly encourage discussion about mental health at home. Schools should use consistent, positive messaging and reinforcement to address and reduce stigma around mental health, both within the school and in the wider community, through engagement with the families of children and young people. Participants described how visible positive outcomes, such as improved student engagement and family feedback, reinforced their commitment to mental health practices. Conversely, a lack of engagement with school staff by some families was described as a barrier to providing support for children and young people in need, highlighting the importance of clearly feeding-back positive outcomes of school-based support to parents/carers, so as to encourage continued engagement.
Sometimes parents don’t want to engage. That’s a big one for me. So, I’m thinking of children who perhaps live with grandparents who make comments like, you’ll end up in the ‘loony bin’ or ‘a mental hospital’, or something like that, and then they opt out. That can be a real challenge. (FG_6, Staff, Primary School)
Discussion
Together, these findings underscore the complexity and multifaceted nature of implementing WSAs to mental health across diverse educational settings. As the Trailblazer programme reflects a specific policy context in England, the transferability of findings from this study to other contexts requires caution; however, parallels with international work suggest that many implementation principles may be broadly applicable (Hoover et al., 2019; Pinkelman and Horner, 2019).
Collectively, the findings presented here illustrate that schools’ ability to embed WSAs depends on a dynamic interplay between capability, opportunity and motivation. Building capability requires enhancing staff knowledge, practical skills and consistent behaviours that normalise mental health support in everyday school life. Opportunity arises when adequate resources, time and supportive relationships enable collaboration across school, family and service boundaries. Sustained motivation is fostered through clarity of professional roles, shared belief in achievable outcomes and reinforcing practices that maintain engagement and optimism across the school community.
Role clarity is critical to implementing school mental health programmes (Forman et al., 2013). Confusion over referral processes (Phillippo and Kelly, 2014) can be mitigated with clear documentation and communication to boost staff confidence, and dedicated resources for mental health leadership roles enhance initiative efficacy. Beyond this, our study highlights the importance of fostering a positive mental health culture in schools (Allen et al., 2018; Fullan, 2016; Wang and Degol, 2016), which can prevent mental health stigma through open conversations, building upon increased empathy observed during the COVID-19 pandemic and the recognition by children and young people that mental health problems are an increasing issue (Hermann et al., 2022).
Previous research has stressed the importance of targeted professional development in improving mental health outcomes in schools (Weist et al., 2012). Our findings highlight that school staff having both a comprehensive knowledge of mental health and practical skills is a necessity, and it is important to enhance this knowledge base through structured and ongoing training programmes. These programmes should cover not only mental health issues but also the operations and limitations of statutory mental health services. By doing so, staff can manage expectations and better navigate the referral processes; reducing frustration and enhancing responsiveness to mental health challenges faced by children and young people. Based on the findings of this study, we highlight the need for adaptable training that evolves with emerging mental health trends, suggesting a dynamic approach to professional development that is responsive to changing mental health landscapes, while taking into consideration the fact that non-specialist school staff should not be expected to take on the perceived role of a therapist (Shelemy et al., 2019).
Strong school and external mental health networks foster collaboration and effective strategies; however, sustaining mental health initiatives requires inter-agency collaboration and resources (Fazel et al., 2014). Our findings signal the need for adequate resources, both financial and logistical, for the successful implementation of mental health initiatives, as budget, staffing and time constraints can hinder WSAs’ success (Childs-Fegredo et al., 2021). It is important to note that in recent years, the NENC (where the present study was conducted) has experienced the largest reduction in funding and seen the greatest decline in children and young people’s mental health in England (Brown et al., 2024). In the present study, there was a stronger emphasis on targeted interventions for students with identified needs, rather than proactive whole-school wellbeing and promotion. This could suggest that in high-need contexts, stakeholders may prioritise addressing acute needs over universal preventive strategies in schools, which was intended to be one of the key functions of MHSTs (UK Government, 2017). Our findings reveal the importance of maintaining optimism and creating a supportive environment that builds confidence among stakeholders, while maintaining the ability to tailor WSAs to the local context and needs of individual school communities (Childs-Fegredo et al., 2021). They also contribute to the ongoing debate about the balance to be achieved between universal and targeted approaches to school mental health promotion, underscoring the need for both preventive and responsive strategies (O’Reilly et al., 2018).
Strengths and limitations
This study was conducted across three Trailblazer sites within the North East of England, which may limit the generalisability of findings to other regions with different demographic or structural characteristics. However, our sample included a diverse range of participants, including senior practitioners, school staff, parents/carers and children and young people (Crouch and McKenzie, 2006; Vasileiou et al., 2018). A key strength of this study lies in its focus on real-world experiences of WSA implementation in active Trailblazer sites, grounding the findings in practical realities of delivering mental health support within complex educational settings.
While parents/carers and children and young people contributed valuable contextual insight, the primary focus was on practitioners’ perspectives on implementation processes and operational challenges, and as such, these perspectives predominated; therefore, the comparatively lower representation of parents/carers and children and young people may have constrained the breadth of viewpoints captured. Future research should prioritise amplifying these voices, specifically those from under-represented or marginalised groups, to ensure that the continued development of WSAs is informed by those with lived experience, as well as those responsible for delivery.
While the use of the COM-B and TDF helped structure the analysis, not all TDF domains were represented in the findings, and some were represented less prominently. This was due to participants raising fewer issues relevant to these areas, reflecting the relative salience of different influences on implementation rather than a limitation of the approach itself. The frameworks were also applied post hoc, rather than being applied a priori while developing our semi-structured topic guides, which enabled participants to speak foremost on the issues relevant to them but still allowed the organisation of views into a behaviourally-informed structure familiar to implementation stakeholders, supporting the translation of findings into actionable insights for policy and practice, while preserving the authenticity of participants’ accounts.
Conclusion
These findings have important implications for policy and practice in implementing WSAs to mental health in educational settings. Clear communication, role clarity and ongoing professional development are central to fostering cohesive and inclusive school environments, yet challenges remain in adequately supporting the mental health of children and young people. Policymakers should prioritise sustained funding, appropriate resource allocation, comprehensive staff training and dedicated mental health roles in educational settings. Alignment with existing research suggests a shifting mental health landscape that warrants further investigation. As the findings from this study are exploratory and context-specific, future research at regional and national levels is needed to assess their generalisability, examine longitudinal impacts and explore links between WSA implementation and specific mental health outcomes.
Footnotes
Acknowledgements
We thank participants for contributing to this research.
Declaration of conflicting interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: At the time of the study and the writing of this paper, HW was the Programme Lead, EJH was the Academic Lead and MW was the Clinical Lead for Education Mental Health Practitioner (EMHP) training at Northumbria University, and they provided oversight to the training programme. LS, NP, DF, GM and JJN declare no conflicts of interest.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: this research was funded by the National Institute for Health and Care Research (NIHR) Applied Research Collaboration (ARC) North East and North Cumbria (NENC) (NIHR200173), Ref: OFC20_05. LS was funded by an NIHR ARC NENC Mental Health Fellowship. The views expressed are those of the authors and not necessarily those of the NIHR or the Department of Health and Social Care.
AI use
No artificial intelligence tools were used at any stage to generate, analyse, write, edit or refine the manuscript.
Data availability
The data supporting this study’s findings are not publicly available due to the need to ensure participant confidentiality. Reasonable requests for anonymised data access will be considered by the corresponding author.
