Abstract
Objectives:
Vaccination in pregnancy is recommended to protect newborn infants against whooping cough, and pregnant people and their infants against influenza. Influenza vaccination is recommended at any time in pregnancy and pertussis vaccination is recommended after 16 weeks gestation. However, some pregnant people are not aware of recommendations or the importance of antenatal vaccination. This study explores the feasibility of adding a targeted prompt for discussion of antenatal vaccination into a maternity client-management software in Aotearoa New Zealand.
Design:
Explanatory cross-sectional study.
Setting:
Midwives practising as lead maternity carers in Aotearoa New Zealand.
Method:
Participants were asked about the feasibility and usefulness of including a prompt in antenatal client-management software to encourage and support discussion about antenatal vaccination. The online survey was composed of multiple choice and Likert-type scale questions with additional free-text options investigating opinions on prompts, how the prompts should occur and potential for supportive resources. Responses were analysed using descriptive statistics and descriptive qualitative analysis of open-ended responses.
Results:
A total of 139 midwives participated in the study. Most respondents indicated they would be open to having a prompt in their client-management software to support discussion about vaccinations and thought it would be useful. Over three-quarters considered a pop-up style prompt would be most convenient if it could be easily turned off when no longer needed.
Conclusions:
A pop-up prompt in antenatal client-management software with additional resources and features would be useful to midwives to support timely discussions about antenatal vaccination. However, for prompts to be useful, they must be designed so as to minimise disruption to midwives’ workflow and be able to be switched off if necessary.
Introduction
In Aotearoa New Zealand, influenza (flu) vaccine at any time in pregnancy and pertussis (whooping cough) vaccine from 16 weeks gestation are recommended to protect pregnant people and their infants from severe diseases; COVID-19 vaccination is also recommended in those at risk of severe disease (Ministry of Health, 2024). Vaccination during pregnancy protects pregnant people, and their newborn infants through transplacental antibodies (Ministry of Health, 2024). Influenza during pregnancy can result in hospitalisation, pregnancy loss and adverse foetal outcomes; infants with influenza also have high rates of hospitalisation (Regan and Munoz, 2021; Vousden et al., 2021). For pertussis, antenatal vaccination protects infants too young to be vaccinated (Regan et al., 2023). It may also reduce transmission of pertussis to infants from infected adults and adolescents, who are the most common source of infection (Mohammed et al., 2019).
Although antenatal influenza and pertussis vaccination has been recommended and is available free of charge for many years in Aotearoa New Zealand, vaccination coverage is low across the country, with less than half of eligible people being vaccinated while they are pregnant, and with lower coverage levels in areas of high deprivation (Howe et al., 2020). Coverage is even lower among some ethnicities, with only 26.5% of Māori and 9.7% of Pacific Peoples vaccinated in pregnancy in 2020 (Hobbs et al., 2023). Low and inequitable vaccination coverage leaves mothers and infants susceptible to severe adverse health outcomes from pertussis and influenza infection.
To increase antenatal vaccination rates, a range of programmatic interventions have been recommended. Most research in this area has explored combinations of interventions targeting both health professionals and patients to promote accessibility and knowledge (Dehlinger et al., 2021; Ellingson et al., 2019; Kaufman et al., 2020; McCarthy et al., 2015; Mohammed et al., 2019; Patel et al., 2021). One of the consistently identified main reasons pregnant people are not vaccinated is because they do not know vaccination is recommended, and/or have not been educated about the severity of infections that can occur (Mak et al., 2015; Shavell et al., 2012).
A recommendation for vaccination by a health professional is an important factor in increasing vaccine uptake (Dehlinger et al., 2021; McCarthy et al., 2015; Mak et al., 2015; Mohammed et al., 2019; Shavell et al., 2012). In Aotearoa New Zealand, there are over 1100 practising Lead Maternity Care (LMC) midwives providing antenatal care through a continuity of care model (Sandall et al., 2024) and who, in 2023, were the lead carer in 93% of pregnancies/births. Midwives are a trusted information source for pregnant people and typically the healthcare provider seen most often during pregnancy; thus, their recommendations are highly valued and positively influence decision-making (McCarthy et al., 2015; Mak et al., 2015). However, discussion of vaccination may not always be prioritised (Young et al., 2023a). Midwives and other health care professionals (HCP) often have a wide range of things they must talk about in limited time and vaccination can be easily forgotten during consultation (Klatt and Hopp, 2012). Some pregnant people have reported they do not recall being informed about vaccination during their pregnancy (Klatt and Hopp, 2012; Maher et al., 2014).
Reminders/prompts that occur when the patient/client is with the HCP have been shown to be the most promising form of reminders (Shojania et al., 2009), and research specific to antenatal vaccination has shown that prompts in healthcare software to discuss vaccination with pregnant people are linked to increased antenatal vaccination rates (Mohammed et al., 2019). ‘Hard-stops’ are alerts/prompts that require interaction with or a response to be input to the alert before the user can dismiss them but can be unpopular with users if perceived as disruptive to workflow (Klatt and Hopp, 2012; Stockwell et al., 2015). Expect Maternity Software is client-management software used by most lead maternity carer midwives in Aotearoa New Zealand (Anneliese Allen, personal communication 31 October 2022). However, currently there is no prompt in the software to remind midwives to discuss vaccination and no information about how midwives view prompts for discussion.
The objectives of this study were to explore the views of midwives about (1) installing a prompt in their client-management software to remind them to discuss influenza and pertussis vaccination with their pregnant clients, and (2) the addition of other links and additional information within prompts to support these sometimes difficult discussions.
Methods
Study design and setting
This explanatory cross-sectional study surveyed Lead Maternity Carer midwives in Aotearoa New Zealand to explore their views on the feasibility of including a prompt in the Expect Maternity software to encourage and support discussions about antenatal vaccination. The survey was disseminated to participants using the Qualtrics survey platform in early December 2023. To increase participation, one reminder was sent 2 weeks later and the survey closed 5 weeks after the initial email. Data collection was anonymous. Participants who were eligible to participate were informed that completing and submitting the survey was taken as consent. Ethical approval for this study was provided by The University of Otago Human Ethics Committee (D23/301).
Participants
Midwives currently practising (or planning to return to practice within the next 12 months) as Lead Maternity Carers in Aotearoa New Zealand who used the Expect maternity software and could speak and understand English were contacted for participation. Recruitment was conducted via an email distributed to the approximately 900 midwives who use the Expect maternity software system.
About the software
Midwives use Expect maternity software to document clients’ clinical information, details and treatment plans. There are two identified mechanisms by which a new prompt could be included in the Expect Maternity software:
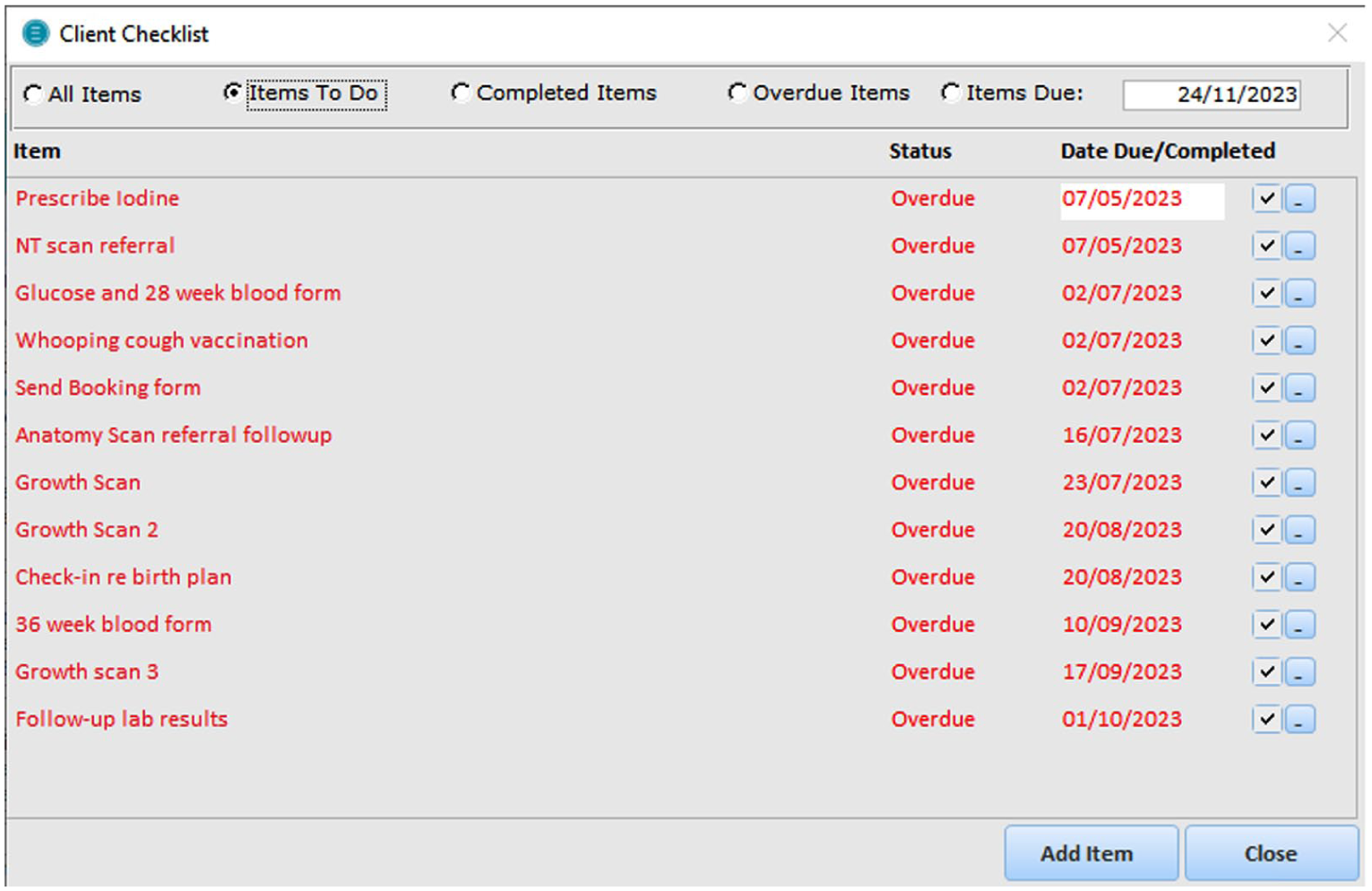
An example of the current checklist in Expect Maternity software.
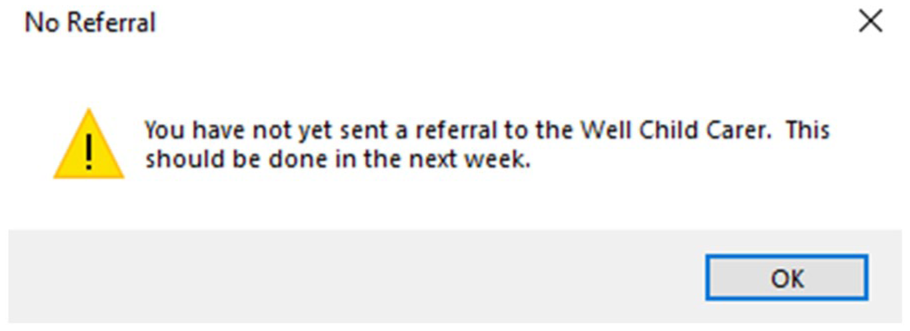
Example of a current pop-up in Expect Maternity software.
Designing the survey
A survey was developed based on the literature around usability of health information technology (Yen and Bakken, 2012) and input from the research team (including Māori healthcare research academics, a pharmacist and a developer of Expect Maternity software).
The survey was composed of multiple-choice and Likert-type scale questions with additional free-text options investigating opinions on prompts to encourage discussion about vaccination, how the prompts should occur and potential for supportive resources. The survey provided possible mechanisms for integrating a prompt into the Expect maternity software and asked questions about whether users would find this useful and what they would like and dislike about the prompts. It also asked about whether participants thought prompts would be effective, and what additional links and features would be useful. Demographic information such as age, gender, ethnicity, time in the workforce and location of practice was collected to compare survey respondents to the general lead maternity carer midwife population using the Midwifery Council New Zealand’s maternity workforce survey 2022 (Midwifery Council, 2022).
The survey was peer-reviewed for validity and suitability of language and piloted with four midwives from the study cohort with additional questions about usability, understandability and request for general feedback. The pilot survey highlighted a number of misunderstandings about aspects of the software; thus, screenshots were added to clarify meaning and some questions were modified. As well as survey piloting, other strategies adopted to minimise attrition bias included keeping the survey questions to a minimum, and adapting other validated survey questions for our study. A copy of the final survey instrument may be made available upon application to the corresponding author of this paper.
The survey was designed to take up to 10 minutes to complete and as a thank you, participants had the option to participate in a draw to win one of five $100 vouchers.
Analysis
Data were extracted into Excel for analysis. Descriptive statistics were used to summarise the frequencies of responses in the survey. Qualitative data were analysed thematically using descriptive qualitative analysis (Kim et al., 2017). Codes were developed based on the free-text survey responses and grouped into themes to add context to the frequency responses. Themes underwent further refinement by reviewing, collapsing and triangulating against the quantitative survey responses to add depth to the findings. These were then reported in the study following the quantitative results.
Non-response bias was analysed by comparing responder demographics with the demographics of the Aotearoa New Zealand midwifery workforce (Sedgwick, 2013).
Results
The survey received 143 responses (out of around 900 potential participants), a response rate of approximately 15%. Eleven participants were excluded due to not meeting the inclusion criteria or not answering survey responses beyond the screening questions, leaving 132 participants in the final analysis. Detailed location information provided in the survey responses was converted to regions based on New Zealand census data. The respondents largely resembled the overall midwifery workforce demographics from a 2022 workforce survey (Midwifery Council, 2022). However, there were more representatives from smaller urban areas and rural communities and from members of the 50–59 age group (Table 1).
Demographics of survey respondents.
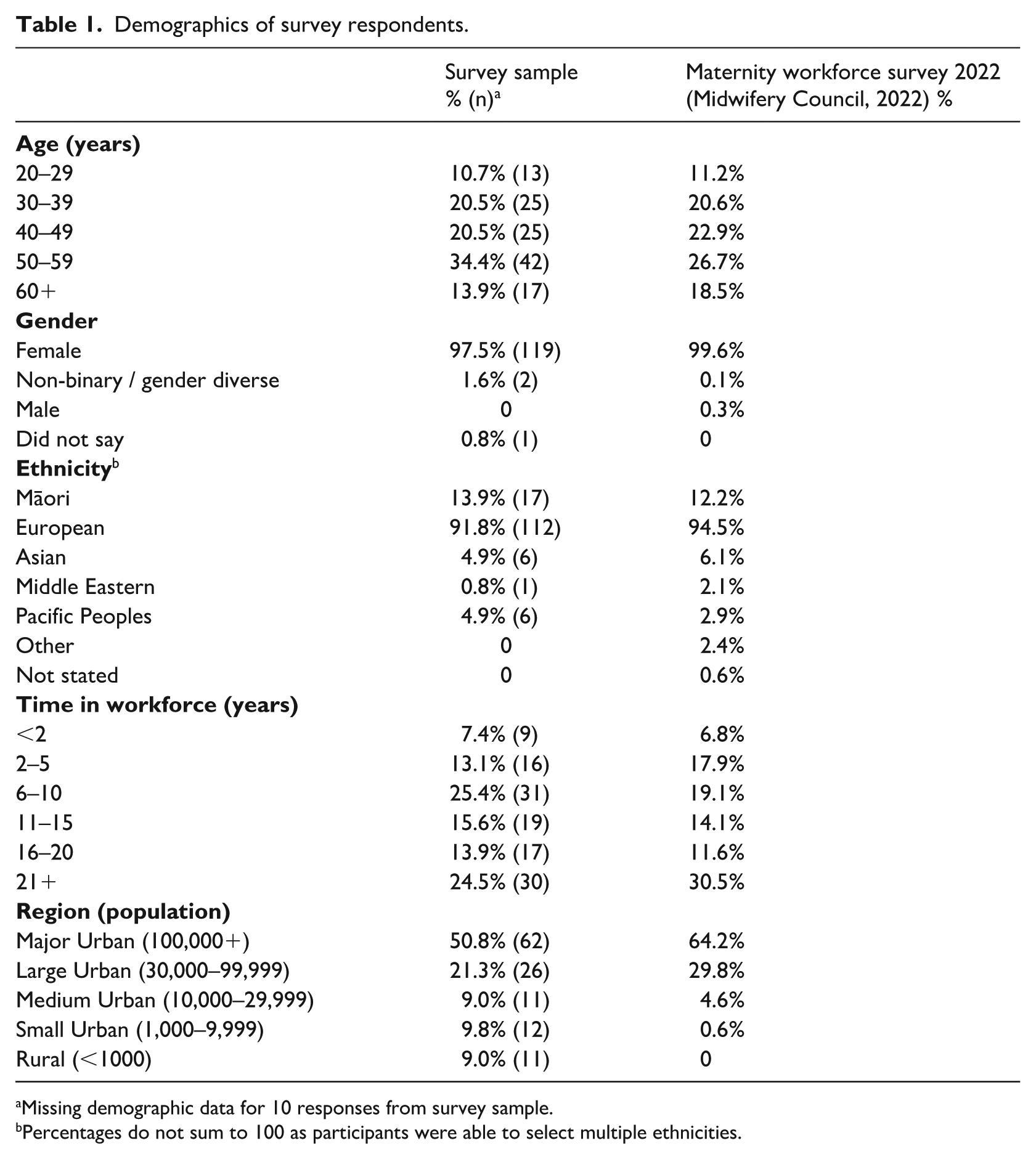
Missing demographic data for 10 responses from survey sample.
Percentages do not sum to 100 as participants were able to select multiple ethnicities.
Introduction of a prompt
Most midwife respondents (64%, n = 85/132) supported the introduction of a prompt reminding them to discuss vaccination with their clients. Over half of the Māori and Pacific Peoples respondents also supported the introduction of a prompt (55%, n = 11/20). Most participants strongly agreed or somewhat agreed that the prompt to discuss vaccination against pertussis and influenza would be useful (37% (n = 49/132) and 32% (n = 42/132), respectively). Few strongly disagreed or somewhat disagreed that it would be useful, 6% (n = 8/132) and 11% (n = 14/132), respectively.
Participants were asked what they would and would not like about a prompt. Forty percent of participants (n = 53/132) said they would like all aspects of a prompt. The most frequent reasons why participants would like a prompt were that it could be turned off (58%) and because it could remind them to discuss vaccination on multiple occasions (49%). Over one-third thought that a prompt could contain other useful information (39%). From a practicality point of view, more participants thought that having a prompt would not take up too much time (30%) and would suit their workflow (19%) than those who thought it would be too time-consuming (3%) and would not suit their workflow (12%). Reasons why participants would not like a prompt included because they thought it would be annoying (42%). A few participants (12%) thought a prompt unnecessary because they did not want to be reminded to discuss vaccination (Table 2).
Reasons why a prompt would or would not be liked by participants.
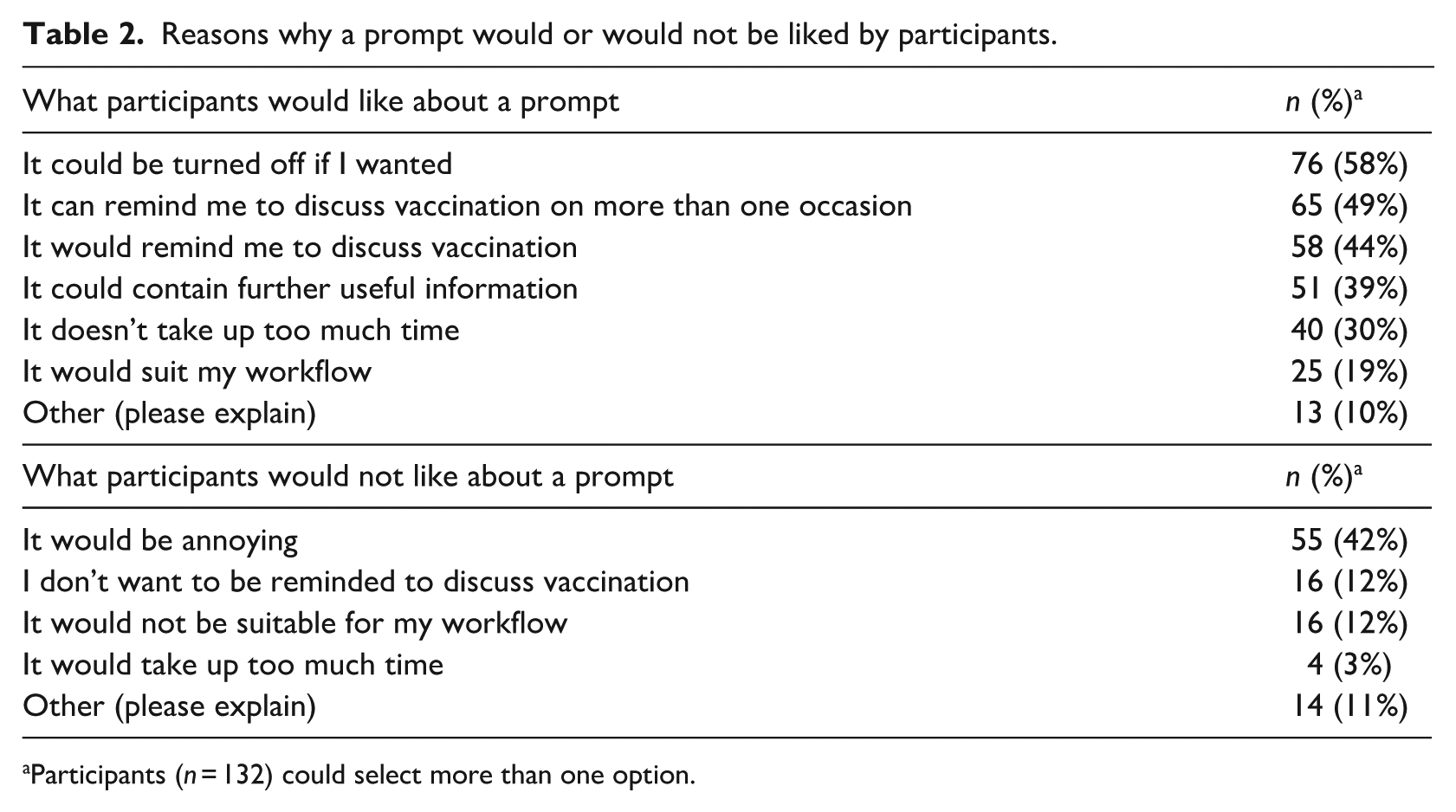
Participants (n = 132) could select more than one option.
Factors identified in our analysis of open-ended responses about what participants would, or would not, want in a prompt were appropriate design, not adding value and disruption. Participants thought a prompt would not be too impactful on workflow if it did not repeatedly pop-up after it had been responded to (as declined, received or discussed) and the timing was appropriate for best practice, for example, after 16 weeks of pregnancy for pertussis vaccination: Just [a] one-off prompt would be good [a repeated] prompt can get very annoying. (P7) It would remind me to discuss vaccination at the RIGHT time; as sometimes may forget until later in pregnancy. (P6)
Many participants provided additional reasons as to why they might not want the introduction of the prompt. Some midwives thought a prompt was not necessary as they already discussed vaccination or they had created their own method of reminding themselves to have these discussions, including using existing features within the software that enabled them to create their own reminders: I already have my own prompts set up in my Care Plan, Auto-text set by gestation and on the check boxes on the antenatal page, as well as checklist in the booklet I give to my clients. (P20)
Others who felt the prompt might be annoying (n = 8) described how current prompts within the system (e.g. for prescribing iodine) could be a nuisance because they came up at the wrong times and continued to pop-up despite being dismissed or resolved: The current prompt for iodine is a pain in the butt. I don’t forget to talk about iodine – it’s routine care, as are discussing vaccinations. More pop ups getting in the way of my workflow would be annoying. (P4)
Respondents who wanted a prompt (n = 85) were asked what style of prompt was preferred. A pop-up style (see Figure 2) was the clear preference (77%, n = 67/85). Only 20% (n = 17/85) of participants preferred the alternative of including a prompt within an existing checklist. Important themes identified in free-text responses were usefulness and workflow. Some respondents said they preferred a pop-up prompt option because they did not regularly use the existing checklist feature. They thought a pop-up would be both more obvious and therefore more effective in initiating discussion, and also because they would need to take action after the prompt to carry on in the system: The popup is in your face, and it can’t be ignored, and you have to acknowledge it to turn it off. (P66)
Those who preferred a checklist liked the fact that they could see other parts of the plan, with less disruption to workflow: [A] checklist would be easier as it won’t interrupt your workflow and you can click on it when it suits you to check you’ve done everything- usually at the end of an appointment. (P7)
Further information and additional features
Fewer respondents completed the section in the survey asking about further information and additional features (n = 125). Over half of them (58%, n = 73/125) said they would like links to more information about antenatal vaccinations included as part of a prompt, whereas 39 participants (31%) replied that they would not like this and 13 (10%) did not know. Participants who responded that they either would like links to further information or were not sure gave reasons why (n = 85). The most popular reason was to help access information in other languages (67%, n = 57/85). Over half of the respondents would like this because it would help them find relevant information more easily (59%, n = 50/85). Some thought that links to resources could help them find useful printable information to give to people (47%, n = 40/85) and support difficult conversations about vaccination (45%, n = 38/85).
One hundred twenty-three respondents answered questions about usefulness and the features they would like included in a prompt. Sixty-three percent (n = 78/123) of these respondents thought that a prompt containing further information could support discussion about pertussis and influenza vaccination. Seventy percent (n = 86/123) thought that links to additional information, such as reputable leaflets (e.g. from the New Zealand Immunisation Advisory Centre, Health New Zealand| Te Whatu Ora, or the Healthify website), could also be useful. Forty-seven percent (n = 58/123) thought links to websites showing locations offering vaccination and videos about the importance of vaccination in pregnancy (44%, n = 54/123) would be useful. Eleven participants did not think additional features with further information would be useful.
Over two-thirds of the 123 participants responding to questions about prompt functionality would like to have checkboxes that, when ticked, would document vaccination discussion in the client record (68%, n = 84/123). Fewer thought links to the National Immunisation Register (NIR)/Aotearoa Immunisation Register (AIR) (30%, n = 37/123) to check vaccination status would be useful.
Discussion
This was a cross-sectional study investigating Lead Maternity Carer midwives’ views of a prompt being included in the Expect maternity point-of-care client-management software to support discussions about antenatal vaccination. Most midwives in the study supported the introduction of a prompt in their software and there was interest in additional features to support discussion and workflow. There is a dearth of research investigating midwives’ experiences of computer prompts; however, the key issues highlighted by midwives in this study, such as ensuring a prompt was not disruptive, are consistent with previous research (Backman et al., 2017).
Reminders or prompts are cognitive aids targeting both providers and/or patients that are used in many parts of health care to improve healthcare provider patient care. They have been shown to decrease the incidence of missed care in healthcare settings (Greig et al., 2023). Alerting providers to prompts at the point of care is an effective strategy to remind the healthcare provider to undertake a task while the person concerned is still with them. A 2009 Cochrane review showed that computer reminders in patient management software were associated with a modest improvement in all the health outcomes investigated, including significant improvements in vaccination prescriptions (Shojania et al., 2009). Due to current low rates of antenatal vaccination in Aotearoa New Zealand, there are significant gains to be made by increasing coverage, especially in Māori and Pacific communities with historically low levels of antenatal vaccination coverage (Pointon, 2020).
Reminders or prompts in healthcare providers’ patient/client management systems have been trialled internationally with the aim of increasing antenatal vaccination by reminding the health provider at point of care. In our study, participants thought that prompts would support discussion about vaccination, and this has been shown to be true in international studies. Klatt and Hopp (2012), for example, found that an addition of a prompt in a Wisconsin obstetrics clinic increased documented prenatal influenza vaccination discussion from 49.5% to 89.5% of the time (p < .001, confidence interval [CI] = 0.35–0.45) (Klatt and Hopp, 2012). Both on their own, and in combination with other interventions, prompts have also shown to increase antenatal vaccine acceptance and vaccine uptake (Klatt and Hopp, 2012; Morgan et al., 2015).
Midwives in the study liked the fact that a prompt would remind them to discuss antenatal vaccine recommendations indicating the potential to prioritise these important discussions, similar to findings from Kwan et al. (2020) whose meta-analysis demonstrated that proportion of patients receiving desired care increased by 5.8% following the introduction of clinical decision support systems (e.g. prompts) in practice. Although the efficacy of prompts in software has mainly been evaluated for medical prescribers working in hospital or primary care settings (Kwan et al., 2020; Van Dort et al., 2021), the clear support that midwives in this study gave to the inclusion of a prompt suggests that implementing prompts to discuss antenatal vaccination in the software they used could help support and encourage discussions in practice.
The preferred pop-up style of prompt was an example of both a ‘point of care’ and ‘hard-stop’ prompt, both of which have been shown to increase efficacy (Klatt and Hopp, 2012). Although there are demonstrable benefits of using software prompts such as those of interest in this investigation, other studies have identified the risk of technology becoming a burden on healthcare providers’ time and patient/client management (Backman et al., 2017). Importantly in the study, participants expressed concern that prompts could become a nuisance and interrupt the flow of their current practice. It is essential, therefore, for prompts to be designed with user-workflow/preference in mind to prevent the development of ‘alert fatigue’ identified in other studies (Backman et al., 2017).
Having a recommendation to receive vaccination from a midwife or other trusted healthcare provider can be a successful way to increase vaccination uptake (Gauld et al., 2022; Mak et al., 2015). However, midwives have a large amount of information to cover when they are meeting with pregnant clients and previous research has reported that they sometimes may not feel confident to discuss vaccinations or struggle to find the time to discuss them in depth (Young et al., 2023a, 2023b). In this study, a small number of midwives thought a prompt was not necessary because they already discussed vaccination with their clients and did not need to be reminded or to have access to further information or educational material. However, previous research has identified that pregnant people often do not remember being informed about vaccine recommendations in pregnancy and midwives may have difficulty in initiating conversations (McCarthy et al., 2015; Young et al., 2022, 2023a, 2023b). This highlights the continuing importance of interventions to support midwives in vaccination discussions.
Strengths and limitations
This study was novel because it explored midwives’ views on the possible introduction of a prompt into the software they used to support the provision of patient care. It also examined the design and functionality of possible prompts. However, despite the use of an incentive (prize draw) to encourage study participation, the response rate of 15% was lower than anticipated. At the current time, the midwifery workforce is overstretched in Aotearoa New Zealand (Whyte, 2022) and this may have impacted willingness to participate in the study, as has been reported in other midwife-focused research in Aotearoa New Zealand with low response rates (Young et al., 2023b). Despite this, the overall demographics of participants were representative of the wider midwife population which supports limited generalisability of the study’s findings.
Conclusion
In this study, most participants considered the introduction of a vaccination prompt into the existing client-management system acceptable, and thought that prompts could support important antenatal vaccination discussions. However, for prompts to be useful, it is important that they are designed to minimise disruption to workflow, can be switched off if necessary and would appear only at relevant times (e.g. after 16 weeks of pregnancy to remind midwives to discuss pertussis vaccination). Midwife participants in this study showed some interest in having links to additional resources to support midwives’ provision of information, including information provided in a variety of languages that could be printed off and videos.
Footnotes
Acknowledgements
We thank Expect Maternity for distributing the survey and the respondents who took the time to complete the survey.
Funding
The authors disclosed receipt of the following financial support for the research, authorship and/or publication of this article: this work was supported by the Health Research Council of New Zealand (HRC Project Grant 23/184).
Use of AI
The researchers did not use AI to develop or fine tune any aspect of this paper.
