Abstract
Objective:
Health apps for smartphones have largely overlooked one means of expanding effectiveness: namely, inviting access by secondary app users who can contribute positively to primary users’ lives. We report on outcomes from field testing a cooking app where dissemination included both mothers who were household cooks (primary users) and their children (secondary users).
Setting and Method:
The app, VeggieBook, aimed to increase the use of vegetables in meals and snacks by household cooks. Clients at 15 community pantries were randomly assigned to receive or not receive the app. The same vegetables were supplied to all participants. In each family in the experimental group, the mothers and a 9- to 14-year-old child were each given their own portal into the app. Interviews before, during and after the project and electronic capture of app use measured key variables. The app’s impact on children was gauged by whether or not they became involved in helping prepare family dinners.
Results:
Availability of VeggieBook increased children’s collaboration with their mothers, even though the app contained scant content urging this. Collaboration occurred most often in families where electronic media (television, phones, earbud devices) did not intrude on socialising during meals, and there were opportunities to acknowledge children’s kitchen contributions.
Conclusion:
Implications are identified for the creation of other health apps intended for disease prevention and management. Secondary users (spouses, home caregivers, children and friends) could also be targeted to use apps meant for primary users (people at-risk for illness or patients), thereby building collective action towards improving health.
Introduction
Health apps continue to multiply as tools for disease prevention and as interventions to assist in managing illness (Powell and Torous, 2020). This form of health outreach has been welcomed by health-care professionals, many of whom have joined the ranks of app developers (Choi et al., 2020; Kerst et al., 2020). Smartphones, in particular, enjoy wide public acceptance. This is partly because traditional means of patient-counselling have often been shown to be ineffective or underused when efforts rely on delivery by medical providers or on campaigns using conventional media such as print or broadcasting (Leavy et al., 2011; Livingston et al., 2013; Morrison and Wertheimer, 2004; Stone et al., 2002).
Regrettably, however, some of this confidence in apps rests on shaky ground. Only a handful of the 325,000 health apps available, as of 2017 (Research2Guidance, 2017), have been field tested for whether they improve indicators of disease susceptibility or illness management (Davis and Oakley-Girvan, 2017; Lau et al., 2020; Neary and Schueller, 2018; Van Velthoven et al., 2018). Regardless, public health programmes continue to build apps and efforts continue to test apps’ claims of health benefits (Nilsen et al., 2012).
The analysis reported here addresses an issue that has not yet received much attention: namely, whether the effectiveness of some health apps may be broadened by including secondary as well as primary users. An app intended for an arthritis sufferer, for example, might also include family caregivers as users. An app intended to log exercise and weight management might also encourage access by a spouse or other significant other. Automated systems for characterising the hundreds of thousands of apps now available have identified a number that link users with their medical team. But few health apps have been built and promoted to reach people who are known to one another in the same families or friendship circles (Paglialonga et al., 2018).
To raise awareness of potential impacts from such multi-use within families, we report our experiences building and field testing an app intended for cooks in low-income households who rely on food pantries. 1 In this case, the primary audience was mothers who are household cooks. In addition to these primary users, we wondered whether the app might reap additional benefits by encouraging use by a secondary target audience in the form of 9- to 14-year-old children in the same household.
This paper focuses on an app that has been successfully field tested (Clarke et al., 2019). A 15-minute demonstration of the app can be found at https://www.youtube.com/watch?v=BBmlMQ2QuEw. See Supplemental Material for details of the app and its objectives. While our app facilitates preventive steps in family diet and nutrition, our findings could be applied in other areas such as oral health, medication management, type-2 diabetes, palliative care, or other issues. Engagement by secondary users can ignite conversation and other social processes that may magnify an app’s usefulness for disease prevention or for engaging with treatment. This case study illustrates how this might occur.
Reasons to engage children as secondary app users
While adults are the likeliest household members to prepare meals, children sometimes contribute to these recurring family needs (Slater and Mudryj, 2016). When adult-child collaborations occur, at least four benefits are frequently claimed. First, children’s participation in kitchen tasks can slow the erosion of food preparation skills between generations, sometimes lamented as the de-skilling of the US kitchen (Jaffe and Gertler, 2006). Second, collaboration with children can blunt the onset or persistence of picky eating because children often become invested in dishes they have had a hand in making (Taylor and Emmett, 2019). Third, the sharing of tasks in the kitchen can help build positive parent–child relationships and promote healthy child development (Meier and Musick, 2014). And fourth, there is evidence that children’s participation in meal preparation is positively associated with the quality of their diet. For example, children’s kitchen involvement has been shown to be correlated with their increased consumption of vegetables and fruit (Chu et al., 2012). Not surprisingly, authoritative guidelines for better family nutrition often invite parents to involve children in meal preparation (Dietz and Stern, 1999).
There are good reasons, therefore, to promote age-appropriate child involvement in assisting with meal preparation. We expected that the emergence of such secondary benefits would be contingent on how rewarded children felt for taking part in kitchen work. In particular, we hypothesised that dinnertime atmosphere would partly explain the likelihood of conversion from bystander to kitchen helper. The dinner table is a site where rewards from collaboration are made manifest. One revealing expression of atmosphere is the extent to which electronic media such as television, mobile phones and devices with earbuds are present and could, potentially, distract during mealtime. Such distractions, we reasoned, might compete with family members’ attention to each other, and could lead family members to grow less alert to the food they are consuming (see Supplemental Material for background about electronic media and eating behaviour).
Methods
The data reported here were drawn from a randomised controlled field experiment testing whether VeggieBook enabled household cooks to incorporate more vegetables into family meals and snacks, compared to families without access to the app (Clarke et al., 2019). Nine food pantries were randomly assigned to the experimental condition with their 183 clients; 6 food pantries, comprising 106 families, were assigned to the no-app control condition. This unequal assignment concentrated field work where variability from the intervention was most expected. All the pantries were in Los Angeles County. Participants were recruited from pantry queues and qualified if they were mothers (or, in three cases, grandmothers) of a 9- to 14-year-old child living at home, were the household’s main cook, had at least one other adult living in the household, could read either English or Spanish, owned at least a basic cell phone (hence excluding families that were inexperienced with mobile technologies), and met other criteria, such as availability for interviews.
The study provided both control and experimental food pantries with equal supplies of fresh vegetables across 4 weeks; participants also received their usual supply of foods. Baseline personal interviews were conducted separately with mothers and with their children, just before the study commenced and again 10 weeks later (the post interview). Phone interviews with mothers in the third or fourth week of supplemental supplies of vegetables gathered information about use of these foods in meals and snacks. Fathers or other men are sometimes a household’s main cook, but our field study was too small to include such atypical cases. For additional details about the randomised trial, its design and measures, and a CONSORT flow diagram showing numbers of households retained at steps of data collection, see Clarke et al. (2019).
Measures
Most of the questionnaire items and other data-collection methods were created especially for the randomised controlled field trial and the present analysis. The exception was the assessment of vegetable usage by household cooks, which was validated in earlier research (Clarke et al., 2011: 575). Research procedures, materials, and staff were approved by the University of Southern California Institutional Review Board. Mothers provided written informed consent and children provided oral informed assent.
Use of VeggieBook by cooks and children
Our app was equipped with a backend analytics function that electronically captured each user’s interactions with the app. We recorded the number of times each cook and each child created a collection of recipes, anchored in one of the app’s inventory of vegetables, and created a collection of Secrets to Better Eating. In the analysis here, these content collections were calculated across the first four weeks of the study protocol, when the project was distributing supplemental vegetables to experimental and control pantries.
Household cooks’ incorporation of vegetables into meals and snacks
In the third or fourth week of receiving supplementary vegetables, phone interviewers asked cooks whether they recalled making any use of the most recent week’s offerings of two vegetables (i.e. broccoli and green beans, or cauliflower and zucchini). Interviewers probed day-by-day since distribution, for what a cook did with each vegetable, what cooking methods were used, which people in the household had eaten some of the preparation, and more. These detailed reports were content analysed to code the number of unique preparations that each cook had made across five days, dishes that were not repeated. Each pantry, control and experimental, received a score for use of specific vegetables. Coding reliability for pantries ranged between .86 and .94.
Cooks’ longer-term use of vegetables
Personal interviews at baseline and at post-interview presented cooks with colour photographs of 27 vegetables and asked how often each had been served in the past week. A principal components analysis revealed that 24 of these items loaded heavily on a single factor, with reliability = .86. Each of the 15 pantries’ deviation at post, from predicted score calculated from baseline, served as the indicator of longer-term change in use of vegetables.
Children’s involvement in preparing dinners
This was assessed by asking mothers and their children, separately at baseline and at post-interview: ‘Did (child’s name/you) ever help with dinner preparations in the kitchen’, and if yes, ‘How often and when was the last occasion?’ Open-ended questions sought details about ‘the help (child’s name/you) provided most recently’. We designated mother-child pairs as collaborators when both reported that help had taken place in the past week and when both provided details about a recent occasion. Mothers and children provided an average of 1.7 codable details each. Other mother-child pairs were judged non-collaborators. Mothers’ and children’s reports about collaboration correlated (Gamma = .48, p = .005).
Dinnertime atmosphere at the table
Interviewers at baseline asked mothers and children, separately, about three possible distractions: ‘How often is the TV on where it can be heard or seen when eating dinner?’ ‘How often does anyone have their phone with them during dinner?’ and ‘How often does anyone listen to things through headphones while eating dinner?’
Answers could range from most of the time, sometimes, to almost never. Mothers’ and children’s reports at baseline were combined into a single index, even though electronic incursions sometimes intercorrelated poorly (not surprisingly, since the use of one device at dinner might often displace interference from other devices). For this analysis, families that seldom dined together at home were excluded.
We intended that our measure of electronic ‘presence’ would invite reports of regular or typical media distractions. Questionnaire items probably overlooked occasions when a digital medium can contribute positively to family atmosphere: for example, when a phone is fetched to settle a conversational curiosity by Googling the answer, or when family members cluster around the television to share in a special event during a meal (Fishel, 2015).
Family dining together
Mothers and children were asked at baseline how often the family ‘sits together, around the same table for dinners during weeknights’, and how often they ate ‘dinner at home during a typical week’. Mother-child pairs where either respondent said the family ‘almost never’ ate together, or ate outside the home four or more times a week, were treated separately in analysis.
Results
To provide context for the current findings about secondary users, we outline the results of the randomised field trial from which present data are derived. VeggieBook’s electronic capture of users’ interactions showed that household cooks created an average of 7 collections of recipes and 4 sets of Secrets to Better Eating, during their first 4 weeks of access to the app. Their children, during this time, created an average of 4 of their own collections of recipes and one set of Secrets, accessing VeggieBook separately through their own Gmail accounts. Once created, collections of recipes or Secrets could be viewed at any time or modified.
During the initial 4 weeks of the field trial, cooks in the experimental pantries began to incorporate more vegetables into meals and snacks. The median score for the nine app pantries was 38% greater than the median score for the six control pantries (N = 15, p = .03), based on preparations that used the most recent week’s vegetables offered by pantries.
On a delayed measure, 6–7 weeks after the trial’s supplementation of pantry offerings to experimental and control sites had ended, cooks in experimental pantries were using significantly more of 24 diverse vegetables than cooks in control pantries.
Cooks in experimental pantries also volunteered that they were gaining confidence in the kitchen, 66% compared to 4% among controls (Clarke et al., 2019).
Collaboration in the kitchen by children
Of central interest in this study was whether VeggieBook drew children more closely into their family’s food culture, even though the app’s content had been aimed at their mothers. Did collaboration preparing dinners increase in experimental families more than controls, prompted perhaps in part by the fact that more than 7 out of 10 children created at least one collection of their own selected recipes, and 4 out of 10 created at least one set of Secrets?
The presence of VeggieBook increased children’s involvement in household dinner preparation. Table 1 compares control families and experimental families on rates of collaboration during the past week. Post-data were collected 6 to 7 weeks after our special distribution of fresh produce had stopped, 10 weeks after baseline.
Percentage of mother-child pairs reporting kitchen collaboration with dinner, by experimental condition and time of interview.
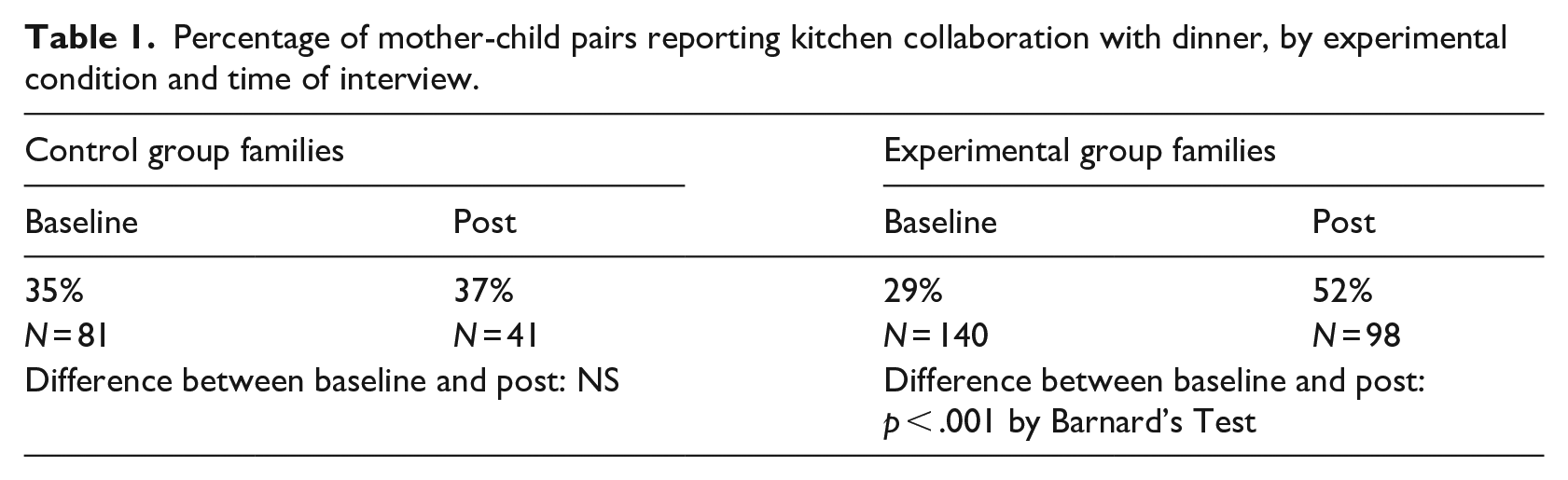
As shown, about one out of three pairs of mothers and children in control-baseline families (35%) and in control-post families (37%) agreed that kitchen collaboration had taken place. Experimental families showed a slightly lower level at baseline (29%). In contrast, collaboration jumped to more than half (52%) among the experimental app families 10 weeks later, a statistically significant gain not found among control families. The relative rate of collaboration among experimental pairs rose by 79%.
There was also a more subtle way in which kitchen collaborations grew. At baseline, girls were more likely to be involved than boys, by a 3:1 margin. But, with the app in the household, at post-interview boys were as likely as girls to start helping (X2 = 10.49, df = 3, p = .015). This suggests that the app recruited boys, unlikely kitchen-helpers, and thereby widened the family discourse about food.
Importantly, it is not likely that attrition between baseline and post interviews distorted these results. This is because the retained sub-sets of control and experimental families interviewed at post were similar to levels of collaboration within their total groups at baseline: 34% collaboration among control families (compared to 35% overall at baseline) and 31% collaboration among experimental families (compared to 29% overall at baseline).
Role of dinnertime atmosphere in creating new mother-child collaborations
As Table 1 shows, the field trial with VeggieBook retained 98 experimental families by the study’s end; 68 of these mother–child pairs had not been collaborative at the start (this number is not shown). Table 2 shows the influence of dinnertime atmosphere on whether these previously non-collaborative families became collaborative. We excluded 14 families that seldom ate together or frequently dined away from home (analysed separately below).
Conversion of no cross-generation collaboration homes into collaboration homes, by level of mealtime exposure to electronic media (experimental households).

Table 2 shows that our expectations about the adverse effects of electronic media were confirmed. Levels of media were divided into four categories with as near-equal numbers of cases as possible. As levels of media distraction increased, the likelihood of children being recruited into help with dinner decreased steadily, starting at a high of 67% conversions and dropping almost fourfold to a low of 18% in a steady decline. These are the percentages of non-collaborators at baseline who became collaborators. The negative correlation (Gamma) between electronic distraction and conversion = -.48, p < .01. Families at level 1 with ‘none or little’ exposure had effectively banned electronic media from tableside, whereas families at level 4 oscillated between ‘sometimes’ and ‘most of the time’.
Another benchmark for comparison is just as revealing. Among the 14 families who frequently dined separately or away from home (not included in Table 2), the rate of conversion to collaboration was 43%. Because of their dining habits, these families suffered from a structural handicap for enjoying the benefits from adult–child collaboration, relatively speaking. Yet, they scored a greater increase in kitchen partnerships from VeggieBook than households that dined together regularly, but usually in the company of electronic devices (among level 3 and 4 families in Table 2). See Supplemental Material for analyses of alternative explanations.
Discussion
Findings from this project offer two kinds of lessons. One is about a nutrition app for low-income cooks and the advantages to be reaped by inviting another household member, a child in our case, to use the app through his or her own portal. See Supplemental Material for discussion of benefits from recruiting kitchen collaborations. A second and more general lesson concerns the rewards that other apps, built for other health purposes, might add by embracing their appropriate secondary users.
Implications for the design of other apps
Several purposes could be served by inviting multiple users to a health app. In some cases, the secondary user may learn important lessons or acquire a new role, as was the case with children in our low-income families. Or, the secondary user may become better equipped to play a functional role in the primary user’s life – either by assisting the primary user with preventive steps, such as remaining vigilant about diet, substance use, or safe sex practices for example; or by helping manage an ongoing condition, serving as a lay care provider, or becoming a more empathic source of social support.
Abundant research in behavioural medicine testifies to the value of collaborative rather than individualistic approaches to disease prevention (Berge et al., 2012; Setkowski et al., 2020). Evidence concerning the importance of informal care providers and social support can suggest many themes which the content or functions of apps can engage with (Tan et al., 2020; Uslu-Sahan et al., 2018; Warshaw et al., 2019).
A health app builder who finds our experiences germane faces four considerations. First, who is the potential secondary user the builder seeks for the app? Second, what outcome or response does the builder desire from the secondary person’s app usage? Third, is it advisable to insert content or functions in the app specifically designed for the secondary user? Fourth, what factors are likely to moderate or mediate secondary users’ app experiences, either magnifying or curtailing secondary effects (MacKinnon et al., 2007)? In this study, our answers to these questions were, briefly: (1) children, ages 9-14; (2) collaboration with household cooks in preparing meals; (3) we did not add content specifically for children; and (4) intrusions by electronic media at mealtimes, occasions when children’s collaborations could be noticed and appreciated.
Possible future application
We illustrate the transfer of the discoveries reported here to a different realm of health apps: namely, women with breast cancer who are coping with the side effects from chemotherapy. Chemotherapy frequently leads to entire body hair loss, which traumatises many patients and discourages adherence to their treatment regimen (Dua et al., 2017). Apps have been built to help women with breast cancer cope with illness and treatment (Baik et al., 2020; Bender et al., 2013; Houghton et al., 2019), so it is reasonable to imagine an app focused specifically on helping patients manage their body image during treatment and afterwards.
Women under treatment for cancer experience distress and loss of well-being, often intensified by a lack of support from spouses or romantic partners (SRPs) (Brusilovskiy et al., 2009), who are often the patient’s primary reference-person for body image. Logically, therefore, an app designed to help women cope with hair loss could also invite SRPs as secondary users (to our knowledge, this kind of app remains unrealised). The aim might be to motivate SRPs to provide social support in relation to their partners’ illness generally (Lewis et al., 2019) and, specifically, to body image management. The app might also be built to engage significant others who are not SRPs, but we set this objective aside for the present discussion.
Ideas and interactive content intended for SRPs could be added to the app. These might include how to help a partner decide when to cut off thinning hair, how to help a partner select and be reimbursed for wigs, assisting in care for a hyper-sensitive scalp, how to help the patient talk about her illness or share body image concerns with close friends, the pros and cons of joining cancer support groups (for patients or for significant others), and much more. Thought might be given to whether primary and secondary users have access to each other’s content, and to whether simultaneous or individual app usage is encouraged. For a digital medium that pursued these issues, before smartphones were available, see Clarke and Evans (1998: 139–143).
The extent to which secondary app users step up to the plate with patient support might be moderated by mutual satisfaction in the patient-SRP relationship, recalled perhaps from before the cancer diagnosis (e.g., a couple’s satisfaction with decision making and means of conflict resolution, happiness with role responsibilities, and other aspects of committed relationships; Fowers and Olson, 1993). One might speculate that among couples with good relationships, SRPs would become heavier users of the app and more responsive to its ideas favouring social support and help with managing the patient’s body image, compared to couples with relatively poor relationships when illness struck. Field research evaluating the app might hope to find cases that deviate from this general rule. It would be gratifying to discover couples with poor relationships where, nonetheless, the app’s availability galvanised social support by SRPs where it was not expected.
Limitations
This case study has limitations. Importantly, it focuses on the secondary benefits of VeggieBook among clients of charitable pantries, where these families sourced food they could not afford to purchase. Perhaps the acute and collective stresses surrounding food insecurity (one out of six US families with children in 2017; Leung et al., 2020) contributed to our findings, limiting their applicability to apps aimed at more advantaged health markets.
Sizable numbers of households were studied here, drawn from clients of 15 pantries, but they were a convenience sample. And, although pantries were randomly assigned to control or experimental conditions, limitations arise from selection criteria. All participants had at least one 9- to 14-year-old child; all households contained two adults, usually parents; all household cooks were mothers or grandmothers. Studying the use of a food app among children of different ages might have yielded different results. It may be that in single-parent households, different from most of ours, the inclusion of children as app users would be harder to achieve. During the study period, single-parent families accounted for 3 out of 10 households having children and below the poverty line in Los Angeles County, the site of our study (see https://kidsdata.org). Recruitment of a child as secondary app user may challenge paternal authority where fathers are principal cooks. Nationwide census data show that 3 out of 10 men with less than high school diplomas, a demographic that aligns with food pantries’ clientele, reported in 2016 that they do ‘some household cooking’, which included cleaning up after meals (Taillie, 2018).
Another limitation of this study is that it did not directly compare households that were given a portal for children against households where children were not given their own portal. Thus, the benefits documented here for inviting secondary app users remain conjectural, which is one reason why this report is labelled a case study.
Finally, while training mothers and children in the mechanics of app usage we focused on the sign-in protocol and navigational issues and abstained from guidance about cooking or food use. Nonetheless, our attention to clients may in itself account for some of the results. Most apps, including health apps, are released to the public without much, if any, guidance about their features. This lack of attention to human factors has been criticised by some developers in the digital community who have noted gaps between the opportunities afforded by cheap broadband computing versus meagre positive impacts on users’ lives (Toyama, 2015).
Conclusion
We invite other health app developers to ponder whether multi-use app design might add a significant benefit to their outcomes-of-interest. Smartphone use has been blamed for corroding empathy, by substituting preoccupation with screen displays for face-to-face communication (Turkle, 2015). As a counterweight, building health apps that connect users with their social support system can invigorate community, helping prevent illness and manage disease through collective action. Such possibilities deserve greater attention than they currently receive.
Supplemental Material
sj-docx-1-hej-10.1177_00178969211049380 – Supplemental material for Cooking app engages kids as well as moms: Inviting secondary users into health outreach
Supplemental material, sj-docx-1-hej-10.1177_00178969211049380 for Cooking app engages kids as well as moms: Inviting secondary users into health outreach by Peter Clarke, Deborah Neffa-Creech and Susan H Evans in Health Education Journal
Footnotes
Acknowledgements
We thank Michael Flood at the Los Angeles Regional Food Bank, collaborating pantries and their clients for their time and insights about VeggieBook. We also thank the project’s field staff, interviewers and software engineers who helped us build the app.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article. This project was supported by Agriculture and Food Initiative Grant no. 2012-68001-15952 from the USDA National Institute of Food and Agriculture, Childhood Obesity Prevention: Integrated Research Education and Extension to Prevent Childhood Obesity.
Supplemental material
Supplemental material for this article is available online.
Notes
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
