Abstract
Keywords
Introduction
Despite national declines, the teen birth rate in the United States is higher than in any other developed country.1,2 Compared with adults, teen parents and their offspring are at greater risk for poor economic and psychosocial outcomes, and children of teen parents are more likely to experience preterm birth, low birth weight, behavior problems, and an increased risk of becoming teen parents themselves compared with children of older parents.3,4 Although there are a number of primary prevention efforts that delay the onset of sexual activity, 5 many adolescents are still at risk of having an unintended pregnancy. 6 Nearly half of all 17-year-olds report having had sex, 7 and their knowledge and use of effective contraceptives is poor—especially for highly effective contraceptive methods. 8 Thus, interventions to improve adolescents’ access to comprehensive, confidential contraceptive information and services are essential. 9
Long-acting reversible contraceptives (LARCs), such as intrauterine devices (IUDs) and hormonal implants, are now recommended as first-line contraceptives for adolescents10,11 because they are highly effective, safe, have few side effects, and do not require maintenance after insertion. Despite these recommendations, less than 5% of teens currently using contraceptives are using a LARC method. 12 Many adolescents are not aware of LARCs, and providers often lack the time, comfort, and knowledge to provide accurate and effective LARC counseling to adolescents.8,13-17 There is emerging research on interventions that can improve adolescents’ attitudes and uptake of LARCs. For instance, the Contraceptive CHOICE study found that when adolescents are offered appropriate counseling and cost is removed as a barrier, 61% to 69% chose a LARC method. 18 Another recent randomized control study found that patient-centered, efficacy-based counseling results in increased uptake of highly effective methods including LARCs. 19 There is also some encouraging evidence that brief educational interventions can improve adolescents’ attitudes toward IUDs. 20 In addition, one study found, that at least among adult women, a computer-based intervention was effective in promoting the uptake of effective contraceptives such as LARCs. 21
Computer-based interventions are a preferred modality for sexual health education and risk assessment among adolescents.22,23 However, few studies have explored the use of computerized interventions to improve contraceptive knowledge and uptake among adolescents.24,25 The purpose of this study is to examine the extent to which use of an interactive, iPad-based mobile health application (app) can improve adolescent girls’ knowledge of contraception and their intent to use more effective contraception methods, including LARCs.
Methods
App Development
Focus groups, interviews, and iterative usability testing sessions with adolescents and providers were conducted to ensure that the content and messaging was relevant, engaging, and youth friendly and that it would facilitate an individualized counseling approach appropriate for adolescents. We conducted a series of 8 focus groups with approximately 6 to 8 adolescent girls (15-18 years old) per group (6 with Latina youth and 2 with multiple ethnicities). Youth expressed enthusiastic interest in using touch-screen tablet computers or iPads to explore information about contraceptive options over traditional health education formats such as brochures. They expressed a great deal of interest in using the app because they felt it was private and they could explore topics on their own time without feeling like they were “being judged” by a health professional. Youth provided input on common misconceptions about sexual health and contraception and suggested using a “myth-busters” style game to assess if common misconceptions about sexual health were a myth or fact. Youth reviewed existing computer-based contraception education tools on several leading websites and reported that these sites seemed more suited for adult women with more education and experience. Youth also felt that the number of contraceptive options presented on websites was overwhelming and suggested presenting methods in a time-line format based on duration of action. Furthermore, they felt that they would not seek out these websites on their own and expressed a preference for being able to use a tablet computer confidentially, in a school-based health center (SBHC) or clinic setting. Adolescent medicine specialists and clinicians from each of the three SBHCs were also interviewed during the development of
Description of Health-E You
The
First, the app provides a brief description of the module and consents the user to participate. It then assesses sexual health knowledge using an interactive truth versus myth game (see Table 1 for the list of knowledge assessment items). Correct answers to the truth versus myth statements are then presented to the user as short, easy-to-read explanations. Next, the app assesses the user’s individual contraceptive needs and use. It then presents a visual continuum of effective contraceptive options based on duration of action and efficacy and the user can select each method to get basic information about the method, its use, and pros and cons (Figure 1). The user also answers a brief series of questions about acceptability of common side effects and is screened for possible contraindications (via CDC medical eligibility criteria). The user can also select different video vignettes featuring young women discussing their experiences with a particular method. 28 Throughout the module, the user is given individually tailored messages. For instance, if she indicates that she is using an ineffective contraceptive method (e.g. withdrawal or the rhythm method), she is warned that many women become pregnant with this method and is directed to explore more effective contraceptive methods. The app also emphasizes dual use of contraception and condoms to protect against unplanned pregnancy and sexually transmitted infections (STIs) and provides information about emergency contraception. At the completion of the module, sexual health knowledge is reassessed using a true/false format, and the user is asked to select the contraceptive method she would like to use in the future. The module concludes with a brief, 5-question app acceptability survey with questions such as, “I found this program easy to use” and “I felt comfortable answering questions on a computer like this,” and a few basic demographic questions. Information about contraceptive choice is then shared with the user’s provider via secure e-mail so that she may be offered her preferred method during a clinical visit.
Knoweldge Assessment Items (Myth vs Fact).

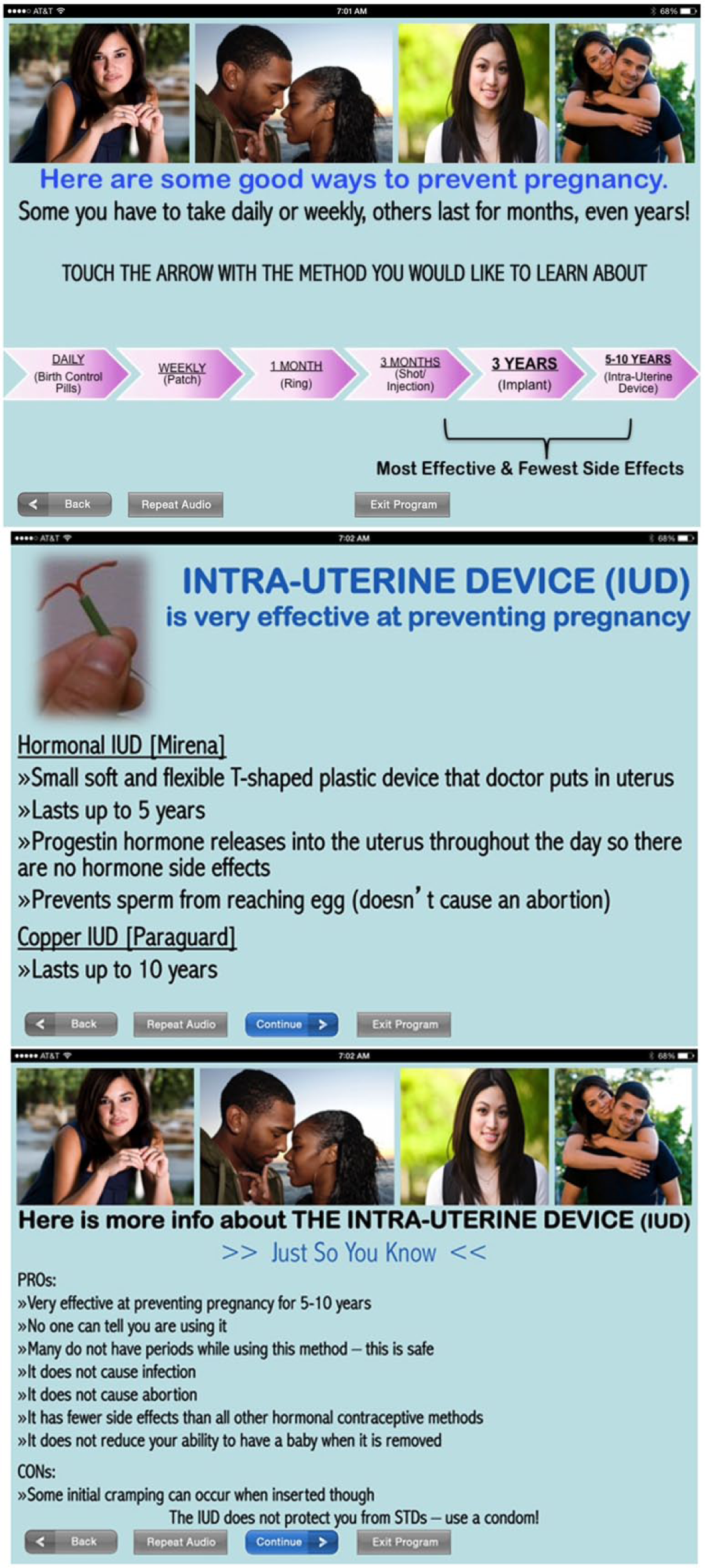
Contraceptive Options.
Procedures
This study examined the impact of
English-speaking girls who presented for care at the SBHCs used the app prior to their clinical encounter. Data were collected in real time and stored in a back-end database with no patient identifiers. Waivers of parental consent were obtained to protect adolescent confidentiality. Informed consent for adolescent participants was obtained via the app. The study was approved by the internal review board at the University of California, San Francisco.
Results
A total of 120 girls used the
Demographic and Background Information About Participants
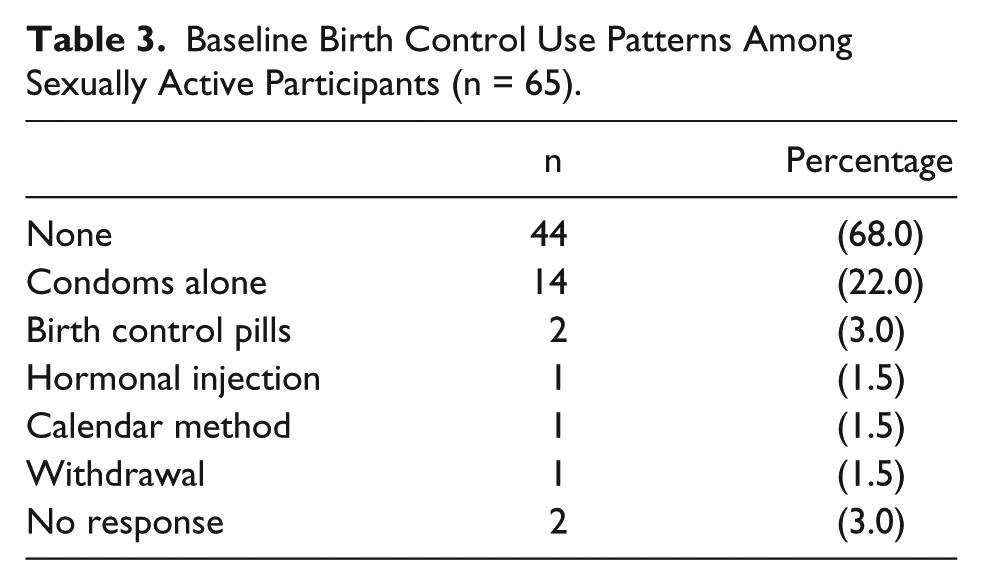
The sample was ethnically diverse (see Table 2). The mean age of participants was 16.4 years (range 12-18 years). More than half of the participants (54%) reported currently being sexually active. Of those sexually active participants, 68% were using no contraception (Table 3). Among those who reported they were using contraception, 22% were using condoms alone, 3% were using birth control pills, 1.5% were using a hormonal injection, 1.5% were the using calendar method, and 1.5% reported using withdrawal. The remaining 1.5% did not specify the method they were using.
Baseline Birth Control Use Patterns Among Sexually Active Participants (n = 65).

Sexual Health Knowledge, Contraceptive Use, and Intentions
There were significant improvements in pre-post sexual health knowledge assessed at the beginning of the app and at the end of the app. The mean proportion of correct answers at baseline was 58% (range = 14%-86%; SD = 0.3), which improved significantly at posttest to 79% (range = 29%-85%; SD = 0.3;
Among the sexually active participants, only 26% (n = 17) reported use of an effective contraceptive method at baseline. Of those, the majority (n = 14) reported only using condoms. After using the app, 66% (n = 43) reported intentions to use an effective method of contraception (p < .001), and 25% indicated that they would use dual contraception (ie, a hormonal method or LARC plus a condom) (Table 4).
Baseline Birth Control Use Versus Intention for Future Use After Using
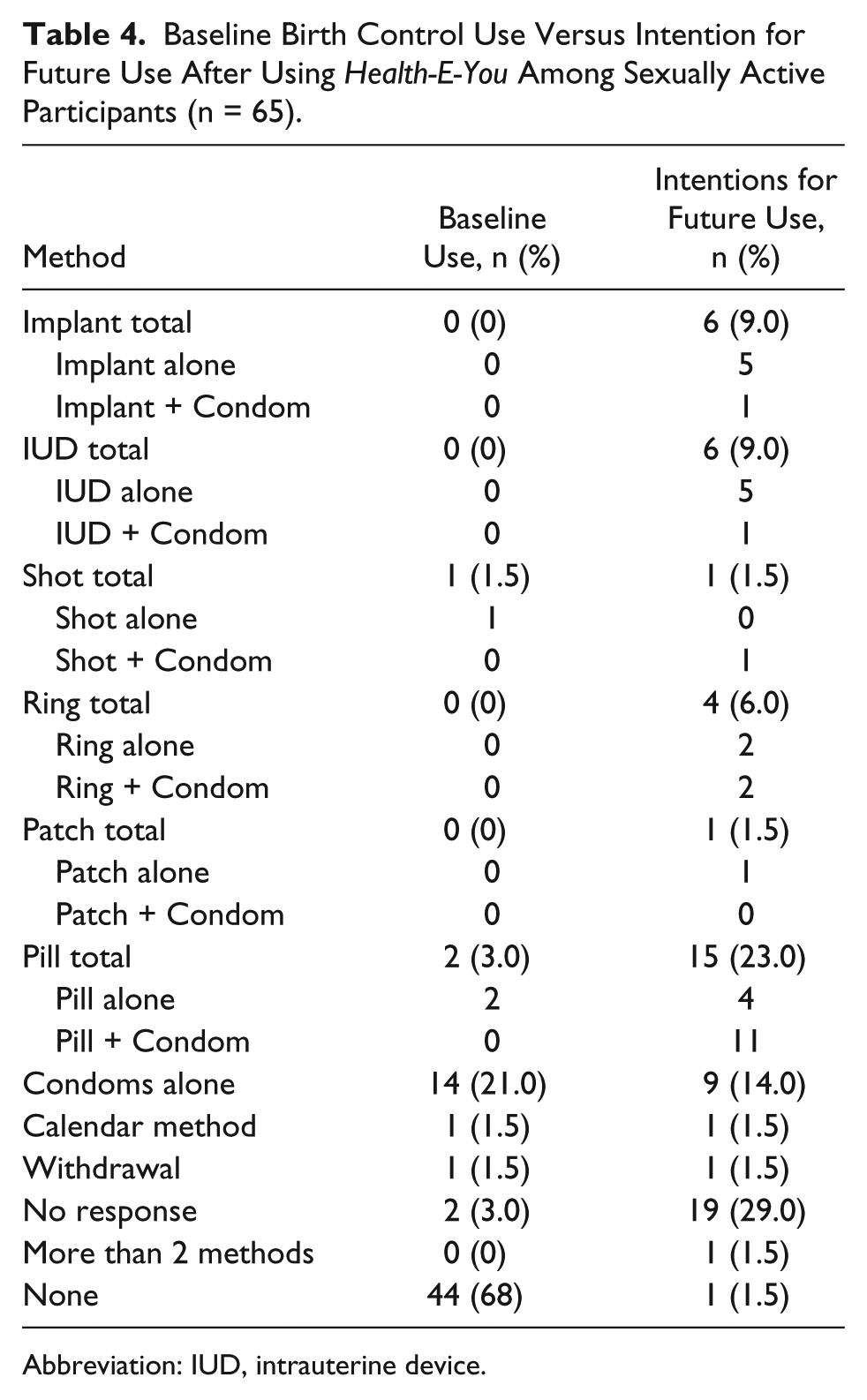
Abbreviation: IUD, intrauterine device.
The most popular method was the birth control pill, with 23% of participants indicating future intention to use this method. The pill was followed by condoms (14%), the IUD and implant (each at 9%), vaginal ring (6%), patch (2%), and shot (2%). None indicated intention to use emergency contraception; 3 participants indicated that they would use an ineffective method such as withdrawal or rhythm method; and 1 participant indicated that she would use more than 2 methods (pill, patch, ring, condoms).
Of the 44 participants who reported that they were sexually active and not using any contraception prior to using the app, 28 (64%) reported that they would use an effective method after using the app. The participants (both sexually active and non-sexually active) who expressed intent to use a LARC method in the future were only slightly older on average than the overall study sample (mean age 16.6 vs 16.4 years); the majority where white, all were sexually active, and 33% were using some form of contraception prior to using the app (Table 5).
Characteristics of All Participants Who Indicated Intention to Use LARC (n = 12) Versus Non-LARC Methods (n = 37).
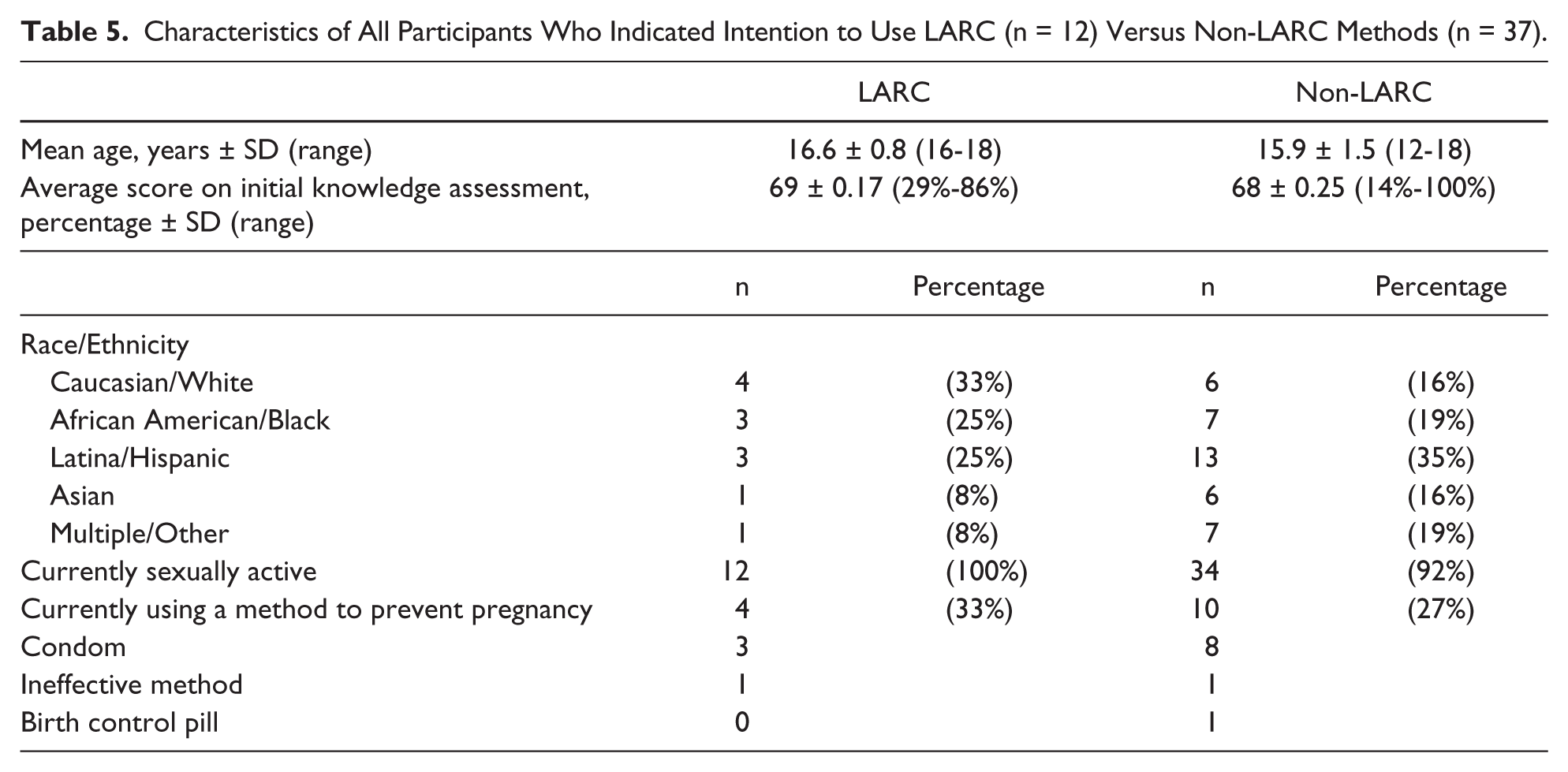
Discussion
This study explored the ability of an interactive, individually tailored app,
This app increased sexual health knowledge and influenced adolescents’ intentions to use an effective or more effective method of contraception. Baseline contraceptive knowledge assessment revealed that, on average, users answered 4 out of 7 questions correctly prior to using the app, indicating important gaps in contraceptive knowledge among the study participants. After using the app, the mean correct scores increased significantly, suggesting that
There are a number of limitations to this study. This study included a relatively small sample of 120 participants, of whom 65 were sexually active. Because of this, our analysis focused on sexually active participants who were at greatest risk for pregnancy. This study was not able to assess the influence of
Author Contributions
KPT conceptulalized study design, development of the app, and data collection methods. VVM was the lead author in writing the manuscript. KPT and VVM both contributed to the conceptualization of this manuscript, conducted data analyses, and provided approval of the final manuscript.
Footnotes
Acknowledgements
We would like to thank the participating School Based Health/Wellness Centers in the Los Angeles and Vallejo Unified School Districts and Kimberly Uyeda, MD, MPH Director, Student Medical Services at LAUSD. Special thanks to our partners who were instrumental in pilot testing the app: Maryjane Puffer, BSN, MPA, and Sang Leng Trieu, DrPH, from the Los Angeles Trust for Children’s Health, and Rebecca Dudovitz, MD, MSHS, from UCLA; and our colleagues Loris Hwang, MD, Claire Brindis, DrPH, Lauren Hartman, MD, and Felicia Rodriquez who provided input on the development of the app.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was partially funded through a PCORI Reducing Disparities Award No. AD-1502-27481, the Hellman Fellowship Fund, and Grant T71MC00003 from the Maternal and Child Health Bureau, Health Resources and Services Administration, US Department of Health and Human Services.

