Abstract
Background:
In primary care (PC) clinical, healthcare utilization, and financial outcomes associated with Lifestyle Redesign® Occupational Therapy (LR-OT), a framework that incorporates healthy habits into daily routines, are not well documented in the United States.
Purpose:
(a) Compare clinical outcomes, healthcare utilization, and associated cost differences between patients who received LR-OT and a control group. (b) Assess the investment required integrate LR-OT into PC.
Method:
LR-OT was integrated into a safety-net PC clinic. In a hybrid effectiveness-implementation clinical trial (#NCT03293914), clinical (glycated hemoglobin A1c [HbA1c], blood pressure, cholesterol, and body mass index) and utilization (outpatient, emergency department [ED], hospital visits) data were extracted from medical records of provider-referred adults with diabetes (HbA1c ≥ 9.0%) who were willing to make lifestyle changes.
Results:
Of 155 referred patients, 142 were randomized to LR-OT (n = 73) or a control group (n = 69), and 42 completed eight LR-OT sessions within 6 months. Underpowered clinical outcomes indicated no significant change, with aggregated trends suggesting LR-OT supports sustained cardiometabolic improvement. Savings of $250,518.96 is attributed to LR-OT, driven by significant decreases in ED visits (p = .03) and hospital days (p = .03), despite nonsignificant increases in outpatient utilization. The projected cost-benefit of integrating a full-time LR-OT in PC is $352,326.72 with a 236% return on investment.
Conclusion:
Clinical trends and significant reductions in acute care services drove healthcare-wide cost savings, demonstrating clinical and financial value of integrating LR-OT into PC.
Introduction
The United States (U.S.) healthcare system is experiencing a costly demand for primary care (PC), exacerbated by a shortage of PC providers (Han et al., 2019). Serving as the primary contact within the healthcare system for individuals with chronic conditions, such as diabetes (Spann, 2006), PC providers are challenged to meet their patients’ complex health and psychosocial needs with limited visit times (Linzer et al., 2009). Underinsured and underresourced non-White individuals with chronic conditions experience unfavorable health outcomes driven by gaps in healthcare access, inadequate PC prescription and diagnosis management, and lifestyle-related struggles (Voura et al., 2024), leading to an increase in preventable emergency healthcare utilization (Dashputre et al., 2020).
Team-based care (TBC) is a healthcare delivery strategy (Wagner et al., 2017) utilized internationally in patient-centered medical homes to promote collaboration among healthcare providers, enhance patient education and engagement, ensure evidence-based practices, and support comprehensive, coordinated care to improve health outcomes (Proia et al., 2014). TBC is a promising approach to enhancing healthcare service delivery with evidence linked to improved patient outcomes (Bray et al., 2005; Kravetz & Walsh, 2016; Shi et al., 2023), decreased medical errors (Shi et al., 2023), improved medication adherence (Bray et al., 2005), fewer hospital days (Shi et al., 2023), enhanced provider productivity, and enhanced provider satisfaction (Helfrich et al., 2014).
Medical management of chronic conditions, such as diabetes, requires continuous monitoring and adherence to health behaviors, which can be optimized through TBC. Although occupational therapy (OT) practitioners are broadly trained in health promotion, behavior modification, illness prevention, and tailored intervention delivery for populations with or at risk of chronic conditions, they remain underrepresented in U.S. PC teams (Bolt et al., 2019; Dahl-Popolizio et al., 2023, 2017; Halle et al., 2018), while in Canada, OT practitioners are integrated into healthcare settings and working to enhance accessible health promotion and prevention services within clinics and among community members (Donnelly et al., 2016).
OT practitioners help individuals achieve greater independence and quality of life by promoting meaningful daily activities, potentially reducing the long-term burden on healthcare systems (Dahl-Popolizio et al., 2023). For example, Lifestyle Redesign® (LR®-OT), an OT intervention framework focused on incorporating healthy lifestyle changes into daily routines for patients with chronic conditions, has shown improvements in clinical outcomes (Pyatak et al., 2019), quality of life (Pyatak et al., 2022), and chronic pain (Uyeshiro Simon & Collins, 2017). However, there is limited documentation of the broader impact of LR-OT’s integration into TBC PC on the health system's service utilization, including outpatient, specialty, emergency department (ED), and hospitalization costs.
This study investigated the impact of integrating LR-OT services within a patient-centered interdisciplinary TBC PC clinic. Its primary aim was to compare differences in clinical outcomes and healthcare utilization between patients who received LR-OT and those who did not. The secondary aim of this study was to assess the associated investment required to implement LR-OT and evaluate the cost-benefit of including LR-OT in PC. Findings of this hybrid effectiveness-implementation study could inform policy decisions on resource allocation and guide the integration of LR-OT programs into PC worldwide, especially in countries with universal healthcare systems (e.g., Canada, Germany, Australia) or healthcare settings affiliated with academic institutions.
Method
Study Design and Setting
The study was implemented in a U.S. safety-net PC clinic within a large urban public health system, serving approximately 14,000–16,000 patients annually, predominantly insured by Medicare or Medicaid. With a strong TBC culture, the PC clinic employed physicians, physician assistants, nurses, medical assistants, clerks, a social worker, a clinical pharmacist, and a psychiatry resident. Participants were randomized to receive LR-OT services or to serve as a no-contact comparison group, using a randomized consent design (Lin & Lui, 2002), to pragmatically assess the overall effectiveness of LR-OT under real-world conditions that mirror usual care. This study followed CONSORT guidelines and was approved by the Institutional Review Board of the University of Southern California, which granted a waiver of consent to extract participants’ relevant clinical and demographic data from the electronic medical record (EMR). No interim analyses or stopping guidelines were specified because the intervention posed minimal risk. No adverse events related to the intervention were reported. The trial registry number is #NCT03293914 (ClinicalTrials.gov, 2017).
Participants
Recruitment of participants took place through referrals from empaneled providers and clinical pharmacists of current clinic patients meeting the following eligibility criteria, developed in collaboration with clinic leadership, OT practitioners, and researchers, based on clinic needs and intervention capacity. These included: (a) diagnosis of diabetes; (b) most recent glycated hemoglobin A1c (HbA1c) value ≥ 9.0%, or no HbA1c within the previous 12 months; (c) age 18–75 years; and (d) per referring provider's judgment, willing to make lifestyle changes. Exclusion criteria, as determined by the referring provider, were diagnoses limiting participation in major life domains, including (a) current, untreated substance-use disorder, (b) behavioral health disorders (e.g., schizophrenia or bipolar disorder), or (c) moderate to severe cognitive impairment. Our original target sample size was 120 based on pragmatic caseload management considerations. The intervention was stopped when the sample reached 155, accounting for approximately 20% attrition and detecting a medium effect (d = .05) with 64 patients per group (Biau et al., 2008), as caseload management proved feasible.
Randomization
Following confirmation of eligibility via EMR chart review, participants referred to the study were randomly assigned to (a) be offered LR-OT services or (b) serve as the no-contact comparison group, using a simple randomized consent design to balance the need to follow usual clinic procedures (e.g., not requesting informed consent from patients not offered LR-OT services) while including a randomized comparison group to assess outcomes rigorously. The research team used a computer-generated allocation sequence that clinical staff did not have access to. Clinical staff were not blinded to group allocation to ensure transparent communication with patients during routine care.
Intervention
Participants randomized to the comparison group continued to receive usual care with no study-related contact. Patients who were randomized to LR-OT and accepted the referral were introduced to the LR-OT interventionist via warm hand-off (personal introduction or direct connection) from a referring provider and completed informed consent, pre- and postsurvey measures, and LR-OT sessions. LR-OT participants had access to usual care and were offered up to eight individual face-to-face 1-hr LR-OT sessions held every 2–3 weeks, which was determined pragmatically, based on the LR-OT caseload management capacity, with support from literature demonstrating the number of sessions that could support meaningful improvements in PC settings (Gonzalez et al., 2015). The treatment emphasized collaborative client-directed goal-setting, autonomy support, and the acquisition of knowledge and skills relevant to incorporating diabetes self-care activities and healthy lifestyle changes into daily routines.
The LR-OT interventionist was an English–Spanish bilingual faculty member employed by the university partner affiliated with this study. The interventionist had advanced training in LR, diabetes education, and motivational interviewing. The LR-OT was fully colocated for 0.5 full-time equivalent (FTE) (20 hr per week) within the PC clinic, with a designated treatment room, and collaborated closely with patients’ care teams through EMR messaging, documentation, and in-person discussions. Appointments were typically scheduled in coordination with patients’ routine PC visits to support standardized, patient-centered TBC.
Data Collection and Measures
Data collection began in October 2016 and ended in March 2019. All patients (n = 142) had clinical and healthcare utilization data extracted from the EMR for 12 months before and 13 months following their study enrollment date. Enrollment date was defined as the date when intervention group participants were referred to LR-OT. This was chosen rather than their randomization date so that the study period would best reflect participants’ exposure to treatment, as some patients were referred several weeks after randomization. Enrollment dates were imputed by the study's biostatistician for comparison group intervention participants, based on the average time between randomization and enrollment for LR-OT recipients.
Relevant background information, clinical outcomes (HbA1c, blood pressure [BP], cholesterol, and body mass index [BMI]), and healthcare utilization data, including PC clinic outpatient visits, specialty outpatient visits, ED visits, and hospitalizations, were extracted from the EMR through retrospective chart reviews. Data collected from EMR are outlined in Table 1. Participants in the intervention component completed pre- and postintervention surveys on health outcomes, behaviors, and psychosocial well-being, as previously reported by Pyatak et al. (2019).
Variable Definitions and Data Source.
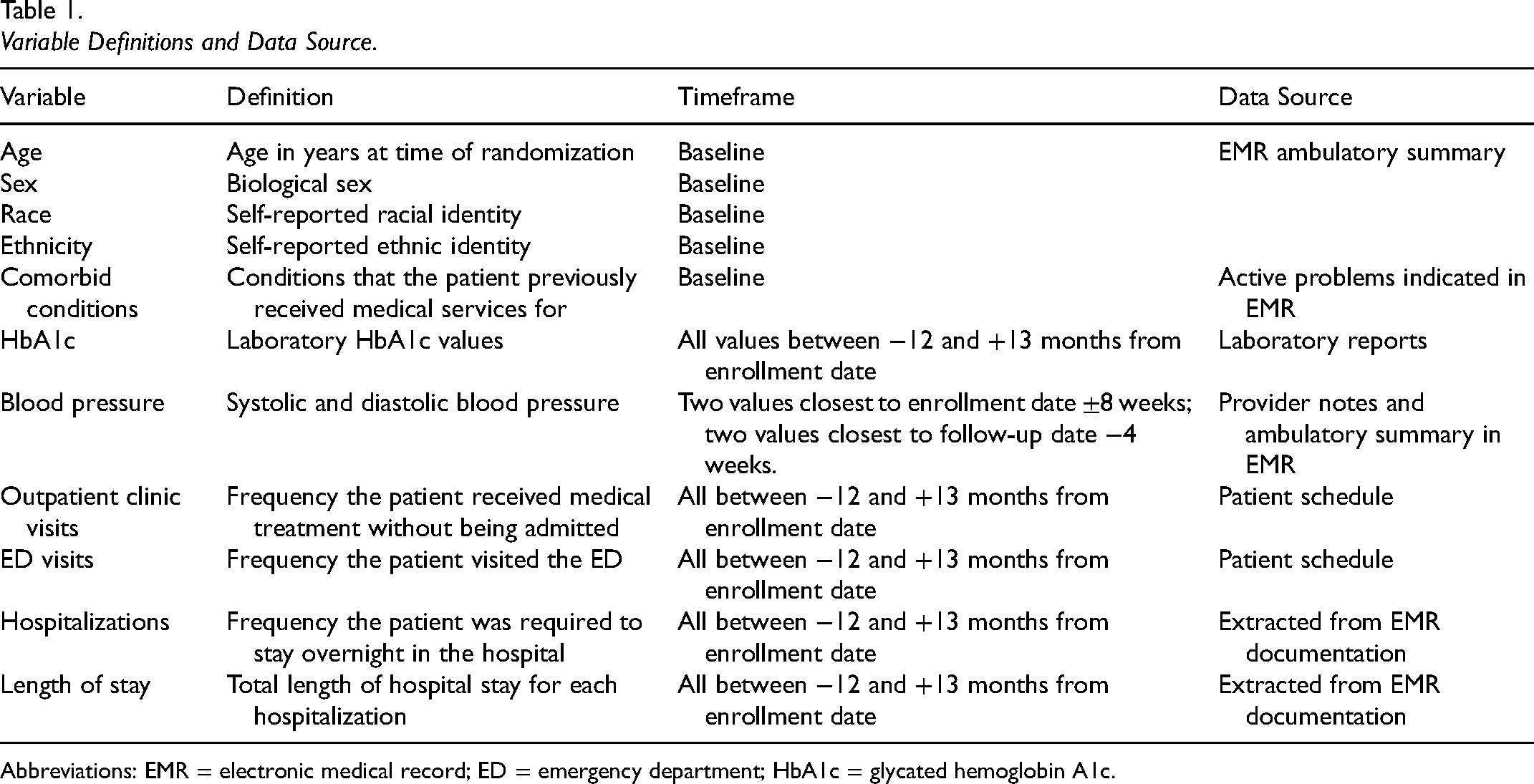
Abbreviations: EMR = electronic medical record; ED = emergency department; HbA1c = glycated hemoglobin A1c.
To conduct the healthcare cost analysis, we used total per capita cost averages of healthcare utilization attributable to diabetes from the Economic Cost of Diabetes in the United States in 2022 Supplementary Data (Parker et al., 2024), as these estimates capture the timeframe of the healthcare utilization in our study. This report utilized aggregated data from 2007 to 2022, sourced from a comprehensive list of national U.S. healthcare utilization, spending, and population health data sources, to calculate healthcare resource use and indirect costs attributable to diabetes (Parker et al., 2024). To conservatively estimate the cost of the 0.5 FTE LR-OT interventionist, we used the U.S. Bureau of Labor Statistics Occupational Employment Wages report (U.S. Bureau of Labor Statistics, 2020), which provided salary estimates for the Los Angeles metropolitan area in 2019. For the projected cost analysis, we used the most recent salary estimates for OT practitioners in the same area from the U.S. Bureau of Labor Statistics (2024) report. To estimate the cost of employee benefits, we utilized the 32% employer contribution as a benchmark, drawn from the California Health Care Foundation (CHCF) (2025), which provides comprehensive estimates of the proportion of an employee's salary typically covered by employer contributions to benefits.
Analysis
Primary Aim
To evaluate changes in health outcomes, PROC GLIMMIX (SAS, version 9.4, SAS, Cary NC) mixed effects regression model was used, including all available measurements for HbA1c, BP, cholesterol, and BMI. An indicator variable was used to specify whether the measurement occurred before or after the start of the intervention. Each outcome variable was modeled as a function of treatment, pre/post period, and an interaction term for treatment and pre/post period. A negative binomial distribution was specified, and the intercept was a random variable. The outcome of interest was a change in clinical outcomes (HbA1c, BP, cholesterol, and BMI) within the intervention group after exposure to the intervention.
To evaluate differences in healthcare utilization, Wilcoxon rank-sum tests (R Core Team, 2025) were performed on the mean change in utilization per person between the two groups for outpatient PC clinic, outpatient specialty, ED, hospital day, and hospitalization visits. To accurately estimate the impact of LR-OT on other healthcare services, LR-OT visits were excluded from the analyses, and missing data were not imputed; analyses were conducted with available cases. The change in the number of visits per patient was calculated by subtracting the respective healthcare utilization visits before treatment from those during treatment. The mean change score was calculated for both groups by averaging individual change scores across patients. A standard significance level of .05 was considered our detectable rate of change for all analyses.
Secondary Aim
To perform the cost analysis (R Core Team, 2025), the mean change in visits per person was multiplied by the sample size and the respective utilization cost estimates to calculate the total costs for each group. Hospitalizations (the number of times a patient was hospitalized) were excluded from the cost analysis to prevent overcounting. Instead, hospital days (the number of days a patient spent in the hospital) were incorporated to provide more accurate cost estimates. Cost savings were determined by subtracting the comparison group's total cost from the LR-OT group's total cost (including the projected cost of the clinical LR-OT salary and benefits), with the differences representing the financial impact of the intervention (i.e., the net cost of the intervention after taking into account the cost of delivering the intervention and its impact on overall healthcare utilization). Therefore, the return on investment (ROI) is based on the attributable observed cost savings and projected LR-OT salary and benefits.
Results
Participant flow is outlined in Figure 1. Of the 155 patients referred to the study, 13 did not meet the inclusion criteria and were excluded from randomization. Sixty-nine patients were randomized to the no-contact control group, and 73 to receive LR-OT services. The baseline demographic characteristics of treatment and control group participants are outlined in Table 2. Participants were 52.6 (±10.1) years of age and 65% women. The majority (71%) reported their ethnic identity to be Hispanic/Latino, 58% reported Spanish as their primary spoken language, and some were codiagnosed with hypertension (68%) and dyslipidemia (57%).
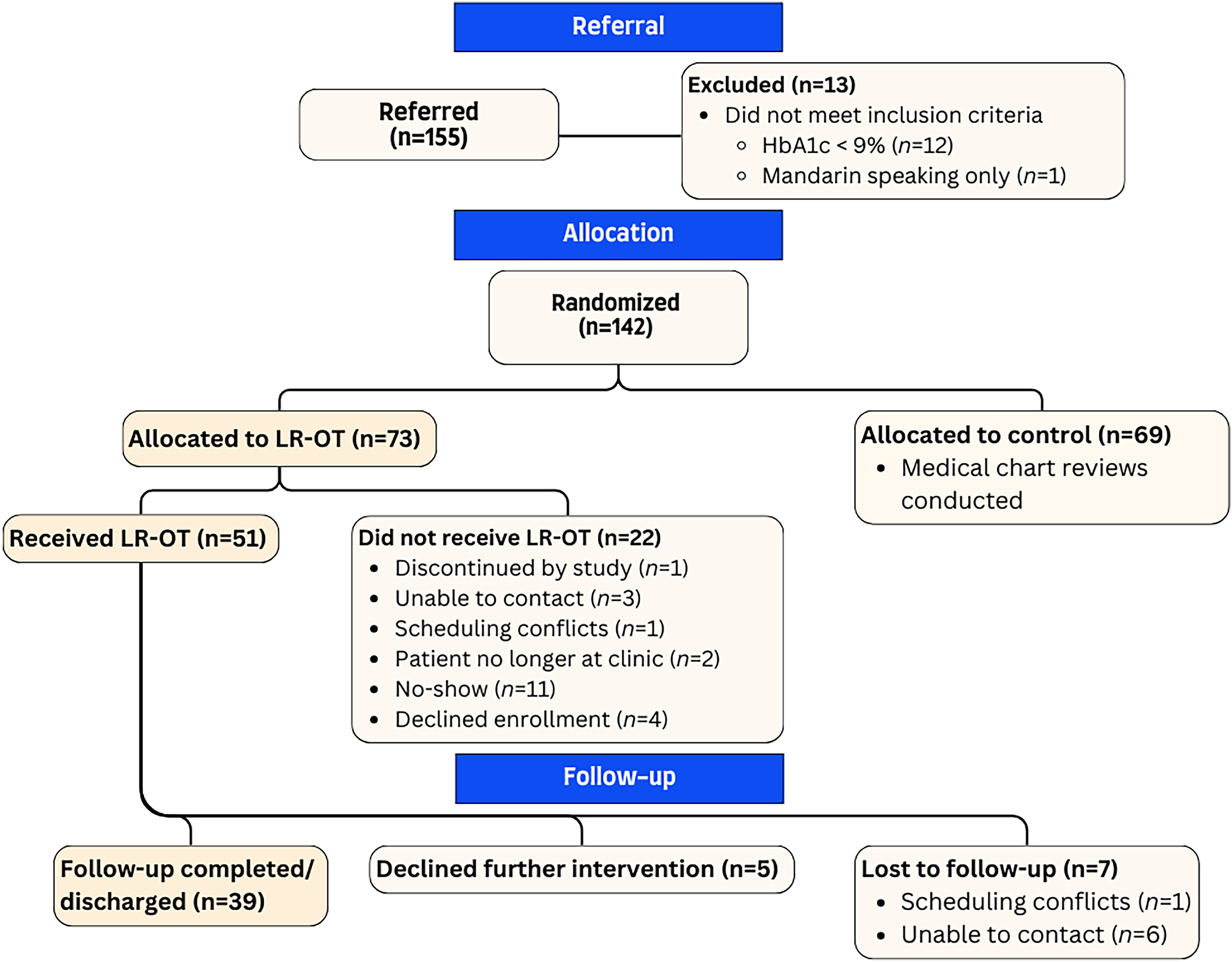
Patient flow chart.
Baseline Demographic Characteristics.
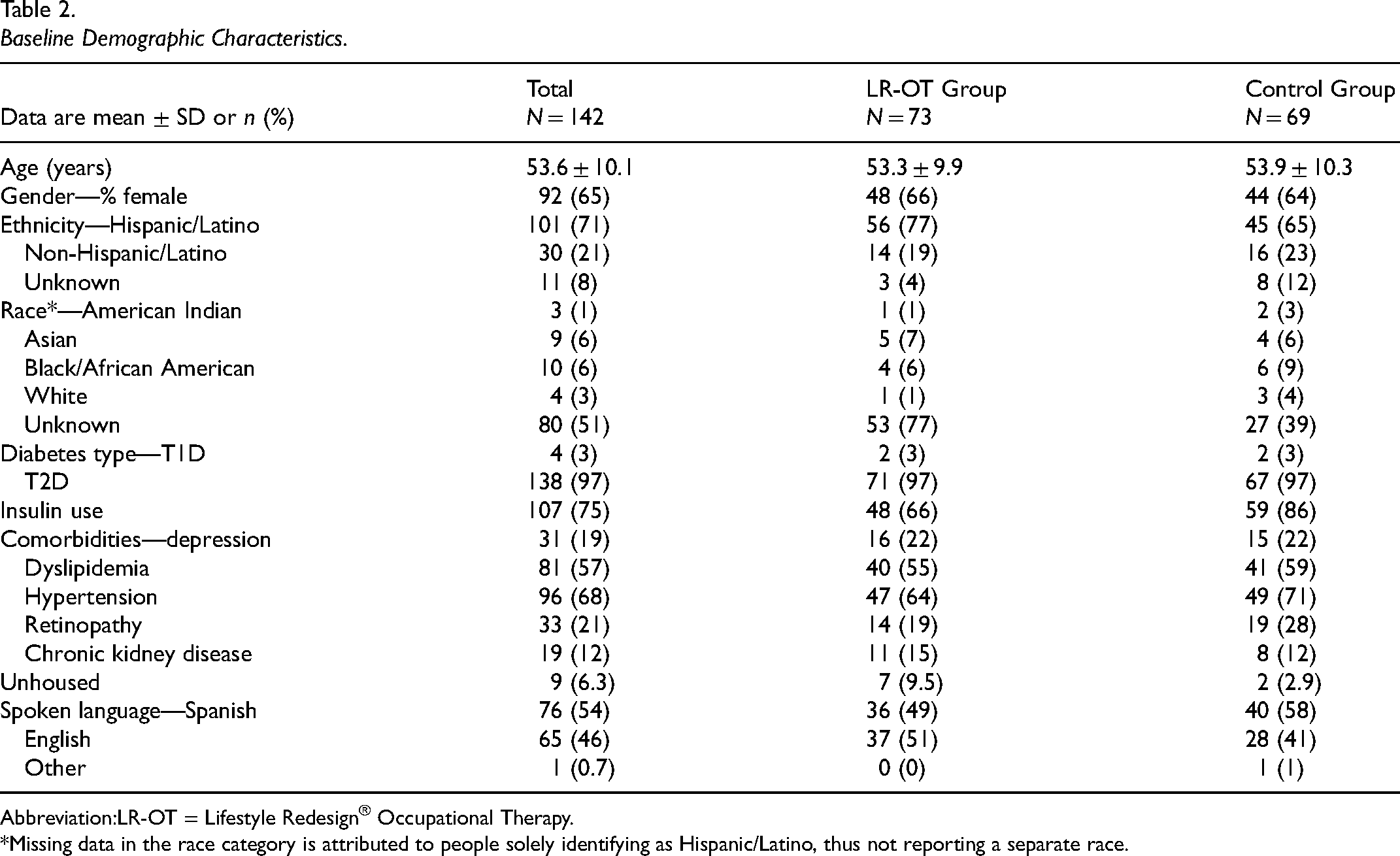
LR-OT = Lifestyle Redesign® Occupational Therapy.
*Missing data in the race category is attributed to people solely identifying as Hispanic/Latino, thus not reporting a separate race.
Among 73 participants randomized to the intervention, 51 agreed to LR-OT treatment (69.9%). These participants completed an average of 6.0 (±2.7) visits, with 26 (51.1%) completing the maximum allowed eight sessions. Excluding eight (15.7%) participants lost to follow-up after their initial evaluation, participants received LR-OT services for an average of 156 (±71) days, with the majority (82%) completing treatment within 6 months. Among participants receiving LR-OT, 305 of 478 scheduled visits (64%) were completed, 55 were canceled (12%), and 118 were no-shows (25%). In comparison, out of the 5,476 non-LR-OT clinic outpatient visits scheduled, 3,568 were completed (65%), 619 were canceled (11%), and 1,296 were no-shows (24%). Therefore, the likelihood of attending LR-OT visits was similar to that of attending clinic outpatient visits.
Primary Aim
Clinical Outcomes
The results indicated nonsignificant changes in health outcomes following the intervention across all variables (see Table 3). For HbA1c, a nonsignificant decrease was observed in the intervention group postintervention (ES = 0.32, p = .28). Similarly, systolic BP showed a nonsignificant reduction in the intervention group postintervention (ES = 0.69, p = .33), while diastolic BP also decreased nonsignificantly (ES = 0.35, p = .73). Regarding cholesterol, a reduction was observed in the intervention group after exposure to LR-OT; however, the sample size was insufficient to perform statistical testing. Finally, BMI increased nonsignificantly in the intervention group postintervention (ES = 0.35, p = .73).
Clinical Outcomes Mean (SD) of Person-Means by Treatment Group (ITT).
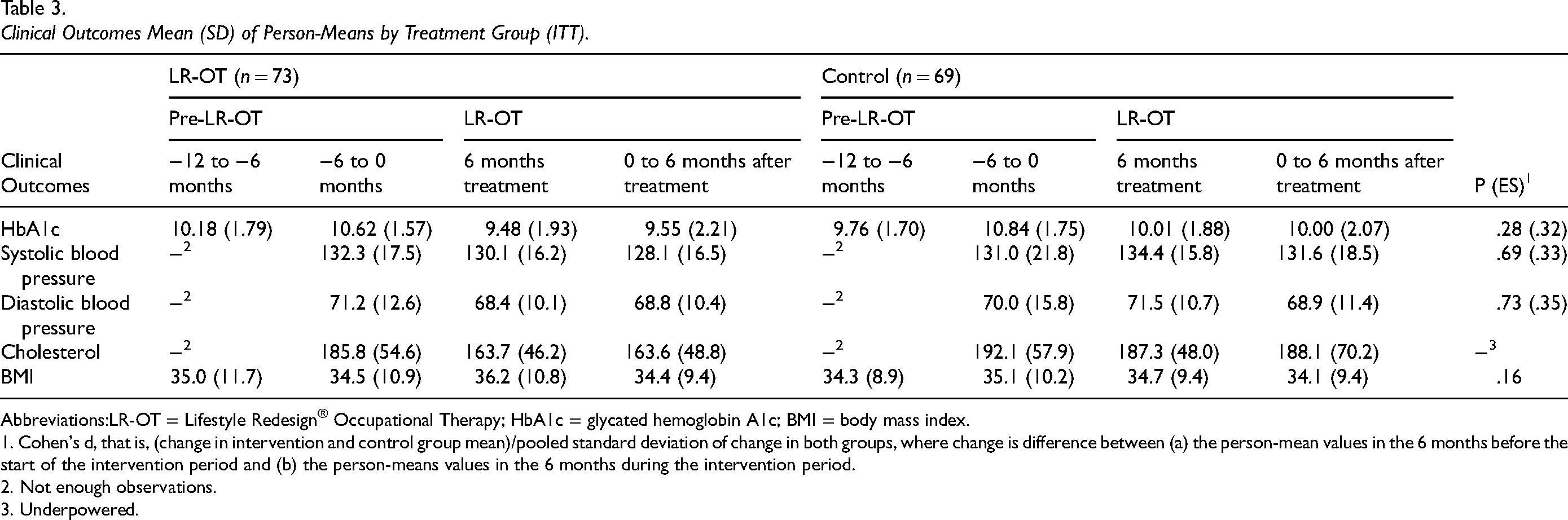

LR-OT = Lifestyle Redesign® Occupational Therapy; HbA1c = glycated hemoglobin A1c; BMI = body mass index.
1. Cohen's d, that is, (change in intervention and control group mean)/pooled standard deviation of change in both groups, where change is difference between (a) the person-mean values in the 6 months before the start of the intervention period and (b) the person-means values in the 6 months during the intervention period.
2. Not enough observations.
3. Underpowered.
Healthcare Utilization
Healthcare utilization analyses (see Table 4) revealed significant differences in care utilization between the LR-OT and control groups. When comparing the year after enrollment to the prior year, the LR-OT group showed a significant decrease in ED visits per person in contrast to an increase in ED utilization in the control group (−0.37 ± 1.89 vs. +0.25 ± 2.61, p = .03). Similarly, the LR-OT group had a decrease in the total number of hospital days in the year following enrollment versus the year before. In contrast, the control group had an increase in hospital days (−0.62 ± 5.75 vs. 0.75 ± 8.96, p = .03). Differences in the change in number of PC clinic outpatient visits (4.67 ± 3.57 vs. 3.57 ± 6.30, p = .22), specialty outpatient visits (3.60 ± 6.19 vs. 3.62 ± 8.31, p = .88), and hospitalizations (−0.11 ± 0.89 vs. 0.04 ± 1.74, p = .11) per person in the year following enrollment versus the prior year between the control and LR-OT groups were not significant.
Healthcare Utilization Differences Between LR-OT and Control Group From BSL to FU.
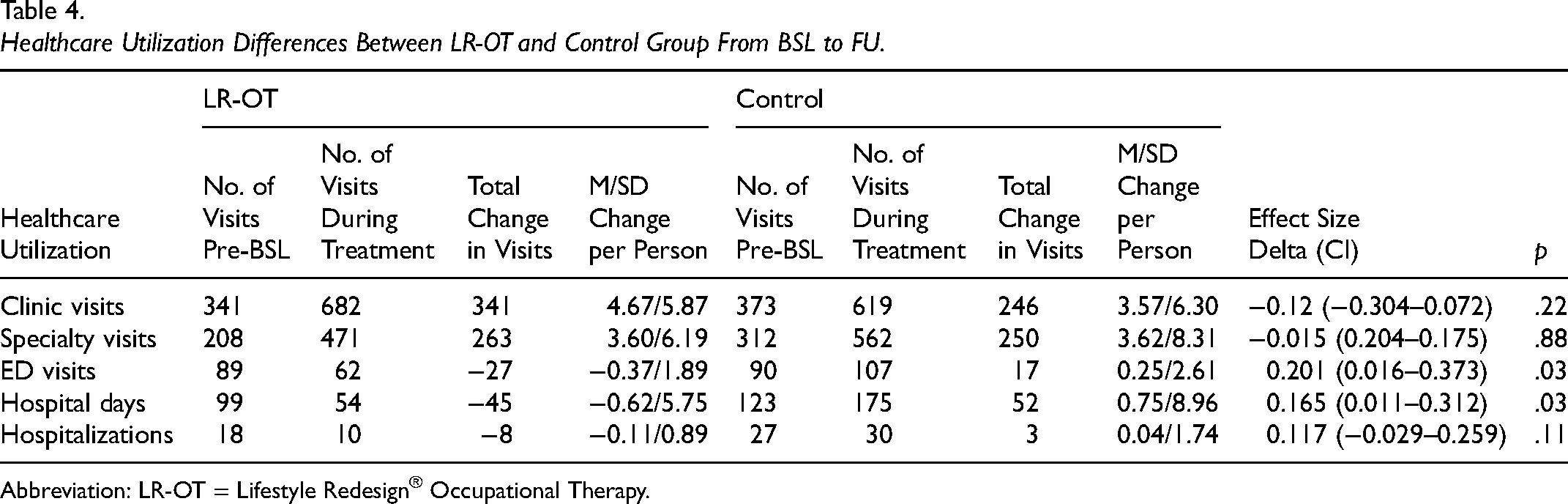
Abbreviation: LR-OT = Lifestyle Redesign® Occupational Therapy.
Secondary Aim
Cost Analysis
The cost analysis for integrating LR-OT services into PC is presented in Table 5. Although the LR-OT group demonstrated a nonsignificant increase in clinic outpatient visits per person, the significant decreases in ED visits and hospital days resulted in estimated savings of $250,518.96 USD ($3,431.77 USD per person) associated with the LR-OT intervention, indicating lower total healthcare costs than the control group.
LR-OT Cost Analysis and Project Cost-Benefit.
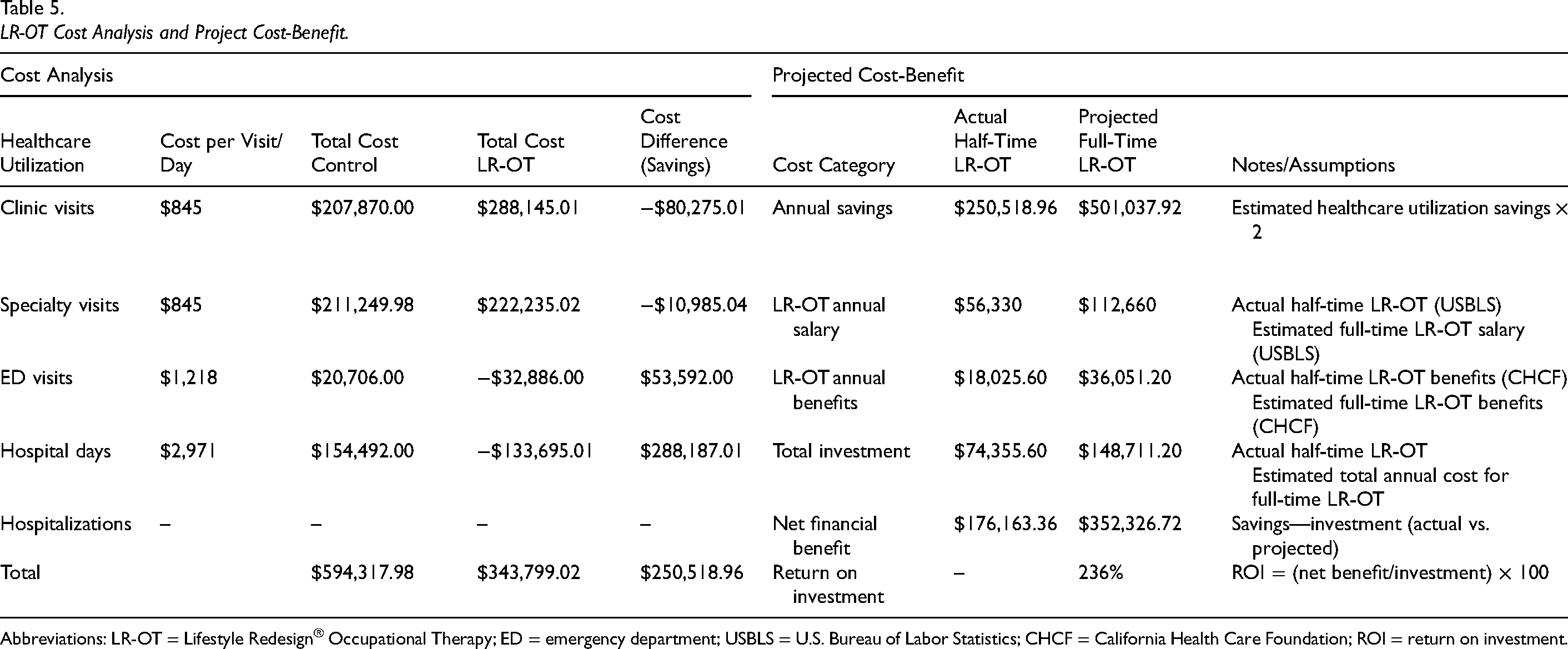
Abbreviations: LR-OT = Lifestyle Redesign® Occupational Therapy; ED = emergency department; USBLS = U.S. Bureau of Labor Statistics; CHCF = California Health Care Foundation; ROI = return on investment.
The estimated investment for implementing the LR-OT program included $56,330 USD for salary and $18,026 USD in benefits for the 0.5 FTE LR-OT, resulting in a total expenditure of $74,356 USD for the 12-month intervention. Considering these cost estimates for the LR-OT intervention and the savings realized by shifting healthcare utilization from acute (ED and hospital) to outpatient services observed within the LR-OT group, the cost-benefit to incorporate a full-time LR-OT into PC settings would be an estimated $352,327 USD, for a total ROI of 236%).
Discussion
The goal of this LR-OT intervention is to promote routine healthy habits to reflect sustained improvement in cardiometabolic indicators over 6 months. This study's primary outcomes demonstrate that, while we did not find significant clinical differences between the LR-OT and control (usual care) groups, during the intervention, trends of improvement were observed in HbA1c, BP, cholesterol, and BMI in the LR-OT group. In contrast, less favorable trends were observed in usual care. Healthcare utilization results demonstrated significantly fewer ED visits and shorter hospital lengths of stay among LR-OT participants. All observed savings were generated by a 0.5 FTE OT, resulting in a net financial benefit of $176,163.36 after accounting for salary and benefits. When projected to a full-time role, the net financial benefit of $352,326.70 suggests substantially greater system-level value, driven by reduced emergency and improved inpatient utilization.
In terms of clinical outcomes, a clear shift in HbA1c trajectory is observed: before intervention, both groups were worsening, with the LR-OT group having higher HbA1c than usual care. During the intervention, the LR-OT group decreased HbA1c by an average of .5% more than usual care, and after the intervention, both groups showed signs of stabilization. This HbA1c trend suggests that LR-OT reverses worsening glycemic trajectories and supports sustained improvement over time. Both groups, before and during treatment, remained in the clinical systolic BP “Hypertension, Stage 1” (130–134), however, there was a clear divergence between the groups, with usual care worsening during intervention, and the LR-OT group consistently improving even after the intervention and shifting to the clinically “Elevated” risk range (128–129). Diastolic BP was already in the normal range at baseline, which limits the magnitude of expected change. However, during the intervention, we observed a similar pattern to systolic BP: an early reduction in the LR-OT group, maintained posttreatment, and an early increase in usual care that converged with the LR-OT group after treatment, suggesting improved overall BP regulation rather than isolated changes associated with the LR-OT group. Cholesterol (a metabolic health indicator) shows the clearest intervention-associated trends. During the LR-OT exposure, cholesterol decreased by more than 20 points, entering a lower-risk range that was maintained posttreatment, whereas the control showed minimal change. BMI (a limited indicator of body composition) increased temporarily during treatment and declined below baseline levels at follow-up. The initial increase in BMI may be attributed to body recompositing, muscular hypertrophy, and changes in water balance (Ribeiro et al., 2023), and subsequently, to fat loss while maintaining healthy habits autonomously after the LR-OT program ended. The nonsignificant observed improvements in cholesterol levels in the LR-OT groups support this assumption of body recompositing. These results are supported by the previous LR-OT analysis, which analyzed only the LR-OT cohort and found significant pre–post improvements in HbA1c that significantly correlated with the number of completed LR-OT visits, BP, health perception, diabetes distress, diet, exercise, pain, mental, physical, social, and role function (Pyatak et al., 2019). The data reflect early stages of LR-OT integration as subsequent iterations have evolved to better address chronic conditions while maintaining fidelity to the foundational framework (Schepens-Niemiec, SL., 2025), and previous research indicates that TBC alone improves practice and patient outcomes (Henry et al., 2018). Therefore, larger studies are warranted to evaluate the conditions under which LR-OT most effectively produces sustainable improvements compared to usual care, particularly for patients with elevated glucose levels receiving care from safety-net institutions (Pyatak et al., 2013).
The primary outcome healthcare utilization results suggest that the LR-OT intervention helped guide patients to healthier lifestyles, reducing the need for emergency services. While both groups experienced a notable increase in outpatient utilization compared with the previous year, there were nonsignificant decreases in specialty outpatient visits compared with the control group. This shift has significant cost implications for the healthcare system, particularly for low-resource populations (Dean et al., 2020), who often receive late diagnoses and irregular care (Voura et al., 2024), resulting in preventable emergency healthcare service utilization (Dashputre et al., 2020). The increase in outpatient visits could represent a cost-saving pattern, whereby patients were followed more closely in a lower-cost setting and potential complications were addressed before they became emergent. The overall increase in yearly healthcare utilization across both groups aligns with the expectation that, in the United States, diabetes-related complications tend to rise with age due to cumulative disease burden and physiological maturity (Li & Chen, 2020), a phenomenon also observed in Canada (Government of Canada, 2024).
The observed increase in clinic outpatient utilization in the LR-OT may have promoted more effective TBC within the PC clinic setting, leading to improved continuity of care. Alternatively, increased clinic outpatient utilization could also reflect the patient-centered focus of LR-OT's guiding framework, which emphasizes collaboratively tailoring daily self-management strategies to individualized lifestyle challenges, often involving assertive communication and self-advocacy in healthcare settings (Pyatak et al., 2022). Therefore, increased outpatient visits may also be linked to LR-OT's emphasis on identifying unmet healthcare needs and ensuring appropriate follow-up through patient-centered, structured TBC collaboration. Previous studies have found that experienced TBC PC practices and continuity of care are associated with fewer hospitalizations and ED visits, although these reductions did not always translate into favorable patient outcomes (Bayliss et al., 2015; Nelson et al., 2014). Because TBC requires significant changes in PC culture, training, and organizational structures (Chesluk & Holmboe, 2010), the results of this pilot implementation study demonstrate the potential for future favorable utilization outcomes as team culture adapts and integrates an LR-OT into the PC clinic.
The secondary cost analysis supports the financial feasibility of LR-OT, demonstrating a total cost savings of $250,518.96 USD due to improved healthcare utilization among the treated population, who often utilize a high number of emergency and specialty services. The projected cost-benefit of the PC clinic formally hiring a full-time LR-OT is consistent with studies highlighting the cost-effectiveness of TBC (Henry et al., 2018) and patient-centered care (Matzke et al., 2018), which is attributed to preventing the utilization of emergency services. In fact, OT interventions within TBC and patient-centered care practices are particularly efficient in improving patient outcomes and demonstrating economic efficiency (Freeman et al., 2025). Given that the PC clinic was already experienced in TBC and transitioning toward patient-centered practices, healthcare utilization for both groups was influenced by those shifts in clinic culture.
These results suggest that a full-time LR-OT position has a cost-benefit and could further reduce healthcare utilization costs, particularly for patients with diabetes. OTs’ cost-effectiveness varies widely across practice settings, underscoring the need to consider local and national healthcare contexts specific to the nature of interventions when evaluating economic impact (Freeman et al., 2025). Although this study was performed in the United States, this LR-OT intervention aligns well with the Canadian public healthcare insurance system because it did not follow the fee-for-service model.
The integration of OT practitioners into multidisciplinary PC teams varies significantly between the United States and Canada due to the contrasting healthcare models. Canada's single-payer healthcare system covers OT for diabetes care through provincial health plans, in theory ensuring that all residents can access services without the direct financial burden of out-of-pocket expenses, incentivizing preventative and health-promoting services (Health Canada, 2024). As a result, 92% of OT practitioners are integrated into multidisciplinary healthcare teams. The demand for OT continues to increase, 1.5% above the national average (Government of Canada, 2025), and in 2021, 9.4% of the population had diabetes (Government of Canada, 2024).
In contrast, in the United States, diabetes care follows a fee-for-service model that incentivizes volume and profit-driven healthcare practices and discourages prevention and care coordination among providers (Streamline Health, 2023). Consequently, as of 2021, 11.6% of the population has diabetes (Centers for Disease Control, 2024). Still, the OT workforce is expected to grow by 11% within the next decade, and services are anticipated to be provided in a broad range of settings outside of healthcare (U.S. News, n.d.). Despite these challenges, OTs in both countries are positioned to alleviate the strain on PC teams by supporting patients with chronic conditions, such as diabetes, through lifestyle modifications and preventive care (Dahl-Popolizio et al., 2023).
Whether operating under a fee-for-service or single-payer system, this study demonstrates that OT practitioners can play a key role in reducing emergency care services and lowering long-term healthcare costs. Simultaneously alleviating strain on PC providers as Americans become increasingly concerned about healthcare costs and access, particularly with obesity-related conditions (Brenan, 2024). This study supports the case for integrating OT practitioners into PC teams, using a patient-centered framework with TBC practices, to improve healthcare utilization outcomes and reduce the long-term costs associated with diabetes complications.
Strengths and Limitations
A strength of this study is the experimental design, which helps mitigate other confounding variables by ensuring that participants in both groups were equally exposed to broader clinic-wide changes, thereby strengthening the likelihood that the unique approach of LR-OT drove the observed differences in healthcare utilization. However, a potential limitation is that randomization occurred after referral, which may have introduced selection bias and resulted in an inaccurate comparison of groups, since all participants were pre-determined (in their provider's judgment) to be willing to make lifestyle changes. Therefore, the differences between groups may be skewed by that pre-existing factor rather than the intervention itself, making it more challenging to detect significant differences.
The small sample size of this study may have resulted in reduced statistical power, making it more difficult to detect significant differences and increasing the likelihood that the findings were due to chance rather than a true effect. Furthermore, because clinical outcomes were collected within the routine flow of clinical care, data were passively collected, which affected analysis. Due to the small sample size and sporadic data collection, recruitment and randomization analyses, such as examining demographic differences between participants and nonparticipants, and Intention-to-Treat analyses, were not feasible. These would have improved the integrity of the analysis by reducing selection and randomization bias, which impacts the generalizability of the findings. Additionally, because this study was conducted within a single clinic, we cannot determine to what extent the observed outcomes are attributable to system-wide changes in healthcare delivery throughout the study.
Although this analysis included OT salary and benefits based on clinic estimates, it did not account for revenue from billable LR-OT services, which likely increases the cost savings. This omission was intentional, as it strengthens our goal of demonstrating that even without billing, LR-OT shows potential for a positive ROI. In a purely clinical setting, the balance of costs and revenues would differ. A limitation of our cost analysis is that it did not account for overhead expenses (e.g., treatment space, administrative workload for scheduling and billing) as there is no standardized approach in the literature for estimating these costs. This is particularly important since reimbursement remains a significant barrier to OT integration in the U.S. PC. The projected cost-benefit analysis assumes that the cost-benefit ratio will proportionally double with a doubling of work hours; however, the actual cost-benefit will vary depending on the dynamics of patients’ needs, resource allocation, and other factors that could influence outcomes. Future studies should include comprehensive cost-benefit analyses with more accurate projections in various settings over extended periods, modeled under both fee-for-service and alternative payment structures.
Conclusion
The primary aim of this practice-based clinical trial was to examine clinical outcomes and healthcare utilization. Although there were no statistically significant clinical improvements between groups, the LR-OT group did demonstrate a significant reduction in ED visits and hospitalizations. The secondary aim of this study was to conduct a cost analysis to determine the financial impact of LR-OT services and project future costs if a U.S. safety-net PC clinic within a large urban public health system integrates a full-time LR-OT into its practice.
This implementation study provides healthcare policymakers, funding bodies, and health insurance programs with real-world data about healthcare utilization trends that help decrease expenditures in this PC setting. LR-OT contributed $250,518.96 USD ($3,431.77 USD per person) to the PC practice's savings, and the projected annual financial benefit is $352,326.72 USD, supporting scalability. These cost savings are intentionally conservative, demonstrating a 236% ROI, without accounting for the revenue that could be generated if healthcare institutions chose to bill for LR-OT services. This demonstrates that even providing free LR-OT prevention services to patients could financially benefit healthcare institutions by reducing dependence on costly ED visits and hospitalizations and improving patient outcomes. In light of U.S. Medicare cuts that will reduce OT reimbursement rates (Parsons, 2024), considering resource reallocation to accessible preventive healthcare models that incentivize healthcare coordination by incorporating LR-OT into TBC PC teams is needed. Future research on practice-based OT interventions within PC warrants a deeper investigation exploring additional factors influencing financial outcomes, such as demographics, comorbidities, and variations in implementation across healthcare systems.
Key Messages
Equivocal Evidence on Clinical Outcomes with Long-term Trends: Integrating LR-OT into PC shows potential to favor patients' health overtime, even if short-term benefits were not statistically significant. Safer and Less Costly Healthcare Utilization: LR-OT integration in PC clinics can lead to reduced crisis-driven utilization and long-term healthcare costs, making it a valuable addition to patient-centered care teams utilizing TBC strategies. Financial Feasibility: The study demonstrates that integrating LR-OT into primary care without fee-for-service has a positive return on investment for healthcare systems, with potential cost savings and fiscal benefits.
Footnotes
Acknowledgments
The strong support from the clinic leadership and providers was invaluable to the program's success. We gratefully acknowledge Grace Cho, Elissa Lee, Daniel Padilla Vega, Megan Linderman, Gabriella Granados, the research participants, and the providers and staff at the Los Angeles County Department of Health Services for their support of this project.
Funding
This research was supported by the Southern California Clinical and Translational Science Institute through the National Center for Advancing Translational Sciences at the National Institutes of Health (Grant No. UL1TR001855).
Declaration of Conflicting Interests
In the United States, OT services face systemic barriers to insurance coverage, often necessitating research and advocacy to demonstrate value in care delivery. The affiliations disclosed below reflect the academic–practice partnerships common in OT to advance evidence-based integration into healthcare systems. The roles are disclosed to ensure transparency regarding potential influences on the research perspective. Valerie Tapia facilitates the OT Primary Care Learning Collaborative, a grass-roots professional network that advocates for integrating OT services into PC. This role includes promoting systemic changes that align with the research outcomes discussed in this article. Elizabeth Pyatak is the director, and Dr Stacey Schepens Niemiec is the associate director of Lifestyle Redesign® Strategic Partnerships, within the USC Lifestyle Redesign® Knowledge Mobilization Initiative, which aims to promote greater synergies across research, education, and practice to develop resources and infrastructure to enable OTs and health system partners to integrate LR-OT into diverse practice settings. Dr Stacey Schepens Niemiec is the editor of this special issue. While she recused herself from editorial decisions on this article, the close professional relationship warrants disclosure.
Data Availability Statement
Data, statistical code, and related materials are available from the corresponding author upon reasonable request.
