Abstract
Introduction
Promoting health and well-being among aging populations is crucial. By 2073, one-third (32.3%) of Canadians will be over 65 (Statistics Canada, 2024), with most (71.6%) living with a chronic condition (Public Health Agency of Canada (PHAC), 2020), a major cause of disability and reduced quality of life (World Health Organization (WHO), 2002, 2005). Health promotion can delay or prevent such conditions (PHAC, 2022), while empowering individuals to increase control over and improve their health (WHO, 2002), notably by strengthening their skills and capacities, such as the adoption of a healthy lifestyle. Human occupations, core to occupational therapy practice, serve as effective means of promoting healthy and meaningful lifestyles. In Quebec (Canada), preventive and health promoting approaches remain minimally integrated into occupational therapy practice despite evidence of their contributions (Ordre des ergothérapeutes du Québec, 2017).
Developed and tested in California, Lifestyle Redesign® (LR) is an effective preventive occupational therapy intervention aimed at developing sustainable, healthy and meaningful lifestyles among vulnerable older adults at high risk of chronic disease, disability and reduced life expectancy (Clark et al., 2015). Targeting the central theme of health through occupation, LR usually combines group (8–10 persons; 2 h/week) and individual sessions (1 h/month; Clark et al., 2015) over six to nine months. The groups, led by a trained occupational therapist (OT), address topics of importance to older adults (e.g., occupation and aging, community mobility, stress management). Based on the assumption that it would positively influence the health, functioning and well-being of older adults (Clark et al., 2015), this approach has been principally tested through two large-scale randomized controlled trials (RCTs) with respectively 361 and 460 community-dwelling older Americans (Clark et al., 1997, 2012). In the first RCT and compared to a social activity group (active control group) or no intervention (passive control group), LR was shown to be cost-effective (<US$$50,000/QALY; Hay et al., 2002) and demonstrated positive effects on daily functioning and quality of life of vulnerable older adults (Clark et al., 1997). Replicating the previous results in a larger and more ethnically diverse population, the second RCT also confirmed the approach's cost-effectiveness (US$$41,218/QALY; Clark et al., 2012) and explored the underlying mechanisms that could potentially explain the approach's positive effects. Its result showed that LR led to increased frequency of activities and a more positive perception of significance of activities, which both predicted decreases in depressive symptoms (Juang et al., 2018). These activity-related factors were, in turn, respectively and partially mediated by increased social connections and perceived control over desired outcomes (Juang et al., 2018).
Despite its robust evidence, the identification of facilitators and barriers to implementation of LR, particularly in new sociocultural contexts, remains limited; an aspect highlighted in recent studies (Hirvonen & Johansson, 2022), and not explicitly addressed in the blueprint guiding the LR research program (Clark et al., 2024). Feasibility studies examining the original intervention and its derivatives have primarily focused on normative variables (e.g., participation and retention rates; Cassidy et al., 2017; Mountain & Craig, 2011; Mountain et al., 2008, 2020) or on models such as ADEPT (Acceptability, Demand, Implementation, Practicality, Adaptation, Integration, Expansion, Efficacy; Bowen et al., 2009) that do not specifically address facilitators and obstacles to implementation (Levasseur et al., 2022; Maeir et al., 2020). To our knowledge, only Pyatak et al. (2019) have explicitly reported on challenges in implementing a LR intervention for diabetes management, including the need for patients and staff education, securing adequate workspace, and establishing a referral process. According to these authors, key elements that supported successful implementation included strong buy-in from clinic leadership, colocation and shared electronic medical record documentation. In Quebec, the French-Canadian version of the approach, translated as “Remodeler sa vie®” (RV; Clark et al., 2021), has demonstrated both feasibility (Levasseur et al., 2022) and positive effects on older adults’ mental health and interest in leisure, as well as improved social participation and attitude toward leisure for those with disabilities (Levasseur et al., 2019). Despite this evidence, the use of RV by Quebec OTs is still very limited and mainly restricted to a research context, partly due to insufficient understanding of implementation factors in this new sociocultural context; key elements in optimizing its benefits, sustainability and transferability. Conducted during the pre-implementation phase, that is, focusing on collecting feedback from key actors, piloting training and materials, and planning for delivery (Kilbourne et al., 2007), this study thus aimed to explore facilitators and barriers to a future implementation of RV in occupational therapy practice, as perceived by OTs, occupational therapy students (students), decision makers and community partners.
Method
Study Design and Participants
This pre-implementation study used a qualitative action-research method with 58 participants including 20 OTs and 4 students with an entrepreneurial profile (OT group), as well as 34 expert-partners, composed of 17 decision makers from organizational, professional and gouvernmental bodies and 17 community partners responsible for advisory tables, associations and community organizations for older adults. This sample size enabled in-depth exploration and data saturation, while ensuring diverse perspectives across practices (physical and mental health), clinical settings (public and private), region (urban and rural) and experiences level (novice and experienced). To be included, potential participants had to be (1) an cuupational therapy clinician or student, a decision maker or community partner working with community-dwelling older adults and interested in prevention and health promotion, (2) able to communicate in French (oral and written) and (3) available to participate in face-to-face training and data collection. Invitations were initially sent to experts working in private or community settings in two regions of Quebec, either known from the research team or identified through publicly available governmental and associative databases [Ordre des ergothérapeutes du Québec (OEQ) directory of private practitioners; Association québécoise des ergothérapeutes en pratiques privées; and ‘211’ information and service for Quebec regions]. In parallel, OTs working in public health and Social Service Centres (HSSC) as well as managers from four programs targeting older adults (home care, mental health, public health and multidisciplinary services) were invited to participate through an institutional suitability procedure. To reach OTs working with community-dwelling older adults and students more broadly, the OEQ's mailling list and two Facebook groups of “Ergothérapie Québec” and “Ergo Maîtrise 2017-2018” were also used. The Research Ethics Committee of the Eastern Townships HSSC approved the study (2018–2482).
Data Collection and Procedures
After an initial group meeting with the first author to receive study information, provide consent and complete a demographic questionnaire, the OT group participated in a one-and-a-half-day training on the French LR. This activity was offered in person on two consecutive days, including a 1.5 h asynchronous online presentation between sessions. It was led by the first and senior authors who primarily translated the University of Southern California 6-h online introductory course. By increasing their mastery of the clinical, scientific and historical content of the LR (Lévesque & Levasseur, 2025), this training aimed at effectively preparing OTs and students for the focus groups and, eventually, implementation of the approach. Although not invited to the training on the approach, the expert-partners attended a presentation on RV at the beginning of the focus group to enrich discussions.
To explore facilitators and barriers influencing the implementation of RV, 11 focus groups were conducted from April to November 2018, namely a first series with OTs and students only (7 groups) and a second series including OTs and students as well as expert-partners (4 groups; Table 1). All groups followed three semi-structured guides based on the Consolidated Framework for Implementation Research (CFIR; Damschroder et al., 2009). These guides were complemented with facilitation tools, such as the Context Analysis Matrix (Figure 1) to guide systemic advocacy actions, verified by 4 coauthors (ÉL, JF, ML, YC), pilot tested with an OT external to the study and refined throughout the process. Group sessions were 3 to 3.5 h long and facilitated by the first author, trained in conducting group interviews, and assisted by the senior author who attended all meetings as an observer summarizing key elements at the end of the discussions. These summaries were approved by the participants. All groups were recorded and transcribed (verbatim) for further analysis.
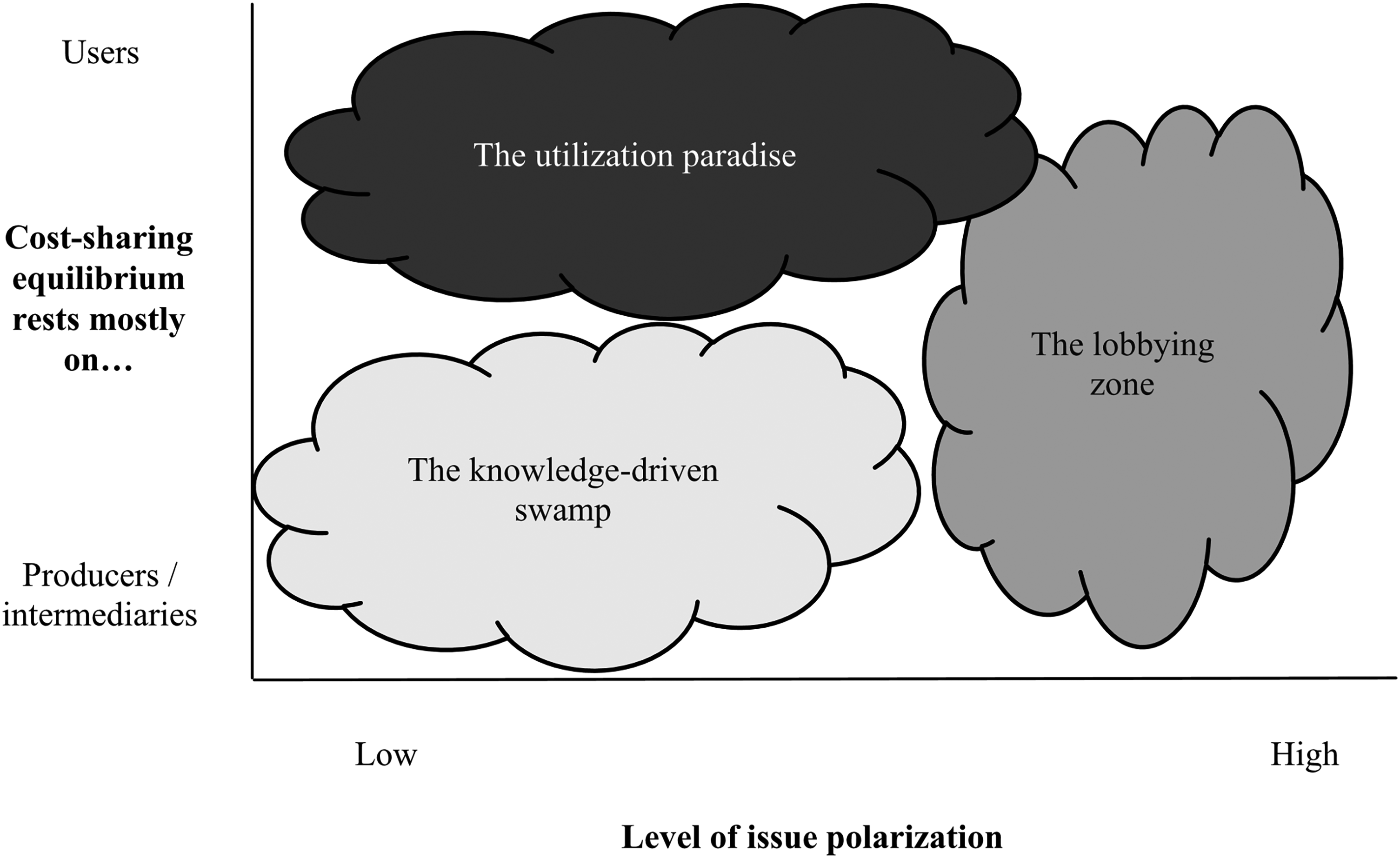
Context Analysis Matrix.
Group Structure.
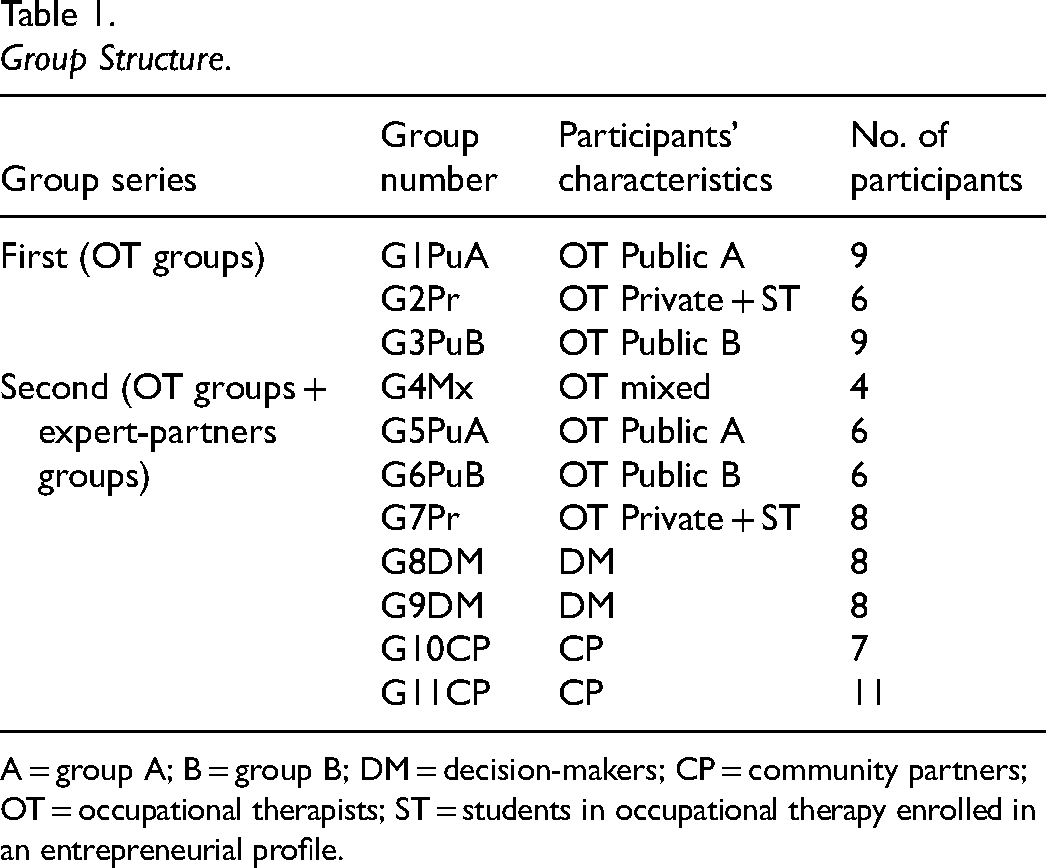
A = group A; B = group B; DM = decision-makers; CP = community partners; OT = occupational therapists; ST = students in occupational therapy enrolled in an entrepreneurial profile.
Participants’ sociodemographic data was analyzed descriptively; focus groups transcripts underwent a two-cycle coding process using a mixed extraction grid (Miles et al., 2020) where verbatim were first revised, segmented into units of meaning and organized according to the CFIR domains and constructs that best reflected its primary meaning (deductive analysis). An inductive analysis using strategies such as in vivo and overlap coding (Saldaña, 2025) was also performed to refine the initial coding structure and capture the complexity (e.g., contextual elements) and factors (e.g., facilitators or barriers) influencing the implementation. To increase credibility, reliability and confirmability (Miles et al., 2020), data was coded based on manifest content with one-third of materiel being co-coded by three research team members (ML, ND-C and YC) using coding rules and a codebook developed through an iterative and consensual approach. In the second cycle, codes were condensed into categories which were reviewed and compared together to identify salient themes in each CFIR domain. Consideration of memos and pertinent theories such as the theory of planned behaviour (TCP; Ajzen, 1991) also generated additional categories and themes that enriched the interpretation of data. Analyses were conducted using IBM SPSS Statistics (Version 25; IBM Corp., Armonk, NY) for quantitative demographic data or NVivo (Version 12; QSR International, Melbourne, Victoria, Australia) for qualitative data.
Results
Demographics
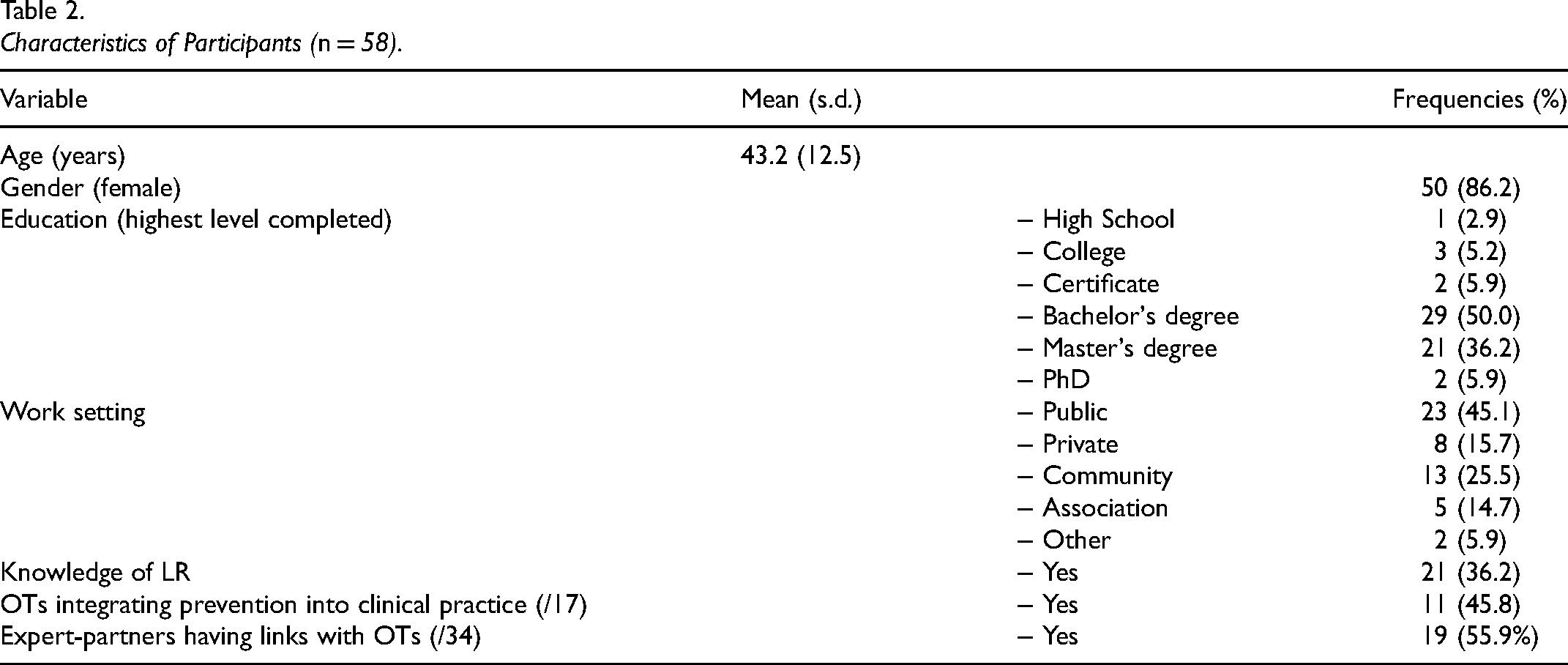
Among the 58 participants, ages ranged from 20 to 72, with the majority being women and holding a university degree (Table 1). The OT group (n = 24) included mostly clinicians (19; 79.2%), the majority working in the public sector (13; 54.2%). Two clinicians were not practicing at the time of the study. Most practicing clinicians worked with older adults (12; 70.6%) and nearly half of them (Table 2) integrated prevention and health promotion activities into their practice, typically through disciplinary or multidisciplinary intervention groups focusing on global health (e.g., physical, psychosocial, cognitive). Most OTs and students (70.8%) had previously heard about LR through scientific conferences or academic training. In the expert-partners group (n = 34), half (50.0%) worked in community and associative settings, while others were from the public (32.4%) or private sector (17.8%). Just over 10% (11.8%) of them were familiar with the approach. Most expert-partners had professional links with OTs, primarily for interdisciplinary collaboration, but also as colleagues and managers (Table 2).
Characteristics of Participants (n = 58).

Facilitators and Barriers
Globally, OTs from the public sector reported more barriers (17) than those working in private settings (12) and expert-partners (7), primarily due to organizational structures, misalignment between the approach's ethos and organizational mandates, and the top-down implementation model requiring authority approval and recognition of preventive action within productivity metrics (Table 3). Key facilitators and obstacles to implementing RV were concentrated within four CFIR domains. First, the innovation domain highlighted RV evidence-based design alongside challenges related to its complexity and cost. Second, in organizational setting, structural factors, resources and readiness for implementation were crucial, but varied across contexts. Third, the individuals involved played a key role, with facilitators such as OTs’ readiness for change, but also barriers like limited advocacy skills and uncertain engagement from older adults. Finally, socio-political context underscored opportunities from new societal trends but also barriers from fragmented policies and constant healthcare and political changes. Although not presenting major facilitators or barriers, process reflected a timely implementation shaped by top-down or bottom-up approach (Table 3).
Summary of Factors Influencing the Implementation of Remodeler sa vie® According to the CFIR.
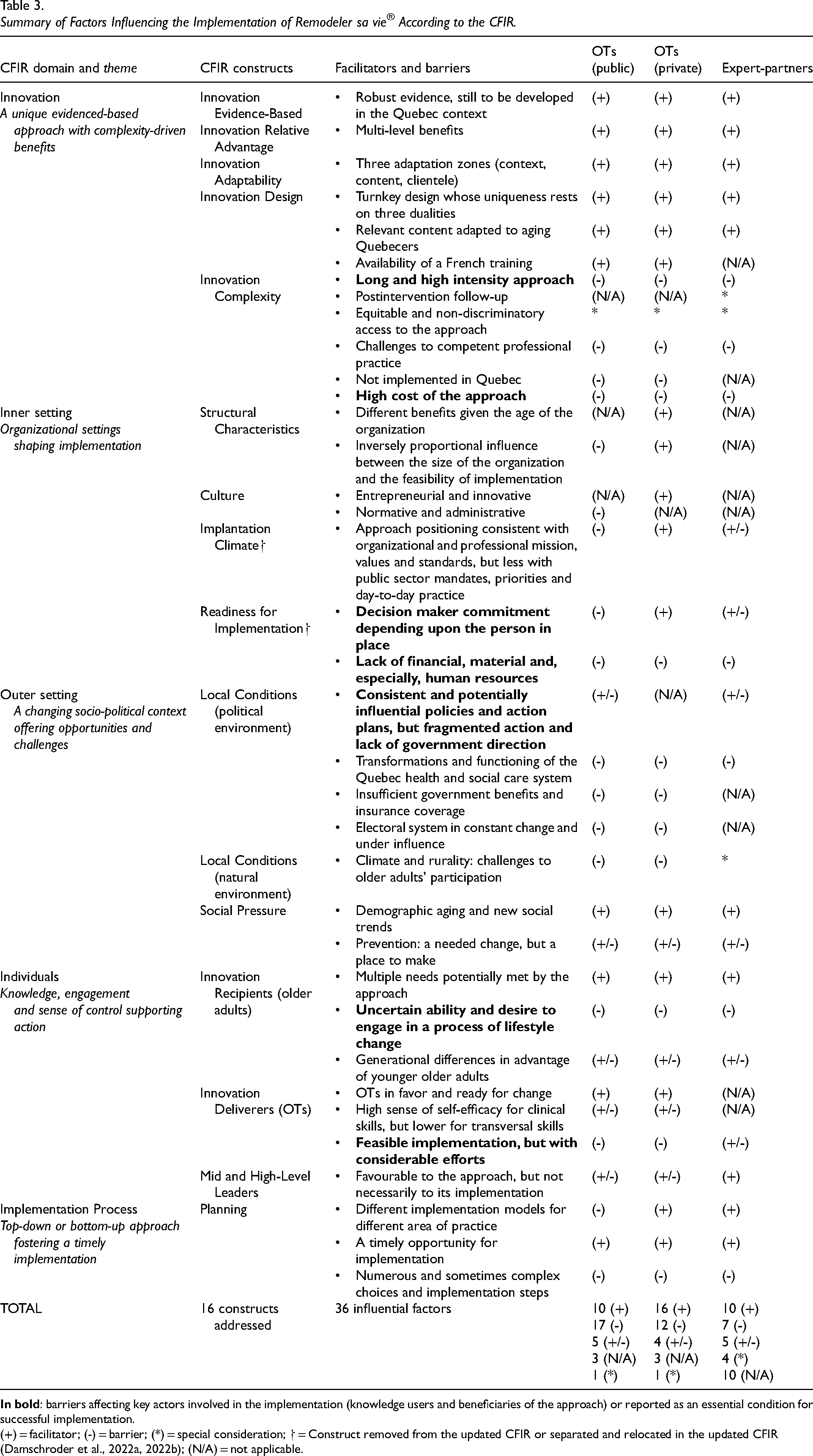
(+) = facilitator; (-) = barrier; (*) = special consideration; ⸷ = Construct removed from the updated CFIR or separated and relocated in the updated CFIR (Damschroder et al., 2022a, 2022b); (N/A) = not applicable.
Innovation: A Unique Evidenced-Based Approach With Complexity-Driven Benefits
According to the participants, the uniqueness of the approach lies in its combination of “novelty and tradition,” “flexibility and structure” and “group and individual” (Table 3). In addition to making it a “turnkey” approach allowing the use of scientific evidence, these characteristics were considered the best conditions for successful preventive intervention: “[The approach] definitely has the winning conditions: a long intervention, a group approach combined [with] an individual approach” (G8DM). Participants also unanimously saw the approach's evidence as key to supporting implementation and convincing key actors (Table 3). For example, quantifying the potential cost savings and health benefits of the approach on older adults was seen as a key element in gaining the support of decision makers. The evidence has also reinforced some OTs’ sense of self-efficacy in presenting the approach, explaining its relevance and illustrating OTs’ disciplinary contribution. OTs felt better equipped to advocate for change in their respective organizations. Similar to the strength of the approach's scientific evidence, its occupational focus positively influenced its potential for implementation by giving it credibility and value: “What is different and interesting is that an OT [delivers the approach], an expert who has relevant knowledge, is trained to listen and can engage [older adults]. Having an OT is less intrusive for older adults and their role in addressing the physical environment opens the door to the social environment. That's a plus!” (G11CP). Although endorsed by the participants as an occupational therapy approach, shared multidisciplinary facilitation was appealing to decision makers and community partners. In addition to preserving the occupational perspective and integrating the expertise of other health professionals, this strategy could distribute workload more equitably (higher cost-sharing; Figure 1) and facilitate adoption and funding by provincial and national governments. “If you want to get a national budget, it can’t be an occupational-therapy-only project. I agree that the OT should be central, but in an interdisciplinary approach” (G8DM). Finally, even if its length involved a substantial investment of financial resources and required a significant commitment from older adults and OTs (high human cost; Figure 1), the approach was unanimously considered necessary (low polarization; Figure 1) to support lifestyle change and create a sense of belonging and meaningful relationships. To manage the challenge associated with duration, a six-month approach spread over two sessions was proposed. In addition to being consistent with the usual programming of social and leisure activities offered in community settings, this adaptation has four types of advantages: (1) reducing the constraint of a long-term commitment for older adults, (2) facilitating the organization, management and financing of the approach, (3) providing an overview of the approach likely to motivate future enrolment and (4) creating an opportunity to tailor the approach according to different levels. A shortened approach format, including a periodic start-up of groups with new clients, could encourage adoption by health care decision-makers and allow clients from private sectors to benefit from tax advantages over two fiscal years. This strategy could potentially reach a greater number of older adults, contributing to the achievement of key results and performance indicators (e.g., penetration rate; Proctor et al., 2011).
Inner Setting: Organizational Settings Shaping Implementation
Including structural characteristics such as the organization's age and maturity, as well as its culture, and readiness for implementation (Table 3), the organizational setting was highly influential to the feasibility of implementing the approach. For example, participants anticipated an inversely proportional influence between the size of the organization and the feasibility of implementation. Smaller settings such as private occupational therapy clinics, mental health programs, day centres, religious communities, and private nursing homes appeared to be more likely to implement quickly, but on a smaller scale. Since its organizational culture was more entrepreneurial and innovative, the private sector seemed to be more likely to accelerate implementation and act as a lever for the public health system, which may prefer to await the outcomes of initial pilot initiatives before committing to a broader adoption: “In the short term, it will be more applicable to the private sector than to the public sector” (G2Pr). To ensure equitable access to the approach and avoid increasing social and health inequalities, implementation in the public sector was however considered an essential finality, although not a starting point: “I strongly believe in the universality of the public network and, compared to the private sector, it would be an advantage if they took on such a project” (G4Mx).
The positioning of this approach generally appeared consistent with the organizational and professional mission, values and standards, but less aligned with the mandates, priorities and day-to-day practice in the public sector. Although promoted as organizational values, prevention, autonomy, involvement and empowerment of individuals were sometimes absent from daily practice: “In the main orientations, health promotion is there, but in our [work setting], an immediate response with immediate results is expected and our priority is toward imminent risk for the client” (G3PuB; Table 3). For OTs working in the public sector, decision-maker commitment was reported to depend upon the person in place. While some managers encouraged innovation and pilot projects, others needed to be sure of the benefits before getting invested. Since managers must also respond to government performance indicators related to funding, their priority would often be imposed by higher authorities, though they retain flexibility for adaptation and personalization. Despite the interest of some managers in the approach, its implementation did not easily match the priorities prevailing at the time of the study. Finally, the shortage of financial, material, and especially human resources was a major barrier across all settings (Table 3). Except for private clinics, access to OTs was reported as an important barrier. In fact, the limited presence of OTs in public health departments, interdisciplinary family medicine clinics, nursing homes and community organizations was perceived as negatively impacting implementation of the approach: “It's a question of human resources…We don’t have any OTs to work with at the moment” (G10CP).
Outer Setting: A Changing Socio-Political Context Offering Opportunities and Challenges
Major historical transformations in the Quebec health and social care system still influence utilization of health care services, especially in older adults. For example, paying for services or consulting preventively would usually not be part of their habits. Many participants also deplored the negative effects of the 2015 health reform—which centralized healthcare governance and reduced local management autonomy— including a lack of long-term vision, unilateral decisions and a culture focused on disease management rather than prevention. According to participants, despite consistent and potentially influential policies and action plans, the absence of ministerial directives limits their impact on health care and social services. Indeed, currently based on the volume of services provided, the government's norms might hinder an eventual implementation. Unlike political context, demographic aging and new social trends, such as a marked interest in aging and self-management of health, created a favourable momentum for the implementation of the approach: “I really feel that prevention is part of the change needed in the healthcare system” (G6PuB).
Individuals: Knowledge, Engagement and Sense of Control Supporting Action
Although key actors may recognize the approach's value, they may still be reluctant to support its implementation (Table 3). Across all participant profiles, lack of knowledge about the approach and, more broadly, about occupational therapy was identified as the main determinant of key actors’ attitudes (e.g., openness, interest) towards the approach itself: “People don’t buy in if they don’t know what it [the approach] is” (G6PuB). In addition, perception of control over external resources (e.g., time, money) could modulate the engagement of managers and community partners towards implementation: “If it involves [getting] a budget, freeing up time or investing money for an OT, [decision makers] will say they don’t have what it takes” (G5PuA). Since access to occupational therapy resources was described as a central issue, OTs felt that some decision-makers may prefer other professionals or non-professionals (e.g., peer older adults) to deliver the approach. Concerning participation of older adults, their ability and desire to engage in a process of lifestyle change seemed uncertain because multiple factors, including lack of knowledge about the approach as well as attitudes of self-agism and passivity about taking charge of their own health: “[One older client] always thought she was too old for everything, like an age restriction on all activities” (G7Pr). Generational differences were also identified: some participants felt that a younger clientele (e.g., Baby boomers), increasingly health-aware, would be more incline to engage. For all these reasons, and because some older adults may feel less concerned and interested about the approach, participants stressed the necessity to assess their needs, concerns and readiness to act preventively, emphasizing that a key aspect of the approach is fostering personal responsibility for one's health. Participants were generally favourable and expressed readiness for change, often describing themselves in a “mobilization” stage, that is, preparing to try the approach: “That's what I’d like to do. I’m 200% motivated” (G1PuA). Perceived as achievable, this implementation however involved considerable efforts from OTs in terms of time and energy. Due to this large workload, OTs situated the approach in the “swamp” zone (Figure 1), characterized by a risk of the desired change becoming mired and requiring federation of partners for successful implementation.
Implementation Process: Top-Down or Bottom-up Approach Fostering a Timely Implementation
Participants perceived a timely opportunity for implementing the approach, which also aligned with the current and future directions of occupational therapy practice. Depending on the area of practice, different implementation models were preferred. Contrarily to the ones working in the private sector, OTs from the public sector were more likely to adopt a “top-down” approach, where decisions are pushed from the executive level to clinicians. Having the endorsement of authorities, including managers, Ministry of Health and Social Services and the professional regulatory body, was thus an essential condition for implementation in the public sector. Since they often had the latitude to determine their services, this concern was secondary for expert-partners and OTs working in the private sector: “I don’t think we should rely on public authorities, who are increasingly disengaged from prevention” (G9DM).
Discussion
This study explored, with OTs, students, decision makers and community partners, factors influencing the implementation of the French-Canadian LR in occupational therapy practice. The main facilitators were rooted in the innovation domain, namely the approach's flexible turnkey design and the quality of its evidence base, as well as in the individual domain, such as key actors’ openness and interest in the approach. The outer setting was characterized by new social trends, including a strong interest in aging and self-care that were also facilitators for future implementation. Although LR was seen as an effective response to complex and growing needs of older adults, barriers influencing its implementation were also identified. The complexity of the approach (cost, intensity, duration) poses challenges within the innovation domain and organizational readiness (e.g., access to resources) further hinders implementation within the inner setting. Barriers related to individuals included older adults’ uncertain desire and capacity to engage in the approach, while the outer setting was marked by a changing socio-political context. Providing equitable and non-discriminatory access to the approach was a shared concern. These issues are however not unique to RV and strategies are discussed below.
Firstly, considering the complexity of the approach, Glasgow and Emmons (2007) recommend fixing a minimum intensity threshold. In the case of programs targeting older adults’ social participation, a minimal duration of six months is recommended to allow the development of meaningful relationships and a sense of belonging (Raymond et al., 2015). Lifestyle change is also acknowledged as a gradual process that requires repeated behaviours in similar contexts (Nielsen et al., 2019). According to Lally and colleagues (2010), the formation of new habits for simple behaviours (e.g., drinking a bottle of water a day) in individuals willing to change could take up to 254 days with an average of 66 days. Accordingly, the adoption of complex behaviours (e.g., engagement in healthy occupations) may require continued and long-term support. While two studies (Cassidy et al., 2017; Schepens Niemiec et al., 2018, 2021) supported the feasibility of a shorter LR (3–4 months), Schepens Niemiec and colleagues (2018, 2021) indicate that participants would have preferred an intervention of longer duration. They reported that despite clinically significant and sustained treatment effects 12 months post-intervention, 16 weeks were deemed suboptimal to enhance sustainability, delve into the content, fully assess health and well-being impacts, and prevent intervener overload through a less intensive and more balanced pace over a longer period. As mentioned, the perspective of a shared, multidisciplinary facilitation appeared attractive as a resource optimization and cost reduction strategy. According to Pyatak and colleagues (2019), this perspective would nevertheless be modulated by a narrow conception of the role of OTs (e.g., home adaptation) and a lack of awareness of their potential contribution in primary care, as well as in prevention and health promotion. Although various models of facilitation with or by other professionals (e.g., ¡Vivir Mi Vida!; Schepens Niemiec et al., 2018) or peer-elders can be viable and beneficial (e.g., Living in Balance; Robitaille et al., 2012), prevention and health promotion approaches should be professionally led to ensure their effectiveness (Lood et al., 2015). Also, since LR is a therapeutic application rooted in occupational science (Clark et al., 2024), and previous studies demonstrate the specific contribution of OTs and the effectiveness of their interventions with older adults (Clark et al., 1997; Levasseur et al., 2022; Mountain, 2008; Pyatak et al., 2022), results converge towards a facilitation of the approach by an OT and combining the complementary expertise of guest speakers. Regarding the relational continuity of care (Archambault et al., 2019), facilitation by the same person should also be preferred. According to Levasseur and collaborators (2019), this continuity can notably promote the establishment of a trust-based relationship with the therapist and a feeling of cohesion among the group. A single facilitator approach, supported by trainees skilled in the approach, or people on reassignment (e.g., pregnancy-related preventive leave) could also reduce the clinical workload and complexity associated with alternating facilitation between different actors (e.g., group organization and follow-up).
Consistent with current knowledge anchored in occupational therapy and implementation science, particularly the study by Pellerin et al. (2019), which used the CFIR, the present results also reveal that organizational readiness is characterized by a limited engagement of decision-makers in implementation and a lack of human and financial resources, with private settings appearing more flexible and responsive than public ones. Considering the importance of their support and involvement which is widely confirmed in the scientific literature (Nielsen et al., 2019; Pellerin et al., 2019; Pyatak et al., 2019), the true question seems rather to determine the most effective ways to foster the involvement of decision-makers from all levels in the approach implementation. Based on the TCP (Ajzen, 1991) and the present findings, fostering decision makers’ involvement should focus on: (1) developing a supportive attitude, (2) experiencing social pressure, or (3) enhancing perceived control. To promote a supportive attitude, dissemination efforts should raise awareness of the approach and advocate for outcome indicators beyond productivity metrics, including health, quality of life, long-term effects and satisfaction among OTs and users. Reinforcing social pressure could involve highlighting the approach's adoption and endorsement by other individuals, organizations or authorities. Since resource access challenges vary across settings (e.g., limited presence or overworked OTs), tailored solutions are advisable to enhance perceived control. For instance, dedicating OTs to prevention or attaching them to public health departments could serve as a basis for discussion.
To address older adults’ uncertain desire to engage in the approach and to foster a posture of action rather than expectation, the relevance of the approach must be emphasized and explained. For example, older adults facing life transitions (e.g., retirement, illness, bereavement) and adapting to new circumstances may be key target for the approach, given their potential for long-term psychosocial health benefits (Chatters et al., 2017; Schepens Niemiec et al., 2021). Moreover, OTs should consider clients’ motivation, a factor reported by both participants of the present study and in the literature (Yang et al., 2019) as central to older adults’ engagement and successful implementation. Although willing and interested older adults could initially be targeted to take part in the approach, it is also critical to reach vulnerable clients for whom the approach was intended. To reach them, behavioural activation strategies (e.g., trial period; McNamara & Straathof, 2017) should be used to effectively engage more vulnerable clienteles who tend to avoid services and face higher morbidity and early mortality risks (Schepens Niemiec et al., 2018). For OTs, and to overcome the reported low cost-sharing of change in implementing RV (Figure 1), a collective action in which everyone contributes to the implementation effort is recommended. Mutual support between OTs in the various implementation settings, as well as the federation of partners would also be essential for successful implementation. Furthermore, OTs’ low sense of self-efficacy in systemic advocacy (Carrier et al., 2021) should not restrict them from advocating for change in practice and policies, including the implementation of new initiatives.
Strengths and Limitations
Conducted as a collaborative knowledge-building process with partners from different fields of expertise and sectors, this study offers a first in-depth examination of the factors likely to influence the implementation of RV, and even LR, an important step in guiding future adaptations and appropriate delivery with various populations. Beyond generating transferable, relevant and applicable knowledge in practice (Camden & Poncet, 2014), this pre-implementation study enhances the chances of implementation success through milestones such as ongoing assessment of influencing factors (Pyatak et al., 2019), better understanding of implementation contexts (Robins et al., 2013) and anticipation of barriers (Glasgow & Emmons, 2007). While this study relied on the original CFIR framework, the analysis was revised to align with the updated version (Damschroder et al., 2022b). Although recruitment was diversified, the study sample was relatively small and limited to only two regions of Quebec. Nonetheless, the results remain transferable to similar healthcare contexts, which represent important potential sites for the implementation of the approach. Finally, we must acknowledge that the selection of participants interested in the RV approach may have generated more favourable results. However, social desirability was minimized by reassuring participants about their anonymous contribution, and the absence of right or wrong answers.
Conclusion
This study explored factors influencing the implementation of the French-Canadian LR for older adults in Quebec, a critical aspect to maximize its benefits, sustainability and generalization to other practice settings. While this approach demonstrates strong evidence and relevance, its implementation requires strategic efforts to address resource deficits, align public mandates and better manage its complexity. Although the approach implementation appeared more feasible in private and community settings, structural and systemic barriers in the public sector must be addressed for an equitable access of the approach. Providing older adults with access to preventive services that could enhance their control over their health and well-being before major health issues arise and reduce long-term reliance on health and social services is an effective response to demographic aging and post-pandemic recovery. While not a standalone solution and requiring integration into broader policies addressing social and health inequalities, this approach has the potential to enhance services. Scientifically, the study findings provide guidance for subsequent phases of research, particularly by maximizing the chances of success for future implementation. As current evidence lacks clear guidance on successful implementation of the approach, including its scaling-up and sustainability, a detailed implementation plan leveraging identified facilitators and defining objectives, actions and responsibilities is a crucial next step.
Key Messages
Given challenges in implementing innovations and the limited documentation on facilitators and barriers to Lifestyle Redesign implementation, this study provides directly applicable knowledge for practice, supporting occupational therapists’ preventive role and promoting innovation.
Identifying facilitators and barriers to French-Canadian LR implementation supports efforts to adapt and expand this key occupation-based intervention, enhancing its sustainability and impact on the health and well-being of older adults.
Footnotes
Acknowledgements
We acknowledge the editing assistance provided by the Research Paper Language Editor GPT by Martins Zaumanis (version July 30, 2024), which helped enhance the clarity, readability and the conciseness of this manuscript, which was also reviewed by Victoria Stecum. We would also like to express our sincere thanks to Stéphanie Roy, Élise Huot Coulombe, Janie Gobeil, Manon Parisien and Nathalie Champoux who contributed to the translation and revision of the training as well as to the OTs, decision makers and community partners who participated in the focus group.
Funding
This study was supported by the Réseau québécois de recherche sur le vieillissement (RQRV). Marie-Hélène Lévesque is a doctoral student and fellow of the Canadian Institutes of Health Research (CIHR) and the Fonds de recherche de Québec–Santé (FRQS). At the time of this study, she was funded by the FRQS and CIRH through a master’s scholarship. Mélanie Levasseur was a new CIHR Scholar (#360880) and she currently holds a Tier 1 Canadian Research Chair in Social Participation and Connection for Older Adults (CRC-2022-00331; 2023-2030).
Author Contributions
All authors made substantial contributions to the study, including drafting the funding application (all), revising the protocol and interview guides (EL, YC, JF, NL, ML), refining the occupational therapist training (EL, MP, DG, VP, JF, NL) and co-coding data (NDC, YC, ML). Data collection, analysis, interpretation and initial drafting were led by MHL, supported by ML and subsequently revised and enriched by all authors. All authors approved the final version for publication.
