Abstract
Introduction
Participatory research is a broad concept encompassing a wide variety of approaches to empower community members to participate in research and thereby engage them in making decisions that influence their lives (Jason et al., 2004). According to Balcazar et al. (2006), a participatory approach includes recognition of persons with lived and living experiences as research collaborators and engages them as active participants in all research phases, including defining the problem to be addressed, data collection, interpretation, and dissemination of findings. One of the significant differences between participatory approaches and other research models is that community members are involved in shaping research questions, and the traditional roles reserved for researchers, consumers, and service providers are reconceptualized (Balcazar et al., 1998).
Participatory research is an umbrella term for a range of approaches that incorporate individuals with lived experiences, service providers, and stakeholders throughout the research process (Cargo & Mercer, 2008). Green et al. (1995, p. 5) defined participatory research as “systematic inquiry, with the collaboration of those affected by the issue being studied, for purposes of education and taking action or effecting change.” While participatory action research is the most familiar term to most researchers (MacDonald, 2012), additional parallel approaches include community-based participatory research (CBPR), action research, and experience-based co-design (EBCD), among others. The purpose of action research is to improve the capacity and practice of the researcher instead of producing theoretical knowledge and does not always engage research participants in the study (Elliot, 1991). In participatory research and CBPR, researchers and community co-researchers collaborate to change a social reality (Whyte, 1998). Participatory action research is the combination of action research and participatory research with the goal of improving the capacity and practice of researchers and changing social reality through participation (Elliot, 1991).
Letts (2003) indicates that two key concepts of occupational therapy have a strong link with participatory research principles: client-centred practice and occupation. Participatory research, like client-centred occupational therapy, emphasizes bringing participants to the process of research and using their expertise to develop knowledge. In both participatory research and client-centred occupational therapy, the knowledge that participants bring to the encounter is crucial (Letts, 2003). The core values of client-centredness, such as the right of a person to choose occupations, are congruent with the holistic view of occupational therapy and the theoretical framework of occupational performance (Law et al., 1995).
A second connection between participatory research and occupational therapy is the concept of occupation (Letts, 2003). Occupation has a significant role in promoting health (Egan, 2022). Participatory research can be thought of as an occupation in itself in that the concept of “action” is considered a key component of the research process (Letts, 2003). In occupational therapy and occupational science literature, participatory approaches have been conducted with persons with different health conditions, including persons living with physical disabilities (Bhagwanjee & Stewart, 1999), adults with mental health conditions (Andonian, 2010), older adults (Andonian & MacRae, 2011), occupational therapists (Egan et al., 2004), children with mental health disorder (Greco et al., 2017), immigrants and refugees (Suarez-Balcazar et al., 2018), and low-income communities and individuals with chronic health conditions (Wang, 1999).
The Relevance of Participatory Research for Persons Living with Mental Illness
The unique strengths and challenges faced by diverse persons who experience mental illness present an important opportunity for using participatory approaches that take an occupational perspective. Mental illness refers to a wide range of conditions that affect cognition, emotion, and behaviour that can create challenges for occupational participation (Manderscheid et al., 2010). The importance of involving diverse individuals with mental illness in the development of approaches that are co-designed has been broadly recognized as an ideal approach in refining and creating innovative health systems (Chodo, 2015). According to Bassman (2001), persons living with mental illness have historically lacked a voice, and they are infrequently involved in decision-making about the mental health services. The historical oppression faced by persons living with mental illness makes this population a key group with which to conduct participatory research, as listening to and acting upon their perspectives is an opportunity to reconcile past oppression (Kleintjes, 2012).
The Current Study
Participatory approaches have been used in a variety of ways within occupational therapy and occupational science; however, little is known about the scope of participatory research conducted with persons living with mental illness specifically. Understanding the breadth of literature in this area will provide a foundation on which to advance research and knowledge in action. Although there are number of reviews on participatory research and health in other disciplines (Stacciarini et al., 2011) or with other populations (Rustage et al., 2021), to our knowledge, there are no existing systematic or scoping reviews which have been conducted to synthesize literature on participatory research with persons living with mental illness in occupational therapy and occupation science. To fill this gap in the existing literature, we conducted a scoping review guided by the research question: What is the scope of participatory research within the field of occupational therapy and occupational science regarding persons who experience mental illness?
Method
We conducted a scoping review following the methodological framework outlined by Arksey and O’Malley (2005) using the PRISMA-ScR guidelines (Tricco et al., 2018). Arksey and O’Malley's framework encompasses five steps, which are described below.
Search Strategy
We initially deployed our search in November 2021 and updated our search in December 2022. Our search combined the concepts of participatory research (e.g., participatory action research, photovoice) and occupational therapy and occupational science (occupational therapy*, occupational science) using a Boolean “AND.” The search strategy was deployed in nine databases (Medline, Embase, CINAHL, Sociological Abstracts, Nursing and Allied Health, Social Service Abstracts, Social Work Abstracts, Cochrane and PychoINFO). A sample of our search, deployed in Medline, is provided in Appendix 1.
Inclusion and Exclusion Criteria
We included articles that: (a) used participatory research approaches; (b) pertained to persons who experience mental illness or mental health challenges; (c) were published in English or Persian; (d) published in all years; (e) pertaining to persons of all ages; (f) scoping and systematic reviews of empirical studies; and (g) had been published within the field of occupational therapy or occupational science (e.g., it was published in an occupational science or occupational therapy journal or was written by a first or last author identifying as an occupational therapist or occupational scientist).
We excluded articles under the following criteria: (a) action research studies that were not explicitly participatory; (b) conference abstracts; and (c) dissertations and theses.
Study Selection
We uploaded our searches from each database into Covidence™ ( Covidence systematic review software, 2022 ), a software program that allows for collaborative review and data extraction. Two independent raters (EJ and CS) subsequently screened titles and abstracts by comparing each against the inclusion and exclusion criteria identified above. The full texts of studies included at the title and abstract screening stage were uploaded, and two independent raters read each paper in full, comparing each against the set of inclusion and exclusion criteria to determine eligibility. Conflicts arising during either of these stages were resolved by consensus. When the conflict could not be resolved using two independent raters, we sought the input of a third rater (CM).
Data Extraction
Using a custom data extraction form developed in Covidence ( Covidence systematic review software, 2022 ), we extracted the following information from each included study: author(s); year of publication; study design; methodology; participant type (e.g., persons with mental illness, occupational therapists, parents, etc.); clinical characteristics of participants; number of participants; demographic characteristics of participants; country of authors; and level of participation. To determine the level of participation of persons with lived experiences of mental illness in each study, we used a framework introduced by Kindon et al. (2007). This framework identifies key actions taken by researchers to involve persons with lived experience in a participatory study, and thus, provides an opportunity to measure the level of participation used in participatory studies. Further, Kindon et al. (2007) introduced five recurrent stages of action and reflection, including establishing relationships and a common agenda with all stakeholders; collectively designing research processes and tools; collaboratively analyzing the findings; working on feeding research back to all participants; and collectively identifying future research and impacts. We used the information provided by the authors of the included studies in the methodology section of each paper to identify whether they reported the process of action and reflection.
Narrative Synthesis
Qualitative content analysis (Graneheim & Lundman, 2004) was employed to code statements in the included studies pertaining to the research question using Dedoose (Dedoose, 2021), a qualitative data management program. This analysis involved reading through the full texts of the included articles to identify statements that were related to the research question. We then coded each statement inductively, followed by creating categories and sub-categories to generate themes and sub-themes that were related to the research question.
Findings
The search yielded 1,311 citations. A total of 894 studies remained after removing 417 duplicates. 856 studies were eliminated during the title and abstract screening. We calculated Kappa statistics to assess the agreement among the raters for both the title and abstract screening and full-text review phases. Inter-rater reliability for the title abstract screening stage was 0.47, which demonstrates a “moderate” strength of agreement according to Ashby (1991). Thirty-eight articles were subjected to full-text review. For the full-text review phase, inter-rater reliability was 0.55, also demonstrating a “moderate” strength of agreement according to Ashby (1991). A total of 28 articles met the criteria for inclusion, and six studies were added from the reference lists of the included articles, which resulted in 34 studies in the final review. See Figure 1 for the summary of the study selection process and reasons for exclusion.
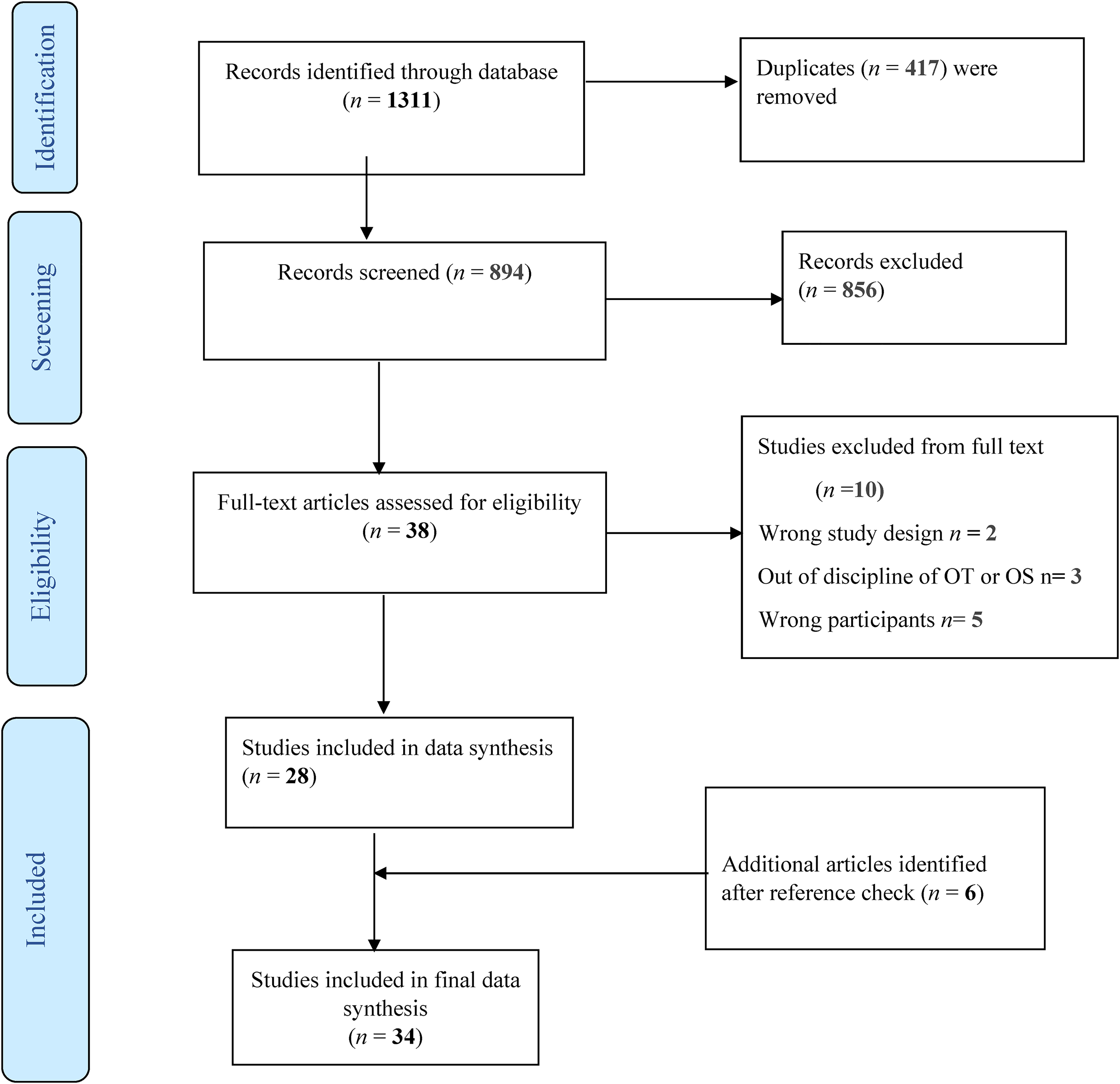
PRISMA diagram.
Of the 34 articles included in this review, 23 (76.4%) used qualitative methods, two (5.8%) studies used mixed methods, five (14.7%) were expert opinion papers, and one was a scoping review. Nearly half of the included studies (52.9%) were conducted in Canada and United Kingdom (nine studies each country), followed by the United States (n = 8; 23.5%), Australia (n = 5; 14.7%), Singapore (n = 1; 2.9%), and South Africa (n = 1; 2.9%), and internationally (North America, South America, Europe, and Africa) (n = 1; 2.9%). Studies included in this review spanned from 1993 to 2022. A total of 22 (73.5%) studies were conducted after 2010. Twenty-two articles (64.7%) were published in occupational therapy journals, 11 (32.3%) in interdisciplinary journals, and one (2.9%) in an occupational science journal. The characteristics of individual studies included in this review are provided in Table 1.
Description of the Included Studies (n = 34)
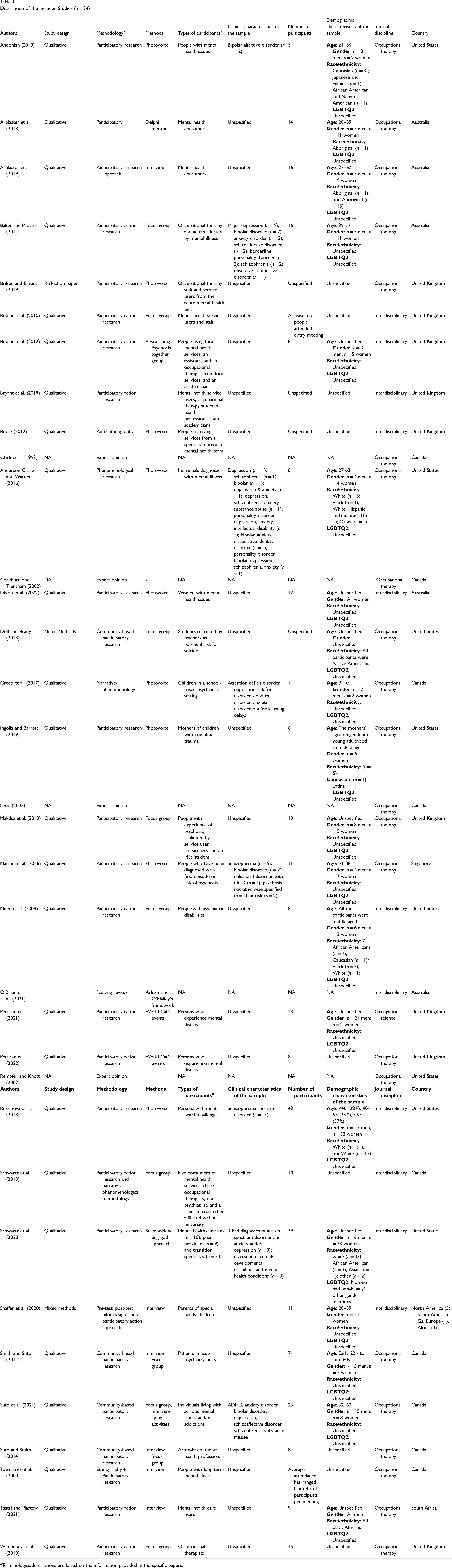
Terminologies/descriptions are based on the information provided in the specific papers.
The level of participation in the included empirical studies (n = 28) according to the framework provided by Kindon (33) is provided in Figure 2. In 14 of the included studies (41.1%), the authors and participants collaboratively decided on the focus of the study. Fourteen studies (41.1%) collectively designed research processes and tools. In 12 of the included studies (35.2%), participants and researchers collaboratively analyzed the findings. Only four of the included studies (11.7%) collectively identified future research and impacts.
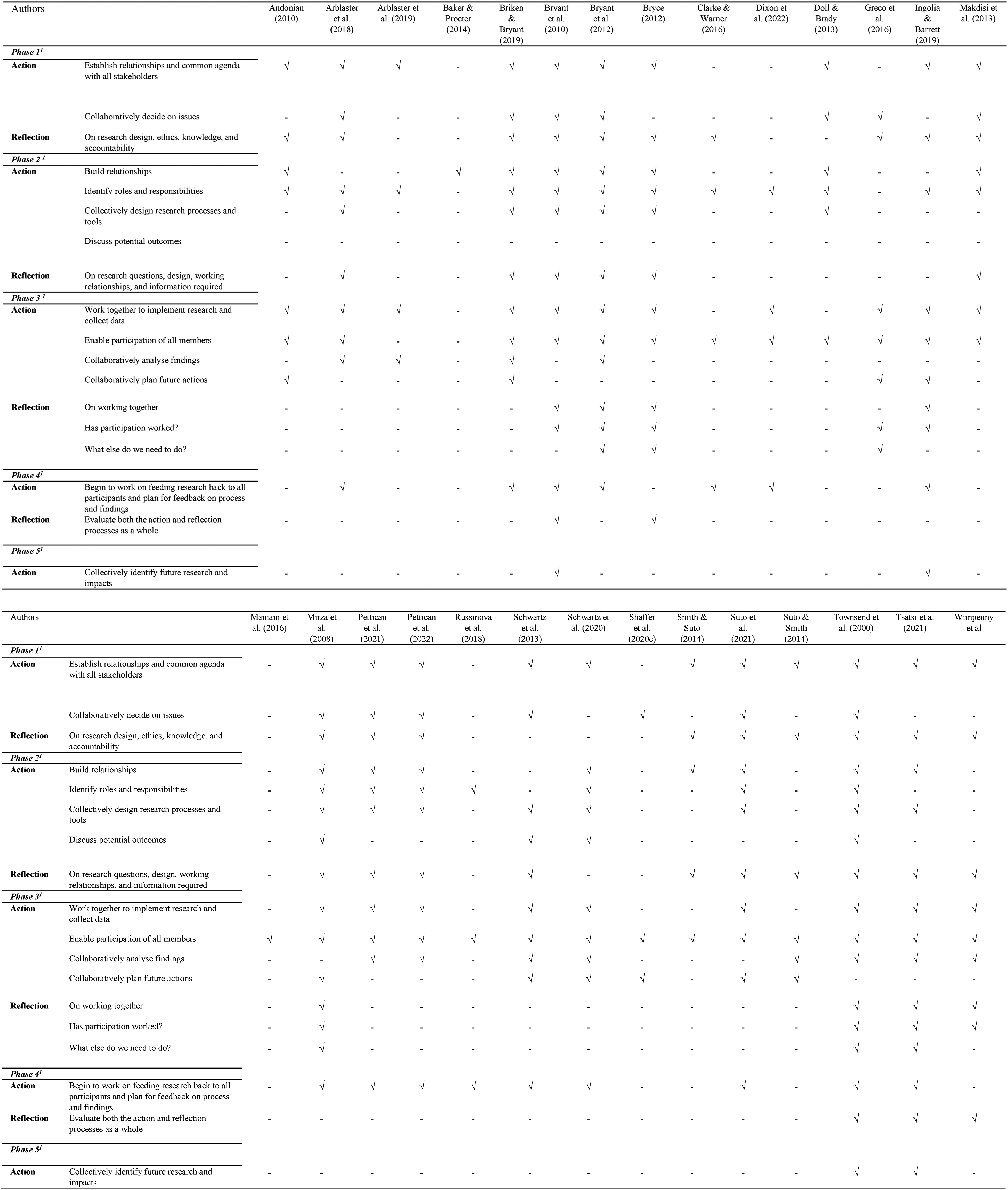
Level of participation of the included studies (N = 28).
Narrative Synthesis
We generated three themes in our content analysis: (a) coming together; (b) unique potentials of participatory research; and (c) challenges of conducting participatory research. Articles associated with these themes and associated sub-themes are presented in Table 2.
Themes and Sub-Themes Represented by the Included Studies

“Coming Together”
The concept of “coming together” was explored in 23 articles (67.64%) in this review (see Table 2). Broadly, coming together can be defined as a context that brings experts by experience (mental health service users), experts by profession (service providers), and researchers who work together and share power to improve the experience of mental health service users. These articles noted that “coming together” is possible through (a) achieving a shared understanding and (b) effective communication.
Achieving a Shared Understanding
The value of achieving a shared understanding between persons with mental illness and service providers and researchers was discussed in 19 of the included studies in this review (See Table 2). Bryant (Bryant et al., 2012) believed that in the context of participatory research, both occupational therapists and persons with mental illnesses have something to learn, and involving all stakeholders in research creates space for all to learn from each other and achieve a shared sense of purpose. In Maniam's study (2016), photovoice as a participatory method was identified as a unique tool for occupational therapists to hold dialogs with their clients. The findings of eight studies found that there is a mismatch between the priorities and goals of people accessing mental health services and the focus of occupational therapy mental health services themselves (Anderson Clarke & Warner, 2016; Arblaster et al., 2018; Birken & Bryant, 2019; Ingolia & Barrett, 2019; Mirza et al., 2008; Rempfer & Knott, 2002; Schwartz et al., 2013; Shaffer et al., 2020). Schwartz et al. (2013) pointed out that the conflict between values of beneficence in medical ethics increases the tension between the occupational therapist and consumer values. In Arblaster's study (2018), it was discussed that occupational therapists usually value clinical reasoning and evidence-based interventions, while mental health consumers want therapists to understand and value their perspective and support their choice. Arblaster et al. (2018) found that “consumer’s emphasis on human connection and ‘doing with’, and a therapist’s emphasis on ‘doing to’.” The participants in Arblaster's study (2018) believed that human connection is a core value that underpinned the recovery-oriented occupational therapy practice. Several studies (n = 11) clearly expressed the need for service providers such as occupational therapists to better understand the needs of persons with mental illness and validate their stories in practice and research (Arblaster et al., 2018; Baker & Procter, 2014; Bryant et al., 2012; Bryant et al., 2019; Bryce, 2012; Doll & Brady, 2013; Makdisi et al., 2013; O’Brien et al., 2021; Schwartz et al., 2013; Schwartz et al., 2020; Suto et al., 2021). Collaborative relationship (Arblaster et al., 2019; Bryant et al., 2012; Suto et al., 2021), learning from lived experiences (Arblaster et al., 2018; Baker & Procter, 2014; Makdisi et al., 2013), professional self-reflection, critically examining power inequity (Arblaster et al., 2019), being open to different knowledge (Bryant et al., 2019), and using co-design protocols (O’Brien et al., 2021) were mentioned as strategies to build up a shared understanding of issues related to mental illness in occupational therapy literature.
Effective Communication
Considerations for effective communication between mental health consumers and occupational therapists were discussed in ten participatory studies (see Table 2). Participants in four studies (Arblaster et al., 2019; Bryant et al., 2019; Smith & Suto, 2014; Suto & Smith, 2014) suggested that occupational therapists need to engage in self-reflection to find effective ways of building a therapeutic alliance with persons living with mental illness. The value of informal and non-clinical communication style in the context of participatory projects was identified as a priority in three studies (Bryant et al., 2012; Schwartz et al., 2020; Tsatsi & Plastow, 2021). Being a co-researcher in a non-clinical context was important for changing how everyone communicated (Bryant et al., 2012). Some participants felt that communication would be easier if professionals could “just take off their labels and see what's going on” (Schwartz et al., 2013, p. 115). In contrast, some service providers believed that setting clear boundaries and expectations can foster trust between mental health consumers and service providers (Schwartz et al., 2020). Building culturally sensitive relationships with co-researchers before starting the co-design research projects was also highlighted in O’Brien's study (2021).
“Unique Potentials of Participatory Research”
Twenty-three articles (67.6%) included in this review identified the unique potential of participatory research for individuals who experience mental illness (see Table 2). The findings of these articles were divided into the following sub-themes: (a) empowerment; (b) sharing power; (c) expressing what matters; and (d) stigma resistance.
Empowerment
The experience of collaborating in participatory research created a potential feeling of empowerment for occupational therapy service users in 13 studies (see Table 2). Having an opportunity to learn from each other, expand the sense of meaning, become more vocal, share expertise with a greater audience, improve self-efficacy, feel a sense of mastery and achievement, achieve acceptance and hope, and take action towards facilitating change in their environment were factors provided in the context of participatory research that helped participants feel empowered (Andonian, 2010; Bryant et al., 2012; Bryant et al., 2019; Maniam et al., 2016; Rempfer & Knott, 2002; Tsatsi & Plastow, 2021).
Sharing Power
Ten of the included studies demonstrated that power could be shared between individuals with mental illness, mental health professionals, and researchers through conducting participatory studies where the traditional roles of “patient” versus “professional” are broken down (see Table 2). In Greco's study (2017), children living with mental illness had the opportunity to take control using photovoice methods, which reduced the power imbalance between children, adults, and researchers. Townsend et al. (2000) suggested that occupational therapists and other professionals need to extend the notion of person-centredness in the context of research in order to reduce power inequity.
Stigma Resistance
Participatory research was identified as a potential tool to resist stigma for persons with mental illness in four studies (see Table 2). These studies highlighted the potential of participatory research to increase the knowledge of stigma, and advocate against it. In particular, Russinova et al. (2018) suggested that photovoice was a transformative tool to reduce the impact of prejudice and discrimination toward persons with mental illness and can translate the experience of stigma by presenting it both visually and conceptually. Russinova et al. (2018) believed that photovoice allows persons with mental illness to express their experiences of stigma in a way that feels psychologically safe.
Expressing What Matters
Fourteen of the included articles pointed out that participatory approaches enable individuals living with mental illness to express what really matters to them to create relevant and meaningful knowledge (see Table 2). Three of the included studies (Pettican et al., 2021; Pettican et al., 2022; Tsatsi & Plastow, 2021) suggested that involving persons with mental illness in conducting research can assist both mental health consumers and mental health professionals such as occupational therapists to identify important ideas and the desired direction for change. In two studies, authors (Dixon et al., 2022; Rempfer & Knott, 2002) noted that including the voice of mental health consumers helps occupational therapists access the knowledge not represented in the scientific literature. Arblaster et al. (2019) suggested using participatory methods within the field of occupational therapy to ensure that focus of occupation is balanced with the lived experience concerns of persons living with mental illness. Greco et al. (2017) believed that the participatory philosophy of the photovoice method can help children with mental health disorders who use occupational therapy services to generate new domains for self-report measures and report what matters to them.
“Challenges in Conducting Participatory Research”
The challenges of conducting participatory research were documented in 11 (32.3%) of the included studies (see Table 2). One of the concerns noted by two authors (Bryant et al., 2019; Letts, 2003) was the process for obtaining ethical approval for studies in which service user researchers were also the subjects. In Bryant's study (2019), a university was unfamiliar with the idea of service user co-investigators, and there were mutual misunderstandings throughout the process of seeking ethical approval. Townsend (2000) believed that expectations of research policies, ethical and funding guidelines, and research presentations and publications create barriers to the inclusion of persons living with mental illness and minimize experiential knowledge. The idea of involving service users in research was described was difficult to achieve because the majority of participatory research agendas are determined by academicians and/or service providers, not service users (Bryant et al., 2010). Finding common ground (Bryant et al., 2019), finding the focus of research (Townsend et al., 2000), and disagreement about ownership (Bryant et al., 2019) and leadership (Letts, 2003) of the project were described as challenges associated with conducting participatory research. Two of the included studies made the point that participatory research is time-consuming and needs more resources than the traditional research methods (Letts, 2003; Rempfer & Knott, 2002). In one study, maintaining the enthusiasm and involvement of people accessing mental health services in all project stages became a concern (Cockburn & Trentham, 2002).
In four studies, participants also experienced individual challenges with the participatory projects in which they were involved (Bryant et al., 2010; Bryant et al., 2012; Cockburn & Trentham, 2002; Maniam et al., 2016). Fear and anxiety during focus groups (Bryant et al., 2012), being unfamiliar with the occupation of research (Bryant et al., 2010), being an active decision-maker (Cockburn & Trentham, 2002), fear of being judged, technical difficulties such as working with a camera (in the instance of photovoice), and fear of not completing the project (Maniam et al., 2016) were reported. Participants in Tsatsi's study (2021), believed that their involvement in the scientific part of the research process was limited because they were only involved in the outcome formulation, initial data analysis, and taking action. Andonian (2010) discussed that selection bias in participatory approaches is assumed because the participants willing to be involved in research projects and have an active role might be different from those not comfortable speaking in group settings.
Discussion
This scoping review aimed to identify the range of research exploring participatory approaches with persons living with mental illness within the fields of occupational therapy and occupational science. Our findings suggest that involving persons with lived and living experiences of mental illness in all stages of the research process can provide several benefits, for all people involved in the research, including researchers, health professionals, and mental health consumers, while also introducing some challenges. The role of co-design and providing opportunities for persons with mental illness to take on leadership roles in health system planning, evaluation, and research is critical for contributing to efforts aimed at reconciling the historical oppression faced by this population. This includes creating the opportunity to identify important research questions, share knowledge, and participate in all stages of the research process, including analysis, interpretation of results, and mobilizing findings into practice and policy, as these are common practices in participatory approaches. However, our review also found barriers to conducting this type of research with this population, including time to do the research and work within institutional challenges that prevent such studies taking place in the first place. We encourage future occupational therapy and occupational science research to document these challenges and propose solutions for the field for how best to navigate institutional challenges, such as ethics/human resources and funding.
The findings of participatory research included in this review highlighted the risk of misalignment between mental health consumers’ priorities and service providers’ goals in practice and research. In one of the included studies in this review, Arblaster et al. (2018) found that human connection and “doing with” are emphasized by mental health consumers, while the focus of mental health professionals is “doing to.” This is consistent with the existing literature, which suggests that occupational engagement of individuals is motivated by the need to belong and connect with others (Andonian & MacRae, 2011; Berger, 2011). We believe that this misalignment should be addressed by working alongside persons who experience mental illness to generate a shared understanding of mental illness and effective approaches for service provision. In research, occupational therapists and occupational scientists can address a historical lack of collaboration with service users by bringing together researchers, service providers, and persons with lived experiences to generate relevant occupation-focused research questions. This suggestion builds on recommendations in previous studies, which suggest that mental health consumers and mental health professionals need to work together to achieve a shared understanding of diagnosis, prognosis, and recovery (McCabe et al., 2013; Papageorgiou et al., 2017).
The findings of this review reveal the unique potential of participatory research for persons living with mental illness. In this review, participants felt empowered by engaging in research projects and being active decision-makers. Clark et al. (1993) believed that involving persons in occupational therapy research is supported by values of occupational therapy practice, in which involvement in decision making is crucial. Given the complexities of environments in which participatory research is conducted, this review suggests that occupational therapy researchers should apply a pragmatic approach that aligns with the core assumptions, principles, and values of occupational therapy (Ikiugu & Schultz, 2006). By doing so, they can effectively support the self-determination of individuals living with mental illness and provide opportunities for practicing social justice.
Collective empowerment aims that characterize participatory research are congruent with occupational therapy's aim to enable empowerment through occupation (Townsend et al., 2000).
This study also demonstrates that research can be an important occupation for marginalized populations such as persons living with mental illness. There is an opportunity to conduct participatory research focused specifically on the occupational injustices faced by this population and identifying opportunities for mitigating these injustices in collaboration with persons with lived experience of mental illness. Considering research as an occupation can be important specifically for occupational scientists who study the concept of occupation itself and it can shed light on the ideas of occupation that are usually taken for granted. In Townsend's study (2000) focused on the clubhouse model, research was considered a meaningful occupation involving three opportunities for exploration: data collection and analysis, education, and action. Research as an important occupation was also discussed by Law (1997), who notes that providing opportunities for individuals to participate in the occupation of research may be considered as an important role for occupational therapists in community development (Law, 1997).
Our review also demonstrates that the experience of being a co-researcher may be challenging for persons living with mental illness.
Being unfamiliar with occupation of research (Bryant et al., 2010), fear and anxiety during the focus groups (Bryant et al., 2012), and technical difficulties are examples of challenges that persons living with mental illness experience as they engage in participatory studies (Maniam et al., 2016). It is important for occupational therapy and occupational science researchers and practitioners to consider the challenges that persons living with mental illness may face in the context of conducting participatory research and identify strategies for addressing some of these challenges to improve the experience for persons with lived experiences. Furthermore, if we want to engage persons living with mental illness in participatory research, we need to be willing to share power and control with persons with lived experiences as co-researchers.
Participatory research as a way of resisting stigma has the capacity to reveal the deeper psychological layers in the subjective experience of the stigma of mental illness and promote stigma resistance. The role of participatory research in promoting stigma resistance among persons with lived experiences of mental illness is documented in the literature (Rudnick, 2012; Whitley et al., 2020). Whitley et al. (2020) pointed out that participatory research is a feasible anti-stigma intervention and could be an effective means of stigma reduction. Rudnick (2012) also believed that stigma is a social injustice and argued that stigma could be decreased by involving persons with mental illness in the research process in which the expertise of these individuals is respected. There is a need within the field of occupational therapy and occupational science to consider the potential of participatory research to mitigate the traumatic impact of stigma among persons living with mental illness.
Implications for Practice
Occupational therapy literature highlights that mental health consumers should be central to decision-making, and their choice should underpin their recovery process (Arblaster et al., 2018; Birken & Bryant, 2019). Participatory approaches align closely with recovery principles, which highlight the need for learning from lived experiences (Arblaster et al., 2019). Occupational therapy and occupational science could benefit from conducting research alongside persons with lived experiences in identifying occupational issues relevant to their lives, and in the co-design of novel interventions that are relevant and meaningful in the lives of persons living with mental illness.
Occupational therapists can find opportunities to collaborate with researchers and persons with lived experiences in conducts of participatory studies. We believe that investigating both the potentials and limitations of doing participatory research with mental health consumers will be insightful for researchers and it helps to achieve a more practical understanding of the participatory research approach.
Implications for Research and Policy
Future occupational therapy and occupational science research in mental health should focus on conducting studies that involve persons with mental illness in the research and that provide refinements to practice. As the popularity of participatory methodologies grows, it is important to include critical reflection to find ways to overcome the obstacles and issues. It is worth mentioning that, in most of the included studies, participants were not engaged in all stages of the research. While it is challenging to incorporate all elements of participatory research into a single project (Gray et al., 2000), optimal outcomes can be achieved when occupational therapists and scientists embrace the values and principles of participatory research, ensuring a balanced power dynamic that maximizes the meaningful involvement of participants across all stages of the study.
There is also a need for policies at the university level to facilitate the process of conducting participatory research and avoid delays in obtaining ethical approval for projects where participants are also co-researchers. Funding opportunities are also needed for participatory projects to provide necessary resources to extend the use of participatory approaches in diverse settings and with diverse persons. We also need policies that support involving persons living with mental health in the design of new and re-design of the existing occupational therapy services to enhance the relevance of practice.
Limitations
Several limitations in this study are acknowledged. First, we acknowledge that we could not distinguish between studies of varying degrees of quality by conducting a scoping review because scoping reviews do not involve a critical appraisal of included studies or the aggregation of data. Second, we reported the level of participation in the included studies based on the information provided by the authors. There is a possibility that some information related to the process of action and reflection in the included studies has been deleted due to word limitations. Third, although all the included studies were within the field of occupational therapy or occupational science, most of the authors did not discuss how participatory research can inform occupational therapy or occupational science. Fourth, the first author analyzed the data (EJ). She identifies as a Muslim woman without the lived experience of mental illness and recognizes that these social locations may have influenced the way that she analyzed and interpreted the findings of the included studies. Finally, most of the studies included in this review did not provide demographic characteristics of the participants such as clinical characteristics, disability, race, ethnicity, or the 2SLGBTQ + status. As a result, it would be difficult to comment on the ways in which the demographic characteristics of co-researchers in participatory projects impact the process of conducting research.
Conclusion
The findings of this study underscore the importance of participatory research within the field of occupational therapy and occupational science with persons with lived and living experiences of mental illness. Involving individuals living with mental illness in all stages of research can help to shape the mental health system to become one that is more relevant, effective, and compassionate by incorporating the wisdom of persons with mental illness in its design and ongoing refinement. The findings of this study suggest that participatory approaches have been increasingly adopted by occupational therapy and occupational science to maximize the possibility that occupation-based services are relevant and meaningful for persons with mental illness. We hope that the findings of this review provide insights for researchers, practitioners, and persons with lived experiences about the use of occupation-focused participatory methods with persons living with mental illness and stimulate novel ideas for using these approaches with marginalized groups more commonly.
Key Messages
Participatory research by persons living with mental illness and occupational therapists can influence service delivery and design.
Further investigation of the potential and challenges of occupation-focused participatory research could increase practical understanding.
Footnotes
Acknowledgements
We acknowledge the research and scholarly communications of the librarian for her assistance in guiding the search strategy and collection of search terms used to conduct this review.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Disclosure Statement
The authors claim no financial interest or benefit arising from the direct applications of this research.
Supplemental Material
Supplemental material for this article is available online.
