Abstract
Psychiatry currently faces the following four intersecting challenges: technological disruption through artificial intelligence (AI); the loss of exclusive prescribing authority; escalating systemic constraints within public psychiatry, and market-driven models in private practice. Together, these forces challenge the specialty’s traditional identity, narrowing its scope towards containment rather than recovery and meaning-making, and risk diminishing the specialty’s relevance if left unaddressed. To respond, we propose a structured approach based on three concentric domains of action, the circles of control, influence, and concern, to differentiate what psychiatry can act on directly, shape through collaboration, or advocate for systemically. Within the circle of control, the AIMS framework (Assessment, Intervention, Monitoring, Step-Up/Step-Down) offers a practical structure to refocus care on relational depth, ethical decision-making, and contextual continuity. The circle of influence is addressed through reform in training and interdisciplinary culture, equipping psychiatrists to lead reflectively and integrate technology wisely. Reclaiming psychiatry’s biopsychosocial identity lies at the centre of this renewal, combining biological sophistication, psychological fluency, and social awareness to restore the discipline’s integrative purpose. Rather than competing with AI, psychiatry must redefine its value through those capacities that cannot be automated: empathy, interpretation, and ethical discernment. The specialty’s future will be secured not by speed or compliance, but by its ability to hold complexity, foster recovery, and sustain human connection in an increasingly algorithmic world.
Keywords
Introduction
Psychiatry is undergoing significant transformation due to advances in artificial intelligence (AI) and the expansion of prescribing rights to other healthcare professionals (Cruz-Gonzalez et al., 2025; Dehbozorgi et al., 2025; Kolding et al., 2025; Ray et al., 2022; Rony et al., 2025). This transformation gives rise to five interrelated challenges that are reshaping the profession’s identity and scope. These developments necessitate a redefinition of the profession’s role, relevance, and scope of practice.
Challenge 1 – technological disruption: artificial intelligence and automation
A major challenge arises from the rapid technological disruption reshaping diagnostic and prescribing practice. Historically, psychiatrists have held exclusive authority in diagnosis and prescribing; however, this exclusivity is diminishing. Emerging AI tools are increasingly capable of assisting with structured diagnosis and risk prediction, while prescribing rights are expanding to general practitioners, nurses, and pharmacists globally (Mac Oscar et al., 2025). Early studies suggest the potential for algorithms to support antidepressant selection, titration optimisation, and polypharmacy risk identification (Koutsouleris et al., 2022; Levine et al., 2024; Lim et al., 2024; Mac Oscar et al., 2025). Consequently, psychiatry risks diminishing its distinctiveness if the specialty remains confined to these functions.
Challenge 2 – expansion of prescribing rights
A second challenge relates to the rapid expansion of prescribing authority beyond psychiatry. As noted previously, compounding this technological disruption is the expanding scope of practice for other healthcare professionals. Prescribing rights, once largely confined to physicians, are now increasingly extended to general practitioners, nurses, and pharmacists across the United Kingdom, Australia, and globally (Alsaeed et al., 2025; Cleary et al., 2017). Nurse practitioners are now able to initiate and manage psychotropic medications, while pharmacists with extended scopes are authorised to prescribe in various settings. Physician associates have assumed broad roles in both physical and mental healthcare, and general practitioners are advocating for direct stimulant prescription for ADHD, supported by new guidelines, patient demand, and AI triage tools. This decentralisation of prescribing authority further erodes psychiatry’s traditional boundaries and underscores the urgent need for a strategic re-orientation.
Challenge 3 – systemic pressures in public psychiatry
A third challenge arises from the structural and systemic pressures that define public sector psychiatry. Mental health systems are also simultaneously experiencing considerable strain (Allison et al., 2018; Castle, 2013). In the public sector, psychiatrists are often compelled by service design and resource scarcity to focus on severe and high-risk cases, such as psychosis, violence, forensic complexities, or entrenched system failures, leading to elevated access thresholds that exclude many individuals in need of care until their condition escalates to a crisis (Woon et al., 2024). Psychiatrists are often overwhelmed by crisis response and high acuity, operate at a pace that constrains sustained engagement and trust-building. This has altered the perception of psychiatrists from healers to gatekeepers of limited resources.
Challenge 4 – market forces in private psychiatry
The fourth challenge emerges from the influence of market dynamics and convenience-led models within private psychiatry. The private sector faces a different challenge: convenience-led care. The proliferation of telepsychiatry and rapid-access ADHD assessments has created an incentive structure that prioritises high-volume, low-complexity work, often with insufficient time for comprehensive formulation or follow-up (Woon et al., 2024). This model, while financially profitable, poses reputational risks, as other medical disciplines question psychiatry’s ethical direction and professional depth (Chaulagain et al., 2023).
Challenge 5 – perceived erosion of professional identity
The fifth and overarching challenge is the cumulative effect of these converging forces on psychiatry’s professional identity. These trends: technological disruption, expanded prescribing rights, public sector constraints, and private market pressures are actively eroding psychiatry’s standing both within and outside the medical community. To other healthcare professionals, psychiatry may appear rigid, inaccessible, or ethically compromised. To patients, it can seem delayed, transactional, or even mechanical. To healthcare systems, psychiatry risks being perceived as expensive and replaceable. The perception is increasingly that psychiatrists are specialists in system management, either through medication or risk, rather than true experts in the human mind.
The way forward: working within and expanding the circles
Having outlined five converging challenges, the remainder of this paper turns to solutions. We begin with a practical stance, working within and gradually expanding psychiatry’s circles of control, influence, and concern, and then develop three interrelated strategies: reclaiming the biopsychosocial identity, clarifying psychiatry’s role in the age of AI and defining distinct futures for public and private psychiatry.
To remain relevant and indispensable, psychiatry must evolve beyond its traditional roles. A more profound and essential version of psychiatry, one centred on complexity, relational safety, meaning-making, and recovery, is possible. This evolution requires drawing from the biopsychosocial model while adapting to a future characterised by technology, team-based approaches, and person-led care.
We frame the response across three concentric domains of action. The circle of control encompasses everyday professional behaviours, listening for meaning, formulation quality, proportional risk decisions, and documentation that fosters connection. Within this circle, the AIMS framework (Assessment, Intervention, Monitoring, Step-Up/Step-Down); originally developed in suicide prevention, offers a practical structure for clinical transformation (Table 1) (Kar Ray et al., 2025a, 2025b). The circle of influence covers how psychiatrists shape training, supervision, referral pathways, and interdisciplinary culture; Table 2 on training reform illustrates how reflective practice, AI literacy, and relational leadership can propagate change. The circle of concern comprises the broader ecosystem; policy, funding, workforce and market incentives, addressed later through structural humility and collaborative advocacy. Consistent action within the circle of control enlarges the circle of influence; coordinated influence can, over time, shift the circle of concern.
Changes using the AIMS framework (assessment, intervention, monitoring, and step-up/step-down).

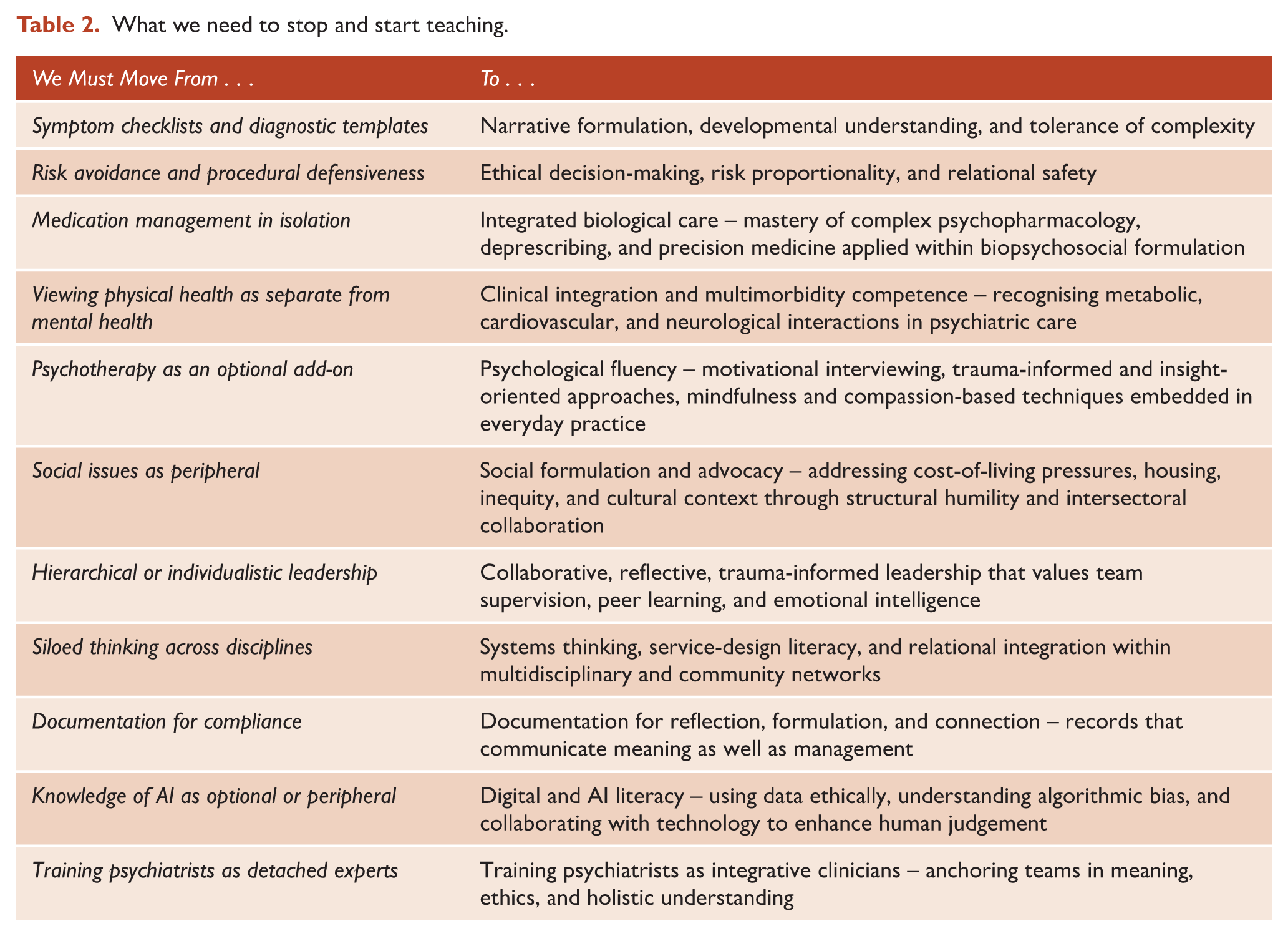
What we need to stop and start teaching.
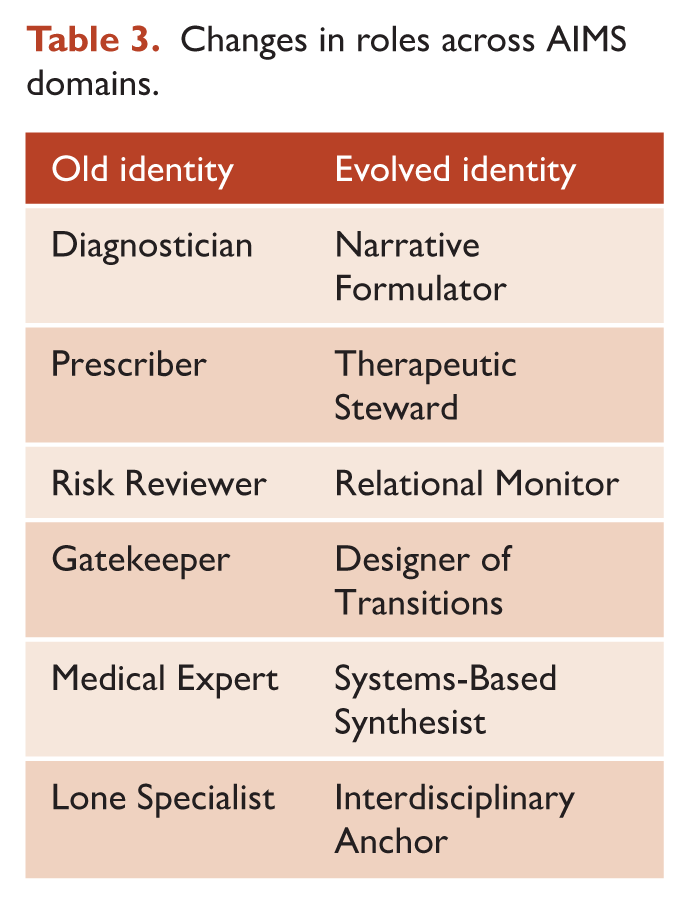
Future psychiatrists will not be defined by competition with AI, but rather by their capacity to perform tasks that AI cannot. Psychiatry relies on relational purpose, trust, and the capacity to engage with suffering. Relational safety is critical for patients to share their experiences and engage in healing, especially in a system increasingly driven by templated assessments and algorithmic alerts. This requires psychiatrists to prioritise empathy and human connection over detached professionalism and efficiency. This entails re-imagining psychiatrists’ roles across the AIMS domains (Table 3) and training reform (Table 2) where everyday supervision and reflective leadership can reshape future practice. As AI assumes more protocol-driven tasks, psychiatrists can reclaim time for narrative formulation and deeper therapeutic presence, transforming the very pace that once constrained care. Psychiatrists are currently perceived more as managers of containment than as facilitators of growth. In public systems, they are often called upon in situations of risk, violence, or non-compliance. In the private sector, the demand is often for quick diagnoses and prescriptions. Rarely are psychiatrists seen as companions through emotional pain or co-creators of recovery. This perception must change. Relational psychiatry implies knowing the patient beyond their risk profile, maintaining curiosity even when behaviour becomes chaotic, offering genuine presence rather than just protocol in moments of despair, and trusting that meaning, not solely medication, can be life-saving. The future does not require psychiatrists who are faster, cheaper, or more compliant, but rather those who look beyond diagnosis, ask more insightful questions, and offer genuine presence rather than just medication.
Changes in roles across AIMS domains.
Reclaiming the biopsychosocial identity
Psychiatry’s foundational strength lies in its biopsychosocial model, which considers biological, psychological, and social dimensions of suffering. However, this model has often been reduced to a theoretical slogan rather than being embodied in practice. In public systems, biological containment frequently dominates, focusing on medication, monitoring, and management. In private settings, psychological exploration is often outsourced to therapists, and the social determinants of distress, such as poverty, violence, and disconnection, are noted but rarely addressed comprehensively. To maintain relevance, psychiatry must embrace the following three areas:
Integrative psychiatry, therefore, is more than just a model; it is a fundamental way of thinking. It involves embracing complexity, refusing to reduce a person to a mere checklist, and listening for the deeper layers beneath a diagnostic label. To rebuild this identity, psychiatrists must develop strong formulation fluency as a core clinical skill, foster interdisciplinary respect rather than hierarchy, lead care plans that are trauma-informed, culturally grounded, and recovery-focused, and offer synthesis rather than asserting supremacy. In a world where AI and allied professionals are increasingly mastering individual components of care, psychiatry’s unique role must be to understand and integrate the whole. Psychiatrists are not just consultants; they deal with complexity and diverse perspectives.
Sustaining this integrative stance requires a transformation in training and professional identity. Future psychiatrists must be equipped to move fluidly between molecules, minds, and meanings; uniting biological sophistication with psychological formulation and social awareness. Training should therefore prioritise the development of both technical and relational expertise: the ability to interpret complex psychopharmacology and multimorbidity alongside the capacity for empathy, reflective practice, and team-based collaboration. Historically, psychiatric education fostered an identity of the psychiatrist as the ultimate expert; yet in contemporary care systems where peer workers, psychologists, nurse prescribers, social workers, and AI assistants all contribute vital knowledge, that stance is no longer viable. Psychiatry must instead position itself as the relational and reflective centrepiece of interdisciplinary care, anchoring the team in meaning, ethics, and complexity. Table 2 outlines practical reforms that can embed this shift, from supervision models to training curricula that cultivate humility, flexibility, and emotional intelligence alongside clinical mastery.
Key skills include formulation fluency (understanding behaviour within developmental, relational, and cultural contexts), digital and AI literacy (wise technology utilisation without outsourcing human judgement), relational presence (attunement, empathy, and therapeutic availability), deprescribing skills, structural awareness, and values-based care planning (helping individuals align their lives with their aspirations).
Furthermore, training environments require change. This involves shifting from tick-box rotations to involvement in team-based, trauma-informed care, as well as reflective practice, and mentorship focused on emotional resilience and professional identity. The next section considers how psychiatry can collaborate with, rather than compete against, artificial intelligence, anchoring human judgement at the centre of technological change.
The role of psychiatry in the age of AI
AI is rapidly assuming many tasks that once defined psychiatric specialisation. These include diagnostic decision support, risk prediction, medication matching and clinical note summation. These highlight areas of psychiatry that can be automated due to their algorithmic nature. AI will undoubtedly excel in pattern detection (speech, movement, facial affect, sleep cycles), triage and risk flagging from electronic health records, medication selection based on complex data, and administrative tasks like form completion and transcription. In these domains, AI will be faster, more consistent, and less biased.
However, AI cannot replicate human attributes such as presence, dignity, and the ability to build hope, or to understand the nuances of trauma and existential suffering. The future of psychiatry lies in collaborating with AI as a clinical partner, focusing on interpreting context, making ethical decisions, creating relational safety, and prioritising meaning over mechanism. This augmentation, rather than replacement, allows psychiatrists to dedicate more time to relational work and understanding individual stories.
As AI transforms assessment, intervention, monitoring, and care pathways, psychiatrists need to adapt without relinquishing their unique role. This adaptation also entails training psychiatrists to interpret AI-derived biological and neuroimaging data wisely, integrating digital biomarkers, genetics, and psychopharmacology within human-centred formulations rather than allowing them to eclipse clinical judgement. Appendix 1 examines how the AIMS model can be applied and adapted to the following diagnoses as AI and prescribing democratisation reshape the landscape: psychosis, mood disorders, neurosis (e.g. anxiety, OCD), eating disorders, personality disorders, and neurodivergence
Distinct futures for public and private psychiatry
While both public and private sectors face pressure leading to role compression, the specific challenges and the approach in each setting are different:
Conclusion
In conclusion, the specialty faces several challenges. AI can now diagnose, monitor, and prescribe; nurses and pharmacists are assuming previously protected clinical roles; healthcare systems demand risk management over recovery; and both the public and professionals are losing faith in the depth and intrinsic value of psychiatric practice.
Psychiatrists therefore need to relinquish roles that others can now perform and concentrate on those skills only they can provide. They should reclaim psychological and narrative work alongside biological management, actively design care systems rather than merely reacting to them, and train psychiatrists for the future, not the past. The profession must advocate for the importance of time, trust, and relationship, instead of succumbing solely to demands for risk management, access, and efficiency.
While many of the systemic pressures shaping psychiatry lie beyond the profession’s immediate reach, the circle of concern defined by policy, funding, and workforce design, the discipline can still model integrity within constraint. Acknowledging that systems often prioritise throughput over depth, psychiatrists can act where they retain influence: clinical reasoning, team culture, and values-based leadership. In time, consistent action at these levels can begin to reshape the very structures that now limit them.
The world does not need faster psychiatrists but deeper ones. It requires more interpreters of meaning, not just more prescribers, and more containment delivered with dignity, not just more control. Psychiatry remains the last medical discipline that truly holds space for the soul, which must not be surrendered to speed, system pressure, or self-doubt. Psychiatry must evolve; it must slow down to matter more, transforming from merely relevant to truly restorative. As Antoine de Saint-Exupéry wisely stated, “The task is not to predict the future, but to shape it.” Psychiatry’s future is not predetermined by algorithms or legislation; it will be written by those within the profession willing to lead with empathy, imagination, and unwavering integrity.
Supplemental Material
sj-docx-1-anp-10.1177_00048674251401028 – Supplemental material for The future of psychiatry: Reclaiming relevance in an era of technological and systemic transformation
Supplemental material, sj-docx-1-anp-10.1177_00048674251401028 for The future of psychiatry: Reclaiming relevance in an era of technological and systemic transformation by Manaan Kar Ray, Frances Dark and Steve Kisely in Australian & New Zealand Journal of Psychiatry
Supplemental Material
sj-docx-2-anp-10.1177_00048674251401028 – Supplemental material for The future of psychiatry: Reclaiming relevance in an era of technological and systemic transformation
Supplemental material, sj-docx-2-anp-10.1177_00048674251401028 for The future of psychiatry: Reclaiming relevance in an era of technological and systemic transformation by Manaan Kar Ray, Frances Dark and Steve Kisely in Australian & New Zealand Journal of Psychiatry
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
