Abstract

To the Editor
Osmotic demyelination syndrome (ODS) arises due to osmotic shifts affecting oligodendrocytes and is associated with rapid correction of chronic hyponatremia (Sheikh et al., 2018; Singh et al., 2014). Numerous neurological and psychiatric sequelae can result from ODS, depending on the location of lesions that are typically identified using magnetic resonance imaging (MRI). Cotard syndrome is marked by nihilistic delusions and has not been reported in association with ODS (Ramirez-Bermudez et al., 2010).
We describe a case of a 46-year-old Caucasian female who presented with ataxia, confusion and nihilistic delusions 6 weeks after an index presentation with confusion, hypovolemia, expressive dysphasia and upper limb ataxia, attributed to hypovolemic hyponatraemia.
The patient’s medical history included mild childhood intellectual disability and epilepsy, hypertension, chronic kidney disease and asthma. Her medications included carbamazepine, hydrochlorothiazide and fluticasone/salmeterol.
The index presentation was precipitated by bizarre dietary changes over the preceding 4 months, consisting predominantly of vegan meals and diet ‘shakes’. Her oral intake precipitously decreased secondary to unfounded fears regarding renal function. Neurological examination demonstrated right horizontal nystagmus, left sided upper limb and bilateral lower limb ataxia. Investigations demonstrated a serum sodium of 115 mmol/L consistent with hypovolemic hyponatremia. She was managed with intravenous normal saline in which her sodium increased from 115 to 125 mmol/L over the next 24 hours. A non-contrast MRI brain demonstrated no cause for her ataxia. Her clinical neurological status improved and she was discharged.
She represented 6 weeks later with decreased mobilisation, assistance with meals/self-care and left arm ataxia. Psychomotor retardation was noted with poverty of thought and speech, dysthymia, insomnia, marked anxiety and nihilistic delusions. She would verbalise that her hands were missing, she did not have a stomach and when looking into the mirror would comment that she does not exist. She required constant prompting to complete basic tasks and her cognitive assessments demonstrated deficits in perception, visuospatial abnormalities and clock-drawing.
A repeat MRI brain demonstrated a non-enhancing T2/fluid attenuated inversion recovery (FLAIR) hyperintensity within the central pons, consistent with a diagnosis of central pontine myelinosis (CPM) (Figure 1).
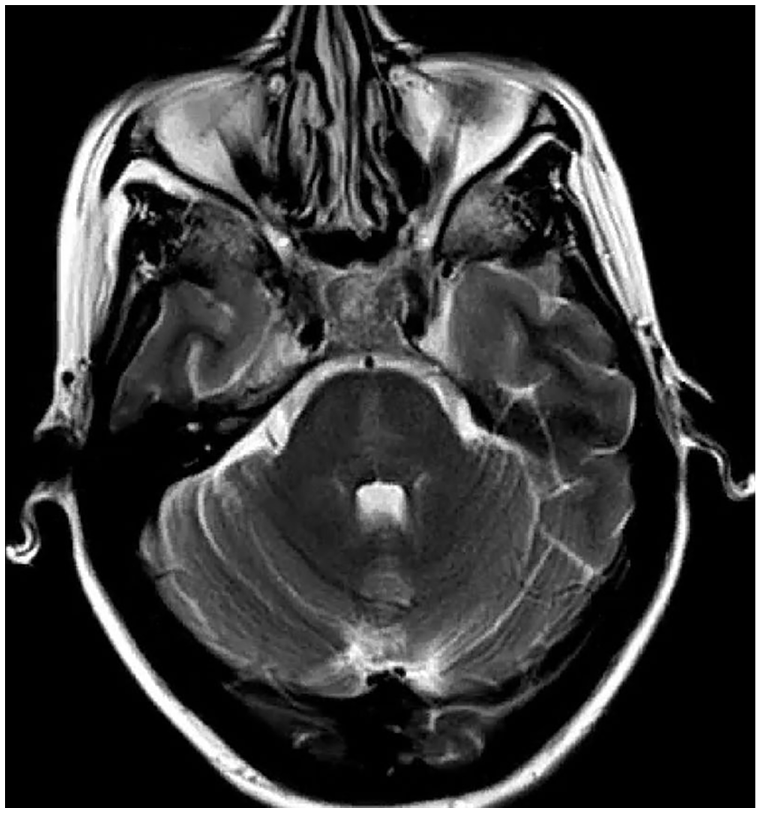
T2 MRI non-enhancing hyperintensity within the central pons.
Olanzapine and escitalopram were commenced and she was discharged with a prolonged rehabilitation admission for her CPM. Her nihilistic delusions and motivation improved at 6-month follow-up.
This case adds to the literature regarding neurological conditions associated with Cotard syndrome and further highlights the need to investigate people with Cotard syndrome for an underlying neurological disorder (Ramirez-Bermudez et al., 2010).
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship and/or publication of this article.
Consent for Publication
The patient has provided written consent for publication of this case report.
