Abstract

To the Editor
Hypoxic-ischemic injury brain injury (HIBI) manifests with cognitive impairments ranging from coma to dementia (Anderson and Arciniegas, 2010). There are no published reports of psychosis in HIBI. A 30-year-woman in her puerperium came agitated, cursing and hitting. She was unable to identify her parents and husband and believed they had turned sorcerers performing religious rituals. She said sorcerers had brought her to a jungle for sacrifice. She avoided communicating with the hospital staff and was suspicious of the food and medications. Her visual and auditory impairments made the interview difficult; her husband served as an interlocutor.
The patient had delivered her third child about 6 weeks ago by Cesarean section and suffered acute severe blood loss due to placenta increta necessitating a subtotal hysterectomy. Following this, she was unconscious for 15–20 days. When she was conscious, she became irritable and suspicious. After discharge, at home, she refused to identify her daughters, said they were dolls implanted by sorcerers. She had no memory of giving birth to her son, refused to hold him, denying ever giving birth to him. Her suspiciousness and hostile behavior caused her current admission. During the inpatient stay, she harbored suicidal wishes, tried jumping from a window, saying that sorcerers were going to sacrifice her, and she would better be dead than killed.
Magnetic resonance imaging (MRI) of the brain revealed multiple T2/fluid-attenuated inversion recovery (FLAIR) hyperintense lesions and extensive ischemic changes in bilateral temporal lobes and hippocampi, as in HIBI (Figure 1). Visual evoked potentials were absent bilaterally. During Brainstem Evoked Response Audiometry, no V nerve peaks were seen. Her orientation and sensorium were intact; however, there were gross lapses in recent memory and executive functioning. A formal neuropsychiatric evaluation was not possible.
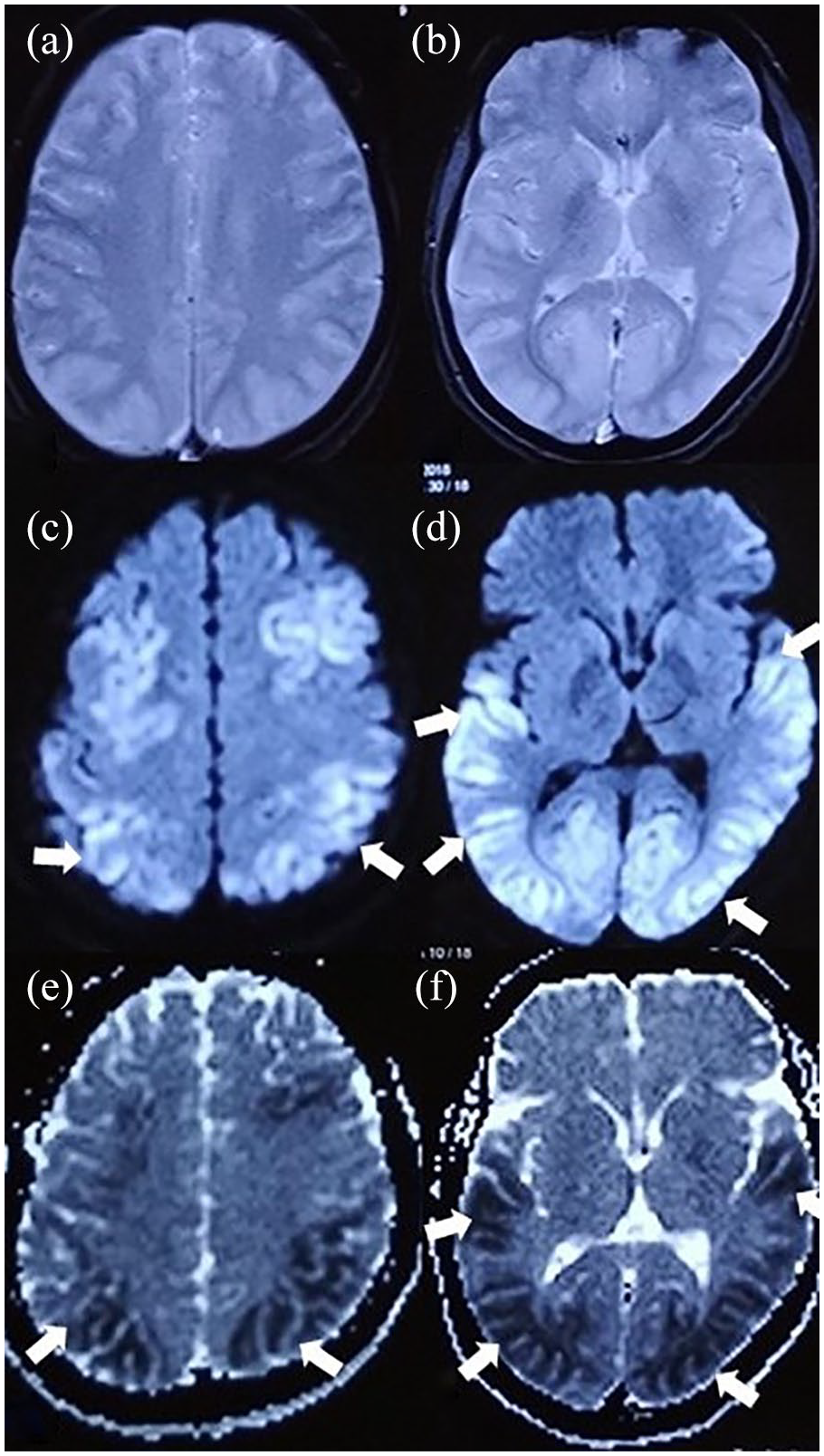
Axial T2W MRI of brain: (a, b) gyral swelling and obliteration of sulci in bilateral cerebral hemisphere. Axial diffusion weighted imaging (c, d) and corresponding ADC map (e, f). Cortical diffusion restriction in bilateral cerebral hemisphere more so in temporo-occipital region (arrows in c–f).
The involvement of hippocampi and temporal lobes was in favor of organic psychosis. The functional involvement of auditory and visual cortical regions could explain the auditory and visual impairments and hallucinations (Oyebode, 2008). The onset of persecutory delusions during the puerperal period and the resolution of psychosis within few months suggested postpartum psychosis (Bergink et al., 2016). We diagnosed organic psychosis due to HIBI and kept postpartum psychosis as a differential as there is no official diagnostic code for postpartum psychosis.
We followed the standard suicide management protocol and pharmacological management with injectable haloperidol 5 mg and promethazine 25 mg, which was helpful. The patient recovered from psychosis but continued having prominent memory deficits even at 6-month follow-up.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship and/or publication of this article.
