Abstract
Objective:
The objective is to summarise recent findings from the 2010 Australian Survey of High Impact Psychosis (SHIP) and examine their implications for future policy and planning to improve mental health, physical health and other circumstances of people with a psychotic disorder.
Methods:
Survey of High Impact Psychosis collected nationally representative data on 1825 people with psychotic illness. Over 60 papers have been published covering key challenges reported by participants: financial problems, loneliness and social isolation, unemployment, poor physical health, uncontrolled symptoms of mental illness, and lack of stable, suitable housing. Findings are summarised under the rubric of participant-ranked top challenges.
Results:
The main income source for the majority (85%) of participants was a government benefit. Only one-third was employed, and the most appropriate employment services for this group were under-utilised. High rates of loneliness and social isolation impacted mental and physical health. The rate of cardiometabolic disease was well above the general population rate, and associated risk factors were present from a very young age. Childhood abuse (30.6%), adult violent victimisation (16.4%) and alcohol and substance abuse/dependence (lifetime rates of 50.5% and 54.5%, respectively) complicated the clinical profile. Treatment with medication was suboptimal, with physical health conditions undertreated, a high rate of psychotropic polypharmacy and underutilisation of clozapine in chronic persistent psychotic illness. Only 38.6% received evidence-based psychosocial therapies. In the previous year, 27.4% had changed housing and 12.8% had been homeless, on average for 155 days.
Conclusion:
Money, social engagement and employment are the most important challenges for people with psychotic illness, as well as good physical and mental health. An integrated approach to recovery is needed to optimise service delivery and augment evidence-based clinical practice with measures to improve physical health and social circumstances. Meeting these challenges has the potential to reduce costs to government and society, as well as promote recovery.
Introduction
The 2010 Australian national survey of psychotic disorders, the Survey of High Impact Psychosis (SHIP), created the rare opportunity to collect detailed data on the profile and experiences of Australians with a psychotic illness using a large, representative national prevalence sample (N = 1825). The interview schedule covered the following: psychopathology, functioning and disability, substance use, education, employment and income, accommodation, medication use, service utilisation and needs. In addition, SHIP measured outcomes related to physical health (including fasting blood tests) and included measures of premorbid and current cognitive function. SHIP also examined the role of non-government organisations (NGOs) in supporting people with severe mental illness. Finally, the Australian Schizophrenia Research Bank funded an additional blood collection for the extraction and storage of DNA and plasma samples. These are currently being analysed, with the DNA collected also part of the ongoing Psychiatric Genomics Consortium Psych-Chip Study.
In addition to the survey findings which were issued as a report to the Department of Health and Ageing at the end of 2011, two comprehensive overview papers were published in 2012 and 2014. The first appeared in the Australian and New Zealand Journal of Psychiatry (Morgan et al., 2012b). As well as presenting a summary of the results, this paper included two important yardsticks for interpreting the survey findings. First, outcomes for people with psychotic illness were compared with data for the general Australian population, especially in the areas of employment, education, homelessness, physical health, smoking and substance use. These comparisons were facilitated by the inclusion of items from the 2007 National Mental Health Survey of 8841 households (Slade et al., 2009) and from various Australian Bureau of Statistics and other population surveys (Morgan et al., 2012b). This approach identified gaps in outcomes and achievements and, where gaps were known to exist, quantified differences between SHIP participants and the general population (Morgan et al., 2012b). The second set of comparisons was against data collected in 1997–1998 in the first Australian national survey of psychotic disorders, the Low Prevalence (Psychotic) Disorders Study (LPDS) (Jablensky et al., 2000); this was possible through the inclusion of many of the same items in both studies. Comparisons between the two surveys were constrained to participants sampled from the same recruitment sources (recorded contacts with inpatient and outpatient/community mental health services over a 1-month period) to optimise comparability. Changes over time were identified or, as in the case of smoking prevalence, lack of change, where change might have been expected (Morgan et al., 2012b). The second overview paper, published in Psychological Medicine (Morgan et al., 2014), presented descriptive findings, including data on premorbid intelligence quotient (IQ) and current cognitive function by diagnostic groups (schizophrenia, schizoaffective disorder, bipolar disorder with psychotic features, depressive psychosis and delusional disorders and other nonorganic psychotic disorders) with detailed supplementary tables by diagnosis for many of the variables measured in the survey (Morgan et al., 2014).
There have been more than 60 publications from SHIP, with more in preparation. The survey’s epidemiological sampling design ensures that its findings are generalisable to adults in contact with public mental health treatment services. However, it does miss those people who are solely in treatment in general medical practices or private psychiatric/psychological settings, homeless people not in contact with any mental health services, people in prison and people with insufficient English or cognitive function to be able to complete the interview. The response rate among the 4189 people contacted for interview from those screen-positive for psychosis and randomised was 44%. Comparison of screening data, including symptom profiles, between interviewed participants and those selected for interview but not participating for any reason indicated no systematic selection biases (Morgan et al., 2012b).
The aim of this paper is to summarise the recent findings for clinicians, researchers, service providers, policymakers, consumers and other stakeholders and to examine their implications for future policy and the planning of initiatives to improve mental health, physical health and social circumstances of people with psychotic disorders (see Table 1). A full list of published studies is provided in Table 2.
Evidence from SHIP on challenges for people with psychotic illness.
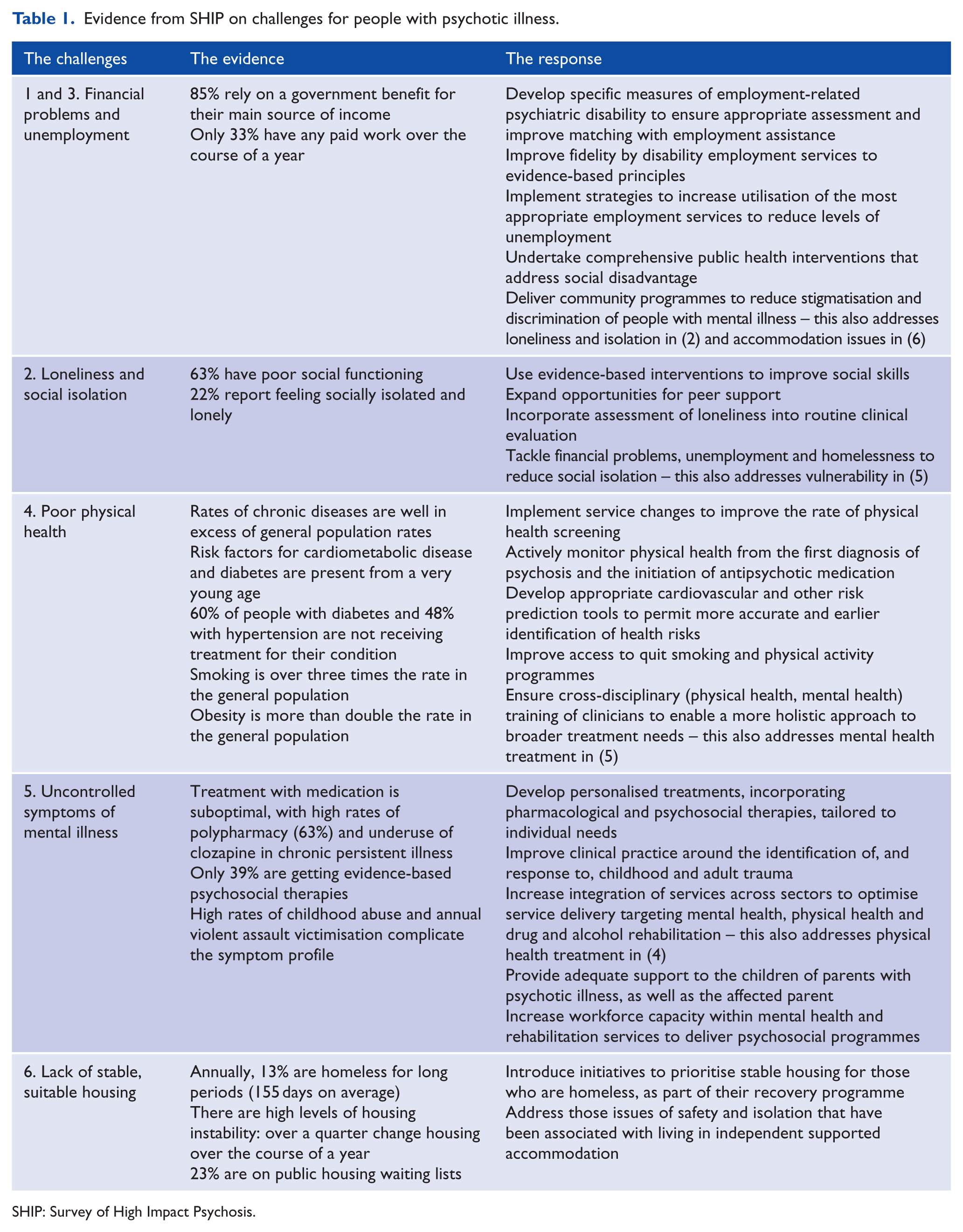
SHIP: Survey of High Impact Psychosis.
Publications, by theme, from the Survey of High Impact Psychosis (SHIP).
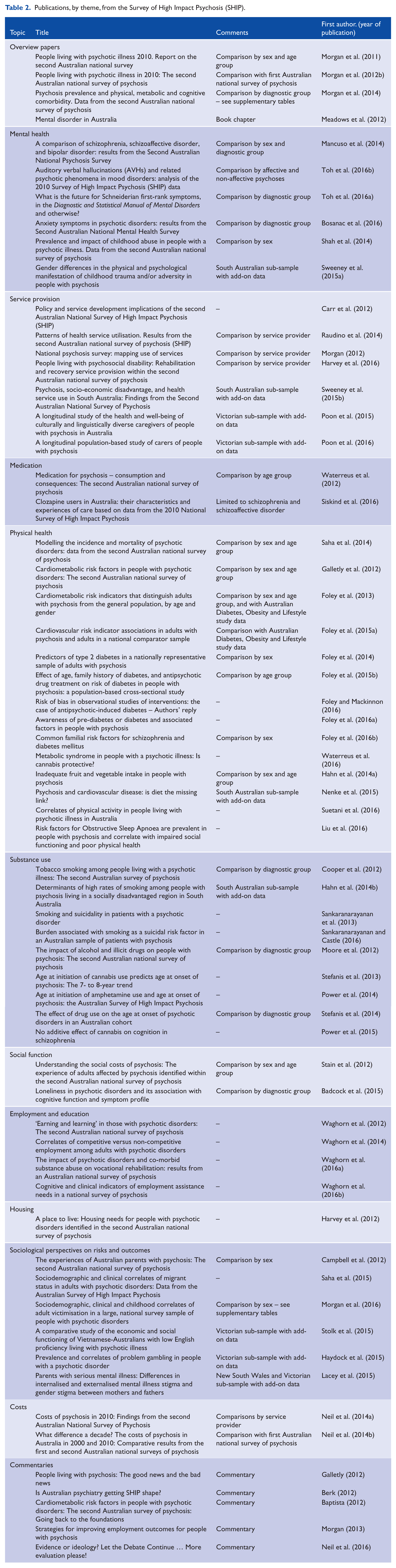
The 2010 SHIP survey was approved by institutional human research ethics committees at each of the seven study sites and all participants provided written, informed consent.
Summary of findings
The framework for presenting these findings will be under the rubric of the six top-ranked challenges that the 2010 SHIP survey participants themselves expressed (see Figures 1 and 2). These challenges were the same for younger (18–34 years) and older (35–64 years) age groups, and for males and females, albeit with some minor variation in the order of rankings.
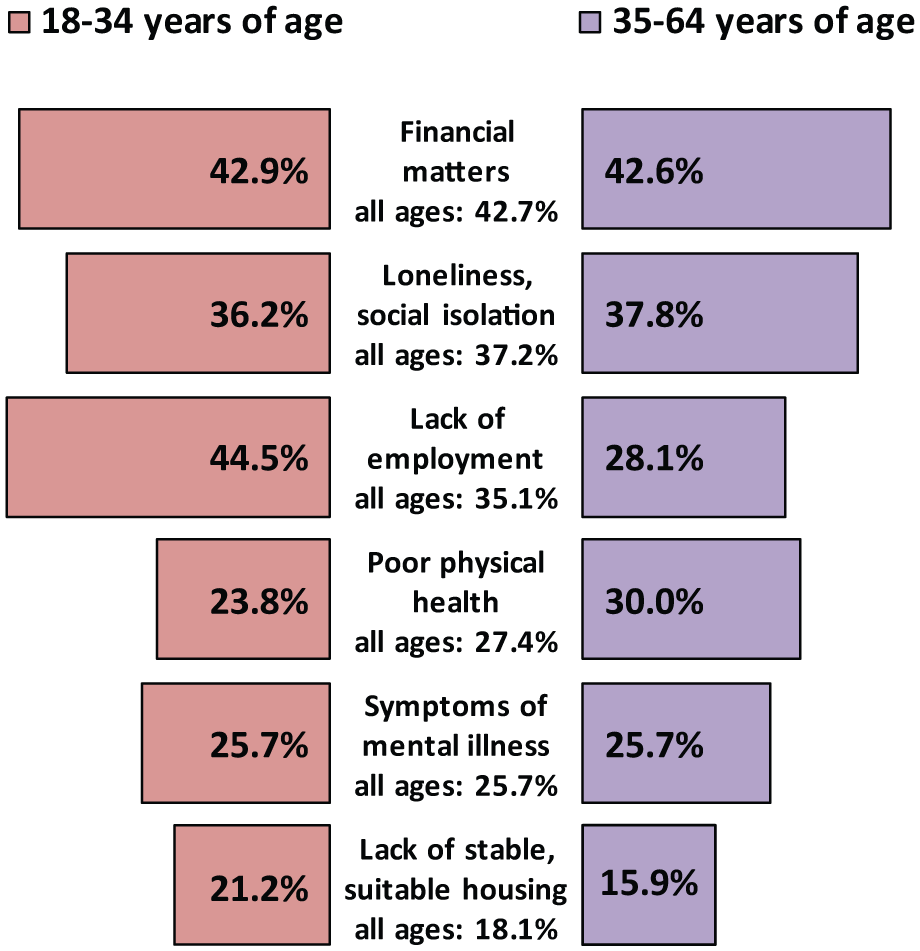
Top-ranked challenges for people with psychotic illness by age group.
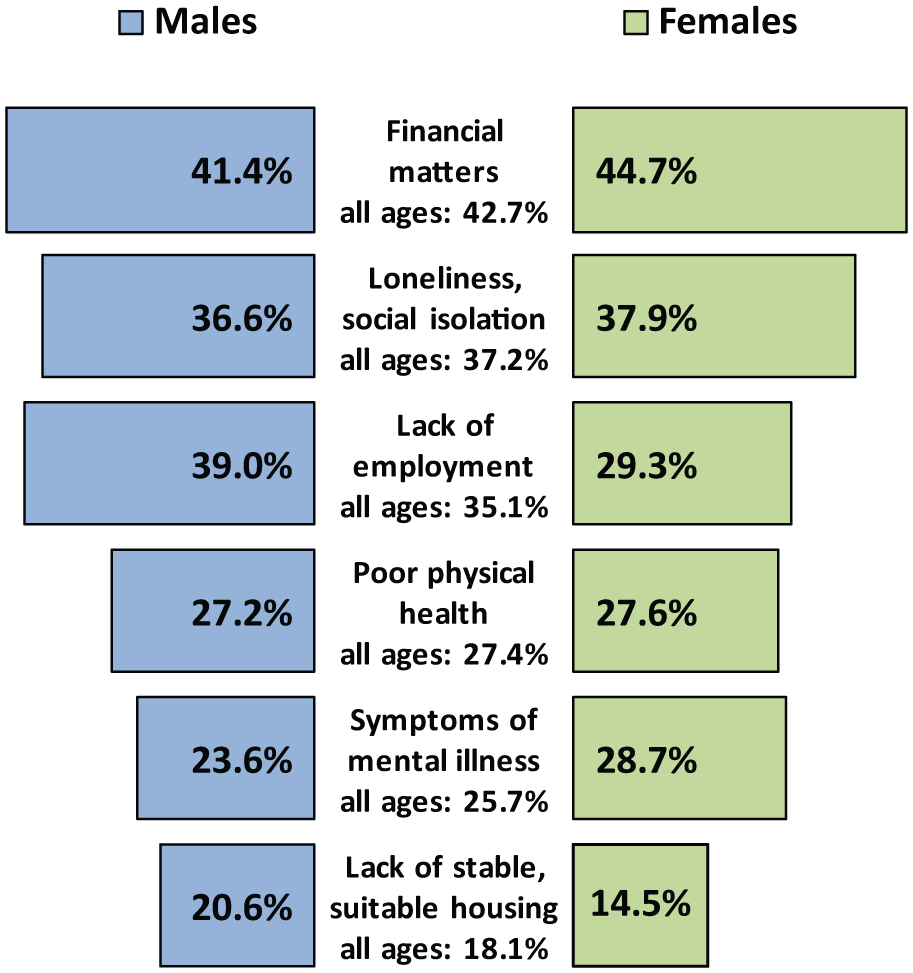
Top-ranked challenges for people with psychotic illness by sex.
Financial problems and unemployment
Employment is the best treatment. Working has helped with my mental health problem. The only way to get better is to keep your mind active. (SHIP participant)
Challenge 1 – financial problems – and challenge 3 – unemployment – are dealt with together since they are closely linked, with access to competitive employment being one of the most effective means of addressing financial challenges. Of note, lack of employment was the top-ranked challenge for those in the younger age group ahead of financial matters, and loneliness and social isolation, but ranked third in the older age group.
The majority of survey participants (59.2%) reported a total net income in the range of AU$500–AU$799 per fortnight, roughly equivalent to the disability support pension at the time of the survey. Since the main income source for 85.0% of participants was a government benefit, this is not unexpected but does highlight the potential for competitive employment to ameliorate financial hardship (Morgan et al., 2011).
SHIP found that 21.5% of participants were employed at the time of interview, and 32.7% had been employed at some time in the preceding 12 months. The percentage in employment had increased since the 1997–1998 LPDS (Morgan et al., 2012b), but was still disappointingly low given national initiatives over that period to improve disability employment services and the growing shift to a recovery-focussed framework for mental health service provision (Waghorn et al., 2012). Notably, the proportion of people in employment was three to five times lower in SHIP participants compared to the general population in the same age range (Waghorn et al., 2012). Moreover, only a very small proportion (4.1% of all participants) were in full-time employment and not reliant on government income support payments as their primary source of income (unpublished SHIP data). Not surprisingly, being employed at the time of the survey was significantly correlated with having completed secondary schooling, attaining a post-school qualification and reporting no difficulty with reading and writing (Waghorn et al., 2012).
Low employment levels give rise to substantial costs to society in terms of lost or forgone production. There are also substantial financial costs to government through the provision of income support payments and additional costs due to tax forgone as a result of lower levels of production. Using SHIP data, Neil et al. (2014a) have quantified the cost of productivity loss (not including costs attributed to carers) at AU$2540 million per year, while the cost to government was assessed at AU$1430 million per year (tax forgone to government: AU$540 million; provision of income support: AU$890 million). There are good indications that the proportion of individuals employed can be increased. Waghorn and colleagues note that only 30.5% of those looking for work were getting assistance from the most appropriate type of service which, at the time, was Disability Employment Services, while 32.1% were receiving assistance from the least appropriate service, namely, main stream employment services – now known as Job Active (Waghorn et al., 2012). More recently, Waghorn et al. (2014) identified a negative correlation between using employment services and being in competitive employment even though competitive employment is the very type of employment that Australian employment services are meant to deliver. This suggests a system-wide deviation at the time of the survey from evidence-based Individual Placement and Support principles.
In order to increase the proportion of individuals employed and reduce the financial burden associated with unemployment, access to disability employment services needs to be better targeted. For example, Waghorn et al. (2016a) found that those diagnosed with psychotic disorders and co-morbid substance abuse were underutilising the most suitable employment services. Moreover, a whole-of-government approach is needed to reduce obstacles to workforce participation, particularly for those in transition to stable employment who are moving in and out of employment during different phases of illness. For them, financial disincentives such as lack of a financial safety net and loss of disability benefits are a continuing barrier that can lead to loss of motivation, similar to issues identified in the US Social Security Administration’s Mental Health Treatment Study (Drake et al., 2013, 2016). A further problem is the lack of a measure of employment-related psychiatric disability for use by rehabilitation professionals to improve the matching of intensive employment assistance to those most in need (Waghorn et al., 2016b). Such a measure is urgently needed, given the recent introduction of the new National Disability Insurance Scheme. This scheme aims to comprehensively support all people with disabilities throughout the lifespan in all major life domains, including community participation, education and employment. At this point in time, psychiatric disorders are defined only by the extent of psychosocial disability, and clear determinations of who can access this programme are still being developed (National Disability Insurance Agency [NDIA], 2016). Concurrently, given that early onset of psychotic illness (before the age of 25 years for 64.8% of participants (Morgan et al., 2012b)) also interrupts educational attainment, recovery programmes that meet educational and vocational training goals are likely to have a positive impact on employment outcomes.
Financial hardship impinges on other aspects of living, including basic needs such as good nutrition and safe, stable accommodation. The implications for participants who were parents with dependent children living with them (23.6% of the women surveyed and 5.5% of the men) are particularly serious (Campbell et al., 2012). Over the previous year, one-quarter (28.4%) of SHIP participants had run out of food at least once because they could not afford to buy more (Morgan et al., 2011). Hahn et al. (2014a) examined adequacy of fruit and vegetable consumption in SHIP and found that running out of food (among other variables) was significantly associated with failure to meet dietary guidelines. This could be accounted for statistically in multivariate modelling that included smoking as a predictor. Although interactions were not examined, the very high rate of smoking in this population, and its associated cost, is likely to be correlated with financial hardship and availability of money to buy food; this is supported by unpublished SHIP data showing that 33.5% of smokers had run out of food in the previous year compared to 18.2% of non-smokers (unpublished SHIP data).
Of interest, Saha et al. (2015) found that migrants with psychosis who were included in the SHIP survey (17.8% of the total) had better outcomes overall than individuals who were Australian-born. Specifically, they were more likely to have completed a higher level of schooling, to live in areas of greater socio-economic advantage, to be employed and, if working, to be employed full-time. This pattern of associations is at variance with other research which generally shows poorer outcomes for migrants (Saha et al., 2015). In part, this difference may be due to pre-migration health screening of potential immigrants, although two-thirds of SHIP migrants were under 16 years of age at time of immigration, suggesting they arrived as part of a family unit. Additionally, SHIP excluded people who were not proficient in English, which may have biased the sample towards migrants who were higher achievers.
Loneliness and social isolation
It is lonely living with a mental illness. Social isolation is the worst thing. (SHIP participant)
Loneliness and social isolation were highly prevalent among people with psychotic illness. Stain et al. (2012) noted that two-thirds (68.8%) of SHIP participants had not participated in any social activities in the previous year, citing experience and fear of stigma, social anxiety and mental illness as barriers to their participation. Badcock and colleagues found self-reported rates of loneliness of 79.9%, ranging from 74.7% in people with delusional disorders to 93.8% in those with depressive psychosis, and 2.3 times the population prevalence of 35% (comparing with available New Zealand data) (Badcock et al., 2015). At the more severe end of the spectrum, 22.4% of participants felt socially isolated, and 13.3% reported having no friends at all (Morgan et al., 2012b). Moreover, trained SHIP interviewers rated 63.2% of participants as having obvious or severe deficits in social skills (Morgan et al., 2012b), a factor highly correlated with loneliness (Sheridan et al., 2015). SHIP data show that loneliness was associated with symptoms of anhedonia and subjective thought disorder (Badcock et al., 2015). Furthermore, poor social functioning (as measured by the Personal and Social Performance Scale (Morosini et al., 2000)) was associated with higher rates of psychiatric inpatient admissions, involuntary admissions and emergency presentations (Raudino et al., 2014). The consequences of loneliness extend beyond mental health, impacting also on physical health morbidity and mortality (Hawkley and Cacioppo, 2010). In keeping with this, Suetani et al. (2016) found an association in the SHIP data between (a) being physically inactive and (b) loneliness and social dysfunction. Overall, these findings have important implications for mental health services, highlighting the need for specific, evidence-based interventions for loneliness and for the development of social skills in people with psychotic disorders. Yet Stain and colleagues observe that very few people had attended communications and social skills programmes provided either through community mental health services (3.1%) or in the NGO sector (6.7%) (Stain et al., 2012). Furthermore, people with the most severe social dysfunction were significantly less likely to use NGO services in addition to services in the clinical sector, thereby restricting their access to interventions that could meet their social needs (Harvey et al., 2016). The findings also call attention to the potential benefits of other types of intervention. For example, while reducing loneliness and social isolation may have an impact on physical activity, engaging in physical activity will not only improve physical health but also has the potential to improve social connectedness. A study of a subgroup of SHIP participants found that smokers were less likely to participate in social and recreational programmes, suggesting that the high rate of smoking may be a further barrier to social engagement (Hahn et al., 2014b). This finding is also supported by the work of Harvey et al. (2016). Outside the clinic, employment is itself a social structure that provides opportunities for social interaction and building meaningful relations with others. Stain et al. (2012) describe it as one of three key factors contributing to social inclusion, along with social participation and education. Therefore, success in meeting Challenge 3 – Unemployment – will be one important means of meeting Challenge 2 and of alleviating loneliness and social isolation, and their associated adverse health outcomes.
Poor physical health
Look at physical health problems people have. Look at all aspects. Don’t consider mental health in isolation. (SHIP participant)
There is clear evidence worldwide that people with psychotic disorders experience greater physical morbidity, especially cardiometabolic disease, than the general population (Kredentser et al., 2014; Lawrence et al., 2001; Saha et al., 2007). Concomitant with this, life-expectancy is reduced – by 18.7 years on average for men and 16.3 years for women – compared to the general population (Laursen, 2011). This alarming gap is widening (Lawrence et al., 2013; Nielsen et al., 2013; Saha et al., 2007). SHIP analyses provide current Australian estimates of the extent of mortality and morbidity in people with psychotic disorders, including the physical health gap relative to community samples.
Saha and colleagues (Saha et al., 2014) have modelled mortality using SHIP screening population data. Of 6942 people screen-positive for psychosis in the census month, 65 had died by time of interview, well above the expected 16 deaths. The annualised, weighted mortality rate was 12.5 per 1000, with a standardised mortality ratio of 5.5. Underlying premature mortality, early SHIP publications showed that physical health conditions, including asthma, heart or circulatory disorders, severe headaches/migraines, arthritis and diabetes, were well in excess of population rates (Morgan et al., 2012b) and pervasive across the psychosis spectrum (Morgan et al., 2014: – supplementary tables). This is particularly concerning, given over a decade of heightened awareness of these issues following publication of the seminal Australian Duty to Care report (Lawrence et al., 2001).
In a series of papers, Foley and colleagues have explored cardiometabolic risk profiles in people with psychotic illness. They compared cardiometabolic risk indicators in SHIP participants with comparator data for the general population aged 25–64 years drawn from the Australian Diabetes, Obesity and Lifestyle (AusDiab) study (Foley et al., 2013). SHIP data showed that Australians with psychotic illness had significantly higher mean body mass index, waist circumference, diastolic blood pressure, triglycerides and glucose (the latter in women only and not at every age) and significantly lower high-density lipoprotein cholesterol than the AusDiab sample from at least the age of 25 years, consistent with an early propensity to insulin resistance. Tracing the mean risk indicators back to 18 years of age in those with psychosis, the earliest age surveyed by SHIP, showed that widely used at-risk thresholds for key indicators of cardiometabolic disease were exceeded very early. For example, the mean body mass index and waist circumference of the sample already exceeded the obesity threshold at or before 18–19 years of age. Key indicators of the poor physical health of people with psychosis are therefore present early, and interventions to reduce that risk from the point of first diagnosis of psychosis are warranted.
Further analyses by Foley et al. (2014) imply a much earlier onset of diabetes in Australians with psychotic illness compared to other Australians. The prevalence of diabetes was 5.8% in 18- to 24-year-olds with psychotic illness and 7.1% in 25- to 34-year-olds, compared to 0.3% for 25- to 34-year-olds in the general population; peak prevalence occurred 20–30 years earlier than expected. Risk factors associated with diabetes in Australians with psychosis were similar to those in the general population, but the associations were often larger in people with psychosis reflecting the severity of those risk factors in the context of psychotic illness. A multivariate additive model showed that body mass index, treated hypercholesterolaemia and family history of diabetes, but not current antipsychotic medication (clozapine or olanzapine vs other antipsychotics) were significantly associated with current diabetes in the SHIP sample, suggesting that these variables may confound the estimated risk associated with antipsychotic drug treatment. While it was not possible to distinguish type 1 from type 2 diabetes in SHIP data, Foley and colleagues estimate from Australian population data that 85–90% of diabetes cases are likely to be type 2.
Next, Foley et al. (2015a) focussed specifically on correlations among 10 key cardiovascular risk factors. These were waist circumference, body mass index, systolic blood pressure, diastolic blood pressure, current smoking, fasting plasma glucose, total cholesterol, low-density lipoprotein cholesterol, high-density lipoprotein cholesterol and triglycerides – all relevant for the accuracy and utility of cardiovascular risk equation estimates in people with psychosis. They found that Australians with psychotic illness again diverged significantly from other Australians, with a weaker and different pattern of correlations among cardiovascular risk indicators and, for a number of factors, no positive correlation with increasing age. The paper notes that the low or absent association with age is consistent with the expression of increased cardiovascular risk in people with psychotic illness at a very early age, as described in the earlier papers.
Finally, two papers explored the impact of family history of diabetes in the SHIP data. A family history of diabetes was significantly associated with a family history of schizophrenia even when controlling for the participants’ diabetes status and demographic factors. This finding was specific to people with schizophrenia and not any other psychotic disorder. The authors speculate that glucose regulation abnormalities may play a role in the aetiology of schizophrenia (Foley et al., 2016b). A second paper reported that a family history of diabetes influenced the association between antipsychotic drug use and diabetes: antipsychotic medication increased the risk of diabetes in those with no family history of the illness to the same level as those with a positive family history but did not further add to that risk (Foley et al., 2015b). The authors postulate that current clinical practice may inappropriately neglect the risk of diabetes in those without a positive family history of diabetes, focussing only on patients whose family history is seen as a risk. Future research exploring the metabolic effects of antipsychotic medication should stratify samples by family history of diabetes in order to maximise power and better understand pathways of risk.
These findings have implications for health screening and monitoring. The very early elevation of cardiovascular risk indicators (Foley et al., 2013) and the different pattern of correlations among these indicators (Foley et al., 2015a) in people with psychotic illness compared to the general population cast doubt on the suitability of using current predictive instruments developed on much older community samples to assess risk in younger people with psychotic illness. Foley et al. (2015a) highlight the need to evaluate the performance of established risk equations in samples of people with psychotic illness and, very likely, the necessity for different weightings for risk indicators in an optimal risk algorithm.
Regrettably, over time, the proportion of people with a psychotic illness who have received a physical health examination or a fasting blood test over a 12-month period has fallen. The percentages in 2010 were 66.1% for a physical health examination and 64.8% for a blood test compared to 79.6% and 83.1%, respectively, in LPDS in 1997–1998 (Morgan et al., 2012b). This decline may reflect the transition of service provision from inpatient care to community mental health care, with a reduction in the percentage of people with at least one psychiatric inpatient admission between the two surveys from 62.9% to 45.6% (Morgan et al., 2012b). Notably, such examinations are a mandatory component of the admission procedure but, arguably, are much more difficult to arrange and monitor in the community mental health setting. This is an area of great concern. Moreover, SHIP data indicate that active monitoring of physical health status needs to commence at the time of first diagnosis of and initiation of treatment for psychosis, not at ages which may be applicable to the general population.
In addition, Galletly et al. (2012) provide strong evidence from SHIP that, even when physical health conditions have been identified, there is a failure to treat. They found that, for three self-reported medical conditions, only half or fewer of affected individuals were taking medication to treat the condition: hypertension (51.7%), diabetes/hyperglycaemia (39.8%) and hypercholesterolaemia (39.4%). Moreover, the majority of those receiving treatment still recorded levels above the critical threshold on fasting blood tests, indicating ineffective treatment, poor adherence or a combination of these two factors.
Several SHIP papers have focussed on identification of modifiable risk factors for cardiometabolic disease, as these are key targets for intervention. Liu et al. (2016) found high rates of symptoms of obstructive sleep apnoea in the SHIP sample, including pauses in breathing (17.4%) and snoring (41.9%); given that the majority of participants were not in relationships, these self-reported data are likely to be underestimates. By comparison, the prevalence of obstructive sleep apnoea in the general population is estimated to be 3–5%. Morgan and colleagues found that, when modifiable lifestyle risk factors for metabolic syndrome were entered into a multivariable model that included important covariates such as psychotropic medication use, cognitive function, diagnosis, age, sex, illness duration and socio-economic status, two modifiable risk factors remained significant: current smoking (odds ratio = 2.3, 95% confidence interval [CI] = [1.6, 3.2]), and body mass index in the overweight and obese ranges (odds ratio = 4.9, 95% CI = [3.1, 7.8] and odds ratio = 16.8, 95% CI = [10.4, 27.0], respectively) (Morgan et al., 2014). SHIP found particularly high rates of smoking for people with psychotic illness which, at 66.1%, have not changed over the 13 years since the LPDS: over the same period, general population rates fell to 20.2%. Data from Cooper et al. (2012) show that people with psychotic illness are motivated to give up smoking: 72% of current smokers had attempted to give up, with an average of 4.5 quit attempts, but only 42% had sought help to stop smoking.
More intriguing, a recent SHIP paper by Waterreus et al. (2016) corroborates emerging general population data that cannabis use may have a cardiometabolic protective effect. Even after adjustment for potential confounders such as lifestyle, smoking, cognition, antipsychotic medication, diagnosis and socio-demographics, frequent cannabis use in the past year remained associated with significantly lower odds of metabolic syndrome (odds ratio = 0.6, 95% CI = [0.4, 0.8]) in people with psychotic illness. This finding will require replication and further investigation.
Uncontrolled symptoms of mental health
It’s hard to cope with everyday life. It’s terrible having a mental illness. I don’t want illness, to have injections, to feel sick, to be paranoid. I do strange things: talk to myself, hear voices, I’m scared of people … (SHIP participants)
SHIP data quantify the prevalence of psychiatric symptoms and associated direct and indirect symptom burden. In addition to positive symptoms such as hallucinations and delusions, which had a 12-month prevalence of 55.8% and 60.9%, respectively (Morgan et al., 2012a), the 12-month prevalence of symptoms of anxiety and depression was 59.8% and 54.5%, respectively (Morgan et al., 2012b). Negative symptoms comprised the six items of Carpenter’s Deficits Syndrome, but without assessment of aetiological attribution (Kirkpatrick et al., 1989; World Health Organization, 1999): 85.2% of participants recorded at least one negative symptom. Most symptoms were pervasive across all diagnostic groups: schizophrenia, schizoaffective disorder, bipolar disorder with psychosis, depressive psychosis and delusional and other nonorganic psychoses (Morgan et al., 2014: – supplementary tables), although the distribution of specific symptoms varied by diagnosis (Mancuso et al., 2014; Toh et al., 2016a, 2016b).
The clinical management of highly prevalent and often enduring psychiatric symptoms, and especially the need for effective interventions to reduce symptom burden, are fundamental to improving quality of life in psychotic illness. However, SHIP data also point to mental health service needs beyond symptom control. For example, the lifetime rate of alcohol abuse and dependence was 50.5% and of drug abuse and dependence was 54.5%; these are 1.7 and 1.8 times higher, respectively, than the rates reported in the 1997 LPDS (Morgan et al., 2012b). High rates of drug and alcohol comorbidity complicate the clinical profile of people with psychotic illness, adversely affecting behaviours and outcomes. As an example, in SHIP, 37.4% and 39.4% of participants reported risk-taking behaviours associated with alcohol use and substance use, respectively, in the previous year (Moore et al., 2012). These substance-related co-morbidities contribute to the complex service needs of this population. This represents a critical area for intervention, underlining the need for an integrated approach to treatment across mental health and addiction clinical settings.
From a therapeutic perspective, there is also a need to recognise and respond to other life course events that may adversely affect symptom burden, quality of life and potential for recovery. This includes victimisation of people with psychotic illness. SHIP documents high rates of childhood and adult victimisation. Using stringent Australian child protection services criteria, the self-reported prevalence of childhood abuse prior to the onset of illness was 30.6% (Shah et al., 2014). This is double the rate reported for the general population (Reeve and Van Gool, 2013). Women were more likely than men to report childhood abuse (43.6% and 21.7%, respectively) (Shah et al., 2014). Adult victimisation was also prevalent among SHIP participants, with a reported rate of 38.6% in the 12 months prior to interview (Morgan et al., 2016). Violent victimisation in the previous year was reported by 16.4% of participants (males 15.2%; females 18.3%): this was 4.8 times higher than the population rate of 3.4% (6.5 times higher for women; 3.7 times higher for men). Psychiatric sequelae of childhood and adult victimisation, including post-traumatic stress disorder, compound the clinical profile of people with severe mental illness and its treatment. However, both childhood and adult trauma are under-recognised within mental health services: their identification and treatment require significant service development across the mental health sector (Cascardi et al., 1996; Dean et al., 2007; Newman et al., 2010; Read et al., 2005; Silver et al., 2005).
From a broader perspective, many SHIP papers have reported on the adverse impact of non-clinical factors on course and outcome for people with a psychotic illness. For example, significant correlates of adult violent victimisation were socio-demographic and behavioural risk factors that are known to predict victimisation in the general community including childhood abuse, younger age, residence in the most disadvantaged neighbourhoods, homelessness, lifetime alcohol abuse/dependence and prior criminal offending; of the clinical variables, only mania and self-harm were significant in the full multivariable model (Morgan et al., 2016). This highlights the need for a comprehensive preventative strategy that addresses the predisposing elements of social disadvantage underlying increased vulnerability; integral to this is the need to tackle the challenges of financial problems, unemployment and homelessness.
Social cognition refers to processes such as social cue perception, experience sharing, inferring others’ thoughts and emotions and managing emotional reactions to others (Green et al., 2015), and may be markedly impaired in psychotic illness. It is therefore an important treatment target, with benefits related to improved social functioning, reduced loneliness and better clinical outcomes, mentally and physically (see findings reported under Challenge 3: Loneliness and social isolation). Targeting social cognitive deficits also has the potential to reduce vulnerability to victimisation by helping individuals adopt self-protective behaviours and identify and manage threatening situations. However, more research is needed on the nature of social deficits in people with psychotic illness and the efficacy of remediation targeting these deficits (Carr et al., 2012).
The majority of participants were taking medication for their mental health (91.6%) (Waterreus et al., 2012). However, polypharmacy remains an issue for this population, with almost two-thirds (63.4%) taking more than one class of medication and over a quarter (28.1%) of participants with schizophrenia using more than one antipsychotic medication (Waterreus et al., 2012). The majority (84.4%) reported medication side effects, including anticholinergic side effects (51.7%), sedation (44.7%), extrapyramidal side effects (42.0%) and akathisia (36.4%) (Waterreus et al., 2012). Siskind et al. (2016) found that only one-quarter (24.5%) of participants with a diagnosis of schizophrenia or schizoaffective disorder was currently taking clozapine. They concluded that clozapine may be underused, with a large proportion of people with ongoing chronic psychotic illness not receiving the most appropriate treatment according to established guidelines (Galletly et al., 2016). A more fundamental issue for mental health revealed in the SHIP data is the low level of access to adjunctive psychosocial therapies. Only a minority of participants (38.6%) reported that they had received any evidence-based psychosocial therapies in the previous 12 months (unpublished SHIP data), including counselling, psychotherapy and group therapy (30.5%), cognitive behavioural therapy (22.3%) and family therapy (11.4%) (Morgan et al., 2012b).
The first SHIP paper on service utilisation by people with psychotic illness suggests that, in general, use of mental health services was appropriate to illness profiles (Raudino et al., 2014). However, more recently, Harvey et al. (2016) have identified a subgroup of SHIP participants with severe social dysfunction who were accessing community mental health services only, and missing out on important NGO rehabilitation services. Moreover, it remains unclear if service providers are using evidence-based interventions, although the poor uptake of psychosocial interventions noted above suggests much room for improvement. Notably, in the 13 years between the first and second national psychosis surveys, two important service-related changes occurred. First, there was a major shift from use of psychiatric inpatient services (down from 58.7% to 37.6%) to the use of ambulatory and community mental health services (up from 75.3% to 92.8%), with a concomitant increase in the use of NGO and rehabilitation services (up 7.6% and 13.9% points, respectively) (Morgan et al., 2012b). Second, the proportion of people reporting that they needed services that were unavailable or unaffordable dropped from 42.4% in 1997 to 24.9% in 2010. Both these changes over time are likely to have influenced the shift in the proportion of people who said that they were satisfied or very satisfied with their independence, which went up substantially, from 57.6% to 70.8%. By contrast, the proportion of people with psychotic illness who were satisfied or mostly satisfied with life as a whole did not change and, at 47.4% in 2010, was well below the Australian general population figure of 81.5% (Morgan et al., 2012b).
Concomitant with changes in health service utilisation between the 1997 and 1998 LPDS and SHIP, there was a significant redistribution of costs within and away from the health sector, including reductions in inpatient care, increased costs for ambulatory care and a shift towards community-based care by NGOs (Neil et al., 2014b).
Lack of stable, suitable housing
No housing – being homeless and moving around – makes it so hard. Stable housing is very important to maintain good mental health. (SHIP participants)
Access to appropriate accommodation was ranked sixth among challenges for the coming year by all SHIP participants, including younger (18–34 years) and older (35–64 years) participants, and males and females. However, it was endorsed by a larger proportion of younger people and males (21.2% and 20.6%, respectively) than older people and females (15.9% and 14.5%, respectively) – see Figures 1 and 2. In a detailed analysis of SHIP accommodation data, Harvey et al. (2012) make a number of salient points. First, half the sample (52.6%) was very satisfied with their current accommodation. However, 27.4% had changed housing in the previous year, reflecting high levels of housing instability in this population, and 22.7% were on public housing waiting lists for independent accommodation. In addition, some 41.8% of participants who had had a psychiatric admission in the previous 12 months could not recall accommodation options being discussed with them at the time of discharge, and 7.5% had not been offered help and did not have anywhere to live on discharge. Finally, there was some mismatch between current and preferred accommodation. For example, 19.1% of SHIP participants were living in a family home (which was not their own home), yet this was the preferred accommodation for only 10.4%, while only 13.1% were living in their own home which was the preferred accommodation for 39.8%. One-tenth (11.0%) were living in supported group accommodation, although this was the preferred accommodation for only 2.8%. Supported accommodation – either group accommodation with onsite support or housing with in-reach staff support – has been developed especially for people with severe mental illness who are at risk of homelessness and has been associated with a range of clinical and other benefits (Harvey et al., 2012). The doubling of the proportion in supported group accommodation since the 1997–1998 LPDS is in keeping with ongoing deinstitutionalisation and related policy changes over the same period, including the growth of integrated services to provide community-based support. This has led to a 38.5% increase in the costs of supported accommodation over the interval between the two surveys while, on the other hand, utilisation of crisis accommodation has decreased with costs reducing by 84.6% over the same period (Neil et al., 2014b). The low level of preference for supported group accommodation is consistent with wider recognition that most, but not all, people with psychosis prefer to live in independent accommodation with in-reach support as required (Sylvestre et al., 2007). However, the latter type of supported accommodation is associated with decreased safety and increased isolation (Harvey et al., 2012); these concerns remain to be addressed.
Of particular concern is the high proportion of people with psychotic illness who have been homeless in the previous 12 months. There were 5.2% currently homeless at the time of the SHIP interview, 10 times the general population estimate of 0.5% (Morgan et al., 2012b). The percentage reporting any homelessness over the past year was higher, at 12.8%. Moreover, homelessness was enduring: those who had been homeless had spent considerable time so, with a mean of 155 days and a median of 99 days of homelessness over the past year. Homelessness has serious implications for mental health, physical well-being and vulnerability to adult victimisation. It is highly correlated with unemployment and financial problems: to deal with the challenge of homelessness, these other two challenges must be met.
Conclusion
There has been an improvement in mental health services since I was first diagnosed. It has changed so much. So much better. Made me the person I am today. Everything is so much more explained and I understand the illness and meds … (SHIP participant)
Despite the challenges for people with psychotic illness, they remain stubbornly optimistic. Three-quarters (77.4%) of SHIP participants believed that their circumstances would improve over the next 12 months (Morgan et al., 2012b). Critical to improving the lives of people with psychotic illness is a personalised, holistic approach to recovery. Such an approach takes into account mental and physical well-being, quality of life and social context. It is premised on a collaborative model of care with shared decision-making by patient and therapist regarding recovery milestones and the most appropriate means to achieve these (Morgan et al., 2013). At the same time, findings from the SHIP survey highlight the complexity of the needs of people with psychotic illness. Consequently, for their circumstances to alter substantially, their needs demand an integrated, multifaceted approach by services which extends beyond the delivery of good clinical practice and includes strategies aimed at improving socio-structural and socio-demographic circumstances, including the provision of basic necessities of everyday living. Such an approach has long been advocated and requires better efforts to improve service integration between mental health and other services, especially employment, education, family, housing and primary care services. This should build on evidence-based strategies including the establishment of programme standards and technical assistance centres, as well as processes for fidelity assessment and improved service-data monitoring (Monroe-DeVita et al., 2012).
Money, social engagement and employment are the most important challenges identified by people with psychotic illness themselves. Employment has the potential to help address all three challenges for many of these people, to exert a positive impact on physical and mental health, and to improve access to stable housing. Our participants’ assessment of the importance of work resonates with other studies that found that work is an expressed goal for the majority of people with severe mental illness (Westcott et al., 2015) and is associated with better quality of life (Drake et al., 2013; Hopper et al., 2007; Priebe et al., 1998). Meanwhile, poor social circumstances and relative disadvantage experienced by people with psychotic illness render them highly vulnerable to strong social and economic gradients in health, including mental health (Marmot, 2015). Taking an even broader perspective, Jablensky and Sartorius (2008) comment, [T]he erosion of social support systems, likely to be associated with the processes of globalization, should be a matter of grave concern. The sobering experience of high rates of chronic disability and dependency associated with schizophrenia in high income countries, despite access to costly biomedical treatment, suggests that something essential to recovery is missing in the social fabric.
In addition to the burden associated with illness, the cost of these illnesses in Australia is very substantial. The annual cost to society is estimated to be AU$4910 million, and the annual cost to government $3520 million. Over half of the estimated total cost of psychosis (53%) is due to loss of productivity ($2600 million), 28% are health sector and medication costs ($1380 million) and 18% are costs related to spending in other sectors outside of health ($930 million) (Neil et al., 2014a). Meeting some proportion of the challenges, people with psychosis face has the potential to reduce costs to government and society, as well as promote recovery.
Future directions
Happy to participate. After all, research is the key. I also hope that my information for this survey will help to improve services too. (SHIP participants)
The second national survey of psychotic disorders in Australia provided an invaluable opportunity to ask questions at the population-level about contemporary issues related to many aspects of the lives of people with psychotic illness and the services they use. The information gathered is currently helping shape policy for future service provision. However, the landscape is changing rapidly with the roll-out of Primary Health Networks, the National Disability Insurance Scheme and other major shifts across sectors in service provision. SHIP findings are contributing to evidence informing the National Disability Insurance Scheme roll-out and the commissioning of services for people with severe and complex mental illness by the Primary Health Networks. In particular, they emphasise the need for clear referral pathways and high-quality care coordination, both of which Primary Health Networks are required to commission, so as to support people with severe mental illness access, and transition between, appropriate services. However, a third survey in the next 3 years, coming a decade after the last survey, is critical to map the new territory in order to continue to inform government planning for future service provision and models of care for people with a severe mental illness.
Footnotes
Acknowledgements
This publication is based on data collected in the framework of the 2010 Australian National Survey of High Impact Psychosis. The members of the Survey of High Impact Psychosis Study Group are as follows: V Morgan (Project Director); A Jablensky (Chief Scientific Advisor); A Waterreus (Project Coordinator); A Mackinnon (Statistician); R Bush, D Castle, M Cohen, C Galletly, C Harvey, P. McGorry, J McGrath, H Stain (Site Directors); V Carr (Australian Schizophrenia Research Bank); A Neil (Health Economics); B Hocking (SANE Australia); and S Saw (Australian Government Department of Health and Ageing). This report acknowledges, with thanks, the hundreds of mental health professionals who participated in the preparation and conduct of the survey and the many Australians with psychotic disorders who gave their time and whose responses form the basis of this publication.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship and/or publication of this article.
