Abstract

To the Editor
Posterior reversible encephalopathy syndrome (PRES) is a syndrome of transient vasogenic edema over the white matter of cerebral posterior regions (Roth and Ferbert, 2011), and PRES-related psychiatric syndromes have rarely been reported. Here, we report a case of PRES-related delusional infestation.
A 57-year-old female uremic patient without personal or family history of mental illness was admitted to the infectious diseases ward because of sepsis 4 months ago. She experienced altered consciousness, blurred vision, right hemiplegia and aphasia with hypertension. Her brain magnetic resonance imaging (MRI) showed symmetric vasogenic edema involving frontal–parietal–occipital white matter, cerebella, splenium of corpus callosum and right thalamus with compression of the right lateral ventricle. Her symptoms resolved 7 days later, and PRES was diagnosed (Figure 1). She then firmly believed that she was being bitten by ‘winged insects’, and she regarded all pigmentations and nevi as evidence of these insect bites and tried to use nail clippers to remove these ‘insects’, although a dermatologic examination revealed eczema without evidence of any bug bites. Aripiprazole 2.5 mg/day was prescribed in a psychiatric consultation, but she was lost to follow-up after discharge.
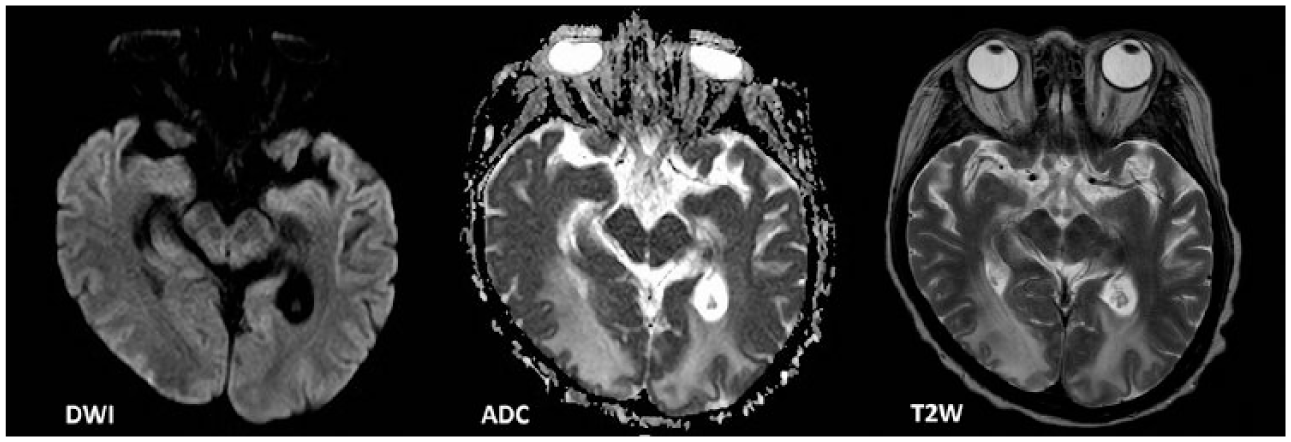
MRI showed symmetric vasogenic edema involving bilateral frontal–parietal–occipital white matter and right thalamus with compression of the right lateral ventricle.
PRES could manifest as visual disturbance, headache, altered mental function and seizures, which usually resolve within a week, and the diagnosis is based on MRI, with vasogenic edema over the white matter of cerebral posterior regions and sometimes cerebellum/brainstem and deep white matters involved (Roth and Ferbert, 2011). This might be the first report of an association between delusional infestation and PRES.
Delusional infestation is a disorder in which patients have firm false beliefs that they are infested with insects against all medical evidence, which can be primary or secondary psychotic disorders. Skin lesions secondary to scratching or self-cleansing are commonly found while patients often try hard to get rid of these ‘insects’ (Freudenmann and Lepping, 2009). The pathophysiology of delusional infestation is still unclear. Several reports of delusional infestations have found abnormalities in the fronto-striato-thalamo-parietal network which may be the cause of delusional infestations as in our case (Freudenmann and Lepping, 2009; Wolf et al., 2014).
In conclusion, we report the first case of PRES with a rare and novel sequelae of delusional infestation. This case should remind clinicians of the importance of an early diagnosis and treatment of PRES to prevent the risk of permanent neurological dysfunction and the possibility of death from cerebral edema.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship and/or publication of this article.
