Abstract
To the Editor
The prevalence of metabolic abnormalities, including elevated waist circumference, hypertension, dyslipidaemia and impaired blood glucose levels, are a critical issue within first-episode psychosis (FEP) (Vancampfort et al., 2013). In 2011, we reported a retrospective, cross-sectional naturalistic study in which the files of FEP patients (n=85) attending the Bondi Early Psychosis Service between 2006 and 2008 were audited (Curtis et al., 2011). Greater than 40% of the sample had an at-risk waist circumference, whilst 12.5% met International Diabetes Federation (IDF) criteria for metabolic syndrome. In total, 55% of males and 42% of females were overweight or obese (Curtis et al., 2011).
During the data collection period (2006–2008), no formalised screening or intervention protocol existed. Pragmatic approaches to counteract the modifiable risk factors began to develop, involving dietetic and exercise physiology students, volunteers and a focus on optimal psychopharmacological prescribing. In addition, the role of metformin to attenuate weight gain was reviewed (Newall et al., 2012). Formal evaluation of this ad hoc intervention was limited by insufficient capacity to offer service-wide implementation. Concurrently, a standardised metabolic monitoring form was developed and adopted as NSW Health statewide policy to improve cardiometabolic screening. Funding was then obtained to evaluate the subsequent formalised intervention – the ‘Keeping the Body In Mind’ (KBIM) program – a 12-week, individualised lifestyle intervention including the establishment of an in-house gymnasium and cooking facilities, with recruitment beginning in March 2013.
Prior to the rollout of the formal KBIM program in 2013, a secondary audit of an independent sample, from the same service, was conducted in 2011. Results from this secondary audit are presented in Table 1. At a median treatment time of 9 months, 53% of males and 22% of females were found to be overweight or obese. Over 50% of females and 39% of males (43% of the total sample) had an increased waist circumference, with a quarter of the sample being hypertensive (females > men; p<0.05). Elevated fasting blood glucose was detected in 15% of the male patients. Approximately a quarter of the sample had raised triglyceride levels (23%) and 29% of the sample had low high-density lipoprotein levels.
Descriptive statistics: demographic and risk factor variables.
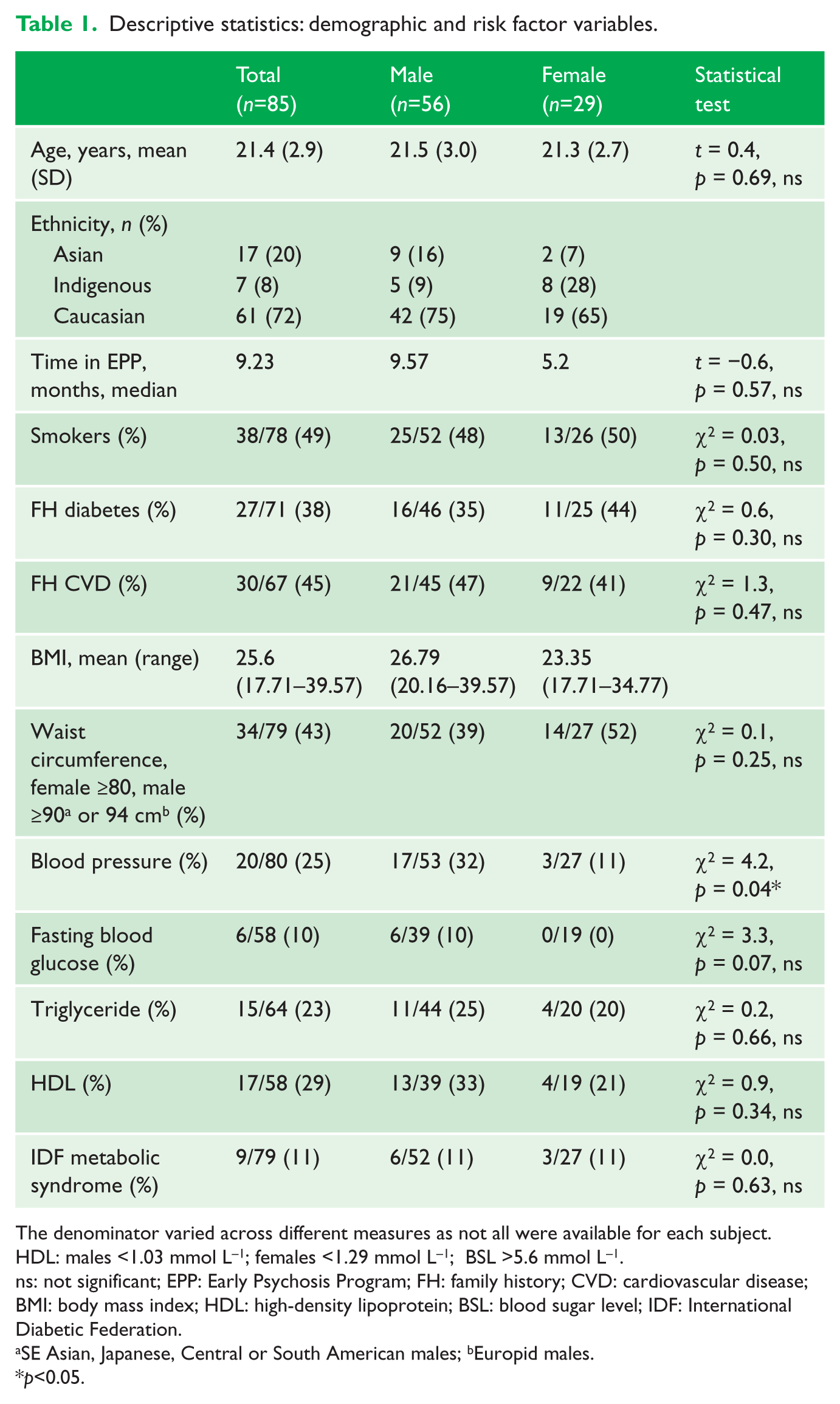
The denominator varied across different measures as not all were available for each subject.
HDL: males <1.03 mmol L−1; females <1.29 mmol L−1; BSL >5.6 mmol L−1.
ns: not significant; EPP: Early Psychosis Program; FH: family history; CVD: cardiovascular disease; BMI: body mass index; HDL: high-density lipoprotein; BSL: blood sugar level; IDF: International Diabetic Federation.
SE Asian, Japanese, Central or South American males; bEuropid males.
p<0.05.
The results confirmed previous findings of the significant rates of cardiometabolic risk in FEP youth. The ongoing KBIM evaluation underpinned by the principles enunciated in the Healthy Active Lives (HeAL; www.iphys.org.au) consensus statement will hopefully demonstrate the potential for sustainable improvements in life expectancy for young people with FEP.
Footnotes
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Declaration of interest
The authors report no no conflict of interest, the authors alone are responsible for the content and writing of this paper.
