Abstract
Objectives:
Residual obstructive sleep apnea (OSA) following adenotonsillectomy (AT) is common in children with obesity. Drug-induced sleep endoscopy (DISE) identifies upper airway obstruction and guides surgery. A gap remains in evaluating multiple DISE-directed treatments. This study evaluates multiple DISE-directed procedure outcomes, obstruction patterns, and BMI in pediatric patients.
Methods:
This single-institution retrospective cohort study included pediatric patients who underwent DISE-directed interventions from 2009 to 2020. Variables included patient characteristics, DISE timing, obstruction patterns, obstructive apnea-hypopnea index (OAHI), and OSA-18 quality-of-life (QOL). Chi-square tests compared patient demographics and comorbidities between single and multiple DISE groups. Unpaired t-tests compared age, OAHI, and OSA-18 scores between single and multiple DISE groups as well as multiple-DISE outcomes for high versus normal BMI groups.
Results:
Of 122 children who underwent DISE, 27 (22%) had multiple DISE-directed procedures. Average age at first DISE for single and multiple DISE patients was 7.25 (SD = 3.93) and 4.99 (SD = 3.63) years, respectively (P < .01). Common obstructions at second DISE involved the epiglottis (N = 20, 74%), adenoid (N = 18, 67%), and inferior turbinates (N = 15, 56%). Multilevel obstruction was identified in 96% (N = 26) of second and 80% (N = 4) of third DISEs. Children with high BMI (versus normal BMI) exhibited shorter intervals between DISEs. Patients who underwent single DISE exhibited significant OAHI improvement (mean 8.48 vs 3.91, P < .05), but this was not significant for multiple DISEs. The OSA-18 score improved significantly in patients with single DISE (mean summed score 61.3 vs 44.6, P < .05).
Conclusions:
Pediatric OSA involves persistent, multilevel obstruction, especially in younger patients with elevated BMI undergoing multiple DISE-directed procedures. These findings support anatomy-guided, patient-specific surgical planning for high-risk groups. While a single DISE-directed intervention can significantly improve OAHI and QOL, repeated procedures may yield diminishing returns, underscoring the need to consider their timing and utility. Early multidisciplinary evaluation and long-term follow-up are essential for managing persistent OSA.
Keywords
Introduction
Obesity is a well-recognized risk factor for obstructive sleep apnea (OSA), with studies demonstrating that children with higher body mass indices (BMIs) are more likely to experience persistent OSA post-adenotonsillectomy (AT).1,2 Children with high BMI often have complex obstructive patterns that require tailored surgical approaches; however, evidence suggests they can still benefit from AT, though potentially less improvement in apnea-hypopnea index (AHI) compared to patients with normal BMI.1,3 -5
In residual OSA after AT in children, drug-induced sleep endoscopy (DISE) is employed to identify various sites of upper airway obstruction to address surgically, often under the same anesthetic. DISE-directed surgical treatment has been associated with significant improvement in both subjective measures of sleep and postoperative obstructive apnea-hypopnea index (OAHI).6 -9 This approach is particularly valuable in pediatric patients who still exhibit symptoms after AT since DISE enables targeted interventions based on precise localization of obstruction and increases surgical success. 10
Although some research has focused on single DISE-directed interventions with largely inconclusive outcomes, 11 there remains a lack of studies evaluating the impact of multiple DISE-directed operative treatments, particularly in children with high BMI. To address this gap, this study aims to investigate the patterns of obstruction observed at various anatomic levels during multiple DISE procedures and assess AHI, OAHI, and quality-of-life (QOL) outcomes after multiple DISE procedures, particularly in children with elevated BMI.
Methods
This retrospective cohort study evaluated pediatric patients (age <18 years) at a quaternary care academic pediatric hospital who underwent DISE with airway intervention procedures from 2009 to 2020. All patients had previously undergone AT. DISE was performed under general anesthesia—typically propofol infusion—with a flexible laryngoscope inserted via the naris and advanced to visualize the entire upper airway to the vocal cords. In many cases, a concurrent direct laryngoscopy and bronchoscopy was also performed, evaluating the upper airway to the carina and bilateral mainstem bronchi. Tracheomalacia was diagnosed if visualized during bronchoscopy. Indications for DISE included OAHI >1.0 events/hour, snoring, pauses, gasps, and/or being a restless sleeper. We collected patient demographics, BMI, comorbidities (eg, Trisomy 21, laryngotracheomalacia, hypotonia, and cerebral palsy), history of prematurity, and DISE findings. Otolaryngology or any provider follow-up periods (ie, time between first DISE and last known appointment) were calculated. Patients with BMI >85th percentile relative to age and sex were grouped into the high BMI category. We also analyzed patients with multiple DISE-directed procedures who had polysomnography (PSG) data such as total AHI and AHI excluding central apnea (ie, OAHI) before and after each DISE. Additionally, we collected OSA-18 QOL survey data, 12 with a total score of 37 to 60 suggesting mild impact, 61 to 80 suggesting moderate impact, and greater than 80 suggesting severe impact. 13 Patients were excluded if they were lost to follow-up after their DISE procedure or if their medical records lacked essential variables such as demographics, comorbidities, or DISE findings.
Statistical analyses were performed in GraphPad Prism 9 (GraphPad Software, La Jolla, CA). Chi-square and Fisher’s exact tests were performed as indicated to compare patient demographics and comorbidities between single and multiple DISE groups as well as obstruction patterns between obese and non-obese groups. Unpaired t-tests were performed to compare age, PSG data, and OSA-18 scores between single and multiple DISE groups as well as durability of multiple DISE-directed procedures for the high versus normal BMI groups. This study was approved by the Vanderbilt University Medical Center Institutional Review Board (IRB #170372).
Results
Patient Characteristics and DISE Timing
Of 231 patients initially identified, 122 patients who underwent DISE met all inclusion criteria (Table 1). The most common comorbidities were laryngo- and/or tracheomalacia (N = 44, 36.1%), hypotonia (N = 33, 27.0%), and Trisomy 21 (N = 29, 23.8%). Of all DISE patients, 95 (77.9%) had a single DISE procedure, 27 (22.1%) had multiple DISE procedures, and 5 (5.3%) underwent a third DISE. Patients who underwent multiple DISE exhibited a higher rate of comorbidities (P < .001). Average age at first DISE for single and multiple DISE patients was 7.25 (SD = 3.93) and 4.99 (SD = 3.63) years, respectively (P < .01). Among patients who underwent multiple DISE, time from first to second DISE was 20.0 (SD = 14.1) months, and mean age at second DISE was 6.31 (SD = 3.51) years. Among patients who underwent a third DISE, time from second to third DISE was 27.8 (SD = 32.7) months, and mean age at third DISE was 9.13 (SD = 4.65) years. The average ENT follow-up period was longer for patients who underwent multiple DISE (89 [SD = 46] months vs 62 [SD = 47] months, P < .01).
Descriptive Statistics of All Patients.
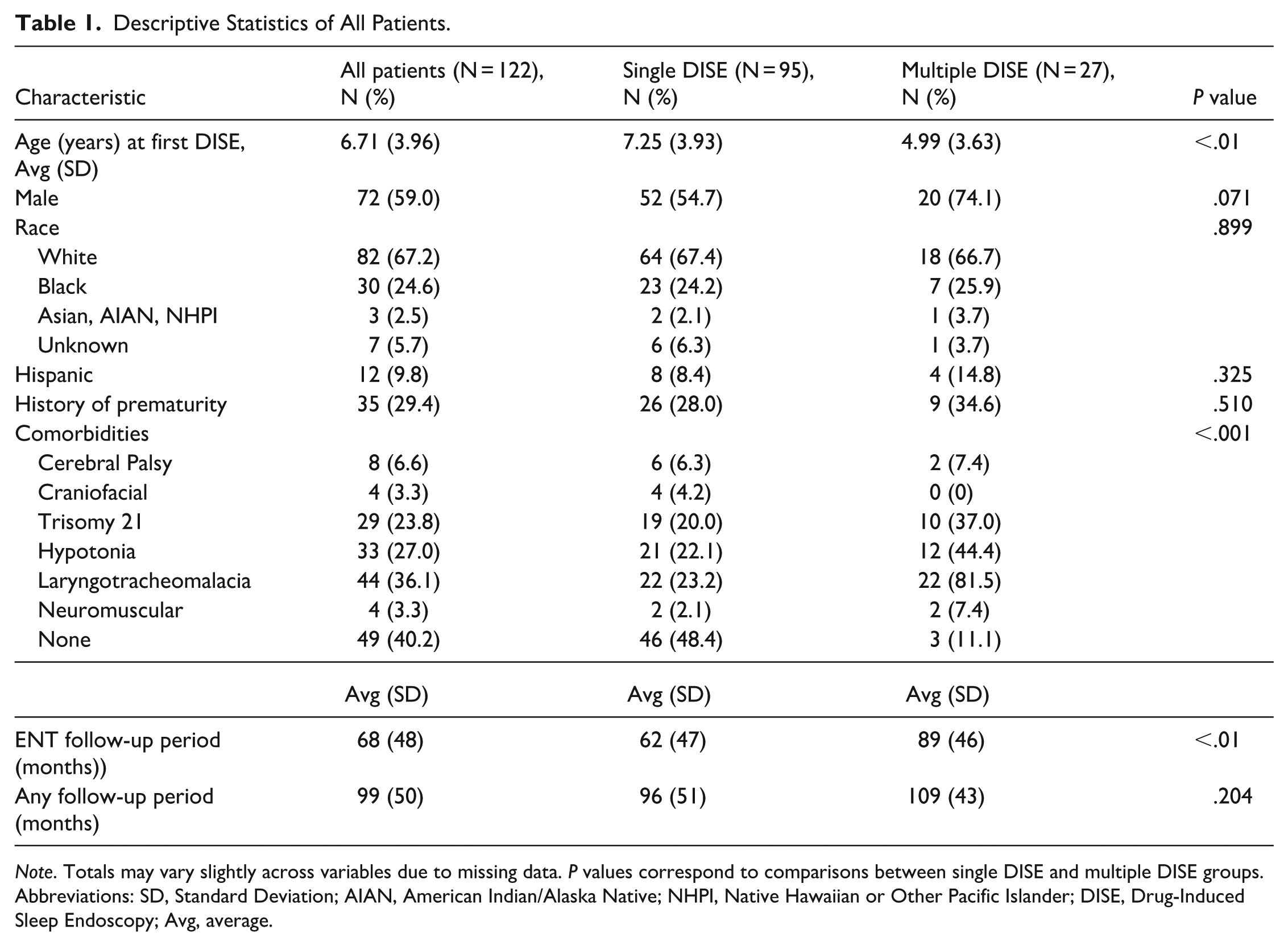
Note. Totals may vary slightly across variables due to missing data. P values correspond to comparisons between single DISE and multiple DISE groups.
Abbreviations: SD, Standard Deviation; AIAN, American Indian/Alaska Native; NHPI, Native Hawaiian or Other Pacific Islander; DISE, Drug-Induced Sleep Endoscopy; Avg, average.
Patterns of Obstruction
The most common locations of obstruction during the first DISE were the adenoid (N = 92, 75%) and inferior turbinates (N = 81, 66%; Table 2). Obstruction during the second DISE occurred most frequently at the epiglottis (N = 20, 74%), followed by the adenoid (N = 18, 67%). Of the 5 patients who underwent a third DISE, obstruction occurred most frequently at the tongue base (80%), followed by the adenoid (40%), epiglottis (40%), inferior turbinates (20%), and arytenoids (20%). Multiple sites of obstruction were found in 93% and 80% of second and third DISE procedures, respectively. Most patients, including children with either high or normal BMI, had at least 2 sites of obstruction (Figure 1).
Sites of Obstruction at First and Second DISE Among Patients with High and Normal BMI.
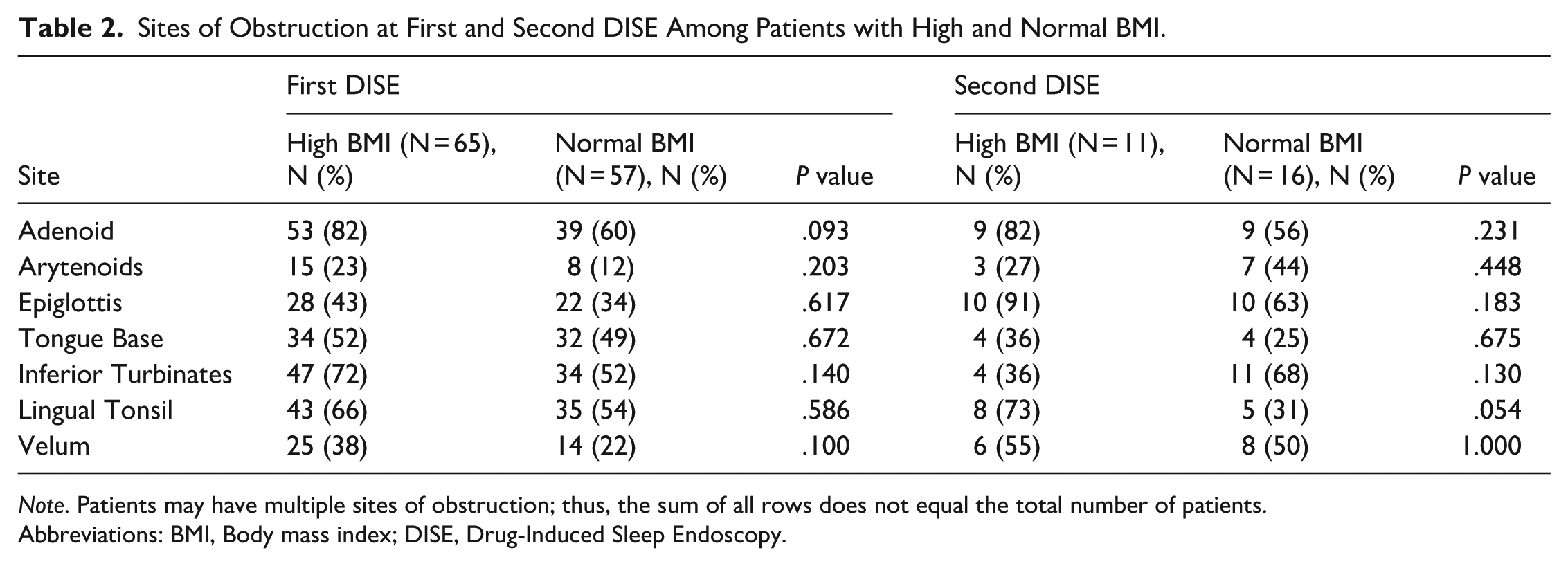
Note. Patients may have multiple sites of obstruction; thus, the sum of all rows does not equal the total number of patients.
Abbreviations: BMI, Body mass index; DISE, Drug-Induced Sleep Endoscopy.
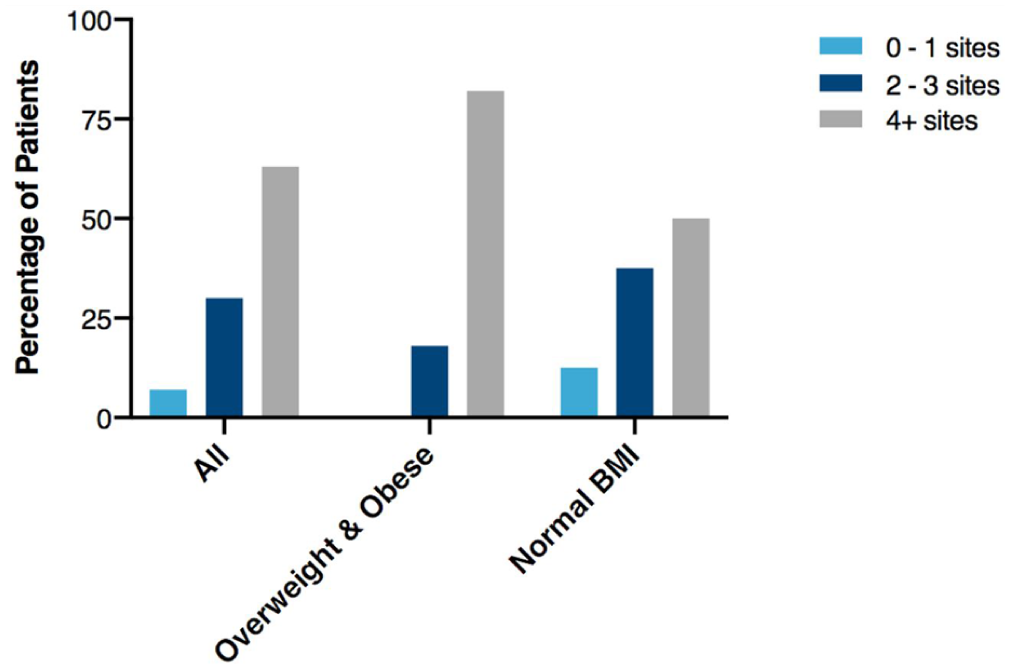
Obstruction patterns during multiple DISE procedures among patients with high and normal BMI.
Role of BMI on Obstruction Pattern and DISE Interval
Compared to patients with normal BMI, patients with high BMI did not exhibit significant differences in obstruction rates by anatomic level on first DISE (Table 2). During the second DISE, there was a non-significant trend toward an obstruction rate difference between children with high and normal BMI at the lingual tonsil (N = 8 [73%] vs N = 5 [31%], P = .054). The interval between DISEs in patients with high BMI versus normal weight was not statistically significant (19.2 ± 16.4 months vs 23.6 ± 19.2 months, P = .570).
Polysomnography and OSA-18 Subset
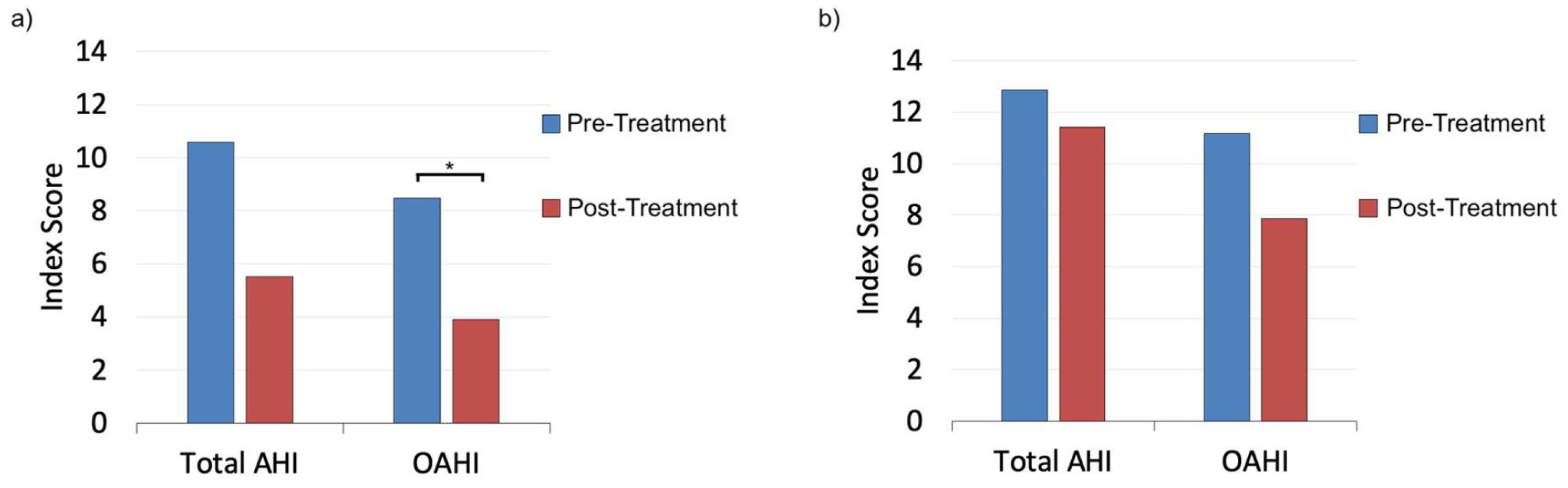
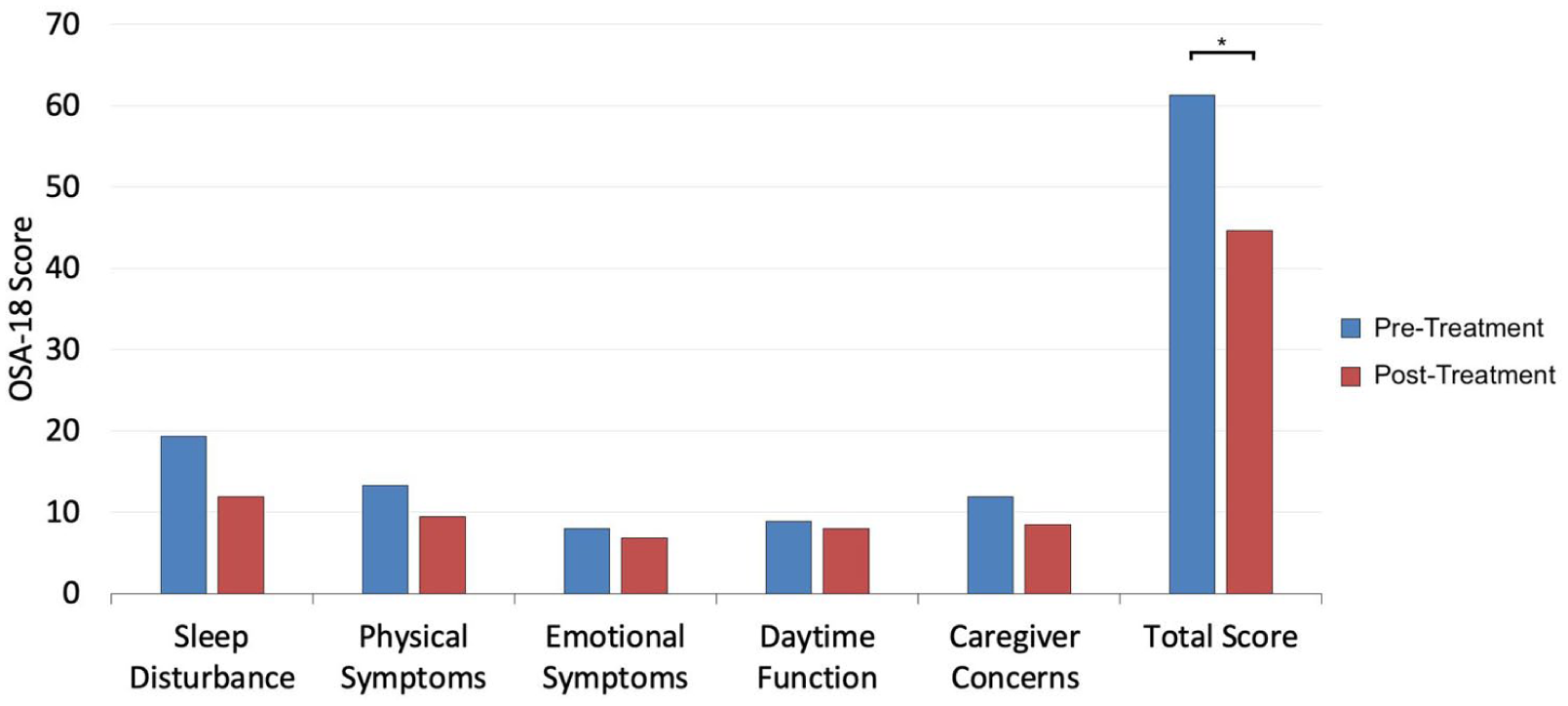
The patient subset with PSG and OSA-18 data included 37 single DISE patients and 23 multiple DISE patients. Improvement in average OAHI was seen in single DISE patients (8.5 vs 3.9 events/hour, P < .05; Figure 2) but not multiple DISE patients (11.2 vs 7.9 events/hour, P = .345). Among single DISE patients, there was a nonsignificant trend toward decreasing total AHI (P = .059). Among the 7 patients with both pre- and post-operative OSA-18 data after a single DISE procedure, the average pre-operative total OSA-18 score decreased significantly after treatment (61.3 vs 44.6, P < .05; Figure 3), signifying a decrease from moderate to mild symptoms. There was also a trend toward lower reported sleep disturbance (P = .050) and caregiver concerns (P = .058). No patients who underwent multiple DISE procedures had both pre- and post-operative OSA-18 data.
Change in OSA-18 quality of life survey scores among patients with a single DISE procedure.
Change in pre-treatment and post-treatment polysomnography data among patients with a (a) single DISE procedure and (b) multiple DISE procedures.
Discussion
This study provides important insights into the patterns of obstruction and surgical outcomes in pediatric patients with residual OSA who underwent multiple drug-induced sleep endoscopy (DISE) procedures. Patients with multiple DISE-directed interventions had their first DISE at a younger age (5 years old) compared to age at single DISE (7.25 years old). Several levels of obstruction were identified among children with multiple DISE-directed procedures such as the epiglottis, adenoid, and inferior turbinates. Children with high BMI exhibited shorter intervals between DISEs compared to children with normal BMI, although this was not statistically significant. We also found that patients who underwent DISE experienced significant symptomatic improvement.
Notably, patients in our cohort who received multiple DISEs received their first DISE at a younger age. Younger children with OSA have increased risk of residual OSA: several studies have shown that age less than 2 to 3 years old is often associated with an increased risk of complications and residual OSA following AT.14 -19 Preoperative OSA severity is a consistent predictor of residual OSA among children less than 3 years old. 16 Anatomical and physiological contributions that may increase risk of residual OSA among younger children include a smaller mandible, 20 narrower airway,21,22 superiorly placed larynx, 23 disproportionately larger tongue,24,25 high chest wall compliance, 23 and unstable ventilatory control. 23 A challenge for treatment involves addressing both the fixed (eg, adenotonsillar hypertrophy) and dynamic abnormalities (eg, airway collapse),25,26 with laryngomalacia being more common in 1- to 3-year-old children.27,28 Sites of obstruction in infants have been found to be retropalatal or retroglossal. 29
Additionally, we found that patients frequently exhibited multiple sites of airway obstruction during their second and third DISE, with the most common locations being epiglottis and adenoid on second DISE and the tongue base on third DISE. Guidelines for treating and documenting obstruction sites during DISE are outlined in the expert consensus statement of the American Academy of Otolaryngology Head and Neck Surgery. 30 Common obstruction sites include the tongue base, adenoid, inferior turbinates, velum, and lateral oropharynx.30 -33 Single DISE findings in a smaller patient population at our institution were previously reported by Wootten et al, 9 which demonstrated frequent multilevel obstruction—particularly at the lingual tonsils, base of tongue, and nasopharynx—and informed our DISE-directed surgical strategies and research question. However, the current study addresses the gap in the literature by detailing obstruction sites found specifically during repeat DISEs. These findings support the importance of site-specific treatment to improve pediatric OSA: for example, obstruction at the tongue base may be improved by lingual tonsillectomy, 34 midline posterior glossectomy, hyoid suspension,35,36 or more novel options such as hypoglossal nerve stimulation. 37
In the current study, patients with higher BMI exhibited multiple sites of obstruction. While some children with normal weight had 0 to 1 sites of obstruction, no patients with high BMI presented with single-site obstruction. Our findings also suggest that patients with higher BMI had shorter intervals between DISE-directed surgeries, although these differences did not reach statistical significance. This finding aligns with previous research indicating that obesity exacerbates the severity and increases the risk of persistent OSA, likely due to the increased upper airway collapsibility and structural abnormalities associated with excess weight.38,39 Pediatric overweight and obese children require close monitoring for OSA, counseling for risk of recalcitrant disease, and tailored treatment approaches.
Patients who underwent a single DISE procedure experienced significant improvement in both OAHI and OSA-18 QOL scores, indicating that a single, well-targeted surgical intervention can improve OSA symptoms. A wide range of potential rescue surgical options exist. 40 An expert consensus statement on the management of pediatric persistent OSA after AT supports the consideration of additional surgical intervention. 41 With success defined as an AHI≤10 events/hour, a meta-analysis showed that phase I (nasal, palate, and tongue surgeries) and phase II (maxillomandibular advancement) procedures fail in more than half of cases. 42 In another study, about 20% of children with Trisomy 21 underwent a second surgery with variable effects on OSA severity, including worse symptoms. 43 Instead of additional surgery, many physicians advocate for treatment with continuous positive airway pressure (CPAP), which has shown some success in managing residual OSA after initial surgery. In some cases, CPAP may be safely discontinued around 1.5 years later. 43 During preparatory discussions for repeat DISE-directed surgeries, patients and their families should be counseled about the risk of persistent OSA and associated symptoms affecting QOL. Future work should aim to assess the utility of repeat DISE-directed surgery since current literature does not answer this question.
Limitations
This study has several limitations. First, this study is limited by its retrospective nature, which may introduce selection bias, restrict the ability to establish causation between variables, and lack information on certain patients since the data were initially collected for patient care rather than a specific research question. As this is a retrospective study, the timing of laryngo- and tracheomalacia diagnosis is not certain; these may have been previously known comorbidities or diagnosed at the time of the DISE. The study was conducted at a single academic institution in pediatric patients, which may limit the generalizability of the results. While the overall sample of 122 patients undergoing single DISE is large for a relatively uncommon procedure, the small sample sizes of second and third DISE patients may limit the ability to detect clinically and statistically significant differences. Additionally, the limited sample sizes in certain subgroup analyses, particularly in Table 2, are underpowered to detect a meaningful difference and should be interpreted with appropriate caution (Supplemental Table 1). Moreover, the OSA-18 is not routinely administered as institutional standard practice due to historically low completion rates. The low number of patients with both pre- and post-operative OSA-18 data after a single DISE procedure as well as the absence of pre- and post-operative OSA-18 data for multiple DISE patients restricts our ability to draw definitive conclusions regarding the long-term effectiveness of DISE-directed surgeries on QOL. A key limitation is the selection bias in postoperative PSG use: persistent clinical symptoms might be more likely to prompt the physician to perform a PSG. Future work is needed to elucidate other factors affecting multiple DISE risks and outcomes.
Conclusion
This study highlights that pediatric patients with residual OSA often present with multilevel obstruction, especially those with high BMI or early age at first DISE. These findings suggest the need for early, individualized surgical planning and long-term surveillance in high-risk populations. The diminishing improvement in objective outcomes after repeated DISE-directed surgeries underscores the limitations of surgical management alone for recalcitrant OSA. Future strategies should prioritize a multidisciplinary approach that integrates personalized surgical, medical, and behavioral interventions, particularly for children with comorbidities and elevated BMI. Additionally, our findings support the need for clearer indications and outcome expectations when considering repeat DISE in pediatric patients.
Supplemental Material
sj-docx-1-aor-10.1177_00034894251381169 – Supplemental material for Multiple Drug-Induced Sleep Endoscopy in Pediatric Obstructive Sleep Apnea: Obstruction Patterns and Outcomes
Supplemental material, sj-docx-1-aor-10.1177_00034894251381169 for Multiple Drug-Induced Sleep Endoscopy in Pediatric Obstructive Sleep Apnea: Obstruction Patterns and Outcomes by Daniel R. S. Habib, Liliana Arida-Moody, Ankita Patro, Jeffanie Wu, Seth Davis, Shilin Zhao, Kalpnaben Patel, Christopher T. Wootten and Amy S. Whigham in Annals of Otology, Rhinology & Laryngology
Footnotes
Author’s Note
Christopher T. Wootten and Amy S. Whigham, MD, MS-HPEd is now affiliated with Vanderbilt University School of Medicine, Nashville, TN, USA.
Ethical Considerations
This study was approved by the Vanderbilt University Medical Center Institutional Review Board (IRB #170372).
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
Data comprise patient information and are thus not available.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
