Abstract
Objective:
Eustachian Tube Balloon Dilation (ETBD) represents an innovative therapeutic approach for chronic Eustachian tube dysfunction (CETD), a common disease in children. Some evidence of a benefit of ETBD in the adults exist in contrast to sparse reports in children. The objective was to analyze short- and long-term outcome of ETBD in children with CETD.
Methods:
A retrospective chart-review was performed in a cohort of 19 children (mean age 13 years, 7-17) who underwent ETBD. The following parameters were analyzed: tubomanometry (R-value), tympanogram, hearing (CPT-AMA, Air-bone gap [ABG]), Eustachian Tube Score (ETS and ETS-7), and Eustachian Tube Disease questionnaire (ETDQ).
Results:
Twenty-four ears were dilated (in 5 patients subsequently after successful first intervention) and grouped as A (17) without and B (7) with additional T-tube insertion. Most children suffered from either chronic otitis media with effusion or chronic perforation (12, 63%), the remainder comprising recurrent otitis media, adhesive otitis media and CETD with barotrauma. Mean duration of symptoms were 7/8.2 years and mean follow-up 13.7/11.1 months. Eighty percent of patients reported a subjective benefit. Accordingly, the R-value, ETS, and ETS-7 were significantly (P < .05) improved. Tympanometry, CPT-AMA and ABG showed a positive trend, but the result was not significant. Tympanic retraction remained largely the same; a spontaneous closure of a chronic tympanic perforation was seen in 1 of 3 cases.
Conclusions:
The high subjective benefit and some significant objective improvement warrants further analysis of ETBD as part of the therapeutic management in pediatric CETD.
Keywords
Introduction
Pressure regulation problems, retraction processes, otitis media with effusion or cholesteatoma represent common pathological conditions of the middle ear in children and can be attributed to a large degree to the impairment of 1 or more of the classic 3 functions of the Eustachian Tube (ET): pressure regulation, protection, and clearance of secretion from either nasopharynx or middle ear. Other factors such as genetics or mucosal gas exchange additionally contribute to the clinical picture. A multitude of measurements for the assessment of ET function exists, with the manometric group being the largest, but without agreement on which tests to use for best evaluation. 1 Not surprisingly, this pathological and functional complexity of the ET leads to the fact that chronic Eustachian Tube Dysfunction (CETD) remains a poorly defined entity in spite of efforts for classification. 2 Classic therapy in most cases consists of adenotomy and/or insertion of grommets. For several years now, Eustachian Tube Balloon Dilation (ETBD) has been propagated as an additional potential therapeutic procedure. The results of ETBD in adults have been published in a number of studies since 2010.3,4 In children only 6 studies exist to our knowledge, all of which report favorable results with regard to a decrease of ear symptoms such as pain or hearing loss and an increase in the ability to perform pressure equalization.5 -10 However, confounding variables have to be mentioned. For instance, 20% of the children in the study by Jenckel received a simultaneous adenotomy and all children had adjunctive procedures in the study by Toivonen.6,10 Additionally, outcome analysis, which has not been agreed upon internationally, includes classic methods such as tympanometry or newly introduced techniques such as tubomanometry, further complicating proper evaluation and comparison. In spite of the difficulties in analyzing ETBD in children, the high incidence of pediatric CETD and the initial reported favorable results of ETBD merit further research of ETBD to improve this condition.
This case-series reports the results of ETBD in children with CETD with the aim of contributing to the evaluation of this novel technique in the treatment plan of children with CETD.
Materials and Methods
Patients
From September 2015 to September 2018, ETBD was performed as a unilateral procedure in 19 children aged between 7 and 17 years (mean 12.9 years, standard deviation 2.6 years). Seven girls and 12 boys were included retrospectively. In 5 of these children the contralateral side was dilated subsequently for a total of 24 ears, as the first procedure was perceived to be beneficial. ETBD only constituted group A (13 children, 17 ears). An additional T-tube was placed in 7 ears in 6 children who formed a distinct group B for analysis.
Tubal dysfunction was assessed by history, otoscopy, pure-tone audiometry, impedance tympanometry, tubomanometry (TMM), the ETS-and ETS-7-score as introduced by Schroder et al 11 and by the Eustachian Tube Dysfunction Questionnaire (ETDQ). 12 A computed tomography scan was obtained preoperatively to rule out bony dehiscence of the carotid artery and anomalies of the ET. ETBD was performed on an outpatient basis under general anesthesia by the use of a balloon catheter (Spiggle & Theis GmbH, Overath, Germany) as described elsewhere. 3 Type and duration of symptoms were noted.
Measurements
All children were investigated 1 week postoperatively clinically and all measurements were repeated 2 months postoperatively and during further follow-up. The follow-up period ranged from 6 to 29 months (mean 13.7) for group A and 6 to 21 months (mean 11.1) for group B. The following parameters were collected preoperatively and after ETBD: subjective improvement, otomicroscopic finding, hearing loss by CPT-AMA and air-bone gap (ABG: average of gaps at 500 Hz, 1 kHz, 2 kHz, and 4 kHz), type of tympanogram, R-value (derived from the tubomanometric measurement, corresponding to the latency of tubal opening and the time of increasing pressure in the nasopharynx and calculated as the average of 2 successive measurements for each pressure level: 30, 40, and 50 mbar), the ETS, the ETS-7 score, and the ETDQ-questionnaire. ETS-, ETS-7 score, and ETDQ are not validated for children, TMM has limited validation in children. 13 However, in the absence of clearly defined outcome measurements, they were included in order to assess outcome in the most comprehensive way and to allow for future comparison. Complications of the procedure were noted.
Statistical Analysis
The Wilcoxon signed-rank test (WSRT) was used to compare pre- and postoperative data. The one-sided test was used because depending on the variable in the data either an increase or a decrease was expected. The tympanogram was assigned the following scores: type A (4 points), slight negative pressure (3 points), type B (1 point) and type C (2 points) (see Gurtler et al 3 for details). As improvement was hypothesized, a shift of the median toward Type A for the postoperative data should be observed. For the R-value of TMM a value of 30 was assigned, if no tubal opening was observed, to prepare R for statistical testing. Details are described in Gurtler et al. 3
Results
In total, 24 ETBD procedures were performed in 19 children: 5 bilateral sequentially, 7 each on the right and left side. Most children (12) including 5 children of group B presented either with chronic otitis media with effusion (6, 31.5%) or chronic perforation (6, 31.5%); the others were categorized as CETD with barotrauma in 3 (15%), adhesive otitis media in 2 (11%), and recurrent otitis media in 2 (11%) (one from each group).
In 16 children—with the exception of the 3 cases with CETD and Barotrauma—conventional therapy with adenotomy and tympanic ventilation tubes had been performed as a first line treatment. There were no syndromic patients.
The following symptoms were reported either alone or in combination: pressure, hearing loss, pain, tinnitus, and difficulties equalizing (Table 1). Vertigo was inquired about, but not indicated by any patient. The duration of symptoms was between 0.75 and 14 years (mean 7 years) for group A and 3 and 12 years (mean 8.2) for group B.
Symptoms and Corresponding Number of Ears Pre- and Postoperatively (Group A, B, and Total).
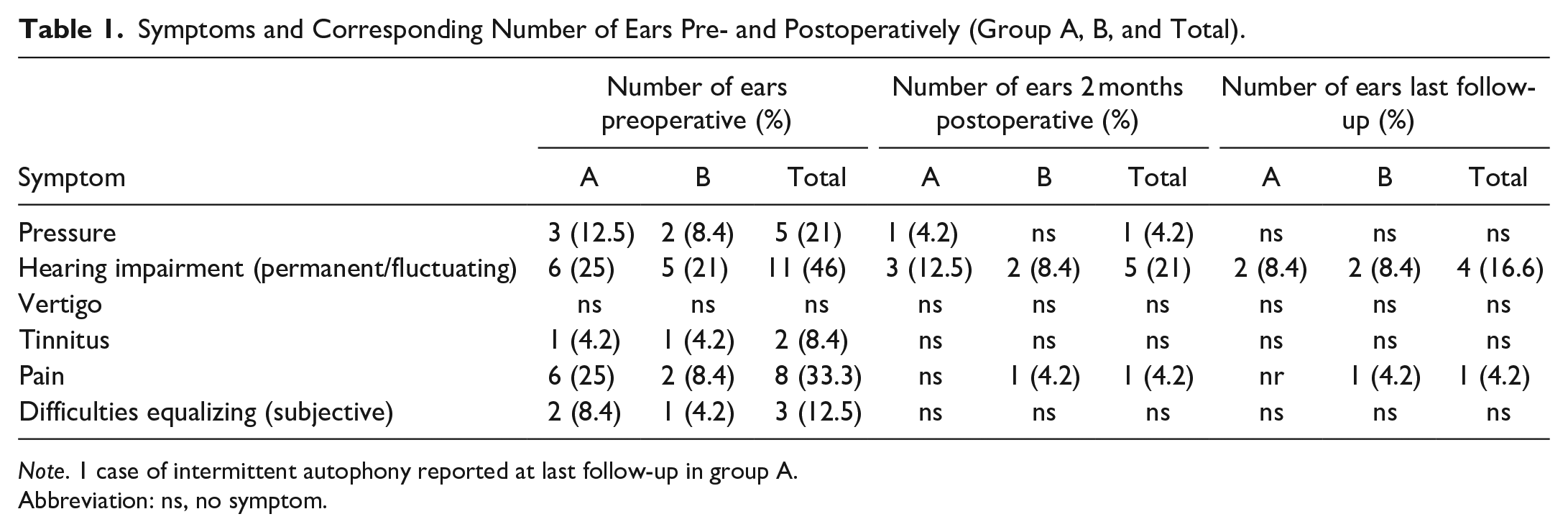
Note. 1 case of intermittent autophony reported at last follow-up in group A.
Abbreviation: ns, no symptom.
Hearing loss was reported in up to 50% of ears followed in frequency by pain and pressure before the intervention as listed in Table 1. A subjective postoperative improvement of various symptoms was perceived by most patients. The frequency of the various reported symptoms declined from 4 to 46% to 4 to 16%. Specifically, hearing impairment (46% to 16.6%) and symptoms related to the ventilation function of the ET, such as pressure (21% to 0%) and pain (33.3% to 4.2%), benefited most from ETBD. However, this also includes the 5 children with chronic otitis media with effusion, who received a T-tube. Equalizing difficulties, reported by 3 children, disappeared completely. A benefit, if present, was usually already seen at 2 months postoperatively. The positive effect of ETBD was stable, especially significant deterioration in the successful cases was not observed over the follow-up period. Pain persisted in 1 patient in the ventilated group (maybe related to myoarthropathy of the temporomandibular articulation) and some degree of hearing impairment in 2 patients of each group.
Episodes of otitis media have not been observed since the intervention in the 2 patients with former recurrent acute otitis media. In 2 patients with chronic otitis media with effusion the T-tube was removed on one side with equally no recurrence over a period of 12 months.
Otomicroscopic finding showed an improvement of tympanic retraction in 1 out of 8 (12.5%) ears and spontaneous closure of a chronic perforation after 2 months in 1 out of 3 (33%) cases.
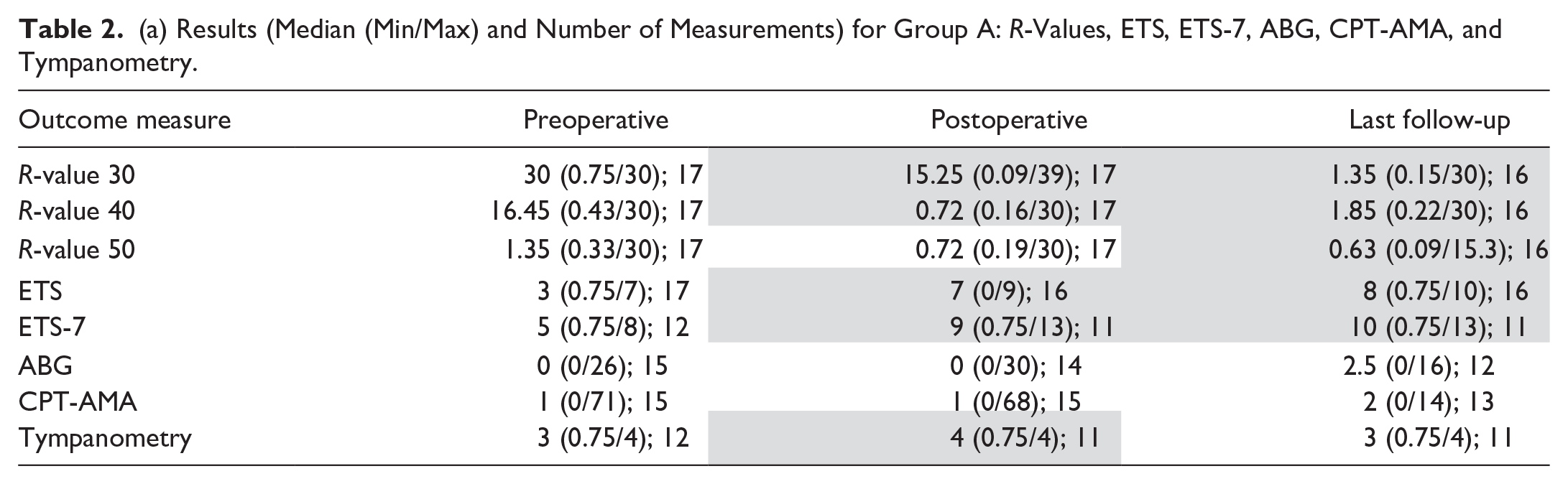
The results of the R-value of TMM, ETS, ETS-7, Tympanometry, and ABG are listed in Table 2.
(a) Results (Median (Min/Max) and Number of Measurements) for Group A: R-Values, ETS, ETS-7, ABG, CPT-AMA, and Tympanometry.
(b) Results (Median (Min/Max) and Number of Measurements) for Group B: R-Values, ETS, ETS-7, ABG, CPT-AMA, and Tympanometry.
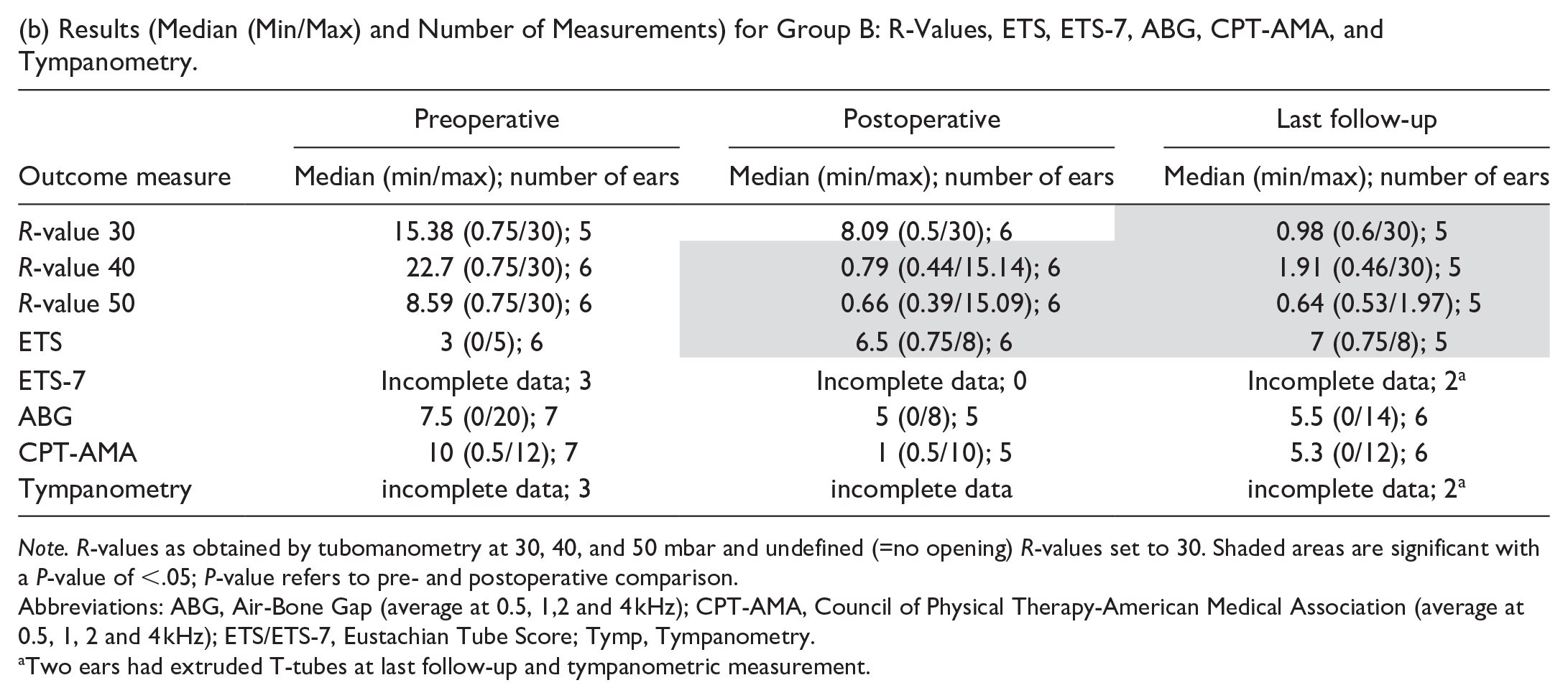
Note. R-values as obtained by tubomanometry at 30, 40, and 50 mbar and undefined (=no opening) R-values set to 30. Shaded areas are significant with a P-value of <.05; P-value refers to pre- and postoperative comparison.
Abbreviations: ABG, Air-Bone Gap (average at 0.5, 1,2 and 4 kHz); CPT-AMA, Council of Physical Therapy-American Medical Association (average at 0.5, 1, 2 and 4 kHz); ETS/ETS-7, Eustachian Tube Score; Tymp, Tympanometry.
Two ears had extruded T-tubes at last follow-up and tympanometric measurement.
There was significantly less failure of tubal openings and a significantly higher number of normal values (Figure 1) resulting in significant improvement of the R-value across most pressure levels (Table 2). Normal R-values (average of 2 measurements, white area in Figure 1) at the last follow-up in comparison to preoperative () were seen in following number of patients: R30 7(1), R40 8(1), R50 10(3) for group A, and R30 3(1), R40 1(1), R50 4(1) for group B.
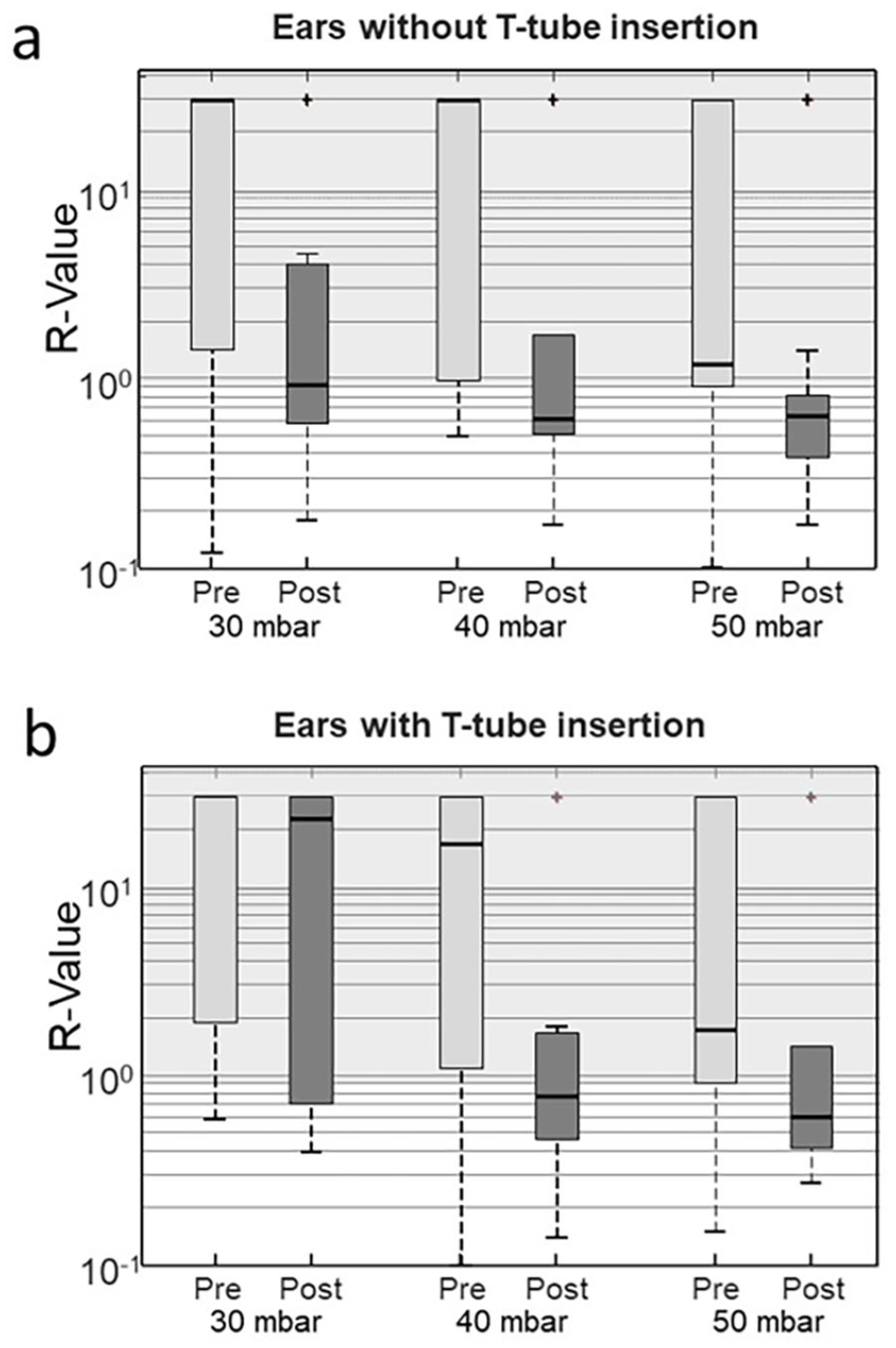
Results of the pre- and postoperative measurements of the R-value at pressure 30, 40, and 50 mbar for group A (a) and group B (b). Two measurements were performed for each patient. In case of no tubal opening, the R-value was set to 30. The white area represents the normal range: R-value between 0 and 1.
For the ETS and ETS-7 (latter incalculable for group B as tympanometry was not measured due to tubes) similar to the reports of subjective symptoms, a significant improvement (P < .005) was observed. Twenty (87%) ears out of 23 measured reached an ETS of more than 5 points (normal) at the final follow-up. Likewise with ETS-7, where a significantly higher figure of points was seen postoperatively.
In the tympanometric measurement of group A, the shift of the median score toward 4 points was significant (P = .0020) only for the first postoperative control, but decreased to 3 at the last follow-up.
While CPT and ABG improved in both groups, the change was not significant. The median indicated that the degree of hearing loss in most patients was not pronounced already preoperatively.
The ETDQ was introduced during the study-period and available for 2 patients in group A preoperatively, 5 patients 2 months postoperatively, and 8 patients at the final follow-up. The respective median values and min/max for the treated side were: 19.5 (14-25), 10.2 (7-15), and 9.75 (7-18).
Following side-effects and complications were noted: rhinitis-like symptoms (Rhinorrhoea, blocked nose) in a few cases. A late sequela—intermittent patulous Eustachian tube—occurred about 9 months after ETBD in 1 patient, but did not require any therapy.
Discussion
CETD continues to persist during childhood in a significant number of children, although exact epidemiologic data is lacking. Children face such potential sequalae as repeated tympanostomy tube placement, conductive hearing loss with resultant developmental delays, or cholesteatoma formation. Therapeutic options for CETD have not changed much during the last decades and mostly focused on relieving symptoms. In contrast, ETBD represents a novel therapeutic approach, which was first reported in children in 2013, with the potential to address the ET itself. 9 It was proposed that ETBD be an option in the treatment plan for CETD to potentially aid in preventing long-term sequelae. In this retrospective study, we focused on the short-and long-term results of balloon dilation surgery with emphasis on a comprehensive functional analysis in a cohort of 19 pediatric patients (24 dilated ears) with CETD of various origins.
Overall subjective improvement was very high and noticed in 19 ears (80%). Specifically, symptoms such as pressure, pain, hearing impairment, and difficulties equalizing were reported to a much lesser degree. The frequency of the various symptoms decreased from 4 to 46% preoperatively to 4 to 16% postoperatively (Table 1). The subjective benefit was in most cases already perceived after 2 months with only slight further improvement over the study-period. The observation of subjective improvement within the first 2 months post treatment was in accordance with previous results published in the literature.6 -8 Information on long-term follow-up was very limited in the available publications. In the study by Leichtle et al 7 only 26% (14 children) of the initial cohort were available at 1-year follow-up. Toivonen reported stable results over a mean follow-up of 2.3 years in 46 children. 10 It remains an open question whether late improvement is related to the procedure or to the natural course of the disease. The mean symptom duration of 7 years in this study group points to a chronic disease with less potential for spontaneous improvement, thus supporting the beneficial effect of ETBD.
The plethora of existing objective outcome measurements for ETBD, often newly developed with limited validation like the questionnaire proposed by Leichtle et al, 7 renders proper objective evaluation and interstudy comparison difficult. 1 In children, the situation regarding proper evaluation is even worse. Despite this fact and in view of the novel method various objective measurements were included in this analysis, albeit ETS/ETS-7, TMM, and ETDQ are not properly validated in children. Both, TMM and ETS/ETS-7, were significantly improved in this group of children. Likewise, Leichtle et al 7 showed a trend toward improvement in TMM, but stated that most children tolerated just 1 measurement. In contrast, Jenckel came to the conclusion that TMM was not a good assessment tool due to the high variability seen in their data. 6 However, the series of 6 measurements performed in this study group renders our statistical analysis much more robust in contrast to the afore-mentioned studies. Additionally, TMM was completed in 17 children and was just partially measurable due to pain in only 2 children. Similarly, Estève in his original work performed TMM in 56 children with otitis media with effusion with and without grommets and did not report any abort due to pain. The R-value he measured was significantly different from the control population group. 14 In this cohort a significant shift of the R-value toward normal values was observed in about half of the patients. ETS, another measurement tool, might represent a helpful assessment tool by combining 5 subjective and objective measures and therefore potentially increasing informative value and validity. The results support stable success in the majority of patients (Table 1). This study is the first one to have included ETS/ETS-7 in the assessment for children. Further data is needed to corroborate its use in the pediatric population.
Objective confirmation of hearing improvement by analyzing ABG and CPT-AMA was not possible. A “small” ABG around 10 to 15 dB HL, as seen in this population, needs a higher number of patients to reach significant sensitivity and specificity. 15 There are 2 publications reporting audiometric outcome. Maier et al 8 showed a decrease of the average threshold value from 18 to 10 dB HL measured in 65 children pre- and in 22 (33%) postoperatively. A similar result was obtained by Toivonen et al 10 : mean 17.5 dB HL preoperatively decreased to 10.8 at 6 months and 5.7 (4.8) at 36 months. However, all children in the latter study had adjunctive procedures such as tympanoplasty among other.
By analogy with ABG, the small number of tympanometric measurements (for 11 ears complete) prohibits sound statistical analysis. Nevertheless, a higher rate toward a normal tympanogram was observed (significant at 2-months follow-up), with slight deterioration at the final follow-up. Similarly, 2 other studies demonstrated an increase of Type A (normal curve), but lacked statistical analysis.7,8 Functional impairment of the ET might not be necessarily related to substantial measurable hearing loss, but improvement as obtained by ETBD might be sufficient to achieve a subjective benefit.
Our data indicates that ETBD seems to improve ET function in a substantial number of children, but normalization is less often achieved. This observation is similar to the one seen in adults. 3 However, with the poor available definition of “normal” ET function, it remains an open question what degree of function is needed for subjective well-being and prevention of sequelae of CETD. ETBD is not expected to release significant adhesive retractions and in our view has limited potential to reduce tympanic non-adhesive retraction, an observation similar to the adult population, although Toivonen et al 10 reported an improvement to Type A in 85%. 3 In contrast, a spontaneous closure of a small chronic perforation was observed in this study.
Limitations of this study include the small number of ears treated and the lack of a proper control-group. Although taking the non-treated side as control is possible—as the children showed bilateral CETD with comparable severity of symptoms for both sides and initially only one side was treated—and analysis showed a favorable outcome for ETBD, the included number of patients renders statistical significance difficult.
While some factors leading to CETD in childhood have been identified and include among others mucosal swelling due to chronic infections, adenoid or muscular insufficiency such as seen in cleft-palate, the exact contribution is not clear. 1
The predominant role of the mucosal tissue has been demonstrated by analysis of a finite element model of the ET function. 16 There is some evidence by histopathologic examination for ETBD to reduce mucosal inflammation by creating a submucosal fibrous scar. 17 With this in mind, ETBD has a major potential to improve the condition of children suffering from CEDT.
Outcome measurements have to be validated and defined internationally to objectively assess ETBD. Additionally, stratification of patients to define groups, who benefit most, and long-term observation remain to be done. Still, the results of this study support further research into ETBD as a therapeutic option for pediatric CDET, especially in view of the few limited surgical methods.
Conclusion
ETBD seems to hold some benefit for children with CETD. It is feasible and safe. The lack of defined outcome measures, which are often poorly validated in the pediatric population, renders analysis and inter-study comparison difficult. However, the available data supports on-going efforts to validate ETBD in children, especially as this method represents a possible “causative” approach.
Footnotes
List of Abbreviations in alphabetical order
ABG: Air-Bone Gap
CETD: Chronic Eustachian Tube Dysfunction
CPT-AMA: Council on Physical Therapy, American Medical Association
ET: Eustachian Tube
ETBD: Eustachian Tube Balloon Dilation
ETDQ: Eustachian Tube Disease questionnaire
ETS and ETS-7: Eustachian Tube Score
TMM: Tubomanometry
Author Contributions
N.G. contributed to the study conception and design. Material preparation, data collection and analysis were performed by both authors. The first draft of the manuscript was written by N.G. and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Consideration
This study was approved by the Institutional Ethics Committee (Ethikkommission Nordwest- und Zentralschweiz, Basel, Switzerland) (approval number 2017-01508). The research was conducted ethically, with all study procedures being performed in accordance with the requirements of the World Medical Association’s Declaration of Helsinki. Written informed consent was obtained from each participant/patient for study participation and data publication
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.