Abstract
Achilles tendon ultrasonography is useful in diagnosing familial hypercholesterolemia, as it allows assessment of its thickening and structure. The association between structural abnormalities in the Achilles tendon and the severity of coronary artery disease (CAD) was investigated in a cross-sectional study. We conducted this study on 353 patients who underwent percutaneous coronary intervention (PCI). Ultrasound was used to examine the thickness and structural abnormalities of the Achilles tendon. Their CAD severity was assessed using the SYNTAX score before the first PCI. Abnormal findings on Achilles tendon ultrasonography were observed in 21 patients (5.9%). The SYNTAX score was compared between patients with and without abnormal Achilles tendon structure. The SYNTAX score was significantly higher in patients who had structural abnormalities but without thickening of the Achilles tendon (P = .002). Multivariate analysis revealed that abnormal Achilles tendon structure was one of the independent risk factors for an elevated SYNTAX score. In patients with CAD who underwent PCI, structural abnormalities in the Achilles tendon identified by ultrasonography were independently associated with an increase in the SYNTAX score.
Introduction
Structural abnormalities or thickening of the Achilles tendon observed on ultrasonography can be attributed to Achilles tendon xanthomas.1–3 Ultrasonographic findings of the Achilles tendon may include localized hypoechoic lesions, diffuse heterogeneous echo patterns, or hyperechoic images owing to calcification and are considered manifestations of familial hypercholesterolemia.2,3 The main components of Achilles tendon xanthomas are lipids (33% of dry weight) and collagen (24% of dry weight), and most xanthoma cells are believed to be of macrophage origin.4,5 Thickening of the Achilles tendon due to xanthoma reflects the cumulative deposition of cholesterol. 6 Notably, radiographs are widely used to diagnose Achilles tendon xanthoma and allow for the evaluation of the degree of Achilles tendon thickening but not its internal properties. 3 Previous studies have reported an association between Achilles tendon thickening detected on radiography and the severity of coronary artery disease (CAD) and prognosis.7–9
With our understanding of the relationship between Achilles tendon ultrasonography results and the severity of CAD, there is the potential to predict the presence of CAD non-invasively and without radiation exposure. Therefore, this study aimed to investigate the association between Achilles tendon ultrasonography results and the severity of CAD.
Methodology
Study Population
This study included patients who underwent percutaneous coronary intervention (PCI) for CAD at Sendai City Medical Center, Sendai Open Hospital, from August 2020 to August 2023. Patients who had multiple PCIs during the study period (subsequent PCIs taken at different times were excluded to avoid duplication of cases), those in whom Achilles tendon ultrasonography could not be performed, those with non-atherosclerotic thrombotic myocardial infarction, those who underwent coronary artery bypass surgery, those in whom testing was not feasible owing to death or severe illness, those with a history of Achilles tendon rupture, and those who had lower limb amputation were excluded. Figure 1 presents a flow diagram of the study participants.
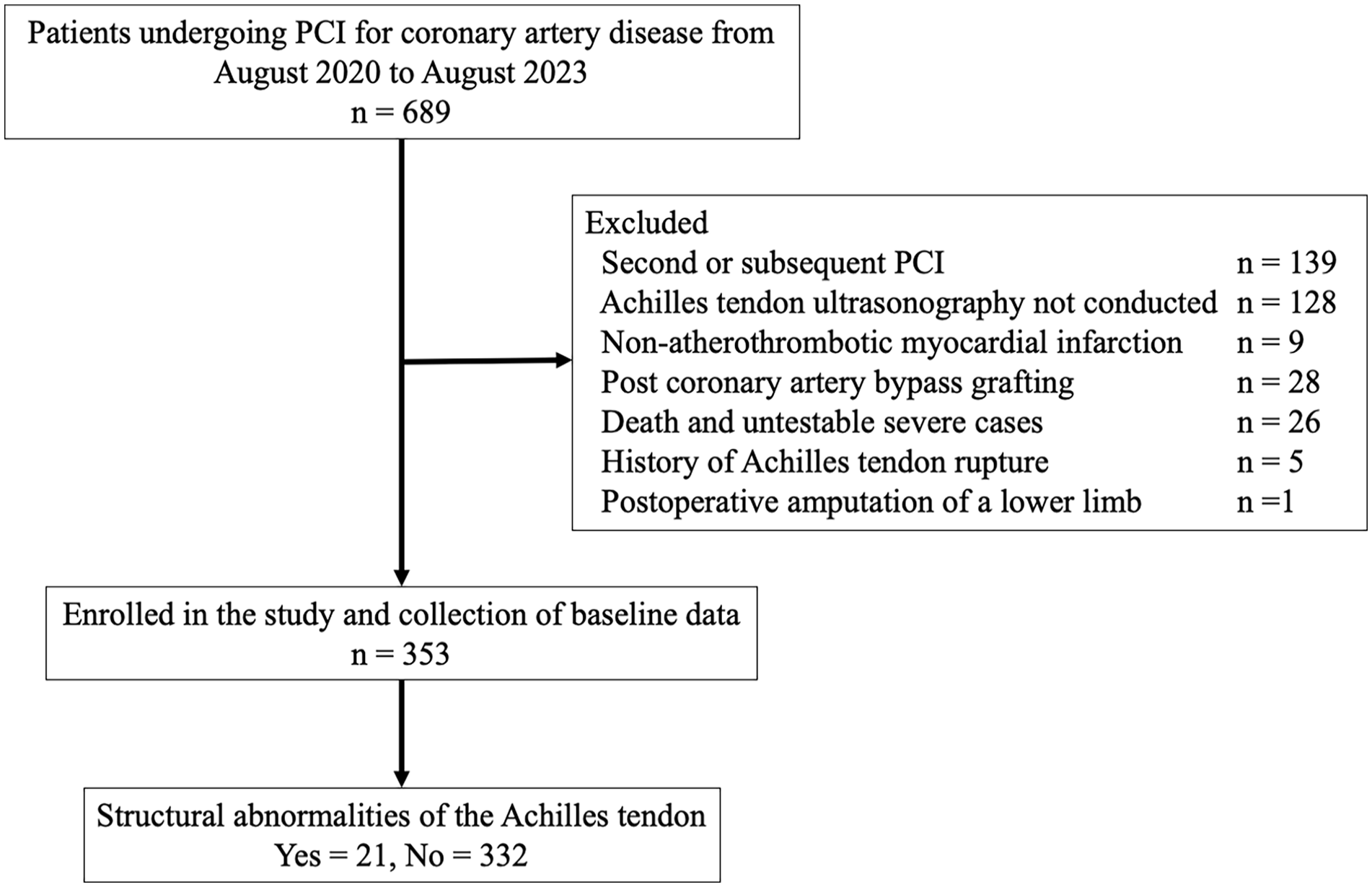
Flow diagram of the study participants.
Protocol
We analyzed various patient characteristics such as age, sex, body mass index (BMI), patient status on admission, and treatment after hospitalization. Diagnoses of hypertension, diabetes mellitus, and dyslipidemia were obtained from the patients’ medical records or patient histories of previous medical therapy. Patients were divided into two groups according to the characteristics of their Achilles tendon.
The study conformed to the principles outlined in the Declaration of Helsinki and was approved by the ethical committee at Sendai City Medical Center (number 2023-0055). All patients provided informed consent in accordance with the method prescribed by the hospital’s ethical committee.
Measurement of Achilles Tendon Characteristics
Ultrasonography was performed on the Achilles tendon to evaluate its thickening and properties. 10 Achilles tendon thickness was measured at the thickest part of the tendon, and the average thicknesses of the left and right Achilles tendons were determined. Abnormal Achilles tendon layer structure, localized hypoechogenicity, and calcification observed using Achilles tendon ultrasonography were defined as abnormal characteristics of the Achilles tendon (Figure 2). Measurements were performed by a skilled ultrasonographer at Sendai Open Hospital. The testing equipment and ultrasound probes included an EPIQ Elite device (Philips Japan, Tokyo, Japan) with a high-frequency linear probe at a central frequency of 12 MHz, a Vivid E90 device (GE Healthcare Japan, Tokyo, Japan) with a high-frequency linear probe at a central frequency of 9 MHz, and an Aplio i700 device (Canon Medical Systems Corporation, Tochigi, Japan) with a high-frequency linear probe at a central frequency of 8.5 MHz. Consistent with a previous study, a cutoff value of 6.0 mm for males and 5.5 mm for females was used to determine the presence of Achilles tendon thickening. 10
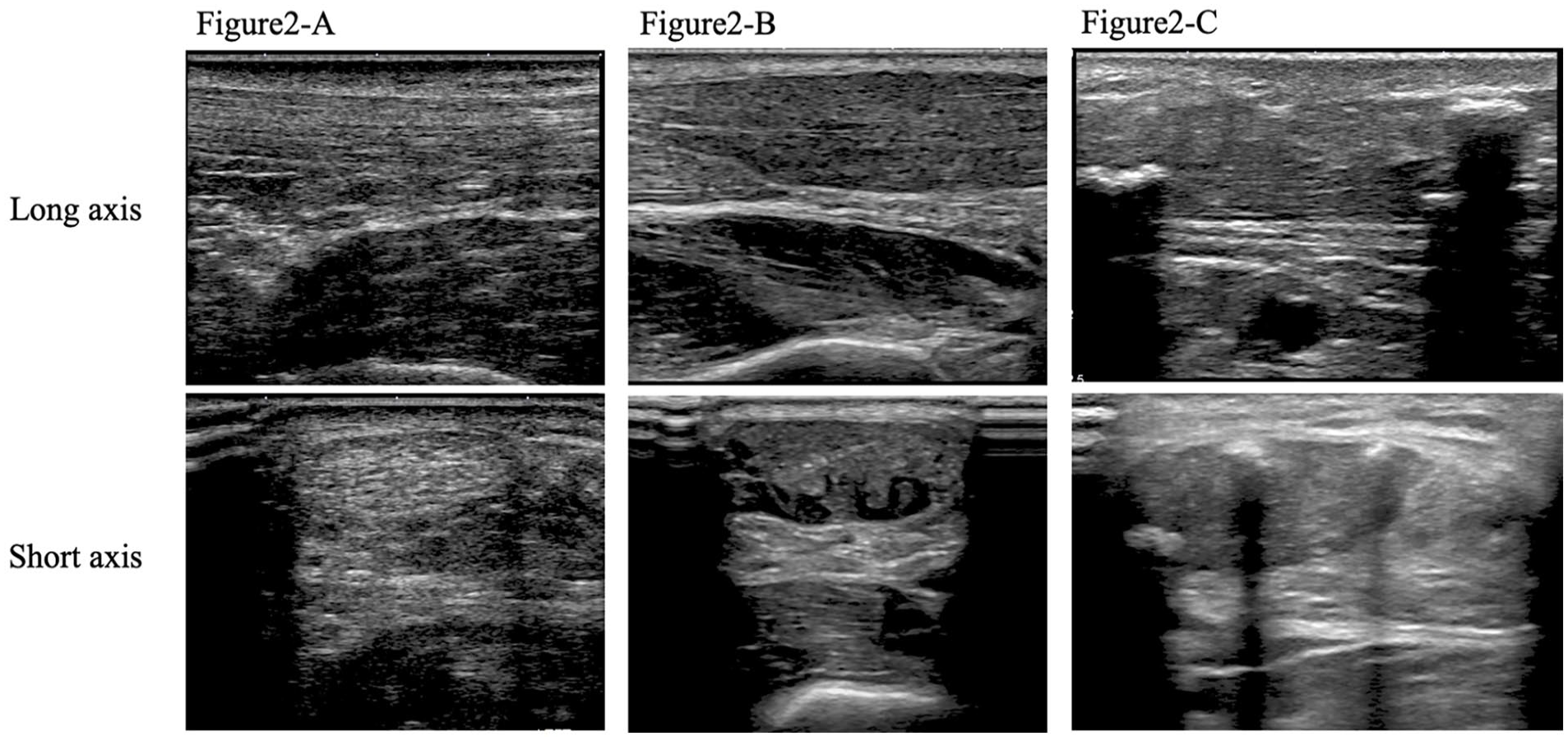
Achilles tendon ultrasonograms. (A) Normal Achilles tendon. (B) Thickening, abnormal layer structure, and localized hypoechogenicity. (C) Calcification.
Evaluation of CAD Severity
Patients undergoing PCI were divided into two groups: a stable CAD group (stable angina, asymptomatic myocardial ischemia, and ischemic heart disease) and an acute coronary syndrome (ACS) group (ST-elevation myocardial infarction, non-ST-elevation myocardial infarction, and unstable angina). The SYNTAX score determines the severity of stable CAD based on coronary artery stenosis, anatomical features, lesions, and lesion status. 11 Furthermore, in this study, we followed previous research and used the SYNTAX score to assess the severity of CAD in patients with ACS. 12 Coronary angiographic images obtained before the first PCI during the study period were evaluated by an experienced cardiologist using the SYNTAX score calculator (https://syntaxscore.org) separately from other laboratory findings.
Statistical Analyses
Continuous data are presented as median and interquartile range and were compared using the Mann-Whitney U test. Categorical variables are presented as numbers and percentages and were compared using Fisher’s exact test. The Spearman’s correlation coefficient was used to determine the relationships between continuous variables. To evaluate the independent determinants of a high SYNTAX score, multiple regression models were constructed, which included age, BMI, glycated hemoglobin (HbA1c), low-density lipoprotein cholesterol (LDL-C), male sex, smoking status, and structural abnormalities of the Achilles tendon (assessed by ultrasonography) as independent variables. Additionally, bootstrap analysis was performed to validate the model internally. Statistical significance level was set at P < .05, and all statistical analyses were performed using EZR version 1.61 (Saitama Medical Center, Jichi Medical University, Saitama, Japan), a graphical user interface for R version 4.3.1 (The R Foundation for Statistical Computing, Vienna, Austria). Multiple regression analyses and the bootstrap method were conducted specifically using R. EZR is a modified version of the R commander designed to add statistical functions frequently used in biostatistics. 13 The missing covariates were left ventricular ejection fraction (n = 6; 1.7%), blood sugar (n = 5; 1.4%), radiographic Achilles tendon thickness (n = 4; 1.1%), HbA1c (n = 3; 0.8%), LDL-C (n = 2; 0.6%), high-density lipoprotein cholesterol (HDL-C; n = 2; 0.5%), total cholesterol (n = 1; 0.3%), and triglyceride levels (n = 1; 0.3%).
Results
During the study period, 689 consecutive patients underwent PCI, of whom 336 were excluded (multiple PCIs, n = 139; Achilles tendon ultrasonography could not be performed, n = 128; non-atherosclerotic thrombotic myocardial infarction, n = 9; post-coronary artery bypass surgery, n = 28; testing could not be performed because of severe illness or death, n = 26; with a history of Achilles tendon rupture, n = 5; lower limb amputation, n = 1). Therefore, 353 patients were included in the analysis (Figure 1). The clinical characteristics of the patients are presented in Table 1. As described in the Methods, the study population was first divided into two groups based on clinical presentation at the time of PCI: the ACS group and the stable CAD group. Subsequently, to investigate the association between Achilles tendon findings and CAD severity, the patients were also divided into two groups according to the presence or absence of abnormal Achilles tendon structures (n = 21 vs n = 332, respectively), and their clinical characteristics are shown in Table 2.
Baseline Characteristics of the Patients Included in This Study.
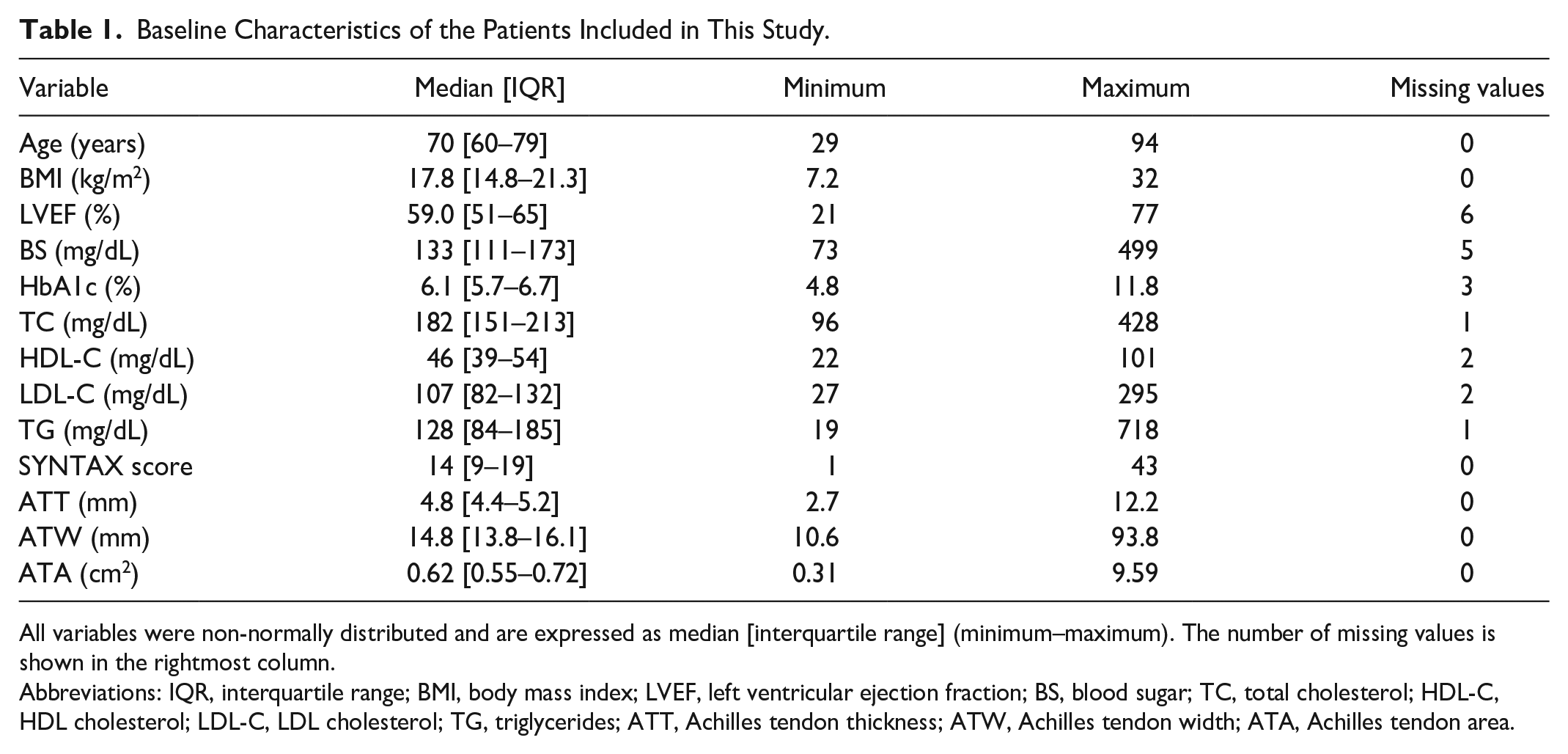
All variables were non-normally distributed and are expressed as median [interquartile range] (minimum–maximum). The number of missing values is shown in the rightmost column.
Abbreviations: IQR, interquartile range; BMI, body mass index; LVEF, left ventricular ejection fraction; BS, blood sugar; TC, total cholesterol; HDL-C, HDL cholesterol; LDL-C, LDL cholesterol; TG, triglycerides; ATT, Achilles tendon thickness; ATW, Achilles tendon width; ATA, Achilles tendon area.
Patient Characteristics Grouped According to the Presence or Absence of Abnormal Findings in the Achilles Tendon.
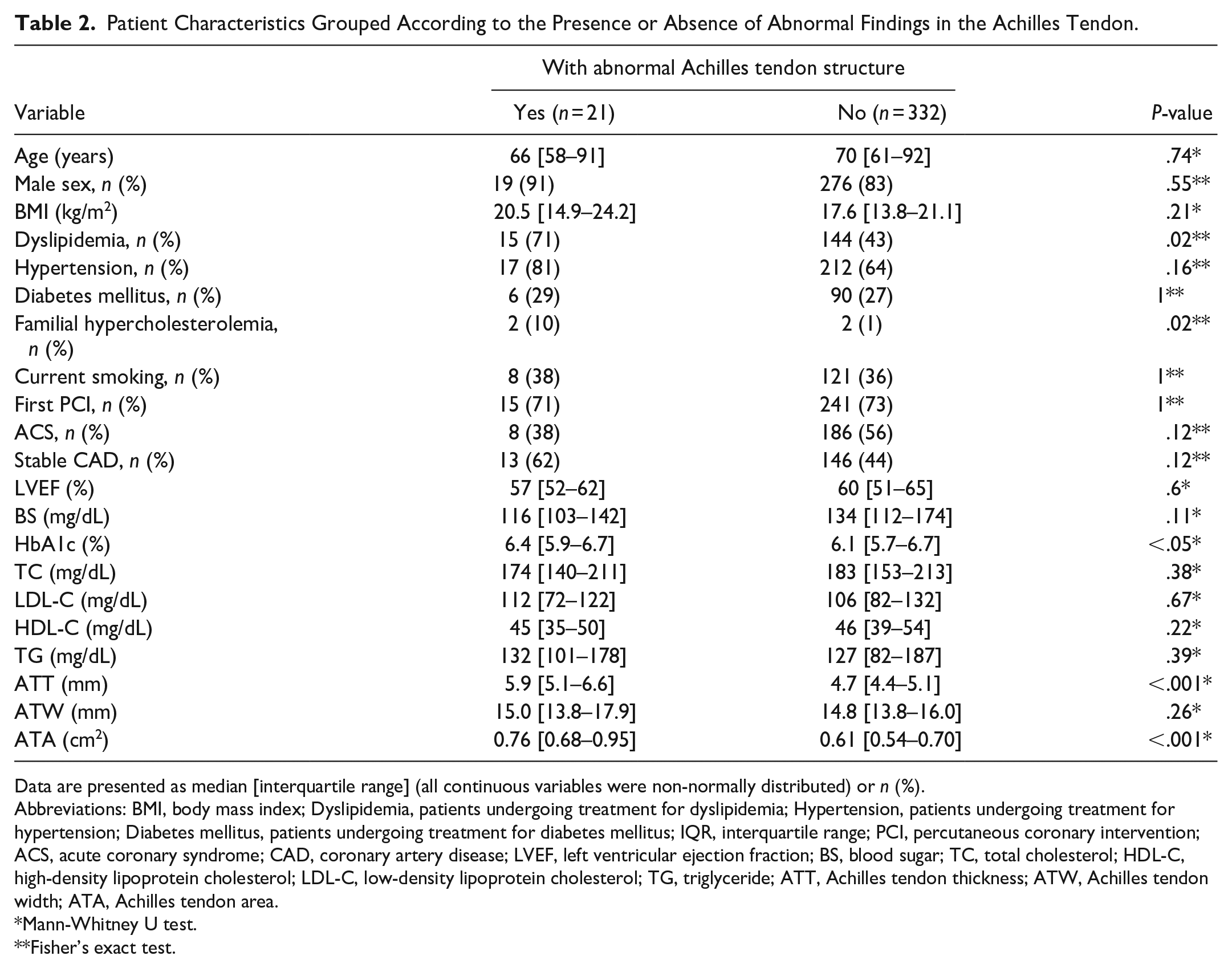
Data are presented as median [interquartile range] (all continuous variables were non-normally distributed) or n (%).
Abbreviations: BMI, body mass index; Dyslipidemia, patients undergoing treatment for dyslipidemia; Hypertension, patients undergoing treatment for hypertension; Diabetes mellitus, patients undergoing treatment for diabetes mellitus; IQR, interquartile range; PCI, percutaneous coronary intervention; ACS, acute coronary syndrome; CAD, coronary artery disease; LVEF, left ventricular ejection fraction; BS, blood sugar; TC, total cholesterol; HDL-C, high-density lipoprotein cholesterol; LDL-C, low-density lipoprotein cholesterol; TG, triglyceride; ATT, Achilles tendon thickness; ATW, Achilles tendon width; ATA, Achilles tendon area.
Mann-Whitney U test.
Fisher’s exact test.
Comparison of the SYNTAX Score and Achilles Tendon Thickness Measured by Ultrasonography
The relationship between the SYNTAX score and Achilles tendon thickness measured by ultrasonography is presented in Figure 3. The Spearman correlation coefficient between the two variables was statistically significant, albeit weak (r = .167; P = .02).
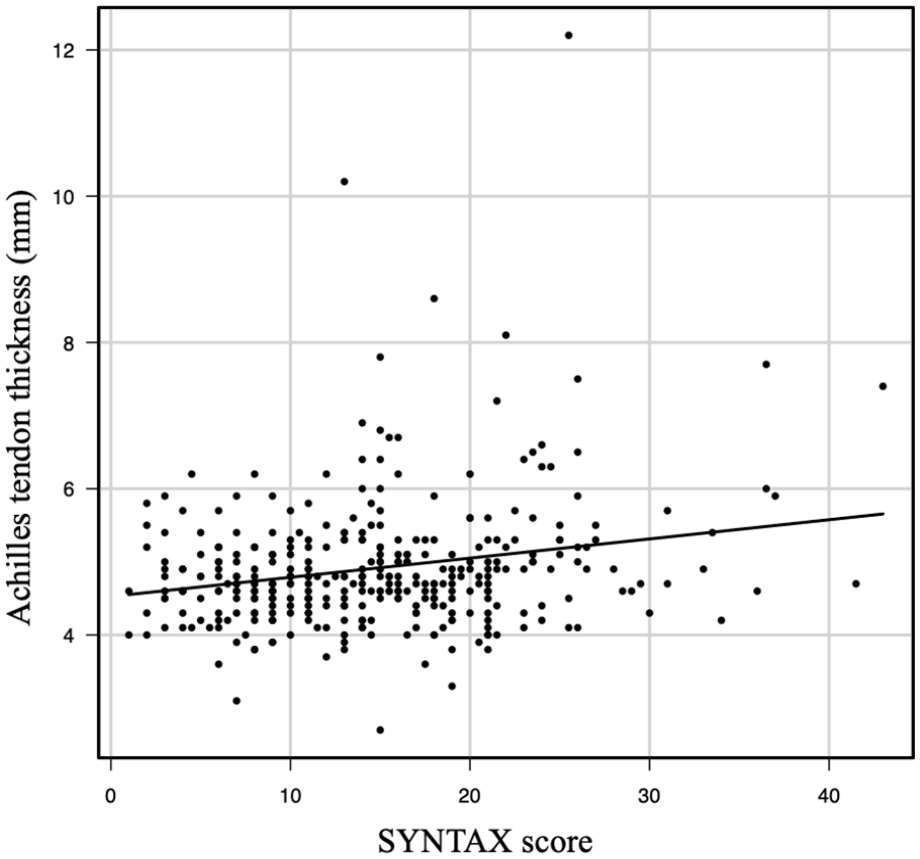
Association between the SYNTAX score levels and the Achilles tendon thickness (r = .167; P = .02).
Comparison of the SYNTAX Score and Presence of Abnormal Achilles Tendon Structures
The Mann-Whitney U test was used to investigate whether there was a difference in the SYNTAX score between the groups with and without structural abnormalities of the Achilles tendon. The SYNTAX score for the group with structural abnormalities of the Achilles tendon was significantly higher than that for the group of without abnormalities in all the cases that we investigated (P < .001). Furthermore, the SYNTAX score was significantly higher in the group with abnormal Achilles tendon structure in both ACS (P = .03) and stable CAD (P < .001) cases. Furthermore, we examined the relationship between the presence or absence of abnormal findings on Achilles tendon ultrasonography and SYNTAX score in a group with Achilles tendon thickness <6.0 mm in men and <5.5 mm in women who were considered to have no Achilles tendon thickening in a previous study. 7 The SYNTAX score was significantly higher in the group with abnormal findings, but there was no thickening of the Achilles tendon (P = .002; Figure 4 and Table S1).
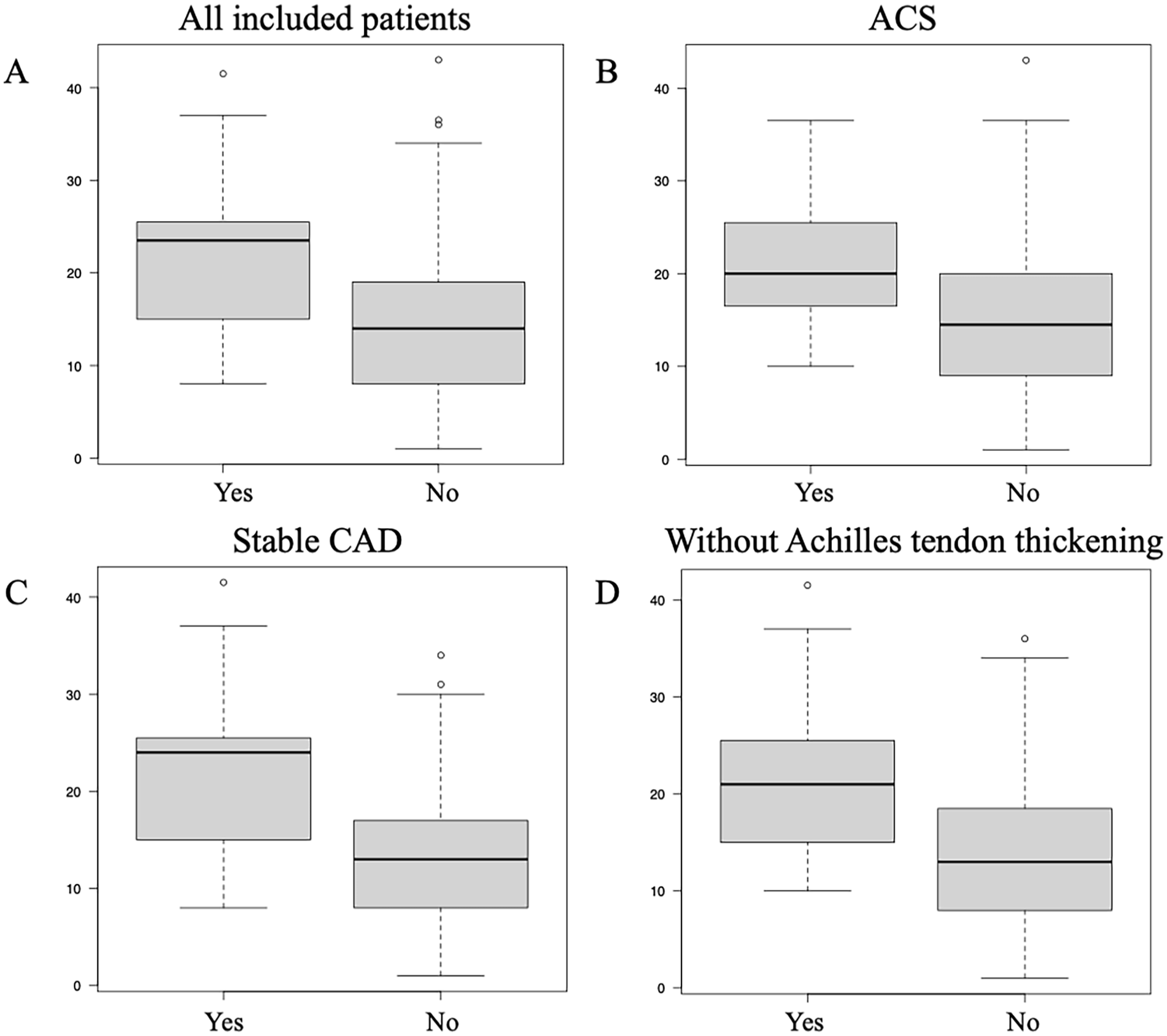
Box plots of the groups with and without abnormal Achilles tendon structural findings in all included patients (P < .001) (A), those with ACS (P = .03) (B), those with stable CAD cases (P < .001) (C), and those without Achilles tendon thickening (P = .002) (D).
Comparison of Age, BMI, HbA1c, LDL-C, Male Sex, Smoking, Structural Abnormalities of the Achilles Tendon, and the SYNTAX Score
HbA1c values, LDL-C levels, and smoking were included in the multivariate analysis as independent variables because they are well-established coronary risk factors that may influence the SYNTAX score. Age, BMI, and the presence of structural abnormalities in the Achilles tendon were also included in the model. In the multiple regression analysis, age (P < .01), LDL-C level (P = .003), and structural abnormalities of the Achilles tendon (P < .001) were statistically significant predictors of the SYNTAX score. The adjusted R2 value was .1009 (Table 3). The variance inflation factor for each independent variable was <5.0. Furthermore, internal validation via the bootstrap method confirmed the statistical significance of age, LDL-C levels, and the presence of structural abnormalities in the Achilles tendon as predictors of an elevated SYNTAX score (Table 3).
Results of the Multiple Regression Analysis of the SYNTAX Score (n = 353).
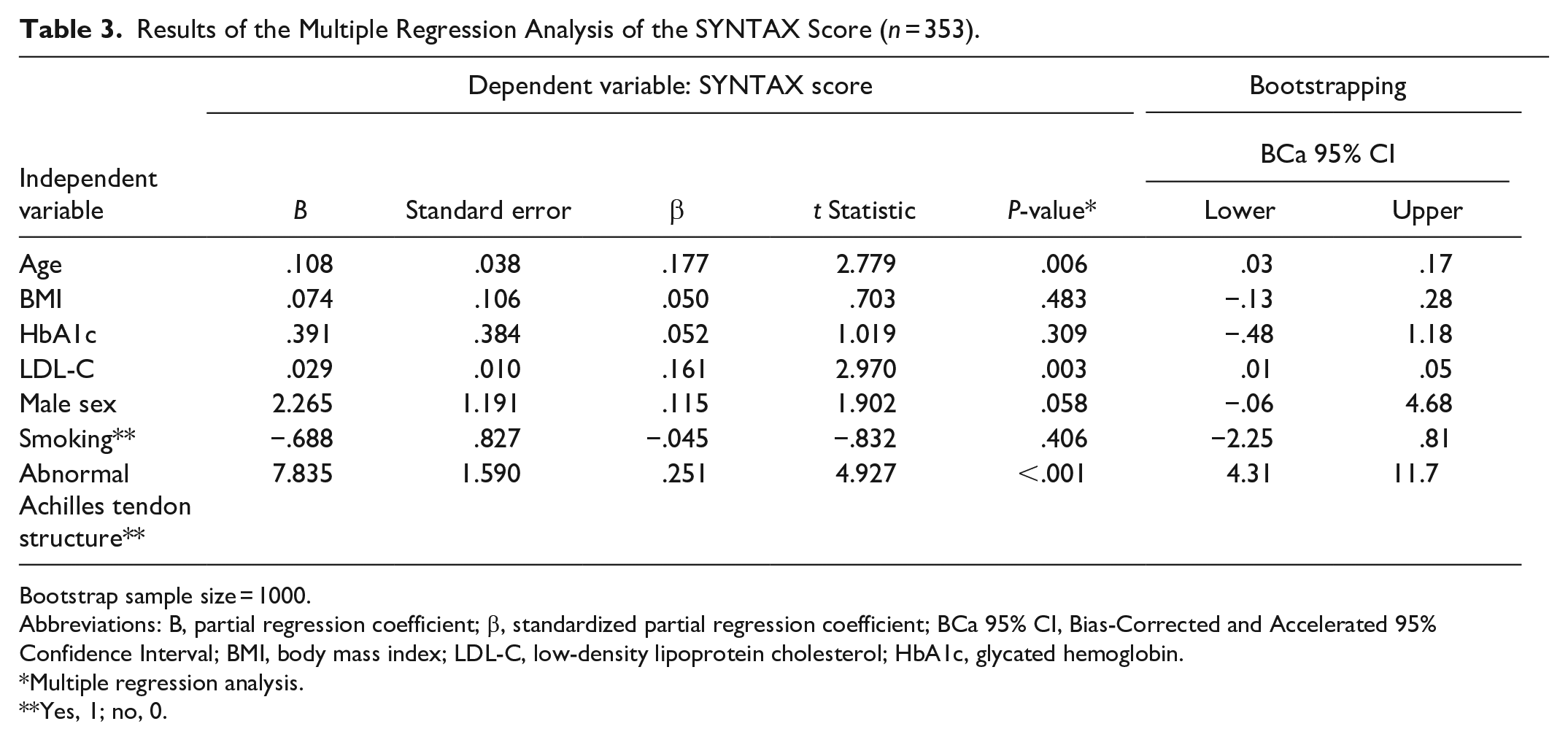
Bootstrap sample size = 1000.
Abbreviations: B, partial regression coefficient; β, standardized partial regression coefficient; BCa 95% CI, Bias-Corrected and Accelerated 95% Confidence Interval; BMI, body mass index; LDL-C, low-density lipoprotein cholesterol; HbA1c, glycated hemoglobin.
Multiple regression analysis.
Yes, 1; no, 0.
Discussion
This study showed that the SYNTAX score was significantly higher in the group with abnormal findings on Achilles tendon ultrasonography than in the group without abnormal findings, whether in the ACS cases, stable CAD cases, or both groups combined. In addition, multivariate analysis showed that age, LDL-C level, and abnormal ultrasonographic findings of the Achilles tendon were significantly associated with higher SYNTAX scores. Therefore, abnormal ultrasonographic findings of the Achilles tendon may be independent predictors of elevated SYNTAX scores. Although the pathophysiological relationship between tendon xanthomas and atherosclerosis remains unclear, it has been suggested that both comprise collagen and foam cells and are associated with LDL-C levels. Moreover, the presence of xanthomas has been linked to an increased risk of cardiovascular disease, suggesting a potential similarity in the pathophysiology of both conditions, consistent with previous findings. 14
Although previous studies have suggested an association between Achilles tendon thickening on radiographic examination and the severity of CAD and prognosis,7–9,15 the correlation between Achilles tendon thickening on Achilles tendon ultrasonography and the severity of SYNTAX score in this study was weak. It has been suggested that Achilles tendon thickness is positively correlated with the product of serum cholesterol level and age 16 and reflects the cumulative deposition of cholesterol, 6 which may be influenced by aging and the LDL-C to which the patient was exposed during that time. However, statin administration has been demonstrated to decrease the Achilles tendon thickness due to Achilles tendon xanthoma. 17 In the present study, 157 of the 353 enrolled patients (44%) were already receiving statin therapy, including 14 of the 21 cases (67%) with structural abnormalities of the Achilles tendon. Therefore, it is possible that the history of statin treatment may have influenced the study results.
Furthermore, even in cases without Achilles tendon thickening, structural abnormalities in the Achilles tendon were observed, and an analysis was conducted within this subgroup, and those with structural abnormalities on ultrasonography had significantly higher SYNTAX scores. Detecting thickening of the Achilles tendon due to xanthoma is considered useful in diagnosing familial hypercholesterolemia. In accordance with previous literature, cutoff values of 6.0 mm for men and 5.5 mm for women were used in this study. 10 These cutoff values were consistent with those reported in previous studies in the United States, which ranged from 5.3 to 5.7 mm for men and from 4.8 to 4.9 mm for women 1 This suggests that these cutoff values can be generalized. Achilles tendon thickening has been suggested to be associated with the severity of CAD.7,18 In recent years, many patients have received statin therapy for dyslipidemia, which may have reduced the Achilles tendon thickening. Consequently, the risk of CAD may have been underestimated. CAD should be considered when Achilles tendon ultrasonography reveals structural abnormalities in the Achilles tendon, even in patients without Achilles tendon thickening.
This study has some limitations. The first was the sample size; the number of patients with abnormal Achilles tendon ultrasonographic findings was relatively small. Second, a genetic diagnosis of familial hypercholesterolemia was not made; therefore, it was not possible to assess the extent to which familial hypercholesterolemia affected the results of this study. Third, patients who underwent coronary artery bypass grafting for severe CAD were excluded due to the inability to evaluate their SYNTAX score. Lastly, the exclusion of cases involving death or severe illness may have introduced survival bias, potentially overestimating the results. A prospective study with a larger sample size is required to further investigate the association between Achilles tendon structural abnormalities and CAD.
Conclusion
In patients undergoing PCI, the presence of abnormal Achilles tendon findings on ultrasonography was independently associated with the severity of CAD. The detection of structural abnormalities of the Achilles tendon using ultrasonography may be useful in identifying patients with high-risk CAD.
Supplemental Material
sj-docx-1-ang-10.1177_00033197251326624 – Supplemental material for Structural Abnormalities of the Achilles Tendon are Associated With Coronary Artery Disease Even Without Achilles Tendon Thickening
Supplemental material, sj-docx-1-ang-10.1177_00033197251326624 for Structural Abnormalities of the Achilles Tendon are Associated With Coronary Artery Disease Even Without Achilles Tendon Thickening by Atsushi Tanita, Shinichiro Sunamura, Masahiro Suzuki, Tsuyoshi Ogata, Kazuki Noda, Toru Takii, Yoshio Nitta, Seijiro Yoshida and Shigeto Namiuchi in Angiology
Footnotes
Acknowledgements
We acknowledge the cooperation of all the echo technicians at Sendai Open Hospital.
Authors’ Note
Author Contributions
All authors contributed to: (1) substantial contributions to conception and design, or acquisition of data, or analysis and interpretation of data, (2) drafting the article or revising it critically for important intellectual content, and (3) final approval of the version to be published.
Data Availability
The data generated and/or analyzed during this study will be shared upon reasonable request to the corresponding author.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Considerations
The study conformed to the principles outlined in the Declaration of Helsinki and was approved by the ethical committee at Sendai City Medical Center (number 2023-0055).
Consent to Participate
All patients provided informed consent in accordance with the method prescribed by the hospital’s ethical committee.
Consent for Publication
Not applicable.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
