Abstract
Background
Mentorship is widely recognized as a critical element of surgical residency training and careers. As more general surgery residency programs look to implement program-wide mentorship interventions, best practices for fostering effective, enduring mentoring relationships remain poorly described.
Methods
Current general surgery residents at an academic medical center participated in individual semi-structured interviews exploring perspectives on mentorship. Interviews were transcribed and de-identified prior to thematic coding using Dedoose.
Results
There were 20 participants (8 interns, 7 mid-level residents, and 5 chief residents; representing 36% of the residency program), with a median age of 30 years and 50% of the cohort identifying as women. Four major themes emerged: (1) mentorship needs evolve throughout training, with an early emphasis on identifying research projects and later shifting toward career development; (2) mentorship needs are often met through multiple mentors including near peers and faculty who fulfill diverse roles; (3) informal relationships are perceived to be more meaningful than formal assignments but require residents to actively seek mentorship; and (4) responsiveness and investment are considered essential qualities of effective mentors.
Discussion
General surgery residents may benefit from programs which help facilitate the formation of mentorship teams comprised of both formal and informal relationships to meet the dynamic needs of residency. Near peer mentors may be particularly valuable in the composition of mentorship teams. Future work is needed to identify effective strategies for supporting residents through major transitions and cultivating behaviors that empower trainees to form the informal mentor-mentee relationships that best meet their needs.
• Mentorship in general surgery residency is perceived as being particularly effective when provided by a team of both faculty and near peer mentors that respond to the mentee’s diverse and evolving needs throughout different stages of training. • Informal mentorship relationships are perceived as more meaningful than those arising from formal assignment but require greater initiative from mentees.Key Takeaway
Introduction
Mentorship is a cornerstone of surgical training, with a range of benefits for residents and faculty including improved career satisfaction, increased academic scholarship, and reduced burnout.1-6 Despite its recognized importance, substantial variability remains in self-reported rates of meaningful mentorship among general surgery residents in the United States (US). 1 Furthermore, only a small minority of surgery departments provide formal training for mentors or mentees. 6 With nearly half of US general surgery residents meeting criteria for burnout, there is an urgent need to better understand how to connect trainees with effective mentors and foster sustainable mentorship relationships.7,8
Although prior studies have reported on the benefits of mentorship in surgical residency and described the implementation of formalized programs at individual institutions, less is known about how residents’ perspectives and mentorship needs evolve throughout training.1,3,6,8-10 The current literature provides limited insight into the dynamic nature of mentorship as trainees in general surgery residency programs navigate their journey through the roles of intern, mid-level resident, and chief resident. Using a qualitative approach, the present study seeks to provide a nuanced exploration of how mentorship needs change through various stages of surgical residency and to identify traits that characterize excellent mentors irrespective of the mentee’s phase of training. Findings from this study will serve to guide mentor-mentee relationships and inform programmatic improvements to better facilitate adaptive and sustainable mentorship models in surgical residency.
Methods
This study was deemed exempt by the University of California, Los Angeles Institutional Review Board. A trained interviewer performed individual semi-structured interviews with general surgery residents at an academic medical center in the beginning of the academic year; this individual was trained in standard qualitative interview methodologies, such as open-ended questioning, active listening, probing for depth, and pacing. The interviewer was neither surgical faculty nor surgical resident, deliberately selected to minimize bias and promote exploratory conversations without the assumption of shared understanding. Eligible participants were recruited via email from three training levels: First-year, mid-level, and chief residents. Informed consent was obtained from all participants.
Interviews explored perspectives on mentorship in general surgery residency training, with prompts encouraging discussion of topics such as components of effective mentorship and forms of mentorship that participants felt were lacking in their training experience. Interview recordings were transcribed verbatim and de-identified prior to analysis. Interviews were continued until thematic saturation was reached, and responses were analyzed via inductive reasoning by individual team members.11,12 The research team then convened to review interview data using conventional content analysis, developing consensus codes to represent thematic elements pertaining to mentorship in general surgery residency. 13 Data analysis was organized using Dedoose version 10.0.35 (Sociocultural Research Consultants, LLC, Manhattan Beach, CA).
Results
Representing approximately 36% of the residency program, a total of 20 residents participated, including eight from the intern cohort, seven from the mid-level resident cohort, and five from the chief resident cohort. The median age of the cohort was 30 years (range: 25-37), and ten participants (50%) identified as women. Four major themes emerged from analysis of interview data.
Mentorship needs evolve throughout training, with an early emphasis on identifying research projects during residency and later shifting toward career development.
Representative Quotations Illustrating Theme 1: Evolving Mentorship Needs

Caption. Mentorship needs evolve throughout training, with an early emphasis on identifying research projects during residency and later shifting toward career development (n = 18, 90% of participants).
During the mid-level and research years, mentorship needs shift toward academic productivity, fellowship preparation, and personal growth. One resident reflected, “In the beginning, my goal for a mentor was: What do I do during my research years, and how do I be the most productive through those years? Following research years, it’s: How do I apply to fellowship, and how can I be the most successful applicant that I can be?” These ideas were echoed by another who shared, “As I progress through residency, I’ve found that the questions I have are becoming geared more towards longer-term career planning […] What should I be doing to set myself up so I can get into fellowship and eventually get a job?” One participant expanded, “During research, I feel [mentorship] is a lot more of how to define your passions both in your career and outside of your career and strategically pursue those.”
Mentorship in the later stages of residency was described as focused on long-term career development and leadership. To that end, one participant explained, “Being a chief resident and having matched, the role of my mentors is now career development […] How do I advance to associate professor? How do I get the key federal grant money to continue my lab? How do you hire people and build a division around you to make for a successful practice?” As another chief resident shared, “I wanted more perspective as a junior resident, and I think I want more nuance as a senior resident.”
Mentorship needs are often met through multiple mentors, including near peers and faculty who fulfill diverse roles
Representative Quotations Illustrating Theme 2: Multiple Mentors

Caption. Mentorship needs are often met through multiple mentors, including near peers and faculty who fulfill diverse roles (n = 15, 75% of participants).
Informal relationships are perceived to be more meaningful than formal assignments but require residents to actively seek mentorship.
Representative Quotations Illustrating Theme 3: Informal Mentorship Relationships

Caption. Informal relationships are perceived to be more meaningful than formal assignments but require residents to actively seek mentorship (n = 15, 75% of participants).
Responsiveness and investment are considered essential qualities of effective mentors.
Representative Quotations Illustrating Theme 4: Responsiveness and Investment

Caption. Responsiveness and investment are considered essential qualities of effective mentors (n = 18, 90% of participants).
Additional Themes. Psychological Safety, Values-Alignment, and Persistence
Three less prevalent, albeit noteworthy, themes emerged from interviews. Several participants spoke to the value of psychological safety in the mentorship relationship, noting that learning and growth in surgical training are especially effective when the mentor establishes an accepting environment. In addition, participants emphasized the importance of values-alignment with a mentor beyond clinical and academic pursuits, particularly for those contending with matters of work-life integration or navigating parenthood in surgical training. Participants also described the need for mentees to demonstrate initiative and persistence when attempting to initiate a mentorship relationship, understanding that successive attempts to reach out to multiple prospective mentors may be necessary before a connection is established.
Discussion
This qualitative study utilized semi-structured interviews to explore perspectives on mentorship among general surgery residents at an academic medical center. Four themes emerged from interviews: (1) Mentorship needs evolve throughout training; (2) needs are often met through multiple mentors fulfilling diverse roles; (3) informal relationships are perceived as more meaningful but require greater initiative; and (4) responsiveness and investment are critical for effective mentorship. Collectively, these themes characterize effective mentorship in surgical residency as a dynamic ecosystem which adapts to trainees’ evolving needs in both professional and personal contexts.
Participants described distinct patterns of evolution for mentorship needs throughout residency training (Table 1). Early residency was characterized as a period during which reassurance and guidance on foundational skills are especially meaningful. Faced with steep learning curves early in surgical training, residents described experiencing “so much self-doubt” and appreciating “mentors that gave the ‘glass half-full’ perspective.” These findings align with prior research highlighting the importance of reassurance and emotional support from mentors.1,9,14 Given their relative approachability, near peers may be particularly valuable mentors for providing both clinical advice and emotional support (Table 2).15,16 One participant described senior-to-junior resident mentorship as more personal because “they’re in the trenches together,” allowing for questions mentees might feel uncomfortable discussing with faculty members. These observations align with the principles of situated learning theory, which describes how learning occurs especially effectively through social interaction; this theory moreover emphasizes how shared experiences help to facilitate skill and identity acquisition. 17
As residents progress to their mid-level and chief years, needs begin to shift towards optimizing scholarly productivity, career development, and alignment with personal identity (Table 1). At this stage, the scope of the mentorship team expands to include individuals able to guide scholarly inquiry, subspecialty exploration, and integration of professional and personal growth. Reinforcing a team-based approach to mentorship, residents emphasized the importance of connecting not only with mentors who offer day-to-day guidance but with those who understand “the bigger picture” of what the mentee hopes to achieve in their career, an attribute of effective surgical mentors described in prior literature (Table 2). 2
Importantly, residents acknowledged that the degree to which various mentorship team members are involved may vary alongside the mentee’s evolving goals (Tables 1, and 2). As clinical, academic, and personal trajectories grow more defined, certain mentors may naturally assume more central roles; however, participants highlighted the value of maintaining relationships with mentors whose roles become more peripheral. Notably, some participants described faculty outside of their intended subspecialty as among their most impactful mentors, suggesting mentor selection need not be restricted to clinical or research interests.
The present study also underscores the tension between the value of informal mentorship and the challenges of establishing such relationships during general surgery residency (Tables 3, and 4). Although requiring greater initiative from mentees, participants considered informal mentorship to be more meaningful than formal assignment; such relationships have been described as more likely to be personal with positive implications for career development and balancing personal obligations. 18 Participants’ emphasis on responsiveness and investment is also consistent with prior literature showing surgical trainees who meet more frequently with their mentors are more likely to feel those individuals are interested in their development.5,10,14 Together, these findings raise the question of how surgical residency programs can best facilitate the development of mentorship teams with informal relationships when time is a critical yet limited resource.
One potential strategy described by participants involves identifying a primary “quarterback” mentor who develops a holistic understanding of the mentee’s goals, provides broad oversight throughout training, and facilitates connections with mentors best suited to address their specific needs (Figure 1, Table 2). While participants did not converge on a single most appropriate identity for a “quarterback” mentor, chief residents and faculty in program leadership were often referenced as being well-positioned for such a role. Irrespective of their specific identity, effective “quarterbacks” were characterized by their understanding of the mentee’s overall goals and trajectory, humility in recognizing the limits of their own expertise, and willingness to leverage professional relationships to connect the mentee with other mentors more appropriate for their specific needs. Such a semi-formal mentorship program would strive to balance the benefits of informal relationships with the practical need for structured advising. Nevertheless, some residents may find it more challenging than their peers to develop informal relationships.
16
Future research should characterize attributes that facilitate formation of informal relationships and identify strategies to empower trainees who struggle with this process, thereby informing programmatic efforts to promote sustainable mentorship; ultimately, building effective mentorship relationships is critical not only during residency training but throughout a surgical career.6,9,14,19 Depiction of a hypothetical mentorship network for a surgical resident throughout their training experience. The blue circle represents the mentee, while the orange circle represents the “quarterback” (Q.B.) mentor. Orange dashed arrows depict connections facilitated by the quarterback on behalf of the mentee; blue solid arrows depict relationships developed directly by the mentee. Colored circles represent individual mentors of varying domains and expertise. Over time, quarterback-facilitated connections mature into the mentee’s own sustained relationships. While not depicted, mentors within the network may also serve as connectors.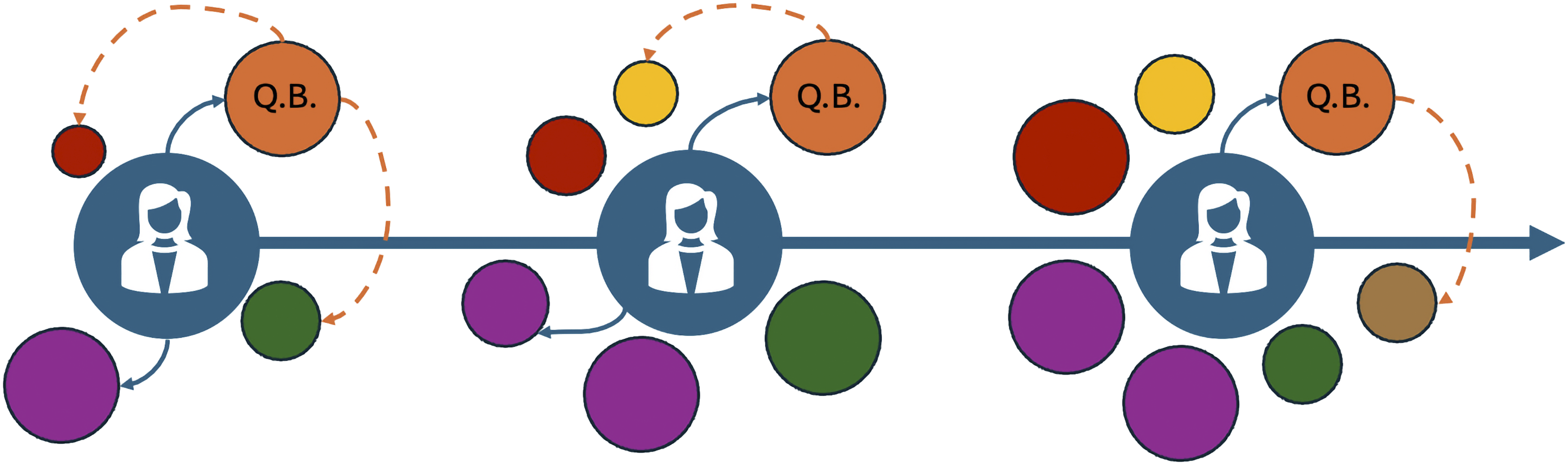
Limitations include those inherent to qualitative research designs. Although unable to establish the effectiveness of any specific mentorship framework, this hypothesis-generating study creates opportunity for future research assessing the impact of semi-formal mentorship programs on measurable outcomes including resident satisfaction or research productivity. While recruitment from a single academic general surgery residency program may limit generalizability to other specialties, institutional contexts, or geographic regions, the described themes remain valid for the examined cohort. As with all qualitative research, readers are encouraged to consider the relevance of the uncovered themes for their population or setting of interest.12,20
This qualitative study illustrates how trainees at an academic general surgery residency program perceive effective mentorship as a multifaceted, dynamic ecosystem of near peer and faculty mentors, shaped by and responding to individual mentees’ evolving needs in both professional and personal contexts. Programs may wish to consider semi-formal mentorship models which facilitate informal relationships while providing structured oversight for anticipated needs throughout residency training. One such model proposed by participants in this study would feature an assigned primary mentor who serves as a holistic longitudinal advisor and connects mentees with a diverse network of mentors to address their specific needs. Although a single universal model would be antithetical to the inherently personalized nature of mentorship, the present study offers theoretical constructs for developing learner-centered programs that can be tailored to institution and program-specific contexts. In addition to exploring the feasibility and effectiveness of new mentorship programs, future work should seek to identify opportunities to empower residents who struggle to form informal mentorship relationships. Future research should also investigate how mentorship themes compare across residency programs in different settings, including community-based and rural programs, to determine whether the themes elicited in this study are broadly generalizable or reflective specifically of the trainee experience in academic environments. These efforts are critical for fostering effective, inclusive, and sustainable mentorship environments that are responsive to the demands of modern surgical residency training.
Supplemental Material
Supplemental Material - Mentorship in General Surgery Residency: A Qualitative Study
Supplemental Material for Mentorship in General Surgery Residency: A Qualitative Study by Terrance Peng, Sloan Senofsky, Kruti Desai, James X Wu, Areti Tillou, Justin P Wagner, Formosa Chen in The American Surgeon™.
Footnotes
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
