Abstract
While reusable surgical scrub caps are associated with lower carbon emissions compared to single-use scrub caps, many hospital systems prohibit reusable scrub caps in the OR. Between 11/5/24 and 3/26/25, an evaluation of scrub cap usage was performed while OR sustainability lectures were delivered to perioperative staff and surgical specialty departments. Pre- and post-lecture Likert surveys assessed OR sustainability knowledge, motivation to improve, and scrub cap preference. Overall, 255 pre- and 230 post-lecture surveys were analyzed. Of pre-lecture respondents, 57.4% felt knowledgeable, 90.8% felt motivated to improve OR sustainability, and 40.2% preferred single-use scrub caps. Pre-lecture odds ratios showed younger respondents (vs older, OR 2.27, 95% CI 1.28-4.04, P = 0.006) and surgeons (OR 3.77, 95% CI 2.01-7.06, P < 0.0001) felt less knowledgeable and other perioperative staff felt more knowledgeable (OR 0.47, 95% CI 0.27-0.82, P = 0.007) than nursing staff. Surgeons felt less motivated than nursing staff (OR 2.60, 95% CI 1.33-5.09, P = 0.006), and younger respondents were less likely to prefer single-use scrub caps (vs older, OR 2.06 95% CI 1.16-3.64, P = 0.01). Post-lecture, 87.9% felt knowledgeable, 94.4% felt motivated to improve OR sustainability, and 42.5% preferred single-use scrub caps. No differences were noted among comparison groups post-lecture. At the end of the study period, official hospital policy was revised to allow use of reusable scrub caps. Comparing the 6 months before and after the policy change, 31,200 fewer disposable scrub caps were purchased at a cost savings of $976.22.
• High levels of motivation for improved OR sustainability exist among all stakeholders. • Following education about OR sustainability, differences in opinions about reusable scrub caps were mitigated. • A multidisciplinary, evidence-based approach enabled a successful hospital scrub cap policy change, resulting in reduced use and cost of disposable scrub caps.Key Takeaways
Introduction
The American health care system generates about 8.5% of total United States (U.S.) greenhouse gas emissions and generates over 4 billion pounds of waste annually.1,2 Despite comprising a small fraction of a hospital system’s physical footprint, operating rooms (OR) account for 70% of health care waste.1,3 ORs are also responsible for 40-60% of hospital supply costs and consume 3 to 6 times more energy per square foot than anywhere else in the facility. 4 Overall, ORs contribute to one third of health care-related greenhouse gases.
The immense opportunity for energy, waste, and cost savings in hospital systems, and in ORs in particular, has been increasingly recognized. 4 Single-use disposable products, such as disposable scrub caps, are the norm. 1 Replacing single-use disposable scrub caps with reusable cloth scrub caps is associated with lower carbon emissions. 5 Despite available data in support of the safety and efficacy of reusable scrub caps when used appropriately,5–10 there has been longstanding controversy regarding what comprises appropriate head coverings in the OR. 11 Reusable surgical scrub caps are recognized by the U.S. Food and Drug Administration (FDA), Advancing Safety in Health Technology (AAMI), and Association of periOperative Registered Nurses (AORN) guidelines as safe and effective,7,8,9 yet many major hospital systems do not allow their use in the OR.
As part of a system-wide environmental stewardship initiative, we assessed attitudes towards reusable scrub caps and describe the process by which our hospital policy requiring use of single-use scrub caps was changed to allow use of reusable scrub caps.
Methods
Establishment of the Environmental Sustainability Committee and OR Sustainability Subcommittee
In 2023, Loma Linda University Health (LLUH) launched the Environmental Sustainability Committee (ESC). This committee consists of a multidisciplinary team across the health care system that includes representatives from executive leadership, environmental health and safety, facilities management, campus engineering, supply chain management, finance, clinicians, community partnerships, process improvement, construction, marketing, trainees, and students. The committee was designed to enable interdisciplinary collaboration among participants throughout the hospital system for implementation of sustainable, cost-effective practices.
OR sustainability was designated a strategic aim of the committee and an OR Sustainability Subcommittee was created that included surgeons, anesthesiologists, clinical epidemiologists, OR management, and medical students. Using the Practice Greenhealth Greening the OR toolkit, 4 multiple initiatives were developed to support OR sustainability. Among the initiatives, the use of single-use disposable scrub caps was assessed.
Evaluation of Hospital Scrub Cap Policy
At project outset, hospital policy required that “All persons must wear hospital-provided single-use disposable hair covering worn in a way to appropriately cover hair. If worn, fabric caps must be covered with hospital-provided single-use disposable hair covering.” Between 11/5/24 and 3/26/25, the OR Sustainability Subcommittee, including representatives from infection prevention and control and supply chain departments evaluated usage, literature, and case studies5,12–15 regarding reusable scrub caps. Key stakeholders involved with changing hospital policy were present at ESC meetings and were informed of the safety, efficacy, and cost savings of using reusable scrub caps.
OR Sustainability Education
In parallel to the evaluation of hospital scrub cap policy change, education workshops were developed by the ESC and delivered to perioperative staff and surgical specialty departments. Pre- and post-lecture Likert surveys assessed perceptions of OR sustainability knowledge, motivation to improve OR sustainability, and scrub cap preference. The specific questions used were as follows: “Please rate how you feel about OR sustainability: (a) I am knowledgeable about particular ways that OR sustainability is practiced at LLUH, (b) I am motivated to improve the sustainability of surgical practices, and (c) I like to wear single-use scrub caps more than reusable scrub caps.” Responses were compared by age group (<40 vs > 40 y), years employed (<6 vs > 6 y), and specialty (surgeon: surgical attending, trainee, or student; other perioperative staff: anesthesia technician, scrub technician, hospital administrators, environmental service workers, or other staff; nursing staff: preoperative, OR, or PACU nurse or OR manager). Likert-scale responses were analyzed as ordinal outcomes, with categories coded from 1 (strongly disagree) to 5 (strongly agree). Associations between participants’ age (<40 vs ≥ 40 years), years of work experience (<6 vs ≥ 6 years), working department and Likert-scale responses were assessed using ordinal logistic regression models. Odds ratios and corresponding 95% confidence intervals were estimated to quantify the strength of associations. Models were fitted under the proportional odds assumption, which was assessed using standard diagnostic tests. All analyses were conducted using SAS version 9.4 and statistical significance was defined as a two-sided P value <0.05. The LLUH IRB determined that this project did not meet the definitions of human subject research.
Results
OR Sustainability Attitudes
Survey Respondent Demographics
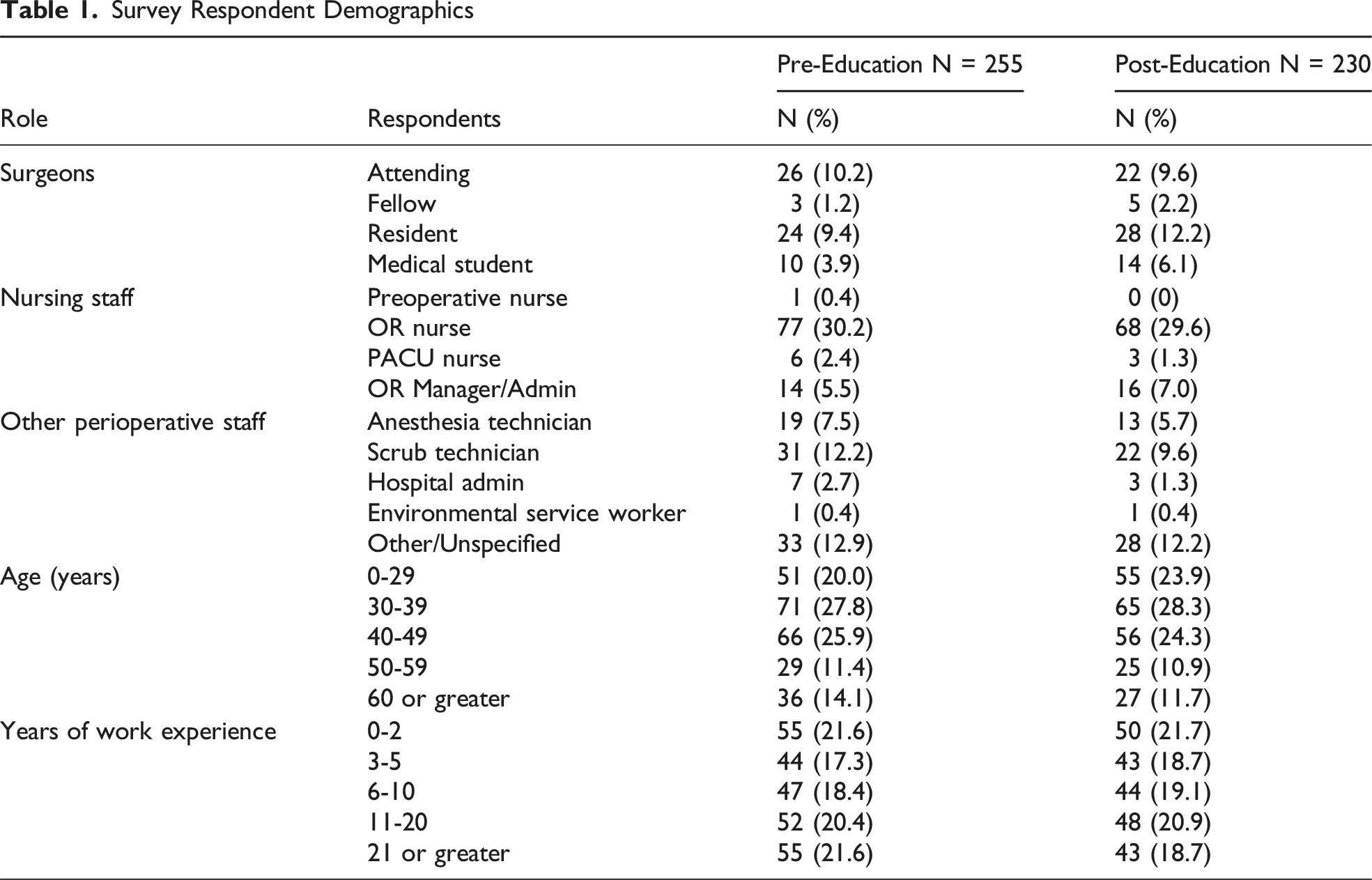
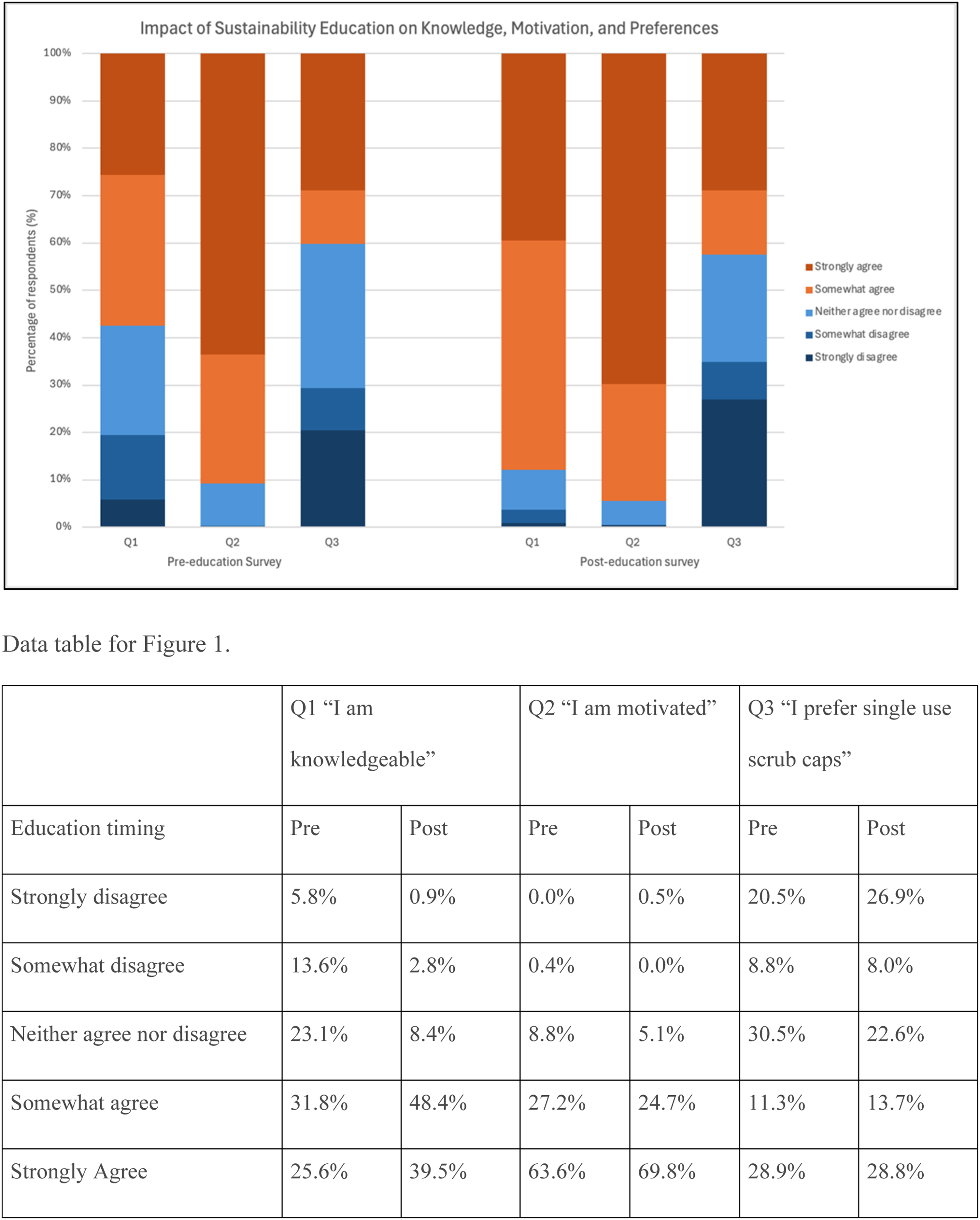
Pre- and post-education responses
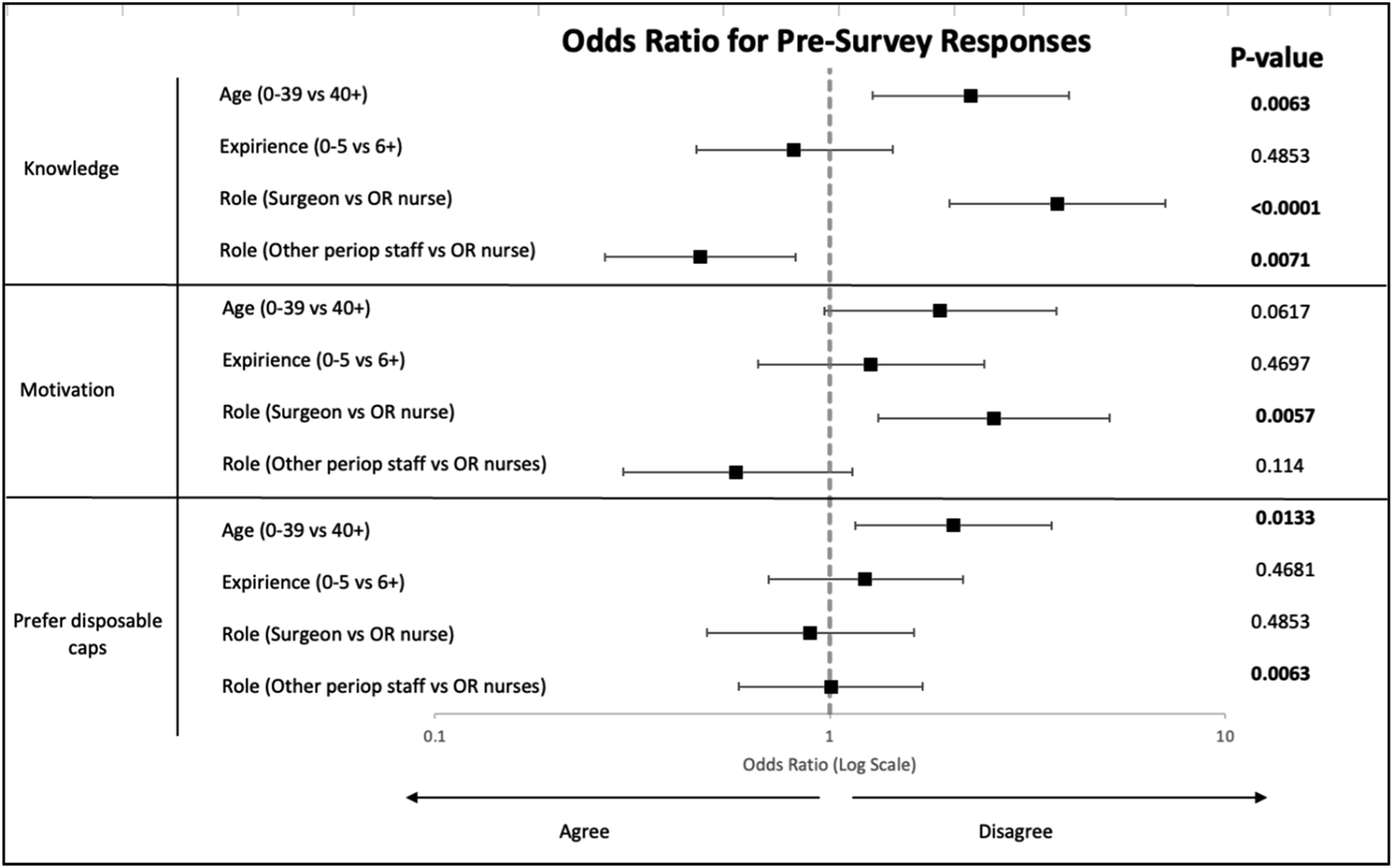
Odds ratios for pre-education survey responses
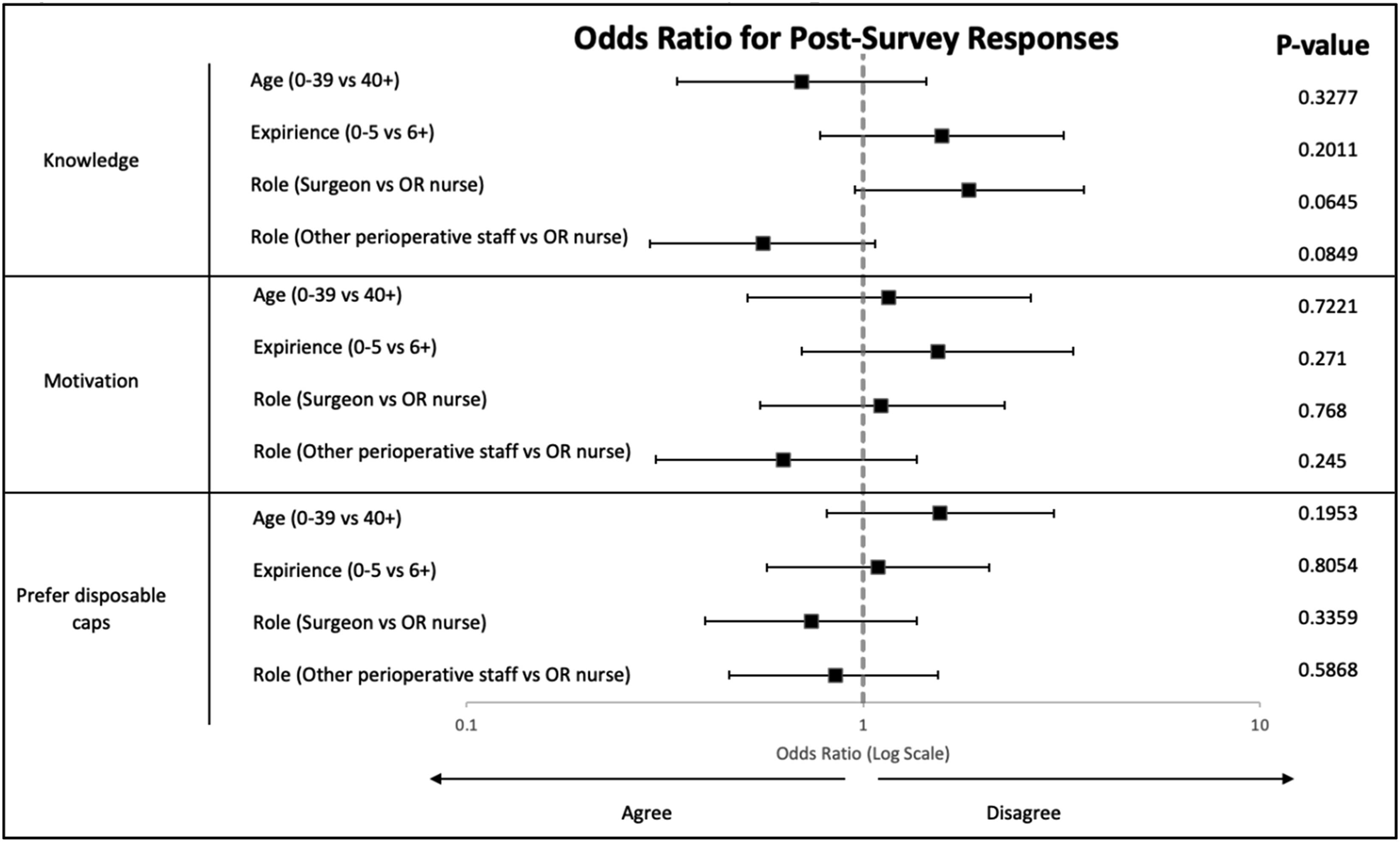
Odds ratios for post-education survey responses
Hospital Scrub Cap Policy
The infection prevention and control analysis concluded that reusable scrub caps are not associated with increased infection risk and would comply with regulatory requirements. Supply chain reports showed that 563,375 disposable scrub caps at a cost of $37,295 were purchased in the prior 12 months. At the completion of background research and information sharing, the ESC supported the adoption of new hospital policy. Official hospital policy was revised to allow use of reusable scrub caps at LLUH-affiliated hospitals. A review of the terminology of hospital policies in California allowing the use of reusable scrub caps in the OR was performed, and terminology was adopted into LLUH policy. New policy language included the following: “Coverings must cover the scalp and hair when entering semi-restricted and restricted areas. Reusable and disposable scrub hats, hijabs, caps, and bouffants are allowed. Reusable head coverings must be visibly clean and intact (ie, not torn, frayed, or otherwise damaged) and be laundered frequently. Head coverings that are visibly soiled or wet must be changed. LLUH is not responsible for laundering employee owned reusable head coverings. Disposable hats do not need to be worn over reusable head coverings.”
The new policy language was submitted to a multidisciplinary surgical quality improvement committee which reviewed and approved the change. The new policy proposal was then submitted to the medical staff executive committee which also approved the change allowing adoption as new hospital policy in March 2025. Notably, members on both of these committees were regularly present at ESC meetings where periodic updates were provided about findings of safety, efficacy, and cost-effectiveness of reusable scrub caps. The ESC meetings were instrumental in informing voting members to allow passage of the scrub cap policy.
Hospital Scrub Cap Usage
Scrub Cap Purchases and Cost 6 Months Pre- and Post-Hospital Policy Change
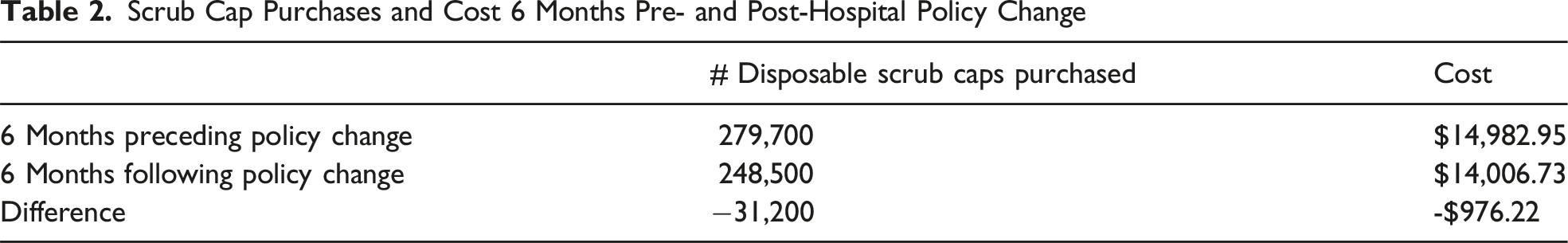
Discussion
There is growing recognition of the need for sustainable practices in the OR. Several strategies have been proposed including creating OR multidisciplinary sustainability committees, developing initiatives to reduce the environmental footprint of surgical activities, educating the surgical community about best practices, and decreasing the use of disposable equipment.16,17 The current report describes how implementation of these strategies has led to success in our institution.
Our process corroborates others that have allowed and encouraged use of reusable scrub caps in the OR. Hospital systems throughout California, the U.S., and internationally have adopted reusable surgical attire. While certainly not an exhaustive list, reusable scrub caps and surgical gowns have been adopted and recently reported by National Health Service (NHS) England, University of California, Massachusetts General Hospital, and University of Maryland Medical Center.12–15 Each of these organizations have reduced OR waste and saved cost by adopting reusable surgical attire. For example, NHS England reported an annual cost savings of ∼50,000 Euros (∼$58,200) and one ton of waste diversion by switching to reusable scrub caps. 12
Our pre- and post-lecture surveys gave us insight into attitudes about sustainability at our institution. Remarkably, 90.8% of respondents before and 94.4% after educational lectures were motivated to improve OR sustainability. While there was strong motivation among all groups of respondents, in the pre-lecture setting, the group representing surgeon attendings, fellows, residents, and medical students were less motivated than the group representing nursing staff. There were also differences in knowledge about OR sustainability in the pre-education setting. Younger respondents felt less knowledgeable than older respondents; compared with nursing staff, surgeons, trainees, and students felt less knowledgeable, whereas other perioperative staff felt more knowledgeable than nursing staff. In the post-lecture setting, differences in motivation knowledge among groups were dissipated. We were unable to explore underlying reasons for differences in attitudes among groups in our survey. Nonetheless, the high level of motivation to improve OR sustainability in our hospital system represents an opportunity to continue engaging our workforce for future initiatives towards OR sustainability.
We observed an unexpectedly high proportion of people who prefer single-use scrub caps rather than reusable scrub caps (40.2% pre-lecture; 42.5% post-lecture). We hypothesize that current hospital culture, speculation about safety, or other unknown motivations may contribute to personal preference. Future efforts will assess preferences following a more prolonged period after the scrub cap hospital policy change.
An additional benefit of allowing reusable scrub caps in the OR relates to proper identification and team cohesion. Two recent studies explored the use of personalized scrub caps with visible names and roles in the OR and found benefits such as decreased misidentification, decreased microaggressions, improved perceived culture of safety, improved team culture and teamwork, improved communication, and improved patient care.18,19 Another study found connections between professional uniform and professional pride and found connections between uniform-wearing and increased brain area activity involved in empathy, reward, and emotional regulation. 20 Reusable scrub caps can be customized to display names and insignias, while disposable caps are rarely personalized.
There are several limitations in this study. Because surveys were submitted anonymously, between group comparisons cannot be assumed to be independent. Follow-up assessment of scrub cap utilization and associated waste generation and greenhouse gas emissions is ongoing; therefore, the full financial and environmental impact of the scrub cap policy change cannot be determined at this time.
This successful policy change highlights the value of a multi-stakeholder committee approach combined with targeted education to support quality improvement in OR practices. While initial cost savings from reduced scrub cap purchases may seem small, wearing cloth scrub caps without a disposable covering is a visible symbol and daily reminder of engagement in sustainability practices within our hospital system. Implementation of the scrub cap policy change illustrates how OR sustainability initiatives can align the motivations of hospital administrators, surgeons, and others across the OR environment.
Supplemental Material
Supplemental Material - Reusable Scrub Cap Attitudes and Hospital Policy Change With Operating Room Sustainability Education
Supplemental Material for Reusable Scrub Cap Attitudes and Hospital Policy Change With Operating Room Sustainability Education by Daniel Nguyen, Ashley Kempf, Jasmine Hutchinson, Hala Nashed, Naveen Solomon, Marianne Schul, Liang Ji, Sharon Lum in The American Surgeon™.
Footnotes
Acknowledgments
The authors would like to acknowledge Dr Ihab Dorotta for his help in facilitating the scrub cap policy change.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
