Abstract
Aims
To evaluate the effect of obesity on postoperative mortality after trauma laparotomies.
Methods
A PRISMA-compliant meta-analysis with meta-regression using random-effects modeling was conducted (last search: August 01, 2025). All studies comparing the risk of postoperative mortality in adult patients with and without obesity (BMI ≥30) undergoing trauma laparotomies were included. The certainty of evidence was evaluated using GRADE system.
Results
Nine studies comprising 19,780 patients were included (obesity group: 6474; no obesity group: 13,306). The obesity and no obesity groups were comparable in terms of male sex (RD: −0.03, 95% CI −0.06, 0.00, P = .090), injury severity score (MD: 0.96, 95% CI −0.36, 2.29, P = .160), penetrating mechanism of injury (RD: −0.01, 95% CI −0.03, 0.00, P = .150), and blunt mechanism of injury (RD: 0.01, 95% CI −0.00, 0.03, P = .150). The patients in the obesity group were older (MD: 4.18 years; 95% CI 2.19, 6.18, P < .0001). The risk of postoperative mortality was higher in patients with obesity (OR: 1.33, 95% CI 1.09, 1.64. P = .006). Injury severity score (coefficient: 0.017, P = .004) and blunt mechanism (coefficient: 0.263, P = .017) were associated with an increased risk of mortality; penetrating mechanism (coefficient: −0.263, P = .017) was associated with a reduced risk of mortality; and age (coefficient: −0.004, P = .779) and male sex (coefficient: −0.055, P = .908) did not affect the mortality.
Conclusions
Obesity is associated with increased postoperative mortality in patients undergoing trauma laparotomies (moderate certainty). Injury severity score and blunt mechanism of injury may increase the risk of mortality in obese patients undergoing trauma laparotomies.
Keywords
Introduction
Trauma remains a leading cause of death worldwide. Trauma laparotomy is the standard procedure performed in patients sustaining life threatening internal injuries in the setting of blunt or penetrating abdominal trauma aiming to interrupt the lethal triad of hypothermia, coagulopathy, and acidosis.1,2 While it can effectively identify and manage intraabdominal hemorrhage, peritonitis, and organ damage amongst other traumatic complications, due to the emergent nature of the surgery it carries a high risk of mortality and morbidity. 3
The global obesity epidemic has amplified the number of trauma patients with obesity; hence, it is not uncommon to encounter an obese patient who needs trauma laparotomy. The available evidence delineates the association between obesity and adverse outcomes in trauma patients.4,5 Obesity results in increased in-hospital mortality, in-hospital complications, and longer length of stay in intensive care unit and hospital in trauma patients.4,5 While the negative impact of obesity on outcomes after non-trauma emergency laparotomies has been demonstrated,6-8 the prognostic significance of obesity in patients undergoing trauma laparotomies remains unknown. Recently, the impact of obesity on mortality in patients undergoing trauma laparotomies has been evaluated in several studies providing a rationale for conducting a systematic review. In this study we aimed to conduct a systematic review and meta-analysis to evaluate the effect of obesity on postoperative mortality following trauma laparotomies.
Methods
Methodological and Reporting Compliance
The methodology of the study followed the Cochrane Handbook for Systematic Reviews (version 6.4) 9 and the reporting of the study followed the Preferred Reporting Items for Systematic reviews and Meta-Analyses (PRISMA) 2020 statement standards. 10
Eligibility Criteria
Study Design
Obesity is a characteristic rather than an intervention and therefore it cannot be randomized. Consequently, identifying a randomized trial addressing the focus of this study was not feasible. All observational studies including cohort studies, case-control studies, and case series were eligible for inclusion in this study. Meta-analyses, systematic reviews, review articles, scoping reviews, case reports, and correspondence articles were excluded.
Population
All patients aged 18 or over who underwent trauma laparotomy were considered eligible for inclusion.
Prognostic Factor of Interest and Comparison
Obesity (BMI ≥30 kg/m2) was the prognostic factor of interest and no obesity (BMI <30 kg/m2) was the comparison of interest.
Outcome
The primary outcome measure was postoperative mortality. This was defined as death from any cause within 30 days of surgery.
Information Sources and Search Strategy
Two independent authors used search keywords, limits, thesaurus headings, and operators to develop a search strategy which was used in the following electronic sources: MEDLINE, Scopus, CENTRAL, the ISRCTN registry, the ICTRP registry, and ClinicalTrials.gov. The following combination of keywords was used: [trauma laparotomy (MeSH Terms) OR trauma laparotomy OR damage control laparotomy] AND [obesity (MeSH Terms) OR obesity]. The search had no language restrictions and the last date for the search was August 01, 2025. The reference lists of the included studies were also searched for more eligible studies.
Study Selection, Data Collection, and Data Items
The titles and abstracts of the identified articles were reviewed by 2 separate authors based and the full text of potentially eligible articles were retrieved to select the eligible articles. A third author was consulted if there was disagreement in study selection between the first 2 authors. The data items (bibliometric parameters, study design, characteristics of included population, age, sex, mechanism of trauma, injury severity score, and mortality) were determined by the authors at the protocol development stage followed by a pilot-testing technique of randomly selected studies. Data collection was done by 2 independent authors.
Study Risk of Bias and Evidence Certainty Assessment
The risk of bias in the included studies was evaluated using Quality In Prognosis Studies (QUIPS) tool by 2 independent authors. The certainty of evidence was evaluated using the GRADE system. If there was any discrepancy in assessment by the first 2 authors, a third author provided opinion.
Effect Measures and Synthesis Methods
RevMan Web was used for comparison meta-analysis and OpenMeta[Analyst] software was used for meta-regression. Risk difference (RD) was used as summary measure for dichotomous baseline characteristics variables and mean difference (MD) was used as summary measure for continuous baseline characteristics variables. Odds ratio (OR) was used as summary measure for postoperative mortality. The unit of analysis was individual patient. Random-effects modeling was used for analyses and forest plot with 95% confidence intervals (CIs) was constructed to present the results. Statistical heterogeneity was measured as I2 using Cochran’s Q test (χ2), and heterogeneity was classified as low when I2 was 0-25%, moderate when I2 was 25-75%, and high when I2 was 75-100%. A multivariable meta-regression analysis was conducted including age, male sex, injury severity score, penetrating mechanism of injury, and blunt mechanism of injury as independent variables and postoperative mortality as dependent variable. The protocol planned to evaluate the risk of publication bias using funnel plot if 30-day mortality was reported by a minimum of 10 studies.
Additional Analyses
Separate analysis for studies with low overall risk of bias and leave-one-out analysis were performed as sensitivity analyses.
Results
Search of electronic databases identified 148 articles of which 138 articles were excluded directly because they did not meet the principal eligibility criteria. Full-text review of the remaining 10 articles resulted in exclusion of 1 additional article because it had overlapping publication with another included study. Therefore, a total of 9 retrospective cohort studies11-19 including a total of 19,780 patients were eligible for inclusion. Figure 1 demonstrates the study PRISMA flow diagram and Table 1 shows the baseline characteristics of the included studies. Study PRISMA flow diagram Baselien Characteristics of the Included Studies BMI, body mass index.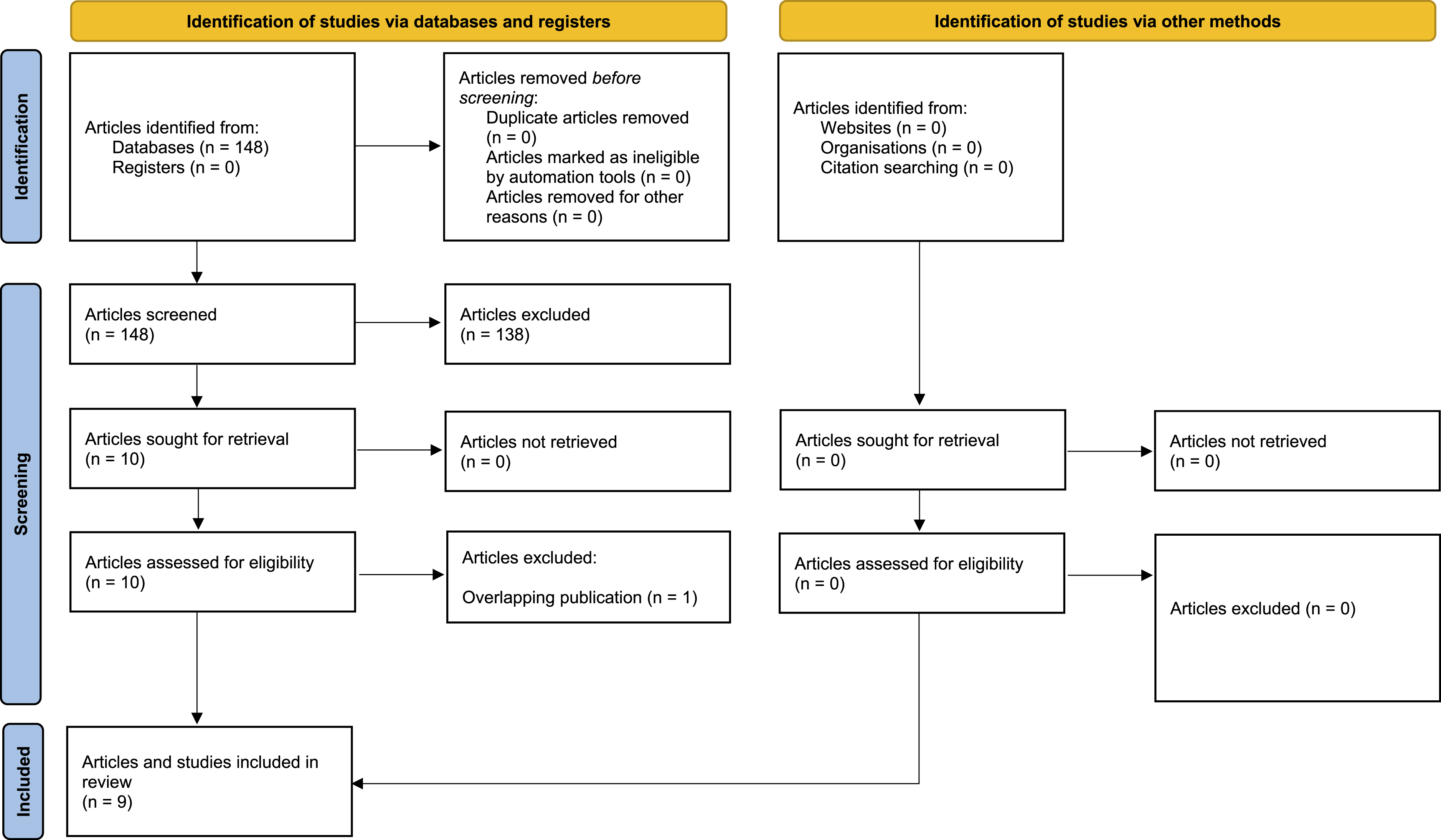
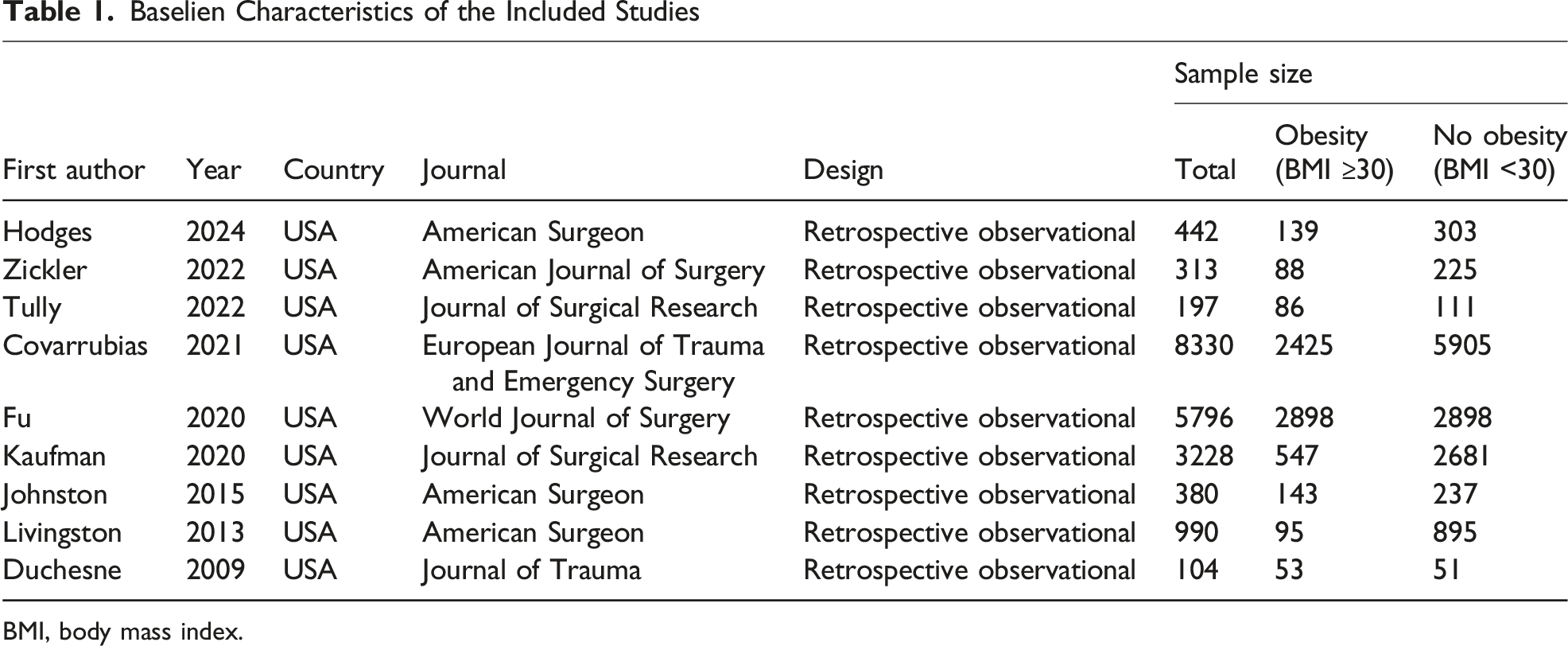
Baseline Characteristics of Included Population
Baseline Characteristics of the Included Patients
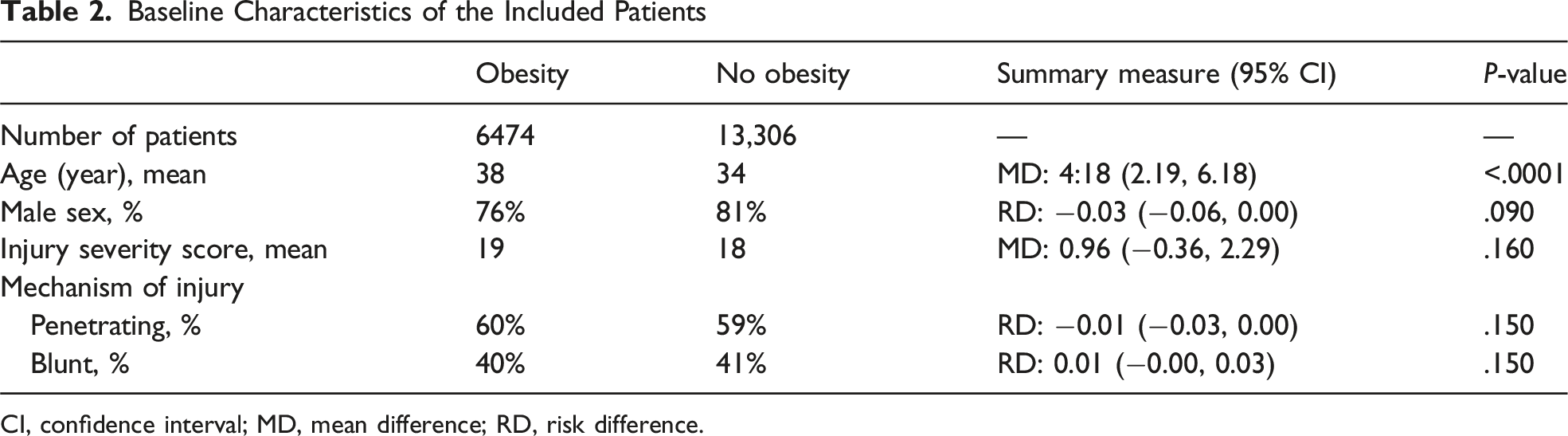
CI, confidence interval; MD, mean difference; RD, risk difference.
Risk of Bias in Included Studies
The included studies were judged to be of high risk of bias in terms of study confounding; however, all the included studies were judged to be of low risk of bias in terms of study participation, study attrition, prognostic factor measurement, outcome measurement, and statistical analysis and reporting.
Postoperative Mortality
Analysis of 19,780 patients from 9 studies showed that the risk of postoperative mortality was higher in the obesity group (OR: 1.33, 95% CI 1.09, 1.64. P= .006). The between-study heterogeneity was moderate (I2 = 48%) and the GRADE certainty of evidence was moderate (Figure 2). Forest plot for comparison of postoperative mortality between the obesity group and no obesity group. Risk of bias legends: (A) Study confounding; (B) study participation; (C) Study attrition; (D) Prognostic factor measurement; (E) Outcome measurement; (F) Statistical analysis; (G) Reporting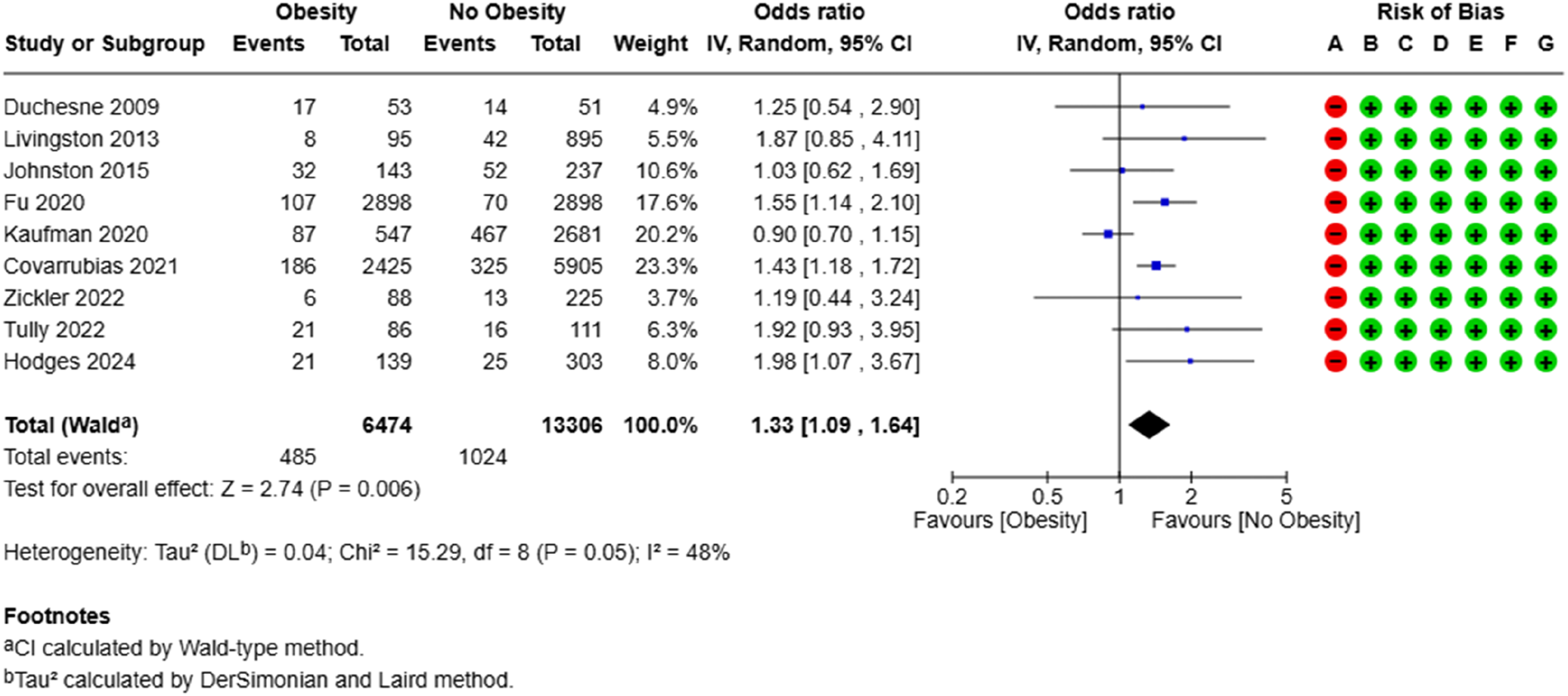
Predictors of Postoperative Mortality
Results of Meta-Regression Analysis for Predictors of Postoperative Mortality in Patients With Obesity Undergoing Trauma Laparotomies
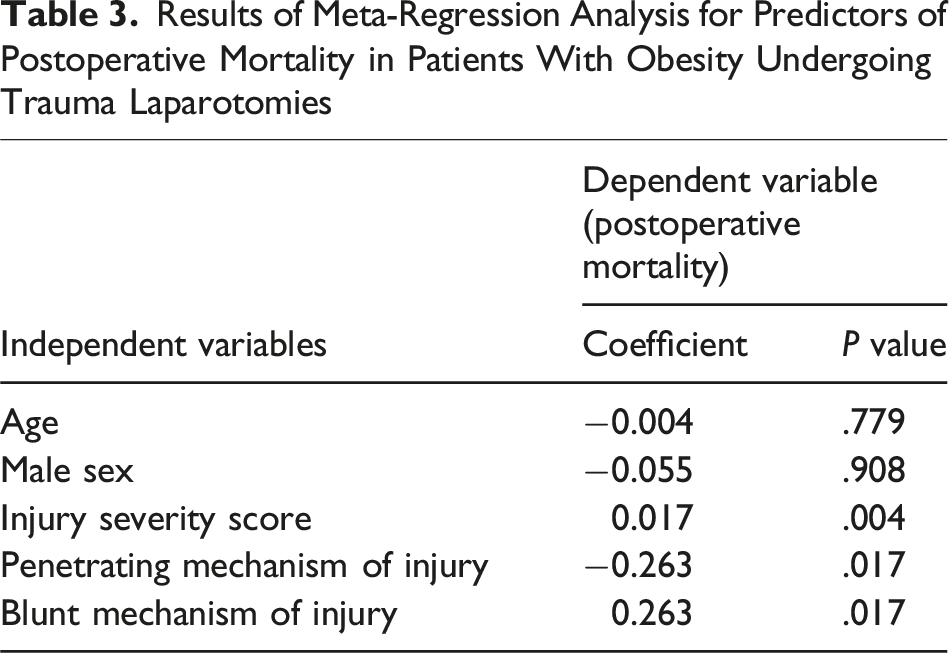
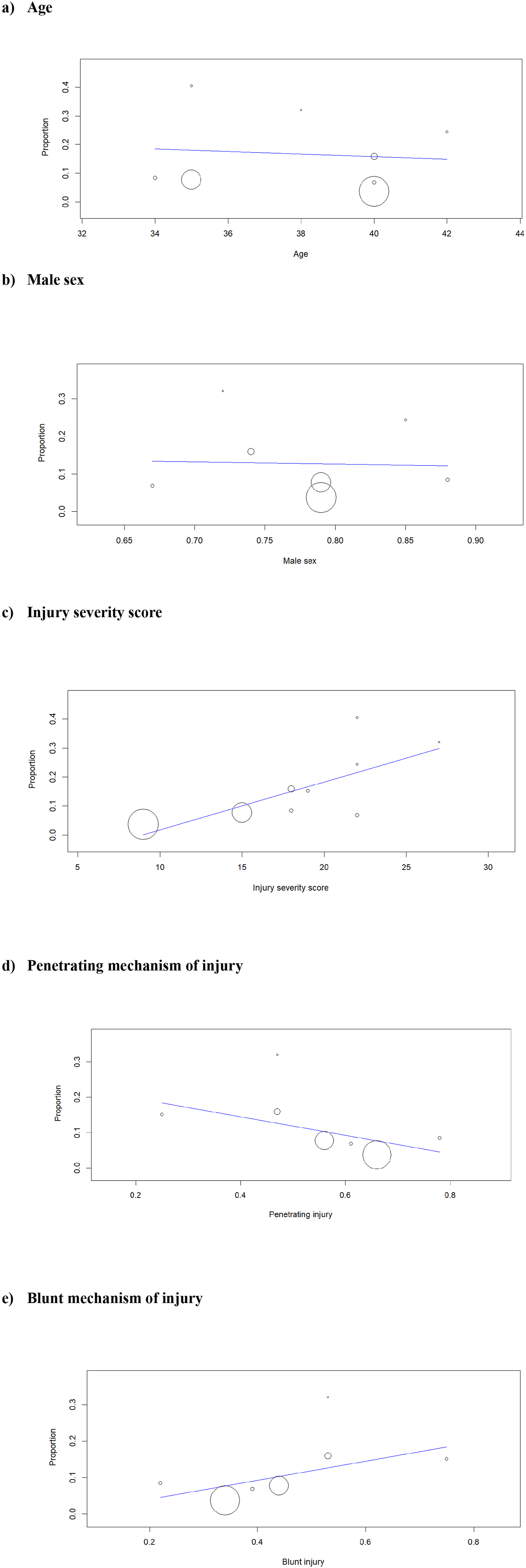
Bubble plots for meta-regression analysis for potential predictors of mortality in patients with obesity: (A) Age; (B) Male sex; (C) Injury severity score; (D) Penetrating mechanism of injury; (E) blunt mechanism of injury
Sensitivity Analyses
The direction of effect size remained unchanged for postoperative mortality when studies with low overall risk of bias were analyzed separately and when leave-one-out analysis was performed.
Discussion
In this study we analyzed of 19,780 patients from 9 studies. The analyses showed that obesity was associated with an increased risk of mortality after trauma laparotomy. Although the current study is the first meta-analysis evaluating the effect of obesity on mortality after trauma laparotomies, the external validity of the findings can be supported by studies conducted in non-trauma setting. Al-Shelleh et al 6 conducted a retrospective study of 385 patients which concluded that obesity was associated with a higher risk of mortality after non-trauma emergency laparotomy. In another study, Marahanumaiah et al 7 reported that obesity has negative impact on the outcomes after non-trauma emergency laparotomies. Moreover, Kassahun et al 8 evaluated 886 patients undergoing non-trauma emergency laparotomies and concluded that obesity is associated with higher risks of morbidity and mortality. The results of the aforementioned studies support our findings.
The negative impact of obesity on mortality can be justified. Patients with obesity are likely to have more comorbidities and higher American Society of Anesthesiologists (ASA) physical status, which are known to increase the risk of mortality after emergency laparotomies. 20 Moreover, obese patients are likely to need prolonged mechanical ventilation which in turn may increase the risk of postoperative complications. On the other hand, obesity can result in metabolic dysfunction and immunosuppression by impairing body’s physiological response to stress caused by trauma or underlying abdominal pathology. 21 All of the above can increase the risks of morbidity and mortality in obese patients.
Higher injury severity score and blunt mechanism of injury were found to be negative predictors of postoperative mortality in the current study. While the association between injury severity score and mortality has been demonstrated previously, 22 the association between blunt injury and mortality requires further clarification. Blunt abdominal injuries are likely to be associated with occult missed injuries which are challenging to detect at early stages of assessments. The delay in detection and management of such injuries, together with adverse consequences of the underlying injuries, may increase the risk of morbidity and mortality. 23 Another possible explanation for the lower risk of mortality in obese patients with penetrating injuries may be the protective effect of extra adipose tissue in abdominal wall.
The findings of the current study have implications for real practice. All trauma centers should adopt a dedicated diagnostic and management pathway for postoperative management of patients with obesity. Patients with obesity should be considered as high risk. They are at increased risks of postoperative infective complications,
24
multiorgan failure,
25
acute respiratory distress syndrome, prolonged mechanical ventilation, and frequent failed extubation attempts.
26
The management pathway of obese patients should be based on strategies aiming to minimize technical difficulties associated with ventilation, hygiene, mobilization, vascular access, and detection of missed injuries.27,28 Such pathways should include the following: • Early admission to critical care unit • Early detection and management of infective complications • Positioning the patient in a head-up position • Using continuous positive airway pressure during preoxygenation • Administrating oxygen via nasal cannula during intubation • Selecting appropriate ventilation modes.
29
The current study has some limitations. The included studies had retrospective design and are subject to inevitable risk of selection bias and confounding bias. In order to take these limitations into account, we downgraded the certainty of evidence. However, it is important to recognize that obesity is a character that cannot be randomized. Therefore, conducting a randomized controlled trial in this setting is not possible and the results from observational studies provide the best available evidence. The included studies were conducted in 1 country which may affect the generalizability of the findings. This meta-analysis included less than 10 studies; therefore, publication bias could not be assessed formally.
The current study has the following strengths. The study had a relatively large sample size which reduces the risk of type 2 error. Sensitivity analyses confirmed consistency of the results and the meta-regression analyses recognized the potential confounding factors. The included population in the obesity group and no obesity group were comparable in terms of most of the baseline characteristics. Although the patients in the obesity group were older, this was not clinically significant as the mean age difference was only 4 years and the meta-regression analyses did not identify age as a significant predictor. Therefore, we do not believe that the difference in age between the 2 groups affected the outcome.
Conclusions
Obesity is associated with increased risk of postoperative mortality in patients undergoing trauma laparotomies (moderate certainty). Injury severity score and blunt mechanism of injury may increase the risk of mortality in obese patients undergoing trauma laparotomies. The risk of publication bias could not be excluded. Evidence from prospective studies is required for more robust conclusions.
Supplemental Material
Supplemental Material - Risk and Predictors of Postoperative Mortality in Patients With Obesity Undergoing Trauma Laparotomy: A Systematic Review and Meta-Analysis With Meta-Regression
Supplemental Material for Risk and Predictors of Postoperative Mortality in Patients With Obesity Undergoing Trauma Laparotomy: A Systematic Review and Meta-Analysis With Meta-Regression by Aya Kambal, Libor Hurt, Michalis Iosifidis, Shahin Hajibandeh, and Shahab Hajibandeh in The American Surgeon™.
Footnotes
Ethical Considerations
Patient consent and approval from Research Ethics Committees were not required in this study because of the nature of the study design (meta-analysis).
Author Contributions
Conceptualization: Shahab H; Methodology: AK, Shahab H; Data curation: AK, Shahab H; Validation and formal analysis: AK, LH, Shahin H, and Shahab H; Supervision: Shahab H; Visualization: Shahin H and Shahab H; Project administration: Shahab H; Writing (original draft): AK, LH, MI, Shahin H, and Shahab H; Writing (review and editing): AK, LH, MI, Shahin H, and Shahab H.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The corresponding author (Shahab H) will provide any additional data related to this study on reasonable request.
Supplemental Material
Supplemental material for this article is available online.
