Abstract
Background
Most studies demonstrating efficacy of surgical stabilization of rib fractures (SSRF) are in patients with isolated severe chest wall injury. Recent evidence suggests SSRF may reduce mortality in polytrauma patients. The present study examines SSRF outcomes in severe polytrauma patients.
Methods
The 2013-2021 Trauma Quality Improvement Project database was used to identify severe polytrauma patients, defined as Injury Severity Score (ISS) ≥15 and abbreviated injury scale (AIS) ≥2 in 2 or more regions, with rib fractures. Exclusion criteria included AIS 6 in any region, death ≤72 hours, or SSRF >72 hours after admission. Outcomes of interest were in-hospital mortality, pneumonia, acute respiratory distress syndrome (ARDS), and length of mechanical ventilation. Adjustment for confounding was achieved using inverse probability of treatment weighting, Poisson regression models and quantile regression models.
Results
A total of 388 091 patients met inclusion criteria, of which 1.3% (N = 5020) underwent SSRF. SSRF was associated with a 57% decreased risk of mortality (P < 0.001) and 53% lower risk of ARDS (P < 0.001). Patients who underwent SSRF also required approximately 1 day less of mechanical ventilation (P < 0.001). Patients with ISS 15-19 exhibited an association between SSRF and a 55% (P = 0.023) lower rate of pneumonia.
Conclusion
SSRF within 72 hours of admission in severe polytrauma patients is associated with a lower rate of mortality and acute respiratory distress syndrome, along with shorter duration of mechanical ventilation. A reduction in the rate of pneumonia was only observed among patients with ISS 15-19.
Key Takeaways
• Surgical stabilization of rib fractures within 72 hours of admission in severe polytrauma patients is associated with a lower rate of mortality and acute respiratory distress syndrome, along with shorter duration of mechanical ventilation. • Surgical stabilization of rib fractures was only associated with reduction in the rate of pneumonia among patients with ISS 15-19.
Background
Polytrauma, defined as significant injury in more than one body region, makes up over one quarter of trauma patients, and these patients have increased mortality compared to their less injured counterparts. 1 Polytrauma is a distinct disease which manifests with physiologic changes greater than the sum of the individual injuries because of an exaggerated systemic stress response and inflammatory cascade at the cellular level. 2 Approximately two-thirds of polytrauma patients have thoracic trauma, and the overall mortality rate for polytrauma patients reaches 18%. 3
Surgical stabilization of rib fractures (SSRF) has shown benefit in flail chest and non-flail rib fractures.4,5 However, polytrauma patients often have other injuries which compete for priority for interventions in their care. Among polytrauma patients requiring admission to the intensive care unit (ICU), the most common injury other than rib fracture is brain injury at nearly 40%. 6 There has historically been concern that rib fixation would have a negative effect on other organ injuries, especially traumatic brain injury (TBI). However, evidence shows that SSRF may improve outcomes in patients with TBI, suggesting that this procedure may also benefit the overall recovery of patients with multisystem injuries. 7
Optimizing pulmonary status is key in the recovery of severely injured patients. Pneumonia is especially morbid and sometimes mortal in the polytrauma patient increasing odds of death by over five-fold. 8 Becker et al performed a retrospective analysis of a multinational trauma database and demonstrated that SSRF in polytrauma reduced mortality, ventilator duration, ICU LOS (length of stay), and hospital LOS. 9 However, that study included patients who underwent SSRF up to 3 weeks after the initial trauma, significantly longer than the recommended 48-72-hour window, possibly confounding outcomes.9,10 In the management of patients with multiple severe injuries, SSRF may not be considered as other injuries are being rapidly triaged and addressed, or the patient is deemed too unstable for fixation. 11 It is not yet known if SSRF is associated with improved outcomes in severe polytrauma patients.
This study uses a large national sample from the Trauma Quality Improvement Project (TQIP) to compare outcomes of operative and conservative management of rib fractures in patients with polytrauma. We hypothesize that SSRF will improve overall mortality and respiratory outcomes in severe polytrauma patients.
Methods
This is a retrospective cohort study of the 2013-2021 American College of Surgeons TQIP dataset. All severe polytrauma patients ≥18 years old who suffered rib fractures from blunt trauma were included. Severe polytrauma was defined as an Injury Severity Score (ISS) ≥15 along with an abbreviated injury scale (AIS) ≥2 in 2 or more regions. Patient demographics, clinical characteristics, and outcomes were abstracted. Patients with an AIS of 6 in any region were excluded as these patients are usually too severely injured to survive. In order to eliminate the effect of immortal time bias, patients were also excluded if they died within 72 hours of admission or underwent SSRF >72 hours after admission. Exemption was granted by the Institutional Review Board from ethical approval due to the TQIP dataset consisting of an anonymized, retrospective dataset. All analyses were performed in accordance with the Declaration of Helsinki and the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) guidelines.
Statistical Analysis
Patients were divided based on whether or not they underwent SSRF and then further stratified based on ISS into following groups: ISS 15-19, ISS 20-24, and ISS 25-75. Variables were summarized using medians and interquartile ranges (IQRs) or counts and percentages depending on if they were continuous or categorical. To determine the significance of differences between the cohorts, the Mann-Whitney U-test, Chi-squared test, or Fisher’s exact test was used, as appropriate. The primary outcome was in-hospital mortality while the secondary outcomes were pneumonia, acute respiratory distress syndrome (ARDS), and length of mechanical ventilation (defined as the cumulative number of calendar days of invasive mechanical ventilation during the index stay, regardless of continuity or re-intubation).
Adjustment for potential confounders was accomplished using inverse probability of treatment weighting (IPTW). The probability of undergoing SSRF was determined using a logistic regression model. This model included age, sex, race, highest AIS in each region (head, face, neck, spine, thorax, abdomen, upper extremity, lower extremity, and external), vitals on admission (systolic blood pressure, pulse rate, temperature, oxygen saturation, respiratory rate, and Glasgow Coma Scale), number of rib fractures (single/multiple), flail chest, sternum fracture, pneumothorax, hemothorax, pulmonary contusion, regional analgesia, epidural analgesia, and spinal analgesia, mechanical ventilation, as well as comorbidities (hypertension, previous myocardial infarction, congestive heart failure, history of peripheral vascular disease, cerebrovascular disease, dementia, chronic obstructive pulmonary disease, smoking status, chronic renal failure, diabetes mellitus, cirrhosis, coagulopathy, currently receiving chemotherapy for cancer, metastatic cancer, drug use disorder, alcohol use disorder, major psychiatric illness, and advanced directives limiting care) as predictors. The weights were calculated as
As a sensitivity analysis, propensity score matching was also performed. Conservatively managed patients were matched without replacement at a 1:1 ratio to patients who underwent SSRF using a nearest neighbor algorithm with a caliper of 0.2. Patients were matched on the same variables included in the analysis combining IPTW and Poison regression. The significance of differences following propensity score matching was determined using McNemar’s test with Bonferroni correction for categorical variables, and a Wilcoxon signed-rank test for non-normally distributed continuous variables.
Statistical significance was defined as P-value <0.05. Missing data were managed using multiple imputation by chained equations. Imputation was performed on the dataset as a whole. In total, 7 imputed datasets were generated and results were pooled using Rubin’s rule. For the subgroup analyses, relevant patients were first extracted from the larger imputed datasets before analyses were performed. Analyses were performed using the statistical programming language R version 4.5.1 (R Foundation for Statistical Computing, Vienna, Austria) using the tidyverse, parallel, quantreg, sandwich, survey, MatchIt, tableone, and mice packages.
Results
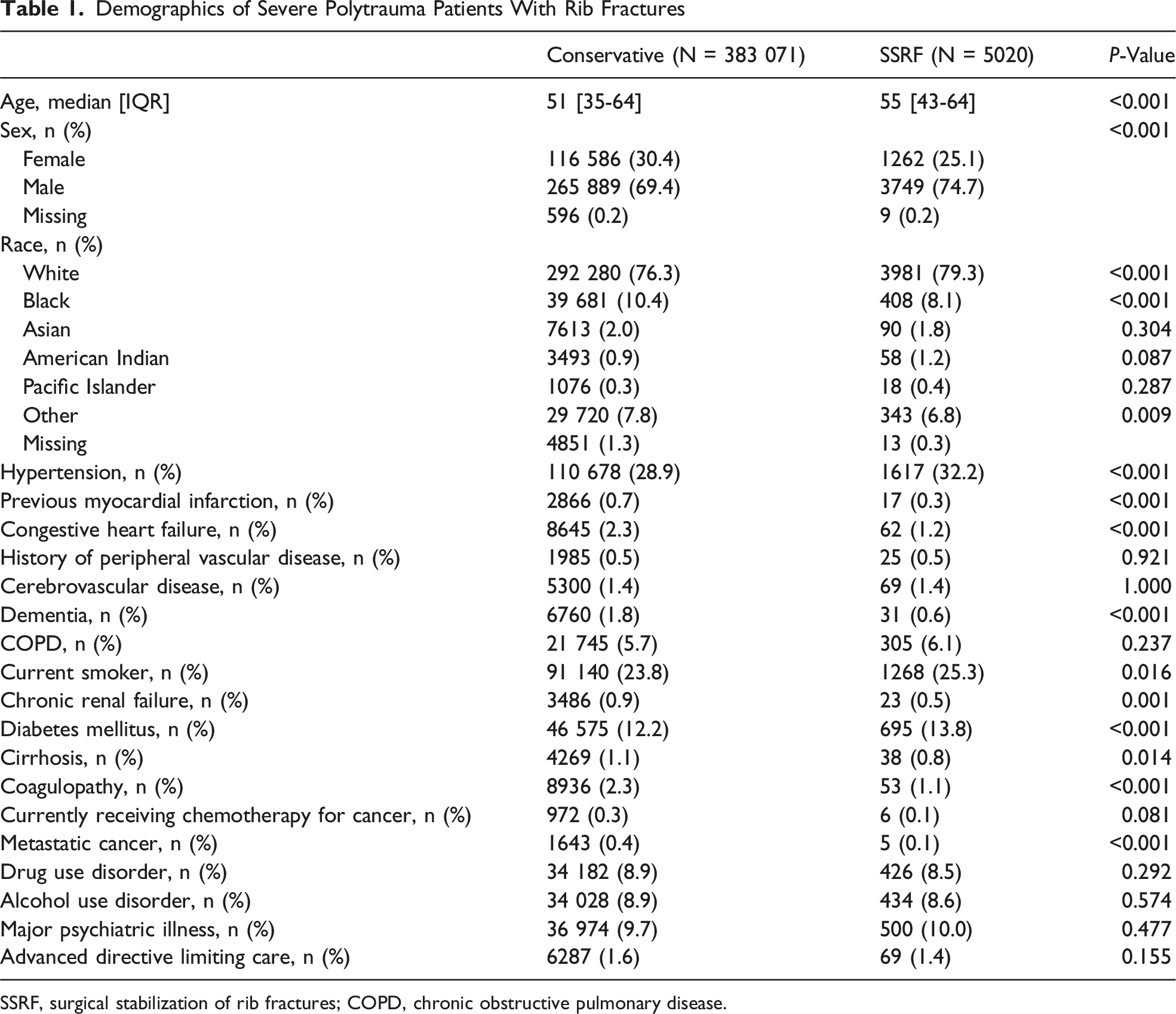
After applying the previously described inclusion and exclusion criteria, 388 091 polytrauma patients with rib fractures remained, of whom 1.3% (N = 5020) underwent SSRF within 72 hours of admission (Figure 1). Patients who underwent SSRF tended to be slightly older (55 vs 51, P < 0.001). Those who underwent SSRF were also slightly more often male (74.7% vs 69.4%, P < 0.001). The majority of patients identified as White in both cohorts. While most comorbidities were rare in this patient population, those who underwent SSRF exhibited higher rates of hypertension, smoking, and diabetes mellitus. Conversely, those who were managed conservatively demonstrated higher rates of previous myocardial infarction, congestive heart failure, dementia, chronic renal failure, cirrhosis, coagulopathy, and metastatic cancer (Table 1). Patient flow chart Demographics of Severe Polytrauma Patients With Rib Fractures SSRF, surgical stabilization of rib fractures; COPD, chronic obstructive pulmonary disease.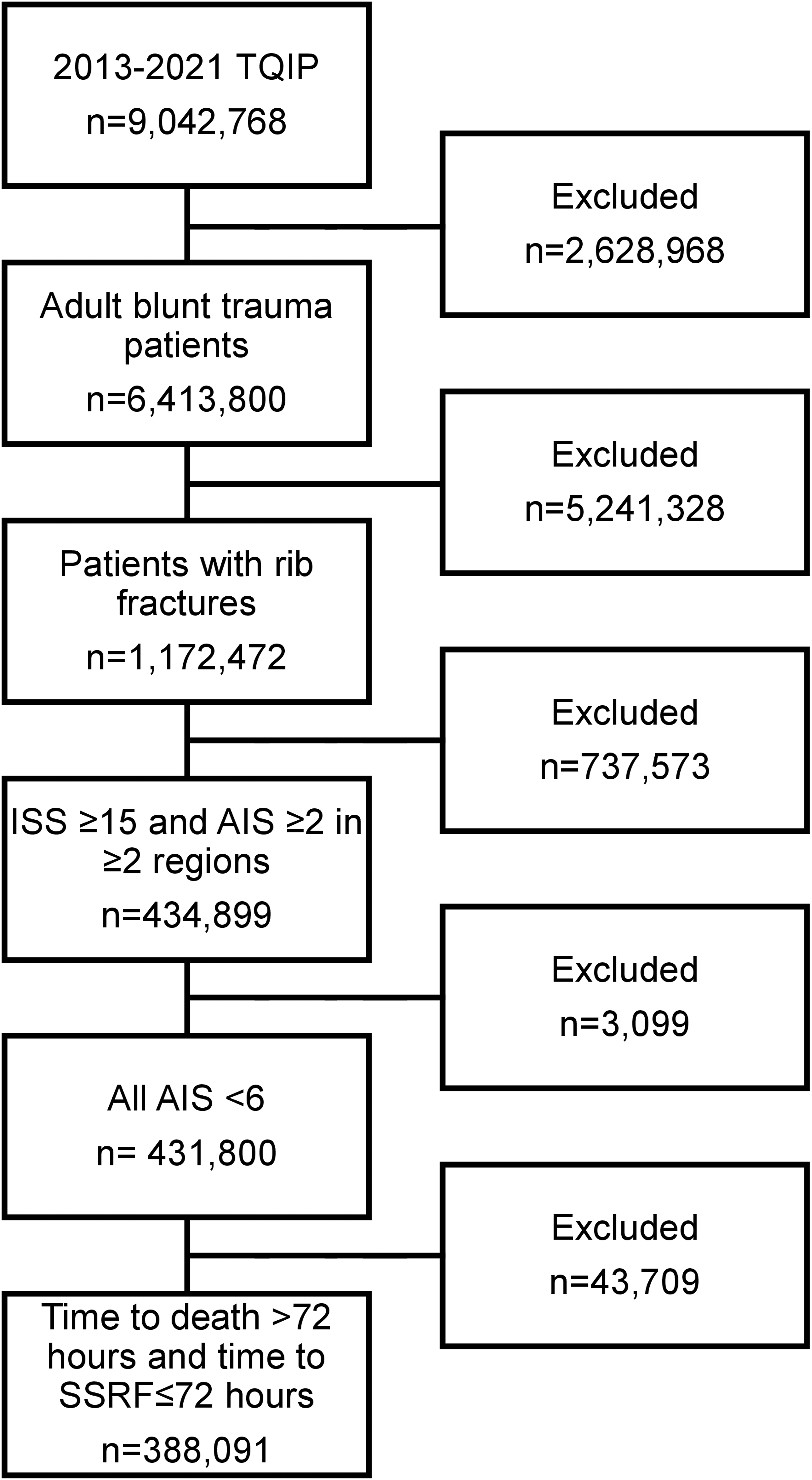
Clinical Characteristics of Severe Polytrauma Patients With Rib Fractures
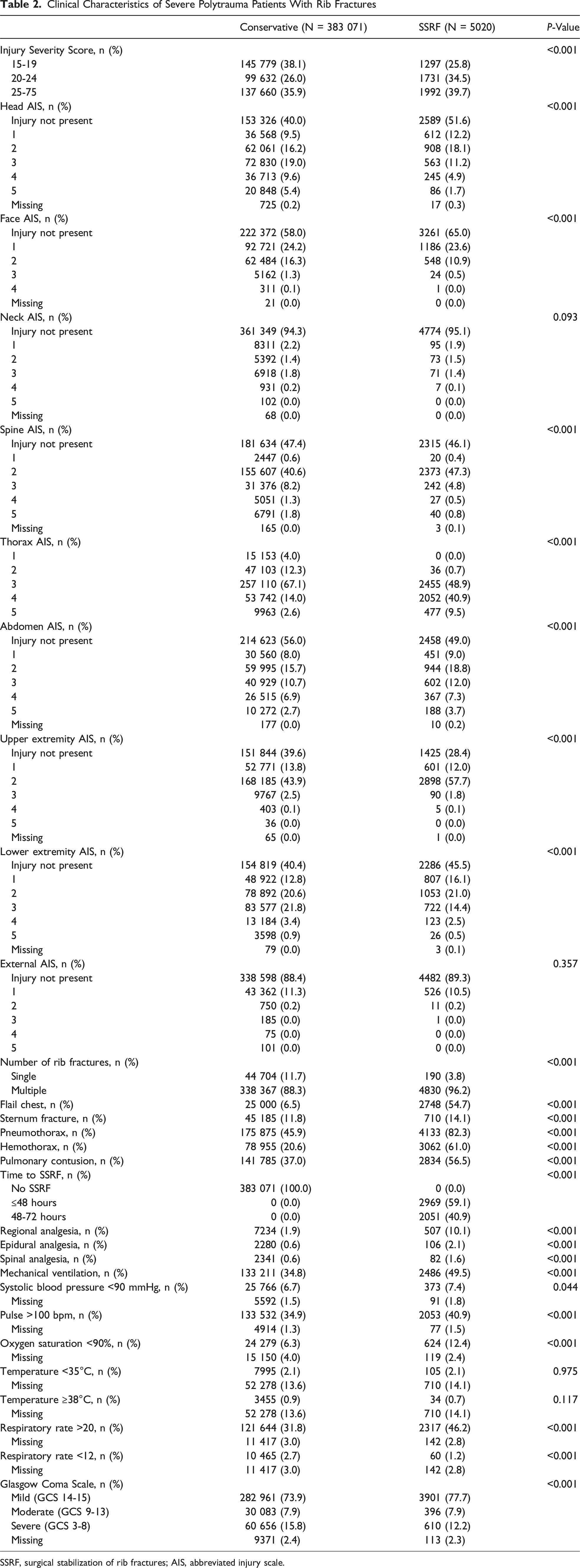
SSRF, surgical stabilization of rib fractures; AIS, abbreviated injury scale.
Crude Outcomes in Severe Polytrauma Patients With Rib Fractures
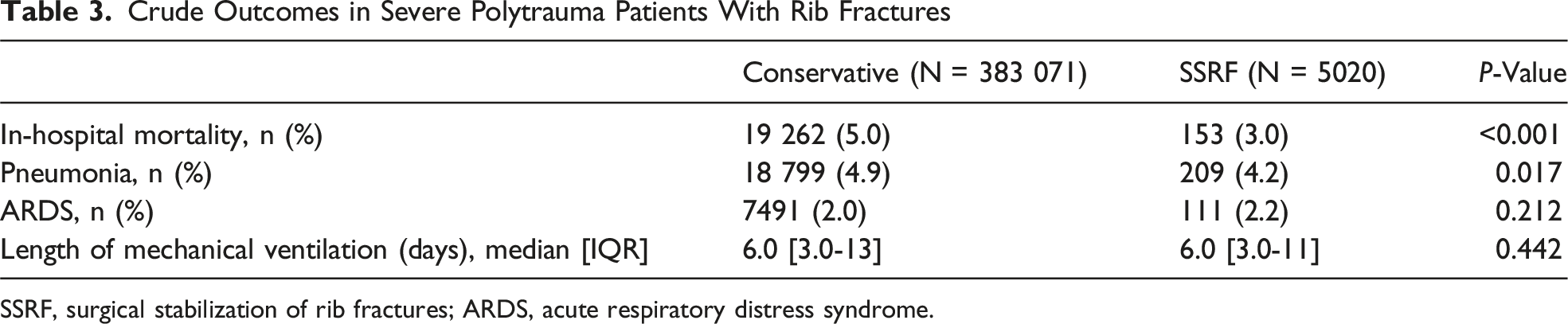
SSRF, surgical stabilization of rib fractures; ARDS, acute respiratory distress syndrome.
Association Between SSRF and Mortality, Pneumonia, ARDS, and LMV in Severe Polytrauma Patients With Rib Fractures After IPTW and Poisson Regression
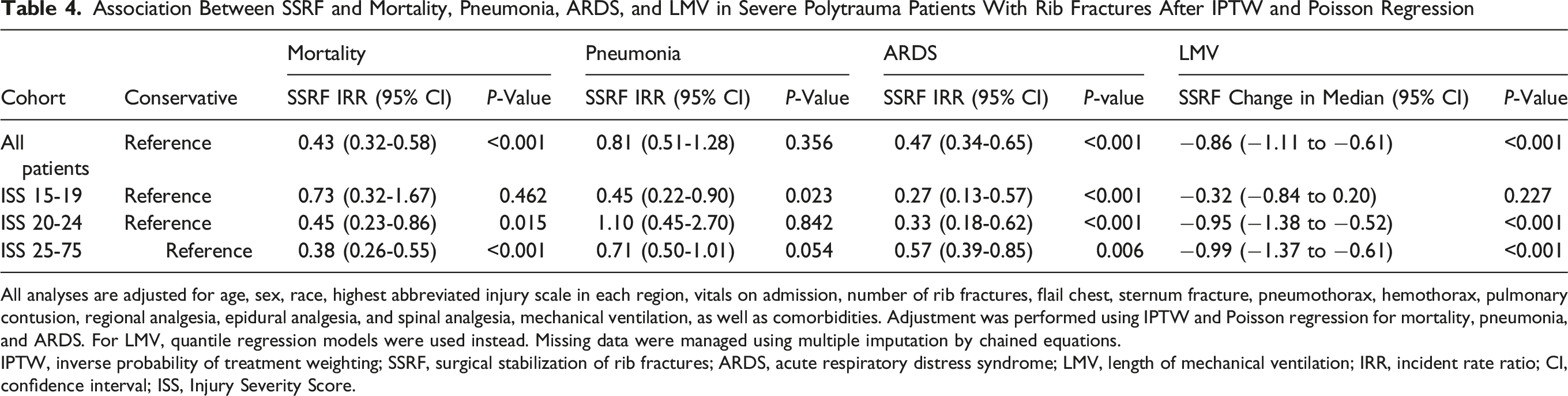
All analyses are adjusted for age, sex, race, highest abbreviated injury scale in each region, vitals on admission, number of rib fractures, flail chest, sternum fracture, pneumothorax, hemothorax, pulmonary contusion, regional analgesia, epidural analgesia, and spinal analgesia, mechanical ventilation, as well as comorbidities. Adjustment was performed using IPTW and Poisson regression for mortality, pneumonia, and ARDS. For LMV, quantile regression models were used instead. Missing data were managed using multiple imputation by chained equations.
IPTW, inverse probability of treatment weighting; SSRF, surgical stabilization of rib fractures; ARDS, acute respiratory distress syndrome; LMV, length of mechanical ventilation; IRR, incident rate ratio; CI, confidence interval; ISS, Injury Severity Score.
In the subgroup analyses, only patients with ISS 20-24 [IRR (95% CI): 0.45 (0.23-0.86), P = 0.015] and ISS 25-75 [IRR (95% CI): 0.38 (0.26-0.55), P < 0.001] exhibited a statistically significant reduction in in-hospital mortality after SSRF. A reduction in the risk of pneumonia was observed among patients who underwent SSRF with ISS 15-19 [IRR (95% CI): 0.45 (0.22-0.90), P = 0.023]. Among patients with ISS 25-75, the reduction in the risk of pneumonia approached statistical significance [IRR (95% CI): 0.71 (0.50-1.01), P = 0.054]. SSRF was associated with a reduction in the risk of ARDS irrespective of the overall injury severity. The median length of mechanical ventilation was approximately a day shorter for those underwent SSRF with ISS 20-24 [change in median (95% CI): -0.95 (-1.38 to -0.52), P < 0.001] and ISS 25-75 [change in median (95% CI): -0.99 (-1.37 to -0.61), P < 0.001] (Table 4).
After propensity score matching, all the same associations were observed as in the previous analyses (Supplemental Table S17-S20). However, several additional statistically significant associations were also identified. After propensity score matching, a significant association between SSRF and a reduction in the rate of pneumonia was also identified in the complete cohort (Relative Risk: 0.52, P < 0.001), as well as among patients with ISS 20-24 (Relative Risk: 0.52, P < 0.001) and ISS 25-75 (Relative Risk: 0.65, P < 0.001) (Supplemental Table S17, S19, and S20). Among patients with ISS 15-19, there was also a significant association between SSRF and a reduction in the LMV in the highest quartile (P = 0.027), after propensity score matching (Supplemental Table S18).
Of note, in the analysis that included all patients, there remained a statistically significant difference in the rate of pneumothorax (84.5% vis 82.3%, P = 0.001) and advanced directives limiting care (0.8% vs 1.4%, P = 0.014) after propensity score matching (Supplemental Table S17). In the subgroup analysis of patients with ISS 15-19, there remained a statistically significant difference in the rate of flail chest (30.3% vs 33.3%, P = 0.015), after propensity score matching (Supplemental Table S18). Nevertheless, these differences were not judged to be clinically significant. There were no remaining imbalances after propensity score matching among the subgroups with ISS 20-24 and ISS 25-75 (Supplemental Table S19-20).
Discussion
In this large study of severe polytrauma patients, SSRF was shown to be associated with a reduction in the rate of mortality. Operative intervention was also associated with a reduction in the risk of ARDS in patients of all injury severities. Patients who underwent SSRF had increased rates of mechanical ventilation, but exhibited an overall shorter duration of mechanical ventilation compared to those managed conservatively. While severe polytrauma was once thought to be a contraindication to SSRF, these results suggest operative rib fixation could be an essential part of early management in severely injured, polytrauma patients.
Previous studies of SSRF have shown mixed outcomes when chest wall injury co-exists with other injuries. Our results are congruent with those of Becker et al who demonstrated significantly lower mortality in polytrauma patients after SSRF. 9 Additionally, after matched pair analysis, their study demonstrated shorter intubation duration, ICU LOS, and hospital LOS in the operative group. However, Becker et al included SSRF up to 3 weeks after the initial trauma, which could introduce confounding factors into respiratory and mortality outcomes. 9 The present study represents a larger population and excludes patients who underwent operative fixation beyond the recommended 72-hour window. Concurrent pulmonary contusion was initially thought to negate benefit from SSRF; however, a later study showed that patients with mild and moderate pulmonary contusion still experienced positive effects on ICU LOS and ventilator duration following operation. 12 There has also been concern that SSRF may increase rates of ARDS, especially with greater numbers of ribs involved, which would be especially detrimental in the polytrauma population. 13 However, the results presented here show SSRF decreased overall pulmonary complications including ARDS. Preventing pneumonia with adequate pulmonary hygiene is essential to improving outcomes.8,14 We suggest that early SSRF in this population may present a key opportunity for preventing this deleterious complication. This is congruent with a meta-analysis of SSRF outcomes which show decreased ICU LOS, ventilator duration, and pneumonia after SSRF. 15 Additionally, SSRF in polytrauma patients was shown to increase odds of discharge to home and decrease odds of lung-related readmissions within 1 year. 16 While we did not include this as an outcome, this is consistent with a previous study which suggested better neurologic outcomes in TBI patients with rib fractures who underwent SSRF. 7
Polytrauma is a complex disease and any intervention in the polytrauma patient must be carefully considered for its benefit. Complications after SSRF are relatively uncommon, and typically mortality is attributed to the initial thoracic injury rather than the operative procedure. 17 Early orthopedic fixation of long bone fractures in polytrauma patients is associated with a favorable impact on inflammation and overall cardiopulmonary function. 18 Given this, it may also be true that early fixation of rib fractures in this population is associated with improved end-organ function, although future studies are needed to assess this.
There are also special populations which may be affected differently by polytrauma, especially the elderly who have 3 times increased risk of death compared to their younger counterparts. 19 Older patients are also at high risk for incurring rib fractures and suffering pulmonary complications. 20 Concurrent extrathoracic injuries worsen these outcomes. 21 Further study on outcomes of SSRF by age group is needed, since the majority of patients in the current investigation were not geriatric.
This study has several limitations. Given its retrospective nature and database use, there is likely selection bias among patients who underwent SSRF based on institutional protocols or provider preference. TQIP also does not provide any hospital level identifiers; consequently, it was not possible to account for clustering in the analysis. Additionally, TQIP only records the total number of ventilator days per patient during the index hospitalization. It does not provide episode-level detail on re-intubations or whether ventilation ended because of death. However, patients undergoing SSRF had lower mortality yet still fewer ventilator days after adjustment, any bias from early death shortening ventilator time would therefore, if anything, bias against the observed association. This is a study of polytrauma patients, which has a varying definition in the literature. Here we use AIS ≥2 in two or more body regions; however, others exist that combine this definition with physiological parameters. 3 Applying a different definition of polytrauma could affect our results as these definitions differently define the population with the highest risk of mortality. Additional studies should be directed at better understanding the protocols driving SSRF in polytrauma patients and which polytrauma patients will most benefit from SSRF.
Surgical stabilization of rib fractures within 72 hours of admission was associated with lower rates of mortality and acute respiratory distress syndrome, along with shorter duration of mechanical ventilation, in severely injured polytrauma patients. A reduction in the rate of pneumonia was only observed among patients with ISS 15-19.
Supplemental Material
Supplemental material - Surgical Stabilization of Rib Fractures in Severe Polytrauma: A Potential Indication
Supplemental material for Surgical Stabilization of Rib Fractures in Severe Polytrauma: A Potential Indication by Mary Matecki, MD, Maximilian P Forssten, MD, Yang Cao, PhD, Babak Sarani, MD, and Shahin Mohseni, MD, PhD, FEBS (EmSurg), FACS in The American Surgeon™.
Footnotes
Ethical Considerations
Exemption was granted by the George Washington University Institutional Review Board.
Author Contributions
Conception and study design: BS and SM. Literature review: BS, SM, and MM. Data acquisition: BS, SM, YC, and MF. Data analysis and interpretation: MF, YC, and SM. Drafting of the manuscript: MM, MF, and SMJ. Critical revision: SM and BS.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
Data is available upon reasonable request.
Supplemental Material
Supplemental material is available online.
