Abstract
Background
The Brain Injuries in Greater East Texas (BIGTEX) criteria were developed to identify patients with mild traumatic brain injury (mTBI) who may be managed at Level IV trauma centers (L4TCs). This study compared outcomes of mTBI patients treated at a Level I trauma center (L1TC) vs affiliated L4TCs.
Methods
A 10-year retrospective review of mTBI admissions was performed. Patients were grouped by location: L1TC or L4TC. Adverse events included neurological deterioration, worsening CT scan, neurosurgical intervention, or death. At L4TCs, patients received routine emergency care with neurological assessments performed by trauma-trained staff. Decisions to transfer were made by the treating emergency physician, independently or in consultation with the affiliated L1TC, using established transfer pathways.
Results
Seventy-four patients were included: 63 treated at the L1TC and 11 at L4TCs. The L1TC group met BIGTEX criteria; several L4TC patients had minor deviations, including low-dose aspirin (n = 5), intraparenchymal hemorrhage 5-7 mm (n = 1), and subarachnoid hemorrhage (focal n = 1; diffuse n = 2). All presented with GCS 14-15, no intoxication, polytrauma, or skull fractures. All remained neurologically stable, with no neurosurgical interventions or deaths. L4TC patients had more CT scans (median 3 vs 2), slightly longer hospital stays (3 vs 2 days), shorter ICU stays (0 vs 2 days), and lower hospital charges ($30,236 vs $38,076).
Conclusion
Selected mTBI patients, including those with minor BIGTEX deviations, were managed at L4TCs without observed adverse outcomes. These findings support the feasibility of local management in carefully selected patients and warrant prospective validation in broader rural trauma populations.
Keywords
Key Takeaways
• Structured clinical criteria (BIGTEX) can guide local management of mTBI patients at rural hospitals, even with minor protocol deviations. • Real-world application of the BIGTEX criteria showed selected patients were managed without transfer to a level I trauma center, without observed adverse outcomes. • Early results support broader validation, and a prospective study is warranted to confirm safety and refine criteria for rural trauma systems.
Introduction
Traumatic brain injury (TBI) is a leading cause of morbidity and mortality worldwide. In 2021, an estimated 20.8 million new cases occurred globally, and nearly 38 million people were living with the long-term effects of TBI. 1 In the United States (U.S.), CDC data from the same year reported over 214 000 TBI-related hospitalizations and 69 000 TBI-related deaths, highlighting the substantial public health impact of this condition. 2 Studies have shown trauma patients treated in tertiary centers experience decreased mortality and improved functional outcomes, 3 which has led to the common practice of transferring most TBI patients to high-level trauma centers with neurosurgical capabilities regardless of injury severity. Mild TBI (mTBI) comprises the majority of TBI in the U.S., accounting for approximately 75% to 90% of all cases.4,5
The diagnostic criteria for mTBI, established by the American Congress of Rehabilitation Medicine utilizing updates by the WHO Collaborating Centre Task Force, are widely accepted. 6 These criteria define mTBI clinically by an initial Glasgow Coma Score (GCS) of 13 to 15, assessed 30 min after injury, with one or more of the following: (1) loss of consciousness <30 min, (2) post-traumatic amnesia <24 h, (3) altered mental state at the time of injury [confusion, disorientation, etc.], or (4) transient neurological deficit, including focal signs, epilepsy, or nonsurgical intracranial injury. Silverberg et al further clarified these criteria by emphasizing structured clinical assessment, considering confounding factors, and introducing a “suspected mTBI” category for cases with incomplete information. 6 This recommendation highlights the importance of objective cognitive, balance, and oculomotor assessments to support diagnosis. While these definitions incorporate a wide variety of presentations, they do not specify management strategies.
National data suggest approximately 3 million TBI-related emergency department (ED) visits occur annually in the U.S., with a growing burden among older adults, particularly for fall-related mTBI. 7 Bhogadi et al found that over one-third of TBI patients transferred to Level I or II trauma centers were discharged within 48 h without any neurosurgical intervention. 8 These findings suggest many transfers may be avoidable and underscore the need for better coordination and triage between lower-level hospitals and tertiary centers.
The BIGTEX Criteria

GCS, glasgow coma scale; SDH, subdural hematoma; EDH, epidural hematoma; IPH, intraparenchymal hematoma; SAH, subarachnoid hematoma.
aIsolated injuries only.
Here, we detail outcomes of mTBI patients managed at a rural L1TC and its affiliated L4TCs, with the aim of focusing on observed clinical outcomes and feasibility of local management, as well as economic implications of non-transfer under the BIGTEX methodology.
Setting and Methods
This retrospective study compares a L1TC mTBI group (2014-2021) with a L4TC mTBI group (2020-2023). Approval was received from the Institutional Review Board at the University of Texas at Tyler. Eligible patients were identified through review of the institutional trauma registry. The L1TC group includes the same single level fall patients described in Murry et al, A Criteria to Reduce Interhospital Transfer of Traumatic Brain Injuries in Greater East Texas. 10
Inclusion criteria for both groups were adults with isolated mTBI who met BIGTEX parameters or mTBI patients deemed low-risk for deterioration by the on-call emergency medical team, even when minor deviations from the BIGTEX criteria were present. These deviations reflect real-world application, where clinical decisions incorporate provider judgment, patient-specific factors, and local resource availability. Documented deviations included low-dose aspirin use (<81 mg), minor imaging variations, and, in one case, a fall from height. Exclusion criteria included polytrauma, penetrating injury, or immediate neurosurgical needs.
The L4TC group was identified through each affiliate trauma registry withing the UT Health East Texas system. All L4TCs have on-site CT imaging, 24/7 emergency department physician coverage, and established telemedicine links with the L1TC trauma team, ensuring immediate access to higher-level consultation when needed.
Only patients who were retained at their local hospital were included in the L4TC group. At the L4TCs, emergency physicians, who are all trauma certified with Advanced Trauma Life Support, determined whether to retain mTBI patients, either independently or after consultation with the on-call L1TC trauma surgeon. Nurses caring for trauma patients at both the L1TC and L4TC affiliates complete a trauma-focused certification training course and provide neurological assessments per the Trauma Nurse Core Course guidelines. 11 All facility protocols and policies are guided by the Texas Trauma Rules, 12 American College of Surgeons (ACS), 13 and Emergency Nurses Association. 14 No new neurological assessment tools or protocols were implemented during the study period. Retained patients received standard emergency care including a complete neurological assessment on arrival with oversight and support from the L1TC through routine communication and established transfer protocols. Any patient with worsening CT findings, neurological deterioration, or indications for neurosurgical intervention are transferred immediately to the L1TC for definitive care.
Data on demographic, clinical characteristics, and outcome variables were abstracted from electronic medical records. The primary outcome of interest was the absence of a critical event, defined as neurological deterioration, evidence of progression on follow-up CT imaging, neurosurgical intervention, or death. Secondary outcomes included number of CT scans, hospital length of stay (LOS), intensive care unit (ICU) LOS, discharge disposition, total hospital charges, and need for transfer from a L4TC to the L1TC. Continuous variables were reported as medians with interquartile ranges (IQRs) and categorical variables as counts and percentages. Given the small sample size and exploratory nature of the study, no formal hypothesis testing was performed. Hospital charges were adjusted to 2023 U.S. dollars using the Consumer Price Index for medical care as published by the Bureau of Labor Statistics. 15 Analyses were conducted using Stata version 16.1 (College Station, TX).
Results
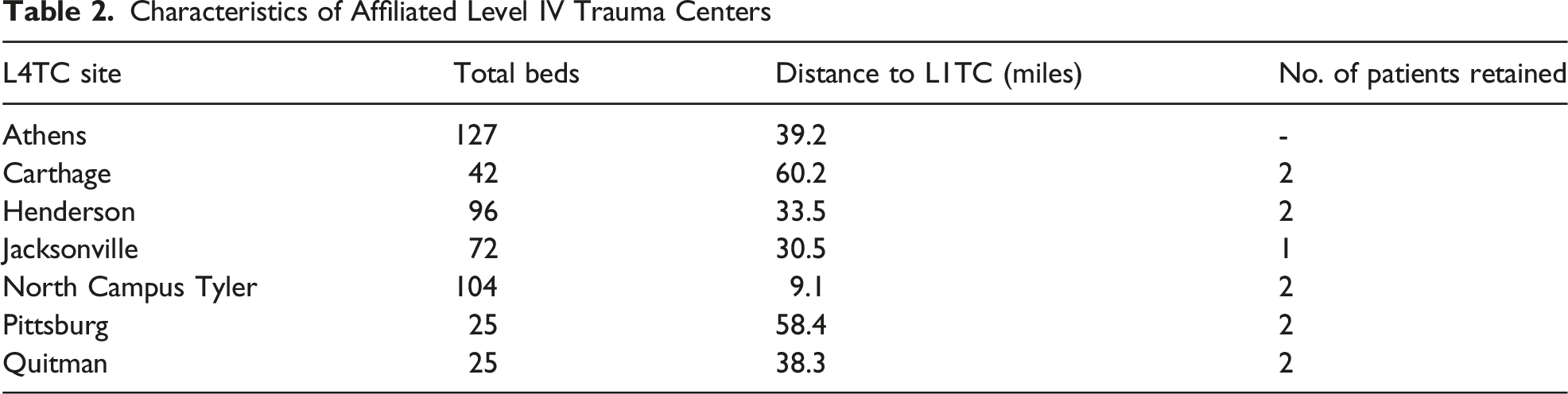
Characteristics of Affiliated Level IV Trauma Centers
Mild Traumatic Brain Injury Initial Presentation
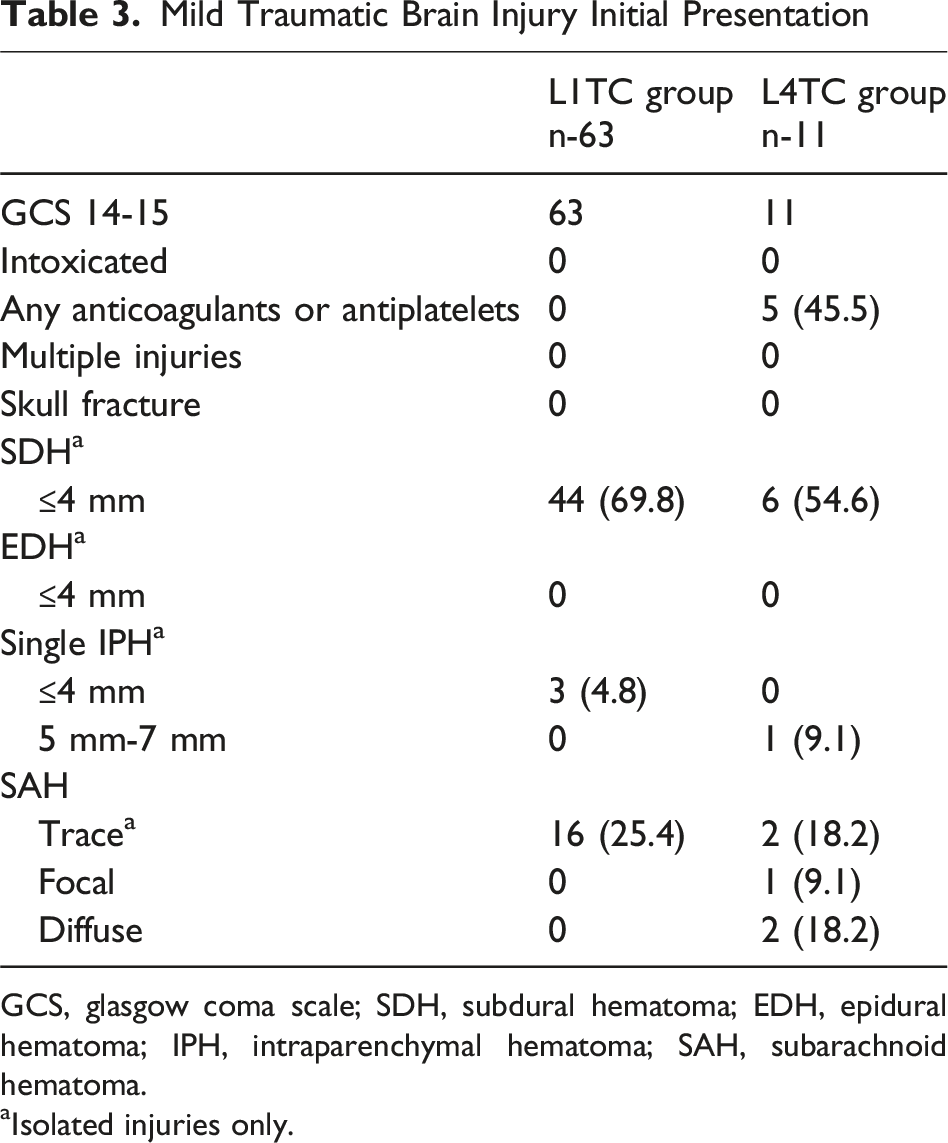
GCS, glasgow coma scale; SDH, subdural hematoma; EDH, epidural hematoma; IPH, intraparenchymal hematoma; SAH, subarachnoid hematoma.
aIsolated injuries only.
In contrast, several L4TC patients exhibited documented deviations from the BIGTEX criteria. Five patients were taking daily low-dose aspirin (<81 mg). Of these five, four also had imaging deviations: one had a 5.1 mm intraparenchymal hemorrhage, two had diffuse subarachnoid hemorrhage, and one had focal subarachnoid hemorrhage. One case was also retained following a fall from height. Despite these deviations, all L4TC patients remained hemodynamically stable, neurologically stable and were retained locally. In one case tele-neurology consultation supported non-transfer management.
Clinical Characteristics and Outcomes of Mild Traumatic Brain Injury Patients by Treatment Center Group
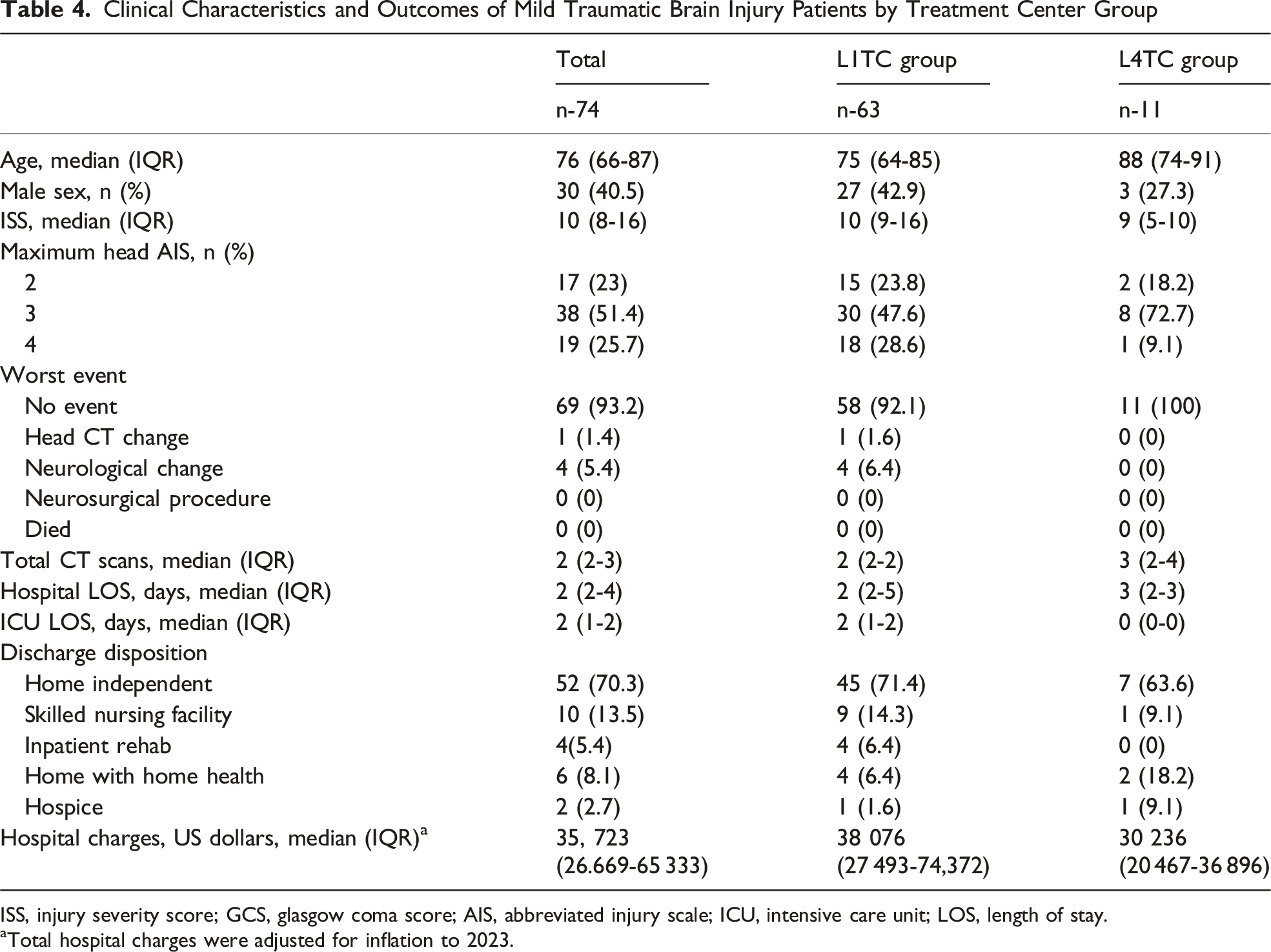
ISS, injury severity score; GCS, glasgow coma score; AIS, abbreviated injury scale; ICU, intensive care unit; LOS, length of stay.
aTotal hospital charges were adjusted for inflation to 2023.
Resource utilization differed modestly between groups. L4TC patients underwent more CT scans (median 3 vs 2), had slightly longer hospital stays (median 3 vs 2 days), and shorter ICU stays (median 0 vs 2 days). Discharge disposition was similar between groups. Most were discharged home independently (70.3%) or to a skilled nursing facility (13.5%). Median hospital charges were lower for L4TC patients ($30,236; IQR $20,467-36,896) compared with L1TC patients ($38,076; IQR $27,493-74,372).
Discussion
This report introduces the preliminary application of the BIGTEX criteria for managing select mTBI patients at L4TCs. No patients retained at a L4TC experienced observed neurological decline, injury progression, neurosurgical intervention, or death during the study period. Further, comparison of resource utilization suggested potential cost savings among mTBI patients cared for at a L4TC compared to the L1TC. Taken together, these early findings offer practical insight into how structured criteria can be applied in rural trauma systems support local retention of appropriate patients at L4TCs, while balancing resource limitations and provider judgment. Oversight from the L1TC trauma team was provided through routine case discussions, phone consultation, and telemedicine support, guiding retention decisions and facilitating rapid escalation when needed. An essential component of this approach is an established institutional agreement whereby any L4TC patient demonstrating neurological deterioration or requiring neurosurgical intervention is transferred promptly to the affiliated L1TC, ensuring access to higher-level care when indicated.
Trauma system development has shown structured networks improve coordination, resource use, and patient outcomes across regions. The ACS Verification, Review, and Consultation program outlines that L1TCs are responsible for providing clinical oversight, education, and performance improvement support for affiliated lower-level centers and L4TCs focus on initial evaluation, stabilization, and timely transfer when indicated. 16 A statewide analysis has demonstrated adoption of ACS verification standards is associated with reduced variability in care and improved morbidity and mortality across trauma systems. 17 Comparisons among ACS-verified Level I/II trauma centers further indicate high-performing verified centers have significantly fewer complications and better adherence to quality benchmarks. 18 Rural trauma literature further highlight ongoing challenges with under triage of severely injured, limited imaging capacity, staffing constraints, and long transfer distances that increase reliance on standardized protocols and telemedicine support from tertiary centers.19-21 These findings are consistent with the design of our regional network and demonstrate the value of integrating L1TC and L4TC care.
Importantly, several patients managed at L4TCs did not meet all of the elements of the BIGTEX criteria, some were on low-dose aspirin, others had hemorrhage dimensions or imaging descriptors outside protocol thresholds, and one had a fall from height. Despite these deviations, all patients remained clinically stable under observation. These cases illustrate how clinical practice evolves beyond rigid protocols, relying instead on real-time judgment, collaborative consultation, and a broader understanding of patient safety within the trauma system. Deviations from the BIGTEX criteria were not exceptions but part of the adaptive process, reflecting how practice-changing guidelines are implemented across diverse clinical settings. These early experiences demonstrate how structured criteria may be flexibly applied in rural systems to support patient retention without observed adverse outcomes.
Resource utilization differed modestly between groups. L4TC patients underwent more imaging and had slightly longer hospital stays, yet incurred lower overall hospital charges, likely due to reduced transfer costs and avoidance of higher-acuity resource use. These findings align with broader concerns about over-triage, which has been shown to contribute to resource misallocation and increased financial burden within trauma systems.22-24 Over-triage also contributes to overcrowding and strain on tertiary trauma centers, further impacting system performance.25,26
A balanced trauma system depends on appropriate triage. Evidence supports a volume-outcome relationship where higher volume trauma centers tend to achieve better outcomes for severely injured patients and lower volume centers tend towards worse outcomes. 27 Registry and cohort studies show critically injured or hemodynamically unstable patients benefit most from treatment at high-volume centers.28,29 In contrast, lower-level trauma centers play a crucial role in managing less severe injuries without compromising patient outcomes. 30 Strengthening L4TCs through infrastructure, training, and telemedicine for neurosurgery and radiology can reduce unnecessary transfers, improve access to definitive care in rural settings, and reserve high-acuity resources for those who need them most. This approach ensures trauma patients receive care appropriate to their injury while maintaining the readiness of L1TCs for the most complex cases.
Recent rural trauma research suggests physiologic severity, rather than transport time alone, is the primary driver of mortality with prolonged transport durations. 31 National recommendations emphasize building regional trauma systems with local stabilization units to ensure early resuscitation and reduce adverse outcomes, particularly in rural regions. 32 Persistent gaps have been documented in clinical information during inter-facility transfers: transferred patients often arrive with incomplete or inaccurate data; however, structured health-information exchange interventions have been shown to reduce these safety risks.33,34 Applying mTBI criteria to guide local retention while strengthening communication pathways may help reduce unnecessary transfers and support timely escalation for patients who deteriorate.
A recent study comparing patient satisfaction in rural vs urban hospitals in the U.S. found rural hospitals consistently scored higher across various hospital determinants, including cleanliness, nurse and doctor communication, staff responsiveness, and overall hospital rating. 35 While specific factors, such as family support and familiarity with local health care providers, are not well studied, these early findings suggest local care should be prioritized when clinically appropriate and supported by system-level safeguards. This approach is particularly relevant for managing patients with mTBI, as local hospitals can offer quality care while maintaining safety standards.
Patient safety must remain a top priority when implementing practice-changing interventions such as the BIGTEX criteria, particularly in rural hospitals where resource shortages and limited staffing may constrain regular monitoring and delay recognition or response to patient deterioration. While this report does not establish safety, prior validation of BIG criteria 36 along with our previous retrospective study 10 together with this preliminary report suggest the BIGTEX criteria may be feasibly applied within other trauma systems with affiliated L4TC networks.
Limitations
The small sample size, particularly in the L4TC group and single-center center design may limit generalizability. The inclusion of patients with documented deviations from the BIGTEX criteria also limits direct comparability to the original guideline thresholds. Although hospital charges were adjusted to 2023 U.S. dollars, meaningful cost comparisons are limited by the long study timeframe, changes in practice patterns, and differences in resource utilization between groups, cost findings should be interpreted as descriptive and preliminary. Further, the majority of patients in both groups had a subdural hematoma or a subarachnoid hematoma, with no epidural hematomas and only three intraparenchymal hematoma cases, which limits generalizability to other patterns of intracranial injury.
Conclusion
Selected mTBI patients, including those with documented deviations from the BIGTEX criteria, were retained and managed at rural L4TCs with oversight from L1TC trauma staff. Retention decisions were supported by established transfer agreements allowing prompt escalation to the L1TC in the event of neurological deterioration or need for neurosurgical intervention. These early findings highlight the value of structured triage, clinical judgment, and collaborative decision-making within rural trauma systems. Broader adoption and refinement of this approach may reduce unnecessary transfers, optimize resource utilization, and expand access to cost-effective care in underserved regions. Prospective validation across diverse rural populations is warranted.
Footnotes
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
