Abstract
Background
Enhanced recovery pathways (ERP) have been shown to decrease length of stay and opioid utilization for pediatric patients undergoing colorectal surgery without compromising outcomes. However, the cost benefits of ERP implementation have not been quantified. We sought to describe, for the first time, the resulting fiscal benefits of ERP implementation at a single-center academic hospital, aiming to highlight the financial benefits to hospitals and payers of ERP utilization.
Methods
We conducted a single-institution retrospective cohort study of patients aged 2-18 who underwent planned colorectal surgery before and after our institution implemented a colorectal ERP. Our primary outcome was total hospital admission costs based on hospital length of stay, narcotic use, crystalloid infusion, and multimodal pain medication use. We sourced our cost data from peer-reviewed literature and publicly available cost data. To account for potential confounding, we created a multivariable Gamma regression for cost using the Akaike Information Criterion selection method.
Results
Our retrospective review identified 345 eligible patients who underwent planned colorectal surgery between 2014 and 2024, with a median cost savings of $5689 per case. After adjusting for cofounders and employing our AIC model selection, we found that ERP implementation was associated with an overall 9% reduction in total admission costs compared to patients managed before the ERP (IRR 0.91, 95% CI 0.84-0.99, P = 0.038).
Conclusions
This is the first study to quantify cost savings after ERP implementation for pediatric colorectal surgery, and savings are independently associated with pathway exposure. To determine whether these single-institution savings are generalizable to other children’s hospitals a formal additional ERP data from other institutions and a formal cost-effectiveness analysis are needed.
Key Takeaways
• Enhanced recovery pathways for pediatric patients undergoing planned colorectal surgery are associated with reduced admission costs.
• The reduced costs do not sacrifice good outcomes for this patient population.
Introduction
Enhanced recovery pathways (ERPs) have gained in popularity for pediatric colorectal surgery.1,2 Multiple prior studies, including those from our institution, have demonstrated that ERPs are associated with reduced hospital length of stay (LOS), shorter time to solid oral intake, and decreased opioid usage without compromising patient outcomes in pediatric colorectal surgery.3-6 While utilization metrics such as LOS, Foley catheter usage, and intravenous fluid (IVF) infusions are potential surrogates for assessing costs in the US, direct cost comparisons of ERP and non-ERP patients have been limited to small retrospective cohorts in China thus far.4,5,7 Prior cost analyses of ERPs after planned surgery are limited to adult populations, whereby perioperative recovery experiences, psychosocial factors, and resource utilization may differ significantly from those of pediatric patients.8-20
Despite these benefits to clinical outcomes in children, and financial benefits for adults, ERP implementation in children has lagged by decades. This is due to the heterogeneity of pediatric patient populations and the relative paucity of cases meeting criteria for ERP utilization in children. Additionally, institutional resources which facilitate ERP development and implementation are also lacking. To understand the financial impacts of ERP implementation, we sought to quantify the cost savings to the institution, and thus the payer, of ERP exposure. This has not previously been performed. We hypothesized that after controlling for pertinent covariates cost reduction after ERP implementation for pediatric patients undergoing colorectal surgery would be independently associated with pathway participation.
Methods
Study Design, Setting, and Participants
We performed a retrospective analysis of a single-institution cohort of patients before and after formally implementing an ERP specific to planned (ie, non-emergent) pediatric colorectal surgeries. Eligible patients were aged 2-18 years and underwent colorectal surgery at a single academic children’s hospital between 2014 and 2024. We excluded patients undergoing emergent surgery. Our ERP protocol and included Current Procedural Terminology (CPT) procedure codes are described in detail in a previous publication (Appendixes A and B). 3
Outcomes
Our primary outcome of interest was total hospital admission costs based on total hospital length of stay (LOS), narcotic use in morphine milligram equivalents (MME), total crystalloid volume infused, and multimodal pain medication dosages (acetaminophen, celecoxib, and gabapentin). We determined the costs based on these parameters, as they could be directly attributed to our ERP.3,21 Our secondary outcomes were preoperative, intraoperative, post-anesthesia care unit (PACU), and postoperative costs.
Exposures and Confounders
Our exposure and predictor of interest was whether a patient was assigned to an ERP for their non-emergent colorectal surgery. Patients who underwent surgery before January 1, 2016, were classified as pre-ERP, while those who underwent surgery after this date were classified as ERP. We identified the following confounders a priori: age, sex, body mass index (BMI), American Society of Anesthesiologists (ASA) health status classification, preoperative diagnosis, and whether a minimally invasive surgery (MIS) was performed. We sourced cost data from published price reports and peer-reviewed literature indexed in PubMed (Appendix A). Because hospital charges can be impacted by differences in health care costs over a study period and external factors such as payer mix, vendor contracts, quality improvement efforts like opioid stewardship and others, we used standardized cost estimates from validated resources normalized to a single year. Institutional charges, even controlled for inflation, would not account for these factors, so costing estimates were used. All other clinical data were sourced from our institution’s electronic medical record under approval from our institutional review board.
Statistical Analysis
Summary and Univariable Comparison of Baseline Health Status Between Pre-enhanced Recovery (Pre-ERP) and Enhanced Recovery Pathway (ERP) Cohorts
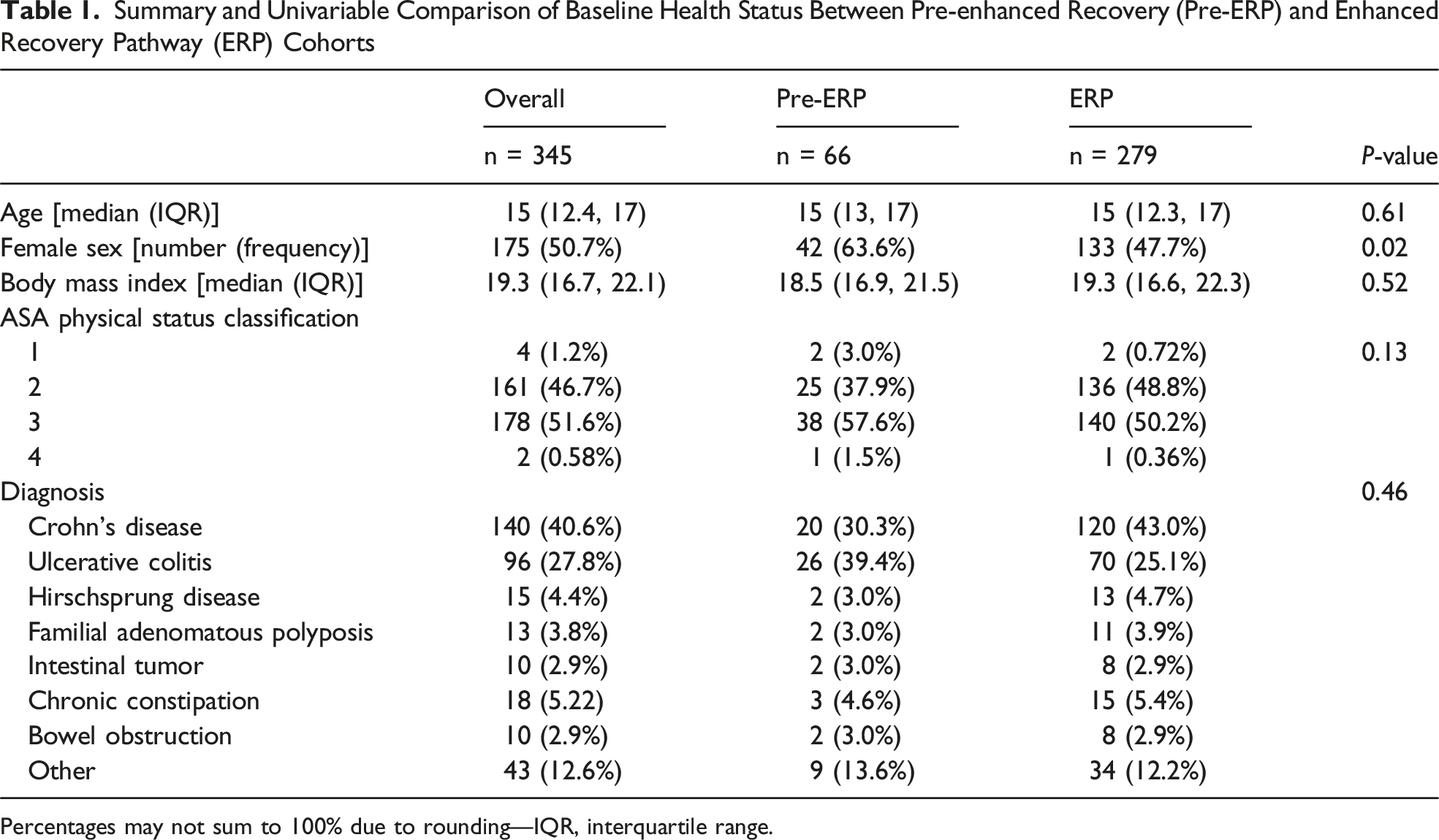
Percentages may not sum to 100% due to rounding—IQR, interquartile range.
Summary and Univariable Comparison of Perioperative Characteristics Between Pre-enhanced Recovery (Pre-ERP) and Enhanced Recovery Pathway (ERP) Cohorts
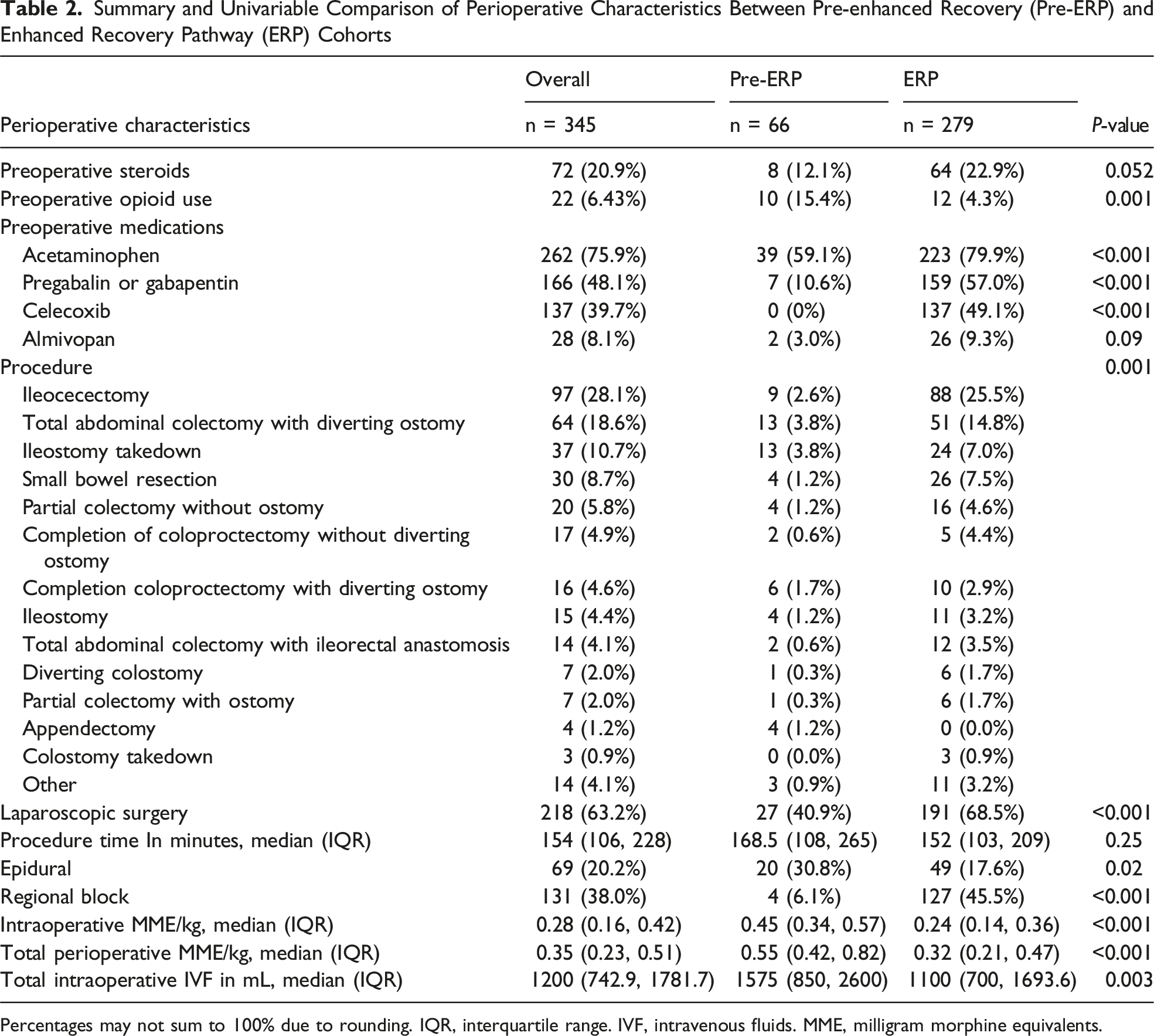
Percentages may not sum to 100% due to rounding. IQR, interquartile range. IVF, intravenous fluids. MME, milligram morphine equivalents.
Unadjusted Comparisons of Median Costs Across Different Phases of Care and in the Entire Admission, Stratified by ERP Status
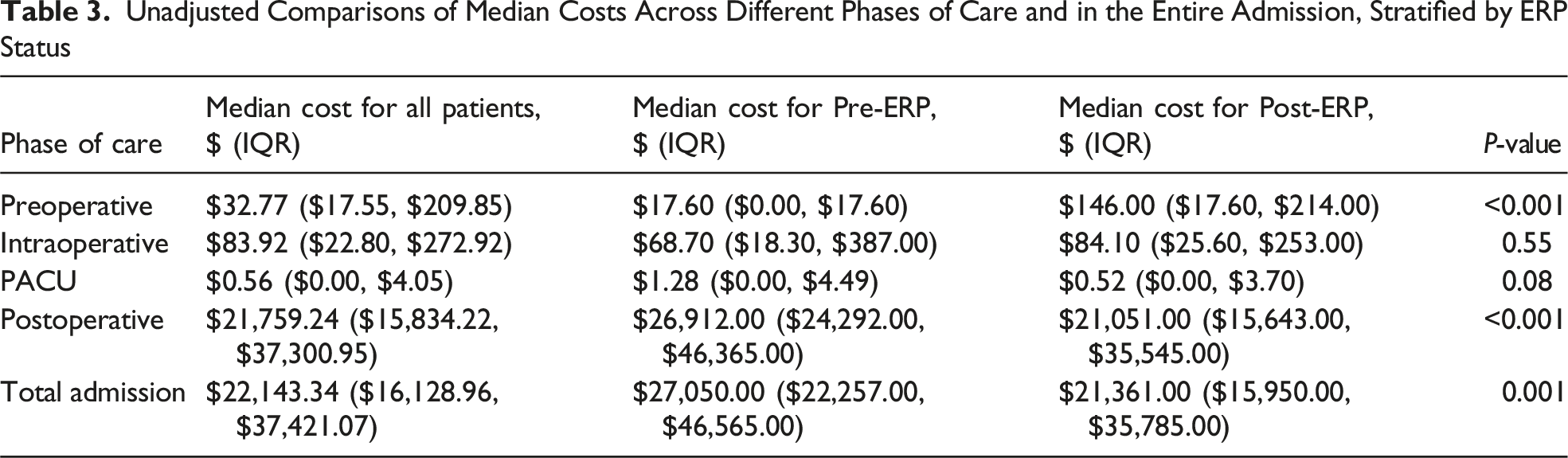
Human Participants
The University of North Carolina at Chapel Hill Institutional Review Board approved this study with a waiver of informed consent.
Results
Baseline Demographics
Retrospective chart review yielded 345 eligible patients who underwent non-emergent colorectal surgery at our tertiary children’s hospital between 2014 and 2024. The cohort’s median age was 15.0 years (IQR 12.4, 17.0) years, 50.7% of the cohort were reported as female, and the median BMI was 19.3 (IQR 16.7, 22.1) kg/m2. Most patients (80.9%, n = 279) in our cohort were in the post-ERP group, while the remainder were in the pre-ERP group. A summary of unadjusted comparisons of baseline, perioperative, and postoperative characteristics of our cohort, stratified along ERP status, is provided in Tables 1 and 2
Cost Analysis
Significant Predictors of Cost in Our Cohort in Our Multivariable Model. Model Selection was Employed Using AIC

Initial predictors entered into the model included reported sex, ASA class, MIS, preoperative diagnosis, and hospital length of stay.
Discussion
This is the first study to quantify cost savings associated with ERP implementation in pediatric colorectal surgery. We found that ERP utilization was independently associated with a 9% reduction in costs per case, even when controlling for LOS. These savings occur without sacrificing the quality of care for pediatric colorectal surgery.3,23 These findings are consistent with larger studies in adult ERP implementations, and follow logically from previously published reductions in LOS observed at our institution and others.3,23 However, this quantification is novel and allows surgeons, hospitals, and payers to estimate the impact of ERP implementation, which may assist in decision-making regarding resource allocation and patient referral patterns.
Our findings corroborate those of a meta-analysis published in China in 2023, which concluded that ERP implementation was associated with significantly lower costs in 3 retrospective studies focused on pediatric patients undergoing colorectal surgery in China. 5 While important context, the US health care environment is quite different from the Chinese system; thus, US studies specific to pediatric colorectal patients are necessary to accurately estimate the cost savings of ERP utilization.24-29 Due to these inherent differences, direct cost comparisons between US and Chinese colorectal experiences are difficult. However, our study still found median per-case savings of over $5000 and a 9% risk-adjusted reduction in overall admission costs in a busy US setting within a much more heterogeneous US payer landscape (compared to cost reductions ranging from $284.42 to $466.16 after conversion in a single-payer Chinese system). 5 This suggests that ERP is consistently associated with reduced resource utilization and costs across different health system models, even if the magnitude of savings may differ. Notably, our findings suggest that the ERP is more impactful in health systems with high baseline costs, such as ours.
Compared to adult studies, our results are notably consistent in both the direction and magnitude of cost savings. The adult literature surrounding ERP cost savings in adult populations who underwent colorectal and other major abdominal surgeries also reported savings per case ranging from $3000 to $7,000, similar to our single-institution finding.15,16,18-20 These similarities suggest that despite physiologic and psychosocial differences between adult and pediatric populations, ERPs can translate into meaningful cost reductions across different demographic groups. While we previously showed that ERPs are associated with reduced LOS in our cohort, the 9% cost reduction that we observed after ERP implementation was independent of hospital LOS. This suggests that the standardized practices introduced by our ERP are independently associated with this cost reduction. When considered in conjunction with adult ERP experiences, our findings underscore the generalizability of ERP and further highlight the need to continue ERP adoption in pediatric surgical specialties. Our ERP protocol, shown in Appendix B, can also serve as a practical blueprint in pediatric colorectal services seeking to implement their own ERPs. While ERPs and their benefits are well-established in the adult literature, studies examining the cost impacts of pediatric ERPs remain sparse, and we hope that our work helps drive continued implementation of similar protocols in North America.
We acknowledge some limitations in our study. First, the retrospective nature of our research is susceptible to reporting bias and the impacts of missing data. We found that fewer than 1% of patients in our cohort had missing data, and thus decided that a complete case analysis of our outcomes was appropriate. Additionally, retrospective data may be biased by several factors; however, given the proven benefits of adult ERPs and the emerging evidence for the efficacy of ERPs in children, a prospective randomized study lacks equipoise. Therefore, we believe that retrospective studies of this nature represent the best available data. To control for potential confounding, we employed a predetermined set of potential confounders and a validated model selection method. This lack of equipoise also means we cannot infer causation from this study due to its retrospective nature. Finally, during the study period, actual health care costs may have varied widely due to payer negotiations, the presence or absence of Medicaid expansion, payer mix, and other factors. Because of this, we used standardized costing data; however, note that this approach may lead to bias in various ways.30,31
Despite these limitations, performing such a cost analysis remains essential. We also proffer that our methodology can be applied by individual institutions seeking to evaluate their ERP protocols in similar settings and patient populations. Future efforts should encourage multicenter pediatric collaborations to assess the reproducibility of these cost savings for pediatric ERPs. Doing so is key to improving the implementation and improvement of pediatric ERPs for planned colorectal surgery to achieve the benefits seen in adult populations.
Conclusions
Implementing an ERP at our tertiary children’s hospital for pediatric patients undergoing planned colorectal surgery was associated with significantly reduced costs. This longitudinal cost analysis demonstrates ERPs present an opportunity to improve the value of pediatric surgical care by decreasing costs while maintaining quality, and that these savings can be used to advocate for resources necessary to support and implementation ERPs in pediatric surgery more broadly.
Supplemental Material
Supplemental Material - Quantification of Cost Savings After Enhanced Recovery Pathway Implementation for Pediatric Colorectal Surgery
Supplemental Material for Quantification of Cost Savings After Enhanced Recovery Pathway Implementation for Pediatric Colorectal Surgery by William Luo, Nicole Buddenbaum, Priya Vasan, Ursula Adams, Adesola Akinkuotu, Robin Koonce, Concetta Lupa, Sean Mclean, Lisa Tracy, and Michael Phillips in The American Surgeon™
Supplemental Material
Supplemental Material - Quantification of Cost Savings After Enhanced Recovery Pathway Implementation for Pediatric Colorectal Surgery
Supplemental Material for Quantification of Cost Savings After Enhanced Recovery Pathway Implementation for Pediatric Colorectal Surgery by William Luo, Nicole Buddenbaum, Priya Vasan, Ursula Adams, Adesola Akinkuotu, Robin Koonce, Concetta Lupa, Sean Mclean, Lisa Tracy, Michael Phillips in The American Surgeon™
Footnotes
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
