Abstract
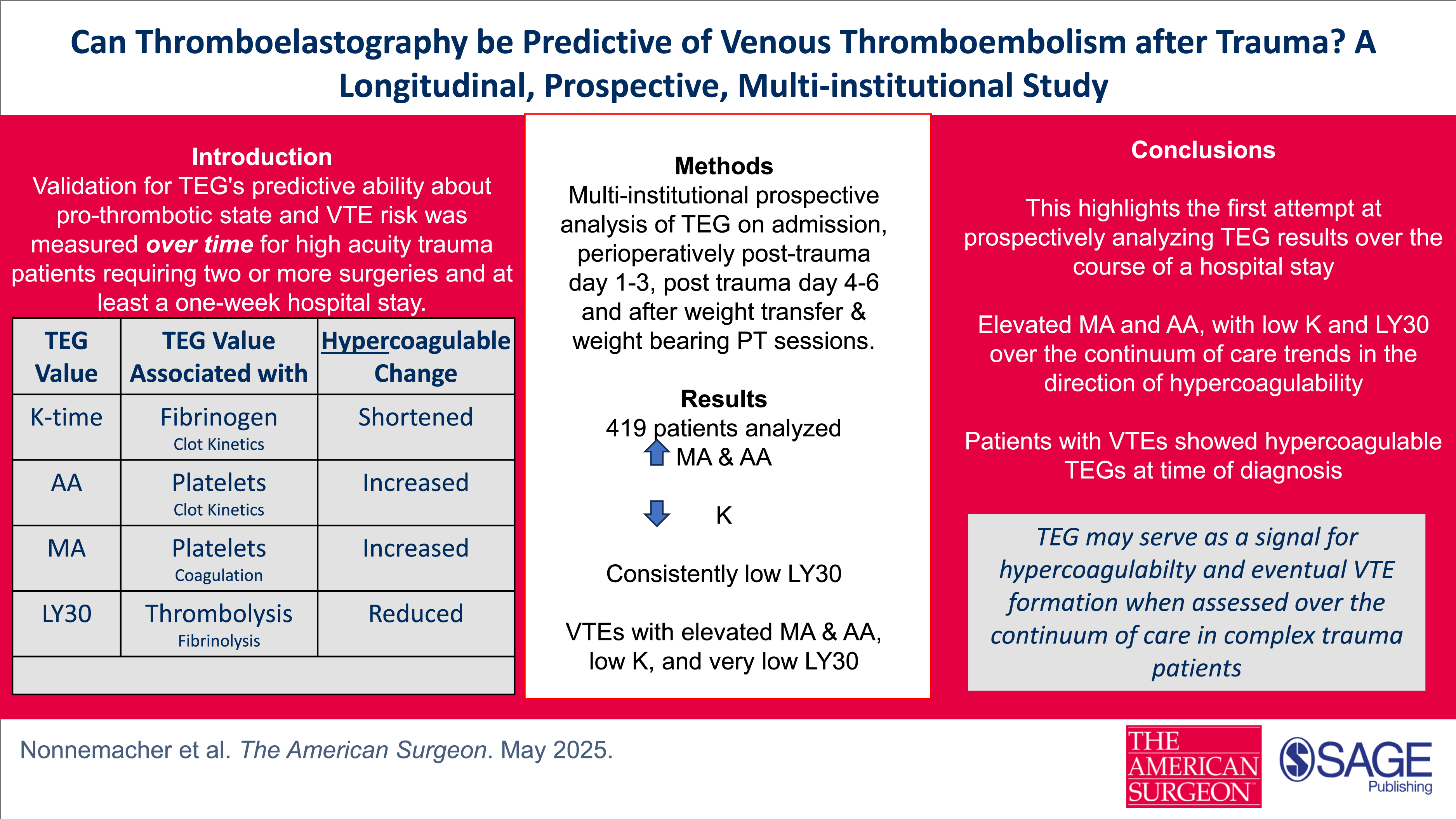
TEG has shown effectiveness in identification and management of coagulopathies. The role of TEG in hypercoagulability is increasing but remains unclear. We look to assess how TEG parameters vary in high risk trauma patients across their hospital stay. Methods A longitudinal prospective multi-institutional study was performed from September 2020 to June 2022. TEGs were collected on admission, in peri-operative periods and after physical therapy sessions and all TEG parameters were assessed for changes. Results 419 patients on admission were included for analysis. Alpha angle and Maximum amplitude trended upward throughout the continuum of care, while K-time was shortened and LY30 remained on the low end of the normal range. 21 patients developed a VTE during the study period with elevated MA, AA and low K and LY30. Conclusion This study suggests a potential TEG parameter signal in VTE formation, specifically increases in MA and AA with decreases in K and a consistently depressed LY30 in high-risk patients over a continuum of a hospital stay after traumatic injury.
Keywords
Background
Venous thromboembolism (VTE) is a major source of potentially preventable morbidity and mortality in trauma patients. Deep venous thrombosis (DVT) is estimated to occur in up to 60% of trauma patients and 13%-31% of patients in intensive care settings with pulmonary embolism occurring in 2%-22% of trauma patients.1-3 The costs associated with the VTEs are high and VTE incidences are a measurable quality metric that hospitals use for improvement. VTE after trauma can occur in patients at low or high risk despite VTE chemoprophylaxis. 1 Modern coagulation assessments do not provide predictive likelihoods for VTE development.
Thromboelastography (TEG) is commonly applied in the management of complex medical and surgical patients to monitor and treat coagulopathies. While more often used to evaluate the coagulation profile of bleeding patients, TEG as a modality for comprehensive thrombostatic function is purported to allow for the identification of hypercoagulable states. A knowledge gap exists as to whether a change in TEG pattern can identify a heightened risk for VTE development or predict VTE occurrence outright. Up to this point, most research related to TEG’s prothrombotic assessment potential has focused on isolated TEG data, usually on admission or at a time when a patient was experiencing a bleeding or clotting event.4-6 While TEG has been studied in the trauma population, predictive correlations for TEG and VTEs are weak, and no studies have evaluated TEG pattern changes over a continuum of care.
TEG parameters result in five lab values. R-time measures the time to initial fibrin formation and relates to coagulation factor quantity and quality. K-time and alpha angle measure the speed of clot formation and relate to fibrinogen function. Maximum amplitude measures the total strength of a clot and Lysis at 30 minutes (LY30) assesses the rate of fibrinolysis. 7
The purpose of the study is to assess whether trends in TEG parameters can be identified over time in the at-risk trauma population, serving as a signal for VTE risk escalation. We hypothesize that trauma patients will demonstrate a prothrombotic change in TEG parameters over their continuum of care, signaling increased risk for VTE development.
Methods
We performed a prospective, observational study at participating Level I Trauma Centers in the state of Georgia from September 2020 to June 2022. Institutional Review Board approval was obtained. Patients were included for study if they were multi-trauma patients admitted to an intensive care unit setting or patients identified as having severe injuries, requiring two or more surgeries, and a 1-week hospital stay anticipated. Patients where anticoagulation reversal was required on admission and patients with a positive coronavirus infection were excluded. Demographic data, Injury Severity Scores (ISS), mechanism of injury, patient comorbidities, body mass index, pre-injury anticoagulation and indication, as well as medication type were identified. DVT chemoprophylaxis was administered to all patients with institution-specific protocols, with most patients receiving low-molecular-weight heparin with the exclusion of those with renal disease. Anticoagulation was titrated based on trending anti-Xa levels. VTE events occurring within the study population were analyzed. Patients were categorized into four groups based on their ISS assignments; ISS 0-17, 18-22, 23-29, 30+. The TEG data accumulated over time were collected and analyzed. TEGs were drawn on admission, in the perioperative period from post-trauma day one to three, post-trauma day four to six and across three physical therapy sessions. Physical therapy sessions were performed while inpatient and generally occurred every other day. Patterns in TEG parameter changes were analyzed over this timeline. All values were compared to normal TEG parameters: R time 5-10 minutes, K-time 1-3 minutes, Alpha Angle (AA) 53-72°, Maximum Amplitude (MA) 50-70 mm, and Lysis at 30 minutes (LY30) 0%-8%. 8
A linear mixed model with all TEG parameters, R, K, AA, MA and LY30, was constructed. Significance was defined at a P-value of <0.05. The maximum likelihood estimate method was used and pairwise t-tests were performed and pairwise comparisons were conducted when fixed effects were significant to determine differences among categories. Statistics were conducted in R 4.3.1 using Imer, ImerTest and multcomp (R Core Team, Vienna, Austria).
Results
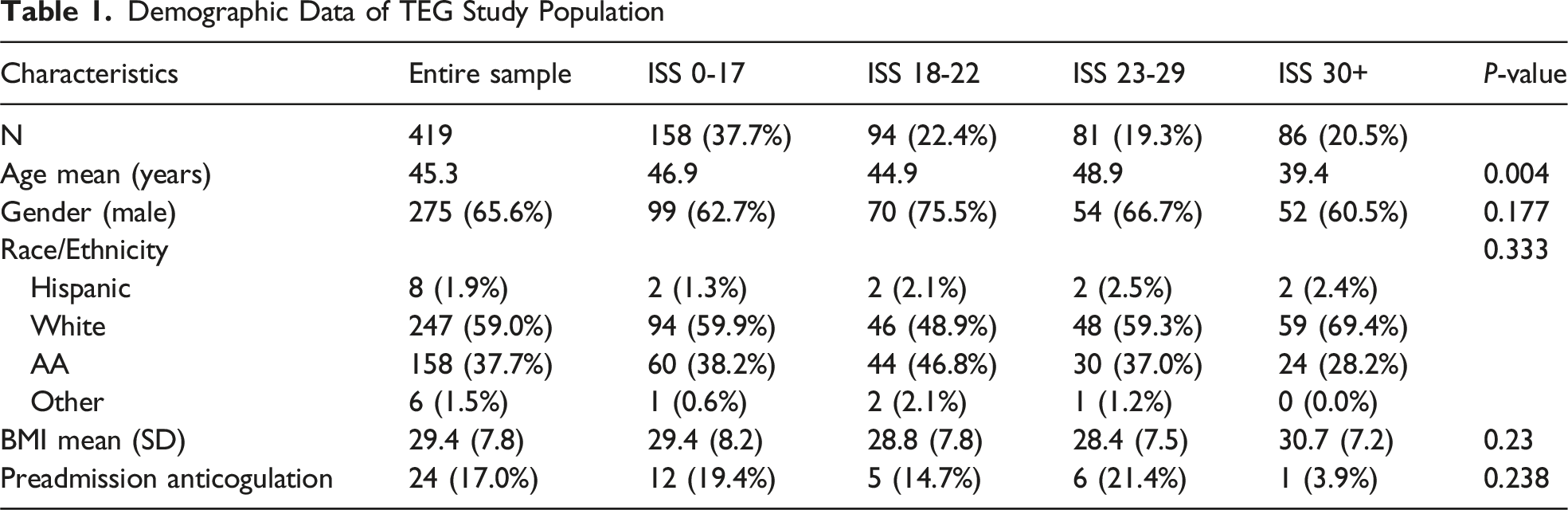
Four hundred nineteen (419) patients were included for analysis (Figure 1). 364 patients sustained blunt injuries and 55 patients sustained penetrating injuries. 158 patients were grouped into an ISS category of 0-17, 94 patients in an ISS category of 18-22, 81 patients in an ISS category of 23-29 and 86 in an ISS category of 30+. 65% of the patients were males, and males predominated all ISS groupings. Ethnicity, BMI and pre-injury anticoagulation were recorded. No statistical differences were encountered across the ISS groupings for these patient characteristics (Table 1). Patient comorbidities showed no statistical difference across ISS groups. STROBE Flow Diagram TEG Predictive Value Demographic Data of TEG Study Population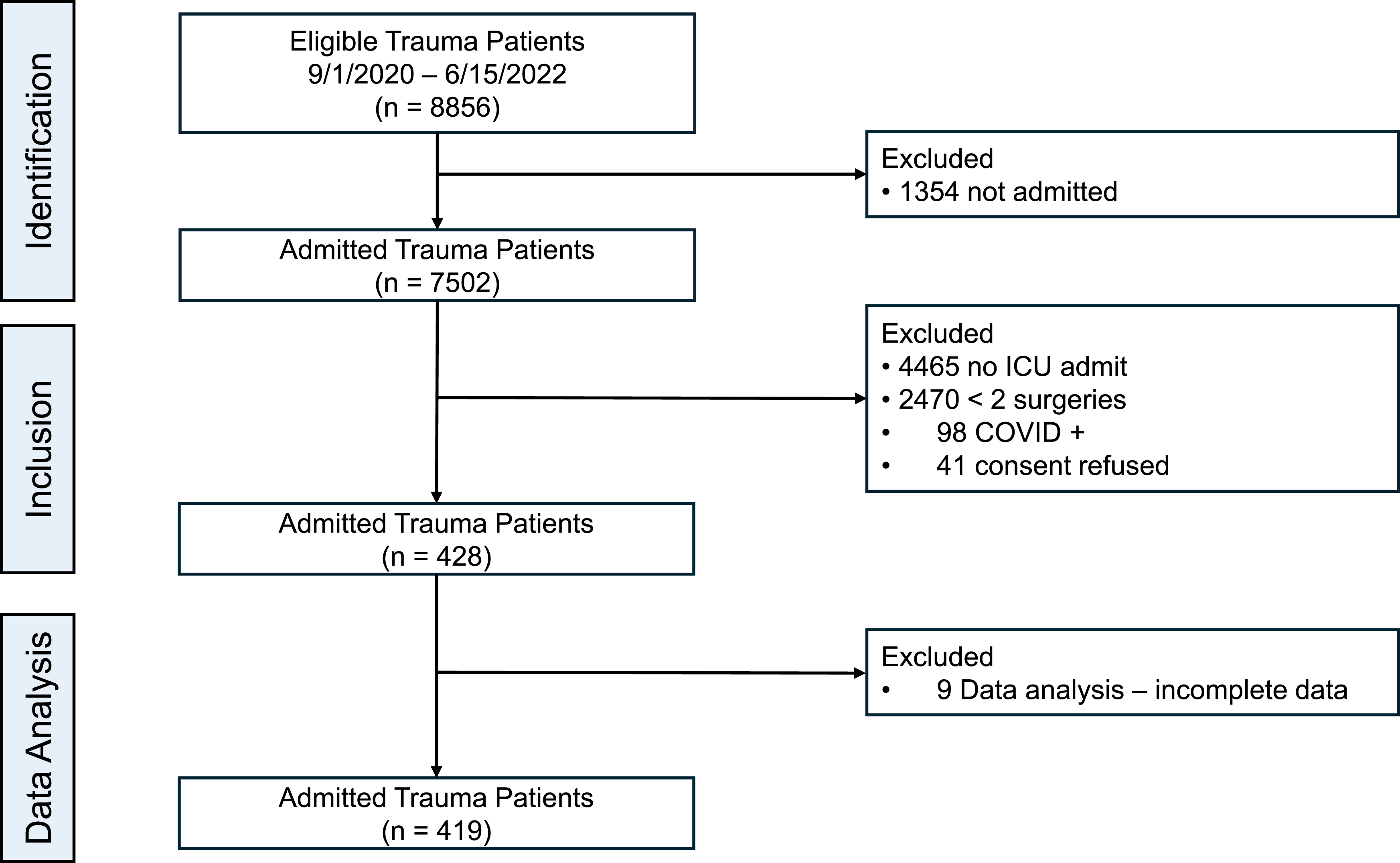
Admission TEG Values Compared Across ISS Groupings
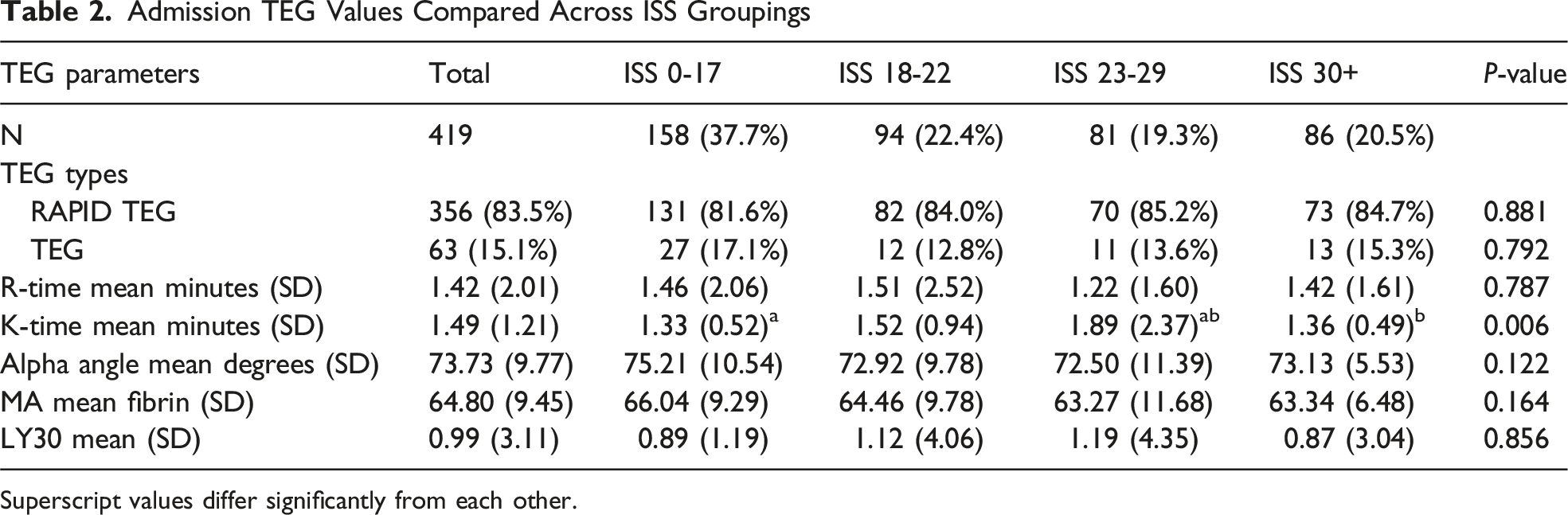
Superscript values differ significantly from each other.
First Perioperative TEG Values Compared Across Operative Groupings
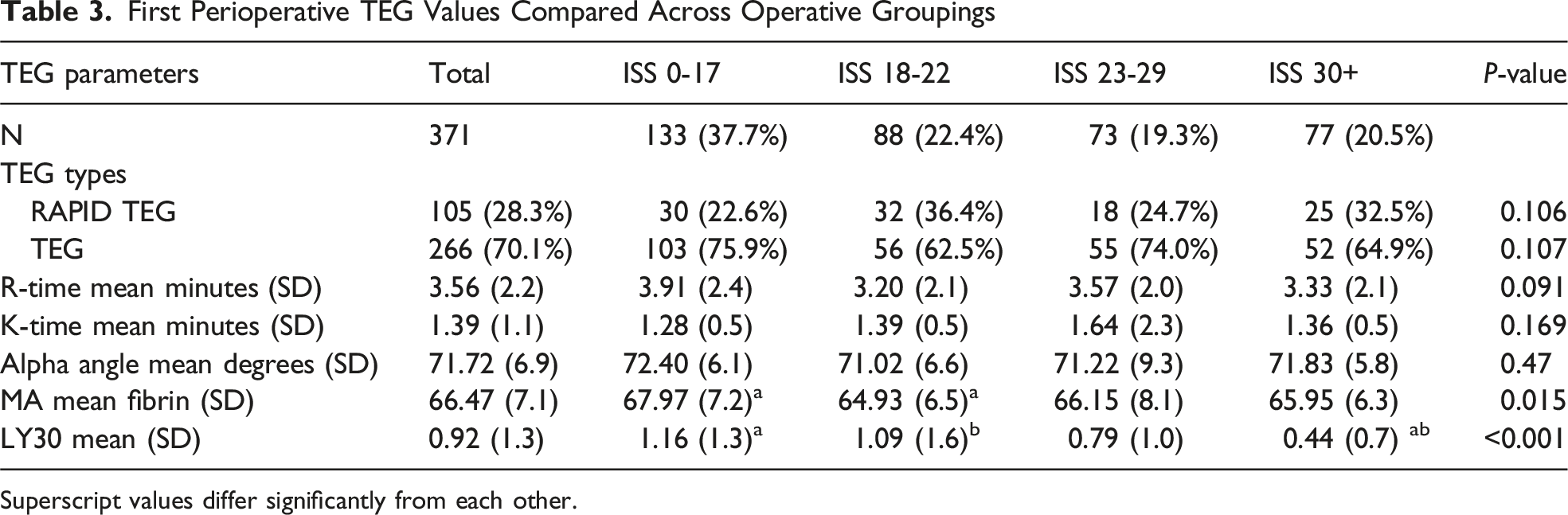
Superscript values differ significantly from each other.
Second Perioperative TEG Values Compared Across Operative Groupings
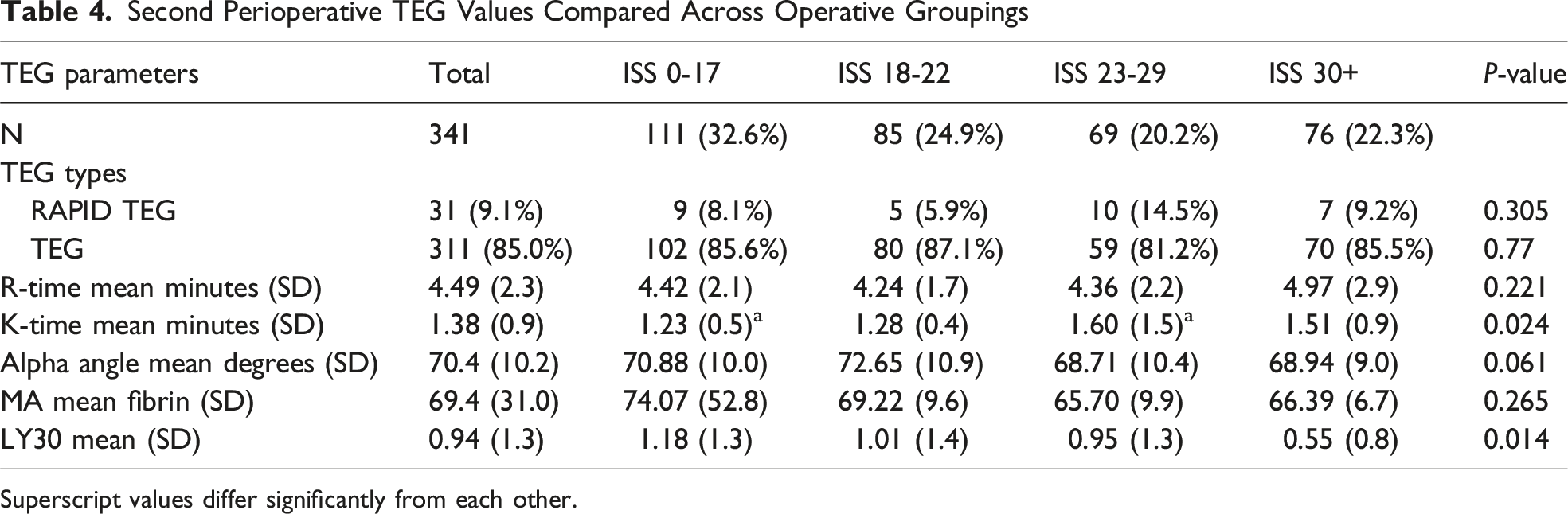
Superscript values differ significantly from each other.
Physical Therapy TEG Values Compared Across Sessions
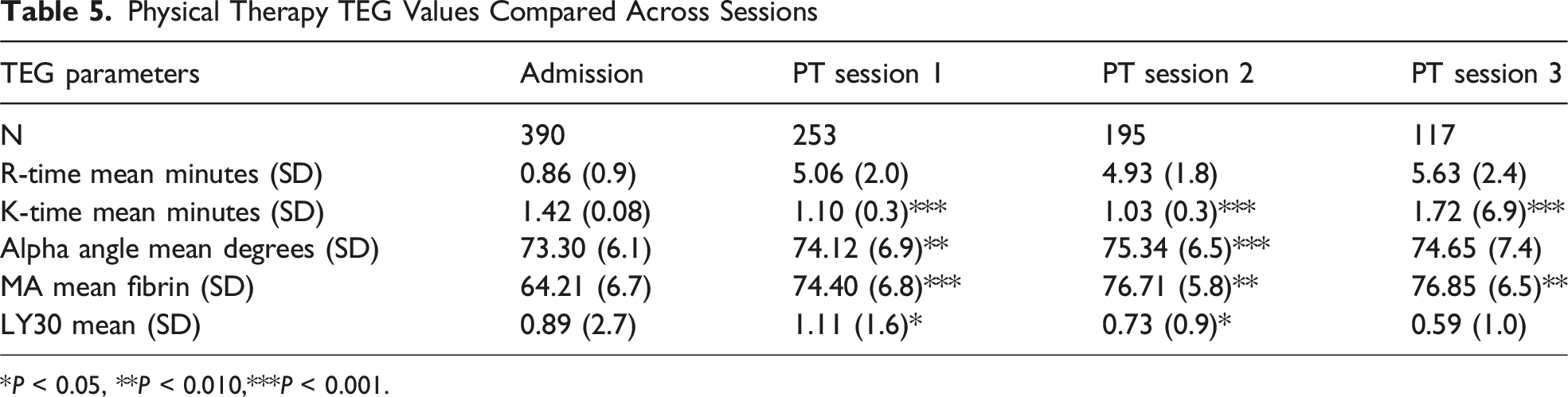
*P < 0.05, **P < 0.010,***P < 0.001.
VTE Detection During Hospital Stay Across ISS Groupings
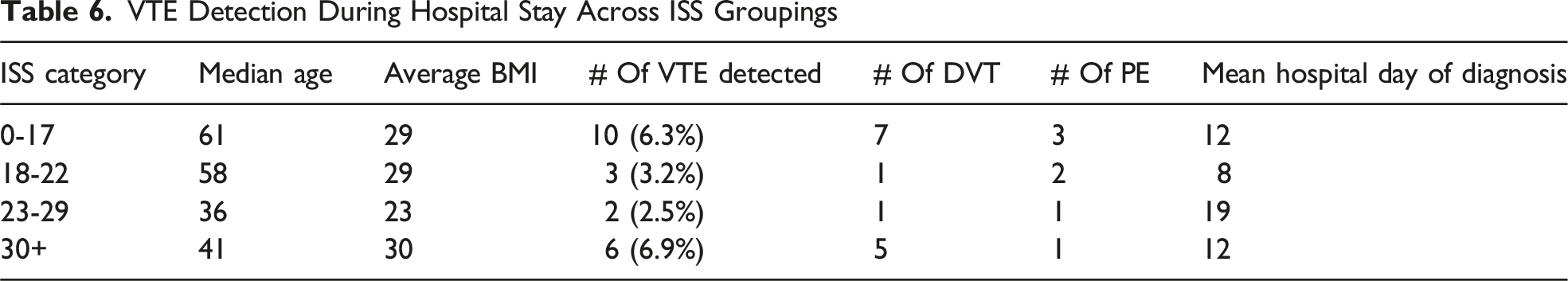
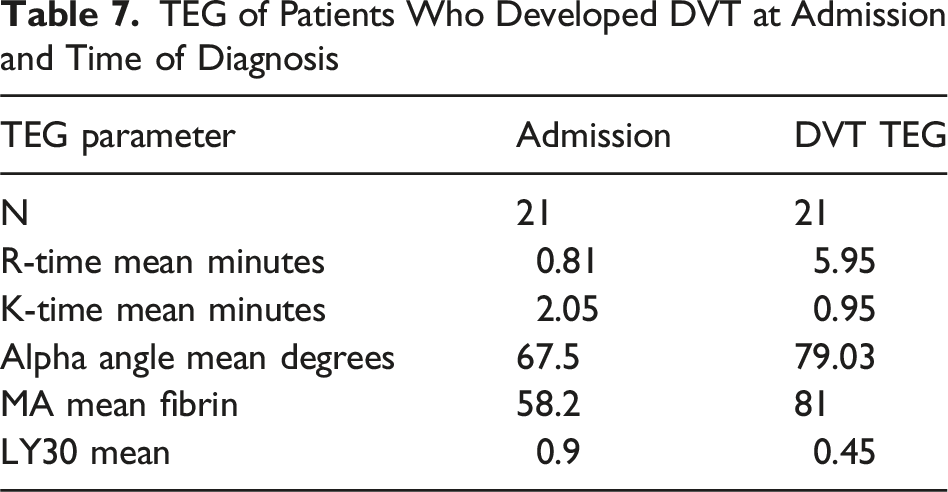
TEG of Patients Who Developed DVT at Admission and Time of Diagnosis
Discussion
TEG is a well-established coagulopathy assessment tool that has proven beneficial in the management of hypocoagulable clinical conditions. Its application in this setting has led to a more comprehensive understanding of the elements contributing to clot formation, opportunities for therapeutic intervention and spotlighted investigative pathways to better understand complex clinical entities such as consumptive coagulopathies that may be associated with heightened mortality risk. However, TEG’s role in assessing hypercoagulable states has been poorly explored, specifically with a lack of analysis of TEG changes over time and analysis of TEG as a whole compared to its individual parts. Given its ability to give dynamic information about clot formation, assessment of TEG could allow for a predictive likelihood of prothrombotic phenomena. With known morbidity and mortality risks and expense of VTE, TEG as a potential screening modality for pro-thrombotic states and evaluation of VTE risk escalations would be beneficial.
Several studies have evaluated admission TEGs but the associations of an admission parameter to an eventual clinical occurrence of VTE development is challenging to validate.2,9-11 One study reports twice the likelihood of developing VTE in trauma patients with an admission TEG with a single hypercoagulable parameter while another analysis shows elevations in risk up to 6.7-fold in patients with elevated MA on admission.2,10 We report the first effort at tracking TEG parameters in high-risk patients over their hospital stay while assessing all parameters of the TEG profile. To the author’s knowledge, there are no comprehensive studies detailing this trend towards a prothrombotic state in the injured patient over time. For reference, the anticipated changes of a hypercoagulable state on a TEG assay would include a shortened K-time, increased MA, increased alpha-angle and a reduced LY30. 12
In our study we identified no real differences across our ISS groupings related to their gender, race or comorbidities, therefore limiting confounders. While R-times were reported, they are not extensively discussed as both rapid and standard TEGs were collected. These modalities use different reagants and lead to varying R-times, make comparisons impossible. Additionally, given that R-time represents the short time to form a new clot, we believe it serves a more valuable role in acutely bleeding patients and has less importance in hypercoagulable assessment. K-times were observed to be significantly different across ISS groupings in the admission data set and the perisurgery day four to six data set, but this finding did not trend across the entire study population. We also found that K-times were on the low end of normal ranges throughout the observation period and decreased by 0.096 units over time (P < 0.001). A steady decrease in K-times corresponds with an intravascular environment that more rapidly forms a fixed strength clot.
As we compared the remainder of our TEG parameters over time, we found that the MA was significantly higher in both peri-surgery data sets as well as the three physical therapy sets when compared to the admission MAs for the respective ISS groupings (P < 0.001). MA levels remained high, or high-normal, when compared to reference range. Additionally, the three physical therapy sets all had significantly higher MA values than those from the perisurgery data sets. The MA values trended upward across the study timeline, representing an intravascular environment rich for generation of stronger clots and would likely elevate thrombosis risk. Similar to the MA value increases, the AA values were recorded at the high end of normal across all ISS groupings throughout the timeline of the study period, implying a fibrinogen-rich intravascular environment. Additionally, the AA trended upward over the study period and was noted to be distinctly elevated in the patients where DVTs were identified. While statistical significance was unable to be established for this finding, it is intuitive that a fibrinogen-rich environment would associate with increased thrombotic event risk.
Our findings related to LY30 did not demonstrate statistical significance when compared across all ISS grouping over the perisurgery and physical therapy time points. However, it was noted that LY30 was in the low range of normal over the study period, suggesting limited fibrinolysis activity. LY30, the lysis of the formed clot as a percentage over 30 minutes, reports a normal range that includes the lower limit of the test potential, 0%. This means that breakdown of 0% of a clot over 30 minutes is considered “normal,” but in a non-hemorrhagic patient there is expected to be a continuous, dynamic balance of clot formation and clot breakdown. Given our target patient population was not bleeding, it begs the question whether the low end of the reference range should not be adjusted when evaluating for thrombosis potentiation. Stettler et al describe different phenotypes of fibrinolysis, with a LY30 of less than 0.6% being consistent with fibrinolysis shutdown and association with increased post-traumatic mortality. 13 As literature on hypofibrinolysis and fibrinolysis shutdown grows, it can be suggested that we cannot solely focus on the currently accepted reference range when evaluating critically ill patients like the ones in our study.
The consistent findings across the study period were a clear upward trend of AA and MA values as well as a consistently low, down-trending LY30. In a stable setting, one would anticipate TEG values aligning with normalization instead of deviation towards hypercoagulable. While we cannot conclude that any given value or parameter absolutely signals thrombosis risk, the combination of elevated MA and AA could represent an environment suited for the development of clot with minimal thrombolysis, features presumably consistent with VTE formation.
Given that TEG parameters are ideally interpreted as a whole, it is not completely understood whether a single parameter, and its deviation from the reported normal range, is of clinical significance especially when taken out of context with patient clinical condition. However, when multiple variables of a TEG assay consistently imply hypocoagulability or hypercoagulability, the viscoelastic assay can be a guiding modality in the management of coagulopathies.
We identified twenty-one VTEs during the study period, which is a rate of 5.0%. Independent analysis of these TEG parameters revealed elevated MA values, increased AAs, shortened K-times and very low LY30 values across all ISS groupings, all findings consistent with a hypercoaguable intravascular state. However, because of the small sample size, no statistical significance could be determined.
Throughout the study TEG values demonstrate incremental changes warranting interpretation. Related to the valuation scale of TEG parameters, the quantitative reporting scale of TEG may not be precise enough to identify deviating values from the normal range in prothrombotic states. Multiple studies have assessed the accuracy of reference ranges for TEG. Wei et al 13 analyzed over 17 000 TEGs on healthy volunteers and found them to be hypocoagulable compared to manufacturer norms with variations between the young, middle-aged and elderly, as well as differences between men and women. Other studies show AA, MA and R-times out of range in healthy volunteers when compared to manufacturer-reported norms.14,15 These findings coupled with what we consider subtle differences in our TEG valuation assessment for a prothrombotic states raises the question of whether a shifting reference range reflecting healthy vs hypocoagulable and hypercoagulable patients may provide enhanced clarity in TEG trend observations.
Our study has several limitations that deserve discussion. The study design targeted TEG draws post and pre-procedure which proved difficult to standardize due to EMR order entry timing, nursing collection protocols and laboratory delivery times of the sample, making the distinction of pre and post-procedure TEGs unreliable. Tranexamic acid is routinely given in the field by first responders for severely injured patients, but identification of its delivery was not feasible and its potential influence on the admission TEG data is unknown. All patients in the study group received institution-specific, protocol-directed DVT prophylaxis which could impact the TEG results, but use of LMWH and heparin was not specifically compared and time to initiation of anticoagulation not tracked. This study did not include routine screening for DVTs, likely limiting the discovery of small asymptomatic thromboses. The timing of physical therapy was non-standardizable due to patient heterogeneity, creating variability in timing for TEG assessment. Some patients opted out of the TEG draw process throughout the study period which is highlighted by the progressive decline in patient totals over this period. Lastly, we were not able to sub stratify type of injury or surgery provided in this analysis which could confound the ISS groupings. Future directions could focus on utilizing artificial intelligence and advanced models to potentially identify signals that otherwise have not been identified. Further prospective work would benefit to strengthen the findings we identified and specifically correlate VTEs with differing TEG parameters to identify signals that may be of clinical significance.
Conclusion
TEG is a fascinating tool to consider for the purposes of VTE risk assessment. Our study suggests a potential TEG parameter signal in DVT formation, specifically increases in MA and AA with decreases in K and a consistently depressed LY30 in high-risk patients over a continuum of a hospital stay after traumatic injury. However, more prospective work will be needed to firmly validate TEG parameter deviations towards prothrombotic potential.
Footnotes
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Funding for this study was provided by a grant from the Georgia Trauma Foundation.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
