Abstract

Leptospirosis is a zoonosis caused by Leptospira spirochetes. The clinical manifestations associated with this infection are polymorphic, from mild to extremely severe (1–3). Leptospira interrogans is the pathogenic species; it consists of more than 24 serogroups and over 230 serovarieties, among them those that may affect humans, causing the disease (L. icterohaemorrhagiae, L. canicola and L. pomona) (1, 4).
Leptospirosis is more prevalent in rural areas. After occupational or recreational exposure to water or soil contaminated with leptospiras (present in the urine of wild or domestic animals), the agent penetrates through mucosa or lacerated skin. After the penetration there is an incubation period of 2–30 days. Most patients start to present clinical manifestations of the disease between days 5 and 14 (4–6). The onset of the disease is abrupt with nonspecific headache, myalgias, fever, nausea, vomiting, conjunctival effusion, skin rash and photophobia. During this septicaemic or anicteric phase, aseptic meningitis is found in up to 25% of the cases (3, 7). During the icteric or immune phase, aseptic meningitis happens in 5–10% of cases and involvement of the central and peripheral nervous systems may occur (1–3, 7, 8). Intracranial hypertension (IH) associated with aseptic meningitis has been described as the initial manifestation of leptospirosis (1–3). However, we have found just one report on IH as the sole initial neurological expression of neuroleptospirosis (9). In this report we describe the case of a woman with IH as the sole neurological manifestation of neuroleptospirosis. Headache was her chief complain during the entire course of the disease, which made the diagnosis of leptospirosis difficult.
Case report
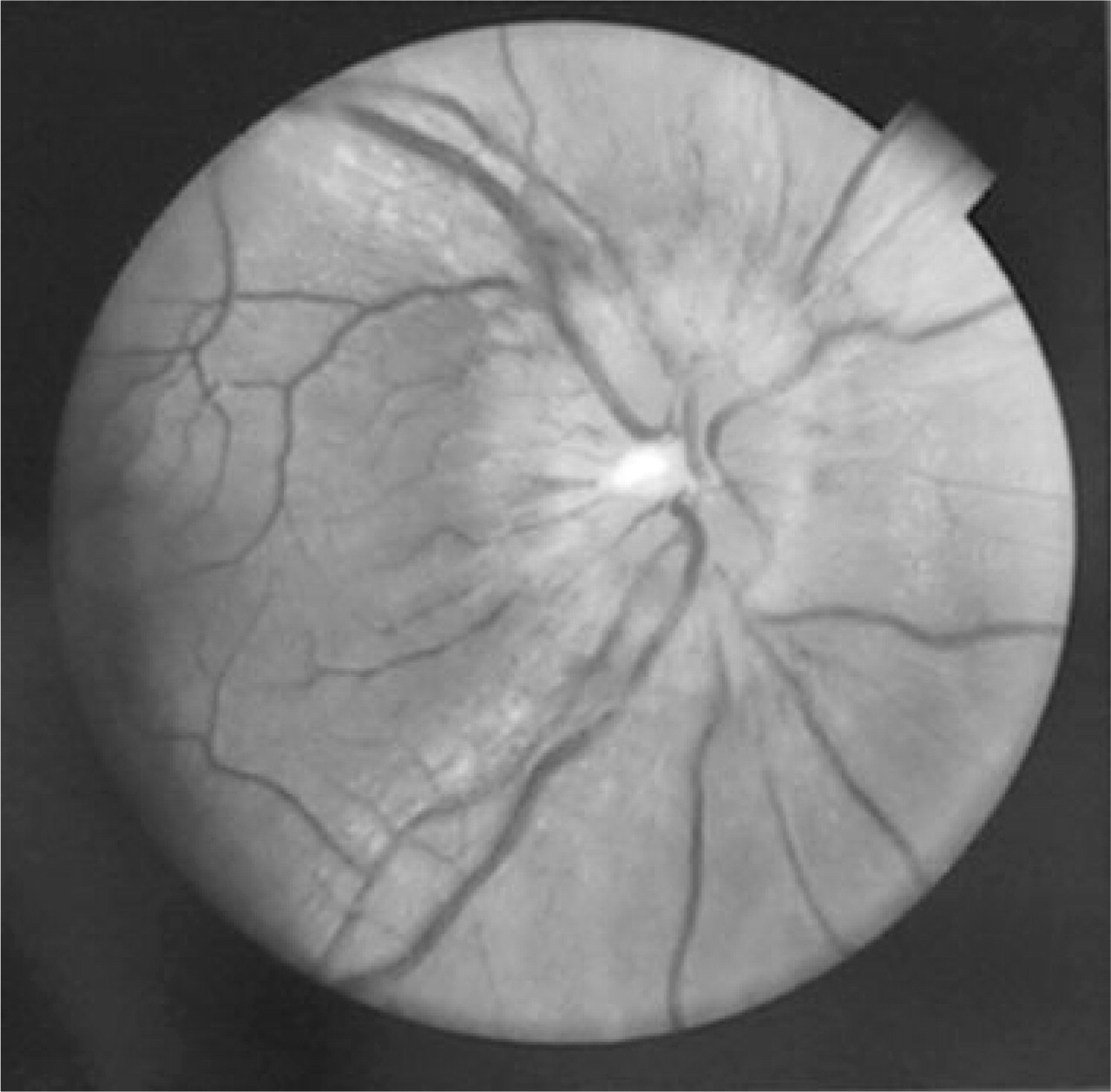
This 37-year-old African–American female presented to a hospital in the rural area of Colombia north-west. Severe holoacranial headache was her chief complain. Symptomatic headache treatment was not effective. After a few days she started to complain about nonspecific malaise and mild fever. Other aspects of her medical history were not relevant. Blood tests showed a positive IgM for hepatitis A and symptomatic treatment was started. She continued to have headache, and started to vomit, being hospitalized. After 6 days of hospitalization she developed bilateral paresis of the VI cranial nerve. At this time, papilloedema was evident (Fig. 1). Her neurological exam was otherwise unremarkable. She had ictericia, but not hepatomegaly. She was admitted in a University Hospital 15 days after the onset of her illness. At admission, tubular vision was found in the campimetry (Fig. 2).

Fundoscopic image showing retinal signs of intracranial hypertension.
Computer campimetry performed when the patient already had signs of intracranial hypertension.
Initial laboratory tests were compatible with an icteric syndrome. The total bilirubin was 3.7 mg/dl (direct bilirubin = 8 mg/dl). Results of the following tests were normal: antigens and antibodies for hepatitis A, hepatitis B, hepatitis C; HIV, VDRL, TSH, Coombs test, rheumatoid factor, anticardiolipin antibodies, antinuclear antibodies (ANAs), antibodies to extractable nuclear antigens (ENAs), anti native DNA, lupic anticoagulant, latex for Epstein-Barr virus, thick film for haemoparasites. The dark-field examination of blood was positive for Leptospira; indirect immunofluorescence was positive for both IgM and IgG antibodies; titres were 1 : 360 (IgM) and 1 : 180 (IgG) (normal values 1 : 40 and 1 : 80).
The contrasted cranial MRI was normal. Lumbar puncture (LP) revealed an opening pressure of 60 cm of water; cerebrospinal fluid (CSF) findings were normal. Five days later, a second LP was performed with an opening pressure of 56 cm of water; CSF examination was again normal. The IH syndrome was treated during the following 4 days with daily LPs, without clinical improvement. A lumboperitoneal shunt was done on the 14th day of hospitalization and produced transient improvement of the symptoms. However symptoms of intracranial hypotension appeared 10 days later after the procedure. They were controlled with the placement of a low-pressure valve in the shunt. Total improvement was obtained.
The patient was treated during 7 days with intravenous crystalline penicillin, 600.000 U every 6 h starting on the 11th day of her hospitalization. CSF remained within normal limits throughout her hospital stay. She got complete improvement of all her symptoms. She is currently asymptomatic, after one year of follow-up.
Discussion
Leptospirosis is a worldwide disease, more prevalent in the tropics; its epidemiology has changed in recent years due to accidental exposure to contaminated water and poor sanitary conditions prevalent in the third world (4, 5, 9). Aseptic meningitis is the initial expression of the disease in 5–13% of cases; it appears in the leptospiremic phase, often associated with IH. Later, during the immune phase, lymphocytic pleocytosis is found in 50–90% of cases associated with increased proteins and normal CSF glucose (3, 4). Other central nervous system manifestations have been described, including myeloradiculopathy, Guillain–Barré-like syndrome, meningoencephalitis, intracerebral bleeding, cerebellar dysfunction and movement disorders (1, 2, 8, 10–13).
Microagglutination has been considered as the best diagnostic method but its complexity has limited its use to reference laboratories (1–3). In other diagnostic procedures such as dark-field examination of blood or urine, false-positive results are frequent (2–4). Antigens or antibodies may be detected by different serologic tests; sensitivity and specificity values differ according to the test used (1, 2). A confirmatory diagnostic test is the polymerase-chain reaction (PCR) which has high sensitivity during the first week of the disease (1, 2).
In the case reported herein, IH without meningitis was the sole neurological manifestation. We diagnosed leptospirosis based on the clinical features (hepatic and central nervous system involvement) associated with the dark-field observation of leptospiras and the presence of IgG and IgM specific antibodies in serum (the tests used in this patient have 90.4% sensitivity and 100% specificity) (14, 15). The patient responded well to penicillin. Several other disorders were ruled out. Because headache was the chief complain, the diagnosis was difficult and not precocious. The most striking feature of this case was the IH syndrome manifesting just with headache for several days and not associated with meningitis. IH was very rarely reported as a single manifestation of neuroleptospirosis (12). An autopsy review of 12 cases with leptospirosis and neurological manifestations revealed IH as the main manifestation in just one (9). To the best of our knowledge, no other reports of headache as the chief complain for several days in patients with leptospirosis have been published.
