Abstract
In a double blind, placebo-controlled study to assess the prophylactic effect of hyperbaric oxygen therapy on migraine, 40 patients were randomly assigned to a treatment group receiving three sessions of hyperbaric oxygen, or a control group receiving three hyperbaric air treatments. The patients were instructed to keep a standardized migraine diary for eight weeks before and after the treatment. Thirty-four patients completed the study. Our primary measure of efficacy was the difference between pre- and post-treatment hours of headache per week. The results show a nonsignificant reduction in hours of headache for the hyperbaric oxygen group compared to the control group. Levels of endothelin-1 in venous blood before and after treatment did not reveal any difference between the hyperbaric oxygen and control groups. We conclude that the tested protocol does not show a significant prophylactic effect on migraine and does not influence the level of endothelin-1 in venous blood.
Introduction
Several observations link oxygen tension to headaches. Hypoxia causes headache, illustrated by the high prevalence of headache in mountaineers before acclimatization to altitudes above 2500 m. A study of people living at high altitude has also shown a correlation between migraine and low partial pressure of oxygen in the blood (1). Oxygen acts as a vasoconstrictor of cerebral vessels (2), and inhalation of 100% oxygen is an effective treatment of cluster headache attacks (3). HBO has also been tested as a prophylactic treatment of cluster headache. A study by Di Sabato et al. (4) showed reduced attack frequency in 6 out of 7 patients after a single treatment at 2.5 atmospheres absolute pressure (ATA). However, in a recent double-blind, placebo-controlled cross-over study Nilsson Remahl et al. (5) found no difference in headache index or prophylactic effect between HBO and sham treatment in 16 patients.
A randomised study has shown no effect from inhalation of normobaric oxygen during migraine, but a significant effect from HBO therapy (2 ATA), aborting attacks in 9 out of 10 patients (6). A significant acute effect from HBO on pain experienced by female migraineurs has also been shown (7). There is thus reason to believe that oxygen plays a role in the pathophysiology of migraine.
A number of theories have been put forward as to the pathophysiology of migraine. It is likely that both central nervous and peripheral vascular mechanisms are involved (8). Specific drugs for averting acute attacks, like ergotamine (9) and sumatriptan (10, 11), act as vasoconstrictors through their agonistic effect on serotonin receptors, while most existing prophylactic drugs, e.g. calcium channel blockers (12) and beta blockers (13), are vasodilators.
The exact mechanism behind a vascular cause of migraine is unknown, but certain peptides may be of importance (14). Endothelin is a peptide secreted from endothelial cells. It is first and foremost known as a highly potent vasoconstrictor agent, but may also have dilating effects (15). Studies have indicated that migraineurs have higher interictal levels of endothelin-1 in plasma than healthy controls (16, 17). Most studies also indicate that plasma endothelin levels rise during the migraine attack (16–20), though ictal reduction has also been reported (21).
Studies have shown increased endothelin levels during experimental and disease state (cor pulmonale) hypoxaemia (22) and high altitude hypoxia (23, 24), and a subsequent normalization of arterial pO2 at high altitude by increasing the fraction of inspired oxygen has been followed by a drop in endothelin (24). It is now known that endothelin production during hypoxia is regulated by an endothelin-1 hypoxia response complex (25). However, the response to hyperbaric oxygen is less well documented. The recent study of Nilsson Remahl et al. (5) found no differences in endothelin-1 levels, before or after treatment, in a small subgroup of cluster headache patients exposed to hyperbaric conditions (2.5 ATA, 100% oxygen or 10% oxygen in nitrogen).
The main aim of the current study was to determine whether a prophylactic effect on migraine could be observed from HBO therapy in migraineurs with frequent attacks. A secondary aim was to investigate the effect HBO on endothelin-1 levels and whether correlation between endothelin levels and possible treatment effects could be observed.
Methods
Patients and protocol
Inclusion criteria for patients in the study were migraine with or without aura according to the International Headache Society criteria (26), with 2–8 attacks per month for the last 3 months. At screening, patients were asked whether they had other types of headache and if so, whether they could differentiate this headache from the migraine attacks. All patients were given a clinical examination including neurological, circulatory and respiratory status. Chest X-rays were taken. Patients with serious claustrophobia or with a history of lung injury or serious lung disease were excluded from the study.
The protocol was designed as a randomised, double blind, placebo controlled study. Forty patients were included in the study and the patients were randomly assigned to the treatment or control group. The treatment group received 3 HBO treatments (100% oxygen, 2 ATA, 30 min) for 3 consecutive days; the control group received the same treatment (2 ATA, 30 min) breathing air instead of oxygen. Only the chamber operator had knowledge of which treatment was given, the patients and all medical personnel were blinded. Communication between the chamber operator and the patient was limited to short instructions before the patient entered the hyperbaric chamber. The chamber operator was specifically instructed not to discuss the topic of treatment gas with the patient or any other participants in the study. The study was approved by the Regional Committee for Research Ethics.
Treatments were given in a HyOx monoplace pressure chamber (HyOx Systems Limited, Aberdeen, UK). A transcutaneous oximeter (TCM3, Radiometer Copenhagen, Denmark) was used to assess the arterial oxygen levels of the patients during treatment. Only the chamber operator had knowledge of the arterial oxygen levels. Treatment days were Tuesday to Thursday for all except one patient who was treated Monday to Wednesday. Treatment was started at 1100h, and lasted for approximately 1 h including compression and decompression.
The patients were instructed to keep a standardized diary containing information of number of headache attacks, their duration and intensity, accompanying symptoms and doses of attack-averting drugs. They should also indicate whether the headache was migraine or not. Subjects were instructed not to change medications for migraine attacks when entering the study. The diaries were kept for 8 weeks before and 8 weeks after the treatments. On the basis of the headache diaries, data were summed up for each week. Weeks 1–8 are the pretreatment period; weeks 10–17 the post-treatment period. The treatment period is called ‘week 9’, but comprises only the 3 treatment days. This period was analysed separately.
Blood samples for endothelin analysis were drawn from the cubital vein into EDTA-vacutainers before and after the first and the last treatment, and immediately cooled in ice water. Samples were centrifuged at 3000 g and 4°C for 15 min to obtain platelet-poor plasma, which was then stored at −80°C until assayed for endothelin.
Endothelin assay
Endothelin-1 was analysed using a sensitive enzyme immunoassay (R & D Systems Europe Ltd, Abingdon, UK). Analysis of the samples was carried out according to the manufacturer's instructions except that vacuum concentration of extracts was only briefly used, after which samples were frozen and freeze-dried. Samples were randomised before assay and analysed blindly. Intra- and inter-assay coefficients of variation were both under 5.2%.
Efficacy parameters
As the primary efficacy parameter we decided to use hours of headache per week instead of the recommended ‘attacks per 4 weeks’ (27). One reason for this was that the use of triptans may make it difficult to distinguish between separate attacks, and the participants would also have to record exactly when the headache started and stopped. Another important reason was the exploratory nature of this trial in which we had little knowledge about relevant treatment doses and the duration of a possible effect. We therefore wanted to have a sensitive parameter, which could also register moderate and relatively short lasting effects of less than one month. As secondary parameters, we also registered days of headache and doses of attack averting drugs per week.
Statistics
For all efficacy parameters, a baseline was determined as the mean level of the 8 pretreatment weeks, and post-treatment changes from this baseline were compared for the 2 groups using the nonparametric Mann–Whitney test. Endothelin data were analysed using Student's t-test. Statistical analysis of the results was performed using SPSS version 10 from SPSS Inc.
Results
Thirty-four patients completed the study strictly according to protocol, 19 in the HBO group and 15 in the control group. Of the remaining six patients included in the study, one patient did not complete the treatment due to a technical problem with the pressure chamber, two patients chose not to participate due to claustrophobia and one patient had an upper respiratory tract infection and could not be compressed due to the danger of barotrauma. One patient had a pathological lung X-ray and one patient withdrew from the study for unknown reasons. Characteristics of the patients completing the study in the two groups are given in Table 1. There are no significant differences between the groups for any of the shown parameters.
Characteristics of patients completing the study in the two groups

Data are missing for one patient in the control group for weeks 16 and 17. The missing data were replaced by the mean value for weeks 10–15 for this patient.
Primary measure of efficacy
Mean hours of headache per week in the pretreatment period was 21.3 h for the HBO group and 16.8 for the control group; the difference is not significant. Figure 1 shows the mean change from pretreatment period for both groups for each of the post-treatment weeks. The graph seems to indicate an initial reduction for the HBO group whereas for the control group there is apparently no effect. The differences between the groups are however, not significant for any of the weeks.

Mean changes from pretreatment baseline in hours of headache per week. □ oxygen group, ▪ placebogroup.
Since we beforehand had no knowledge of the duration of a possible treatment effect, it would make sense to analyse the results using a model where the assumed duration could be changed. This can be done by calculating a weighted average for each patient, where the early post-treatment weeks are weighted more than the later weeks. A weighted average can be obtained from the formula:
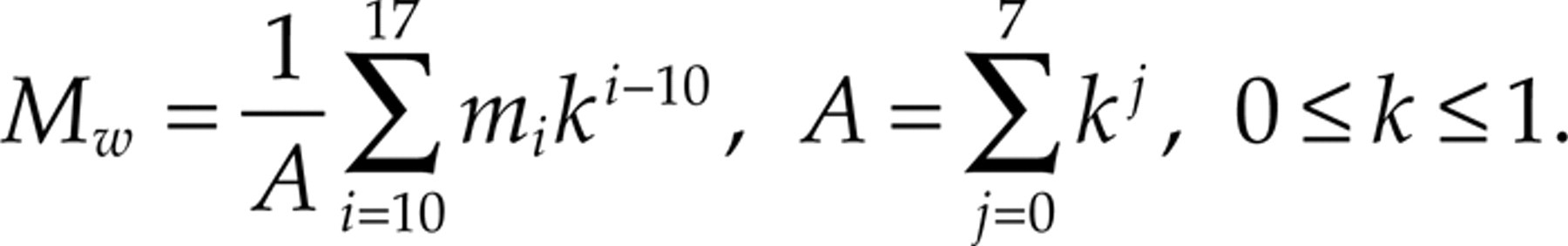
where Mw is the weighted average calculated for each patient, mi is the number of hours of headache for week i, and k is a factor for weekly reduction in treatment effect. The factor k should be chosen on the basis of the expected duration of the effect studied. Choosing k = 1 gives the arithmetic mean (constant effect). The value k = 0.5 corresponds to a 50% effect reduction per week, and k = 0 corresponds to no effect after the first week. Table 2 shows P-values for a difference between the HBO and control groups for some values of k. There is no significant difference for any tested value of k.
P-values for a difference between the hyperbaric oxygen and control groups for different values of k

For a further exploratory analysis of the data we looked at female participants separately. There were no significant differences between the oxygen and control groups when we compared each post-treatment week separately. Calculating weighted means as described above with a factor k of 0.5 we found a 4.5 h reduction in hours of headache per week for the HBO group and a 1 h increase for the control group. This difference is significant (P = 0.045).
The treatment period (‘week 9’) was analysed separately. We found no difference between the oxygen and control groups, but there was an increase in hours of headache experienced by both groups compared to the pretreatment level. Corrected for the number of days the increase was 6.9 h per week for the HBO group and 4.7 h for the control group.
Endothelin levels
Average total endothelin-1 levels measured in the blood samples are shown in Table 3. The results were normally distributed. The range for all samples was 0.46–1.48 pg/ml, as opposed to the range cited by the manufacturer for a random population (0.3–0.9 pg/ml, n = 25). Overall 47% of the migraineurs in this study had a plasma endothelin-1 level in one or more samples on or above the upper level cited by the manufacturer. However, Student's t-test showed no significant differences between the HBO and control groups or within either of the groups before and after treatment. There was also no observable correlation between treatment response and changes in endothelin-1 levels (not shown).
Endothelin-1 levels (pg/ml) in plasma, mean ± SD

Other parameters
We also investigated the number of days with headache per week and doses of attack-averting drugs per week. Changes from baseline were compared for the two groups for each post-treatment week separately and for a weighted post-treatment average, as described above, with k = 0.50. No significant differences between the groups were found for either of the parameters.
The transcutaneous arterial oxygen measurements showed that in 46 of the 57 HBO treatments (81%) the arterial oxygen partial pressure exceeded 99.9 kPa, which is the upper limit for the oximeter. For the treatments where this level was not reached, the oxygen levels were in the range 65.1–93.2 kPa. For the control group the mean peak oxygen level observed during the treatment was 18.4 ± 4.7 kPa. Pre-treatment baselines were 9.2 ± 2.2 kPa and 8.3 ± 2.1 kPa for the HBO and the control groups, respectively. There was no observable correspondence between maximum oxygen level reached and response in hours of headache in either of the groups.
Looking at the acute effect of treatment, we registered 12 cases of pretreatment headache and 7 cases of post-treatment headache in the HBO group. For the control group the numbers were 14 and 9, respectively. There was no significant difference between the HBO and the control groups in the reduction of acute headache during the treatment.
Discussion
There is no agreement on the proper dose to use in hyperbaric therapy protocols. The upper limit of oxygen is given as 280 kPa to reduce the risk of central nervous system oxygen toxicity (28). However, these oxygen tensions are only used for treatment of decompression sickness (29). In clinical practice, oxygen tensions between 150 and 250 kPa have been used, with treatment times varying between 30 and 90 min (30). The protocol used in the present study was a compromise between several considerations. Previous studies have shown 200 kPa to be sufficient to abort acute migraine attacks (6). Furthermore, the study of Bergo and Tyssebotn (31) showed that even 150 kPa oxygen gave a significant vasoconstriction of the brain circulation with reduction in blood flow.
When choosing treatment duration and the number of repeated treatments we had to consider the risk of decompression sickness in the control group. The control group received air at 2 ATA to make the procedure identical for the groups. To minimize the risk of decompression sickness we chose to give the control group compressed air instead of normoxic nitrox (10.5% oxygen at 2 ATA). The control treatment used in the study was therefore not strictly placebo, as the oxygen partial pressure was twice that of breathing air at sea level.
Some 25% of migraine sufferers are men, whereas only 5% of the subjects included in this study were male. Female migraineurs are generally more debilitated by their ailment than men and more frequently seek medical help. Subjects in most clinical studies are recruited from patients already ‘in the system’. Thus, as in this study, there is often a relative preponderance of female subjects. Indeed, in some studies female gender is actually an inclusion criterion. Our exploratory analysis of the data shows a significant difference between the HBO and control groups if the two male patients are excluded. The numbers are too small to decide whether this difference is caused by a true gender difference or by coincidence.
Previous studies have shown an effect of HBO in aborting attacks in patients with migraine refractory to medication (6, 7). Our results show a decrease in the occurrence of headache when comparing immediate pre- and post-treatment, the reduction is similar for the HBO and control groups. However, if we look at the treatment days there is a nonsignificant increase in hours of headache for both groups compared to the baseline level. This may be related to the stress induced by the treatment itself, the blood samples taken, and tests performed before and after the treatment.
The endothelin-1 levels measured in plasma were generally higher than might be expected from a random population, but since all the patients were migraineurs this was not unexpected (16, 17). However, we observed no significant effects from HBO therapy on the level of endothelin-1 in venous blood, regardless of whether pre- and post-treatment was compared, or whether the HBO group was compared with the control group. One possible explanation for this could be that a reduction in cerebral blood flow caused by the high oxygen levels outweighs the biochemical effect of the increased partial pressure of oxygen (31).
We conclude that the tested treatment protocol shows no significant prophylactic effect on migraine on the tested population. It does not reduce the doses of attack-averting drugs used by the patients, and has no measurable influence on endothelin-1 levels as measured in venous blood. However, although not significant, we do see a trend towards reduction in hours of headache for the HBO group. Hence, we cannot rule out the possibility that an optimal treatment protocol and comparison with a normoxic control group would make the differences significant in favour of HBO treatment.
Footnotes
Acknowledgements
This study was supported by the Norwegian Research Council and AGA AB Medical Research Fund. The authors wish to thank the patients who took part.
