Abstract

Introduction:
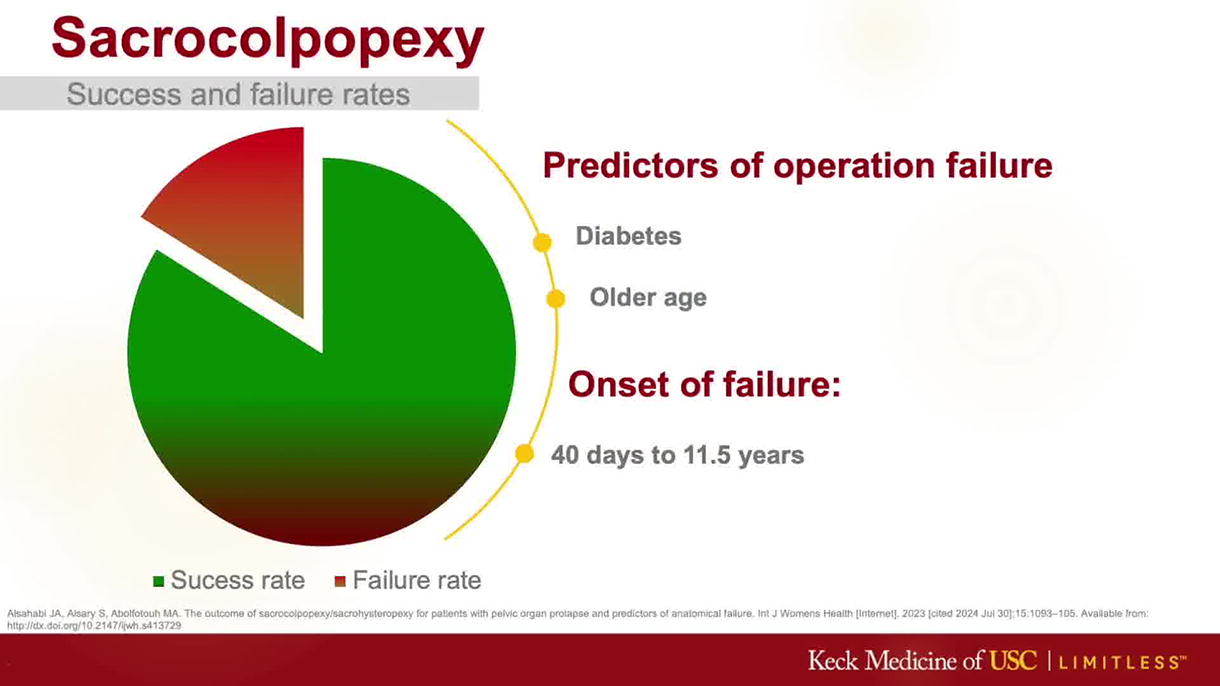
Pelvic organ prolapse (POP) is a condition where weakened pelvic muscles allow pelvic organs to slip down and bulge through the vaginal canal; it affects 30% of women to varying degrees. 1,2 Around 300,000 surgeries are performed each year in the United States, accounting for 10–19% of women. 2 This number is expected to increase given the aging population and improvements in quality of life. 2 Unfortunately, these patients have a 15.9% risk of necessitating further re-intervention due to adverse effects or failure. 3 Abdominal sacrocolpopexy is the current gold standard repair for vaginal vault prolapse and includes the placement of a mesh. Polypropylene is the most popular synthetic materials. 4 –6 Intraoperative risks such as presacral bleeding, injury to the urinary system, and postoperative complications account for 3–10% of cases. 7,8 This video showcases three cases of mesh-related complications along with their respective approaches and techniques.
Methods:
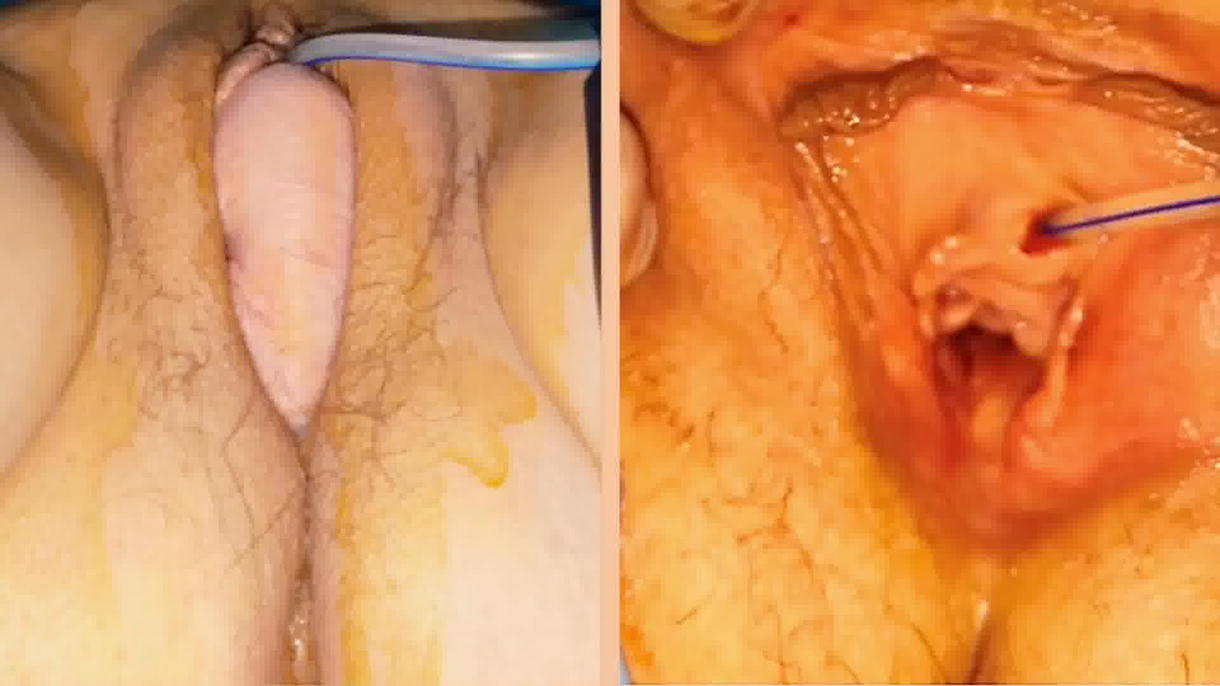
In this study, three cases of patients who underwent abdominal re-sacrocolpopexy in 2022–2024 by a single surgeon were collected. Surgical management was individualized and depended on the type of complication the patient had suffered. Case number 1 involved a 53-year-old woman complaining of pelvic organ prolapse recurrence. Case number 2 was a 75-year-old patient who presented with vaginal discharge and spotting. Case number 3 consisted of a fistula formation between the bladder and the vagina.
Results:
Successful robotic approaches were achieved in all three cases, resulting in the reduction of pelvic organ prolapse, abscess removal, and repair of the fistula, respectively. In the first case, surgery was tailored to remove the previous mesh and insert a new one, but the mesh was left in place with the intention of not compromising the patient’s recovery. Estimated blood loss was 60 cc, and operating time was 2 hours and 22 minutes. The patient was discharged 24 hours postoperatively with a urethral catheter and drain, which were both removed at 72 hours. In case number 2, the mesh was removed entirely. Estimated blood loss was 10 cc, operating time was 3 hours and 6 minutes, and the patient was discharged on day 5. Before sending the patient home, the Foley catheter, ureteral stent, and Blake® drain were removed. Successful evolution was achieved for up to 4 months following surgery. In the third case, the mesh was removed entirely.
Conclusion:
We have successfully demonstrated the feasibility of robotic re-do sacrocolpopexy along with its technical challenges, emphasizing its need when re-intervention is imminent. Awareness of complications is crucial for preventing them, correctly choosing the appropriate management, and ensuring proper follow-up. In addition, this study has shown that transvaginal mesh excision may not always be sufficient or appropriate, potentially causing increased distress and uncertainty in patients.
Authors have received and archived patient consent for video recording/publication in advance of video recording of the procedure.
Runtime of video:
8 mins 21 secs.
Get full access to this article
View all access options for this article.
