Abstract
Introduction:
Congenital wandering spleen is a condition that occurs when there is an absence or abnormal embryologic development of the ligaments that maintain the spleen in its normal anatomic location. 1 Without proper attachments, the spleen is able to twist about the pedicle or wander within the peritoneal cavity, which can result in abdominal pain, pedicle torsion, splenic infarction, splenomegaly, gastric varices, gastric volvulus, or anemia. In stable patients with a viable spleen, splenopexy is recommended that can be performed through methods such as direct suture to the capsule or hilum, use of a mesh sling, or creation of an omental pocket. 1,2 We demonstrate a unique technique for laparoscopic splenopexy by creating a peritoneal pouch.
Materials and Methods:
The patient is a 16-year-old female with a history of chronic abdominal pain who was diagnosed with wandering spleen after an abdominal MRI revealed an abnormal position and rotation of the spleen, as well as the presence of two accessory splenules. Laparoscopic splenopexy through the creation of a peritoneal pouch and excision of the accessory splenules was recommended.
Results:
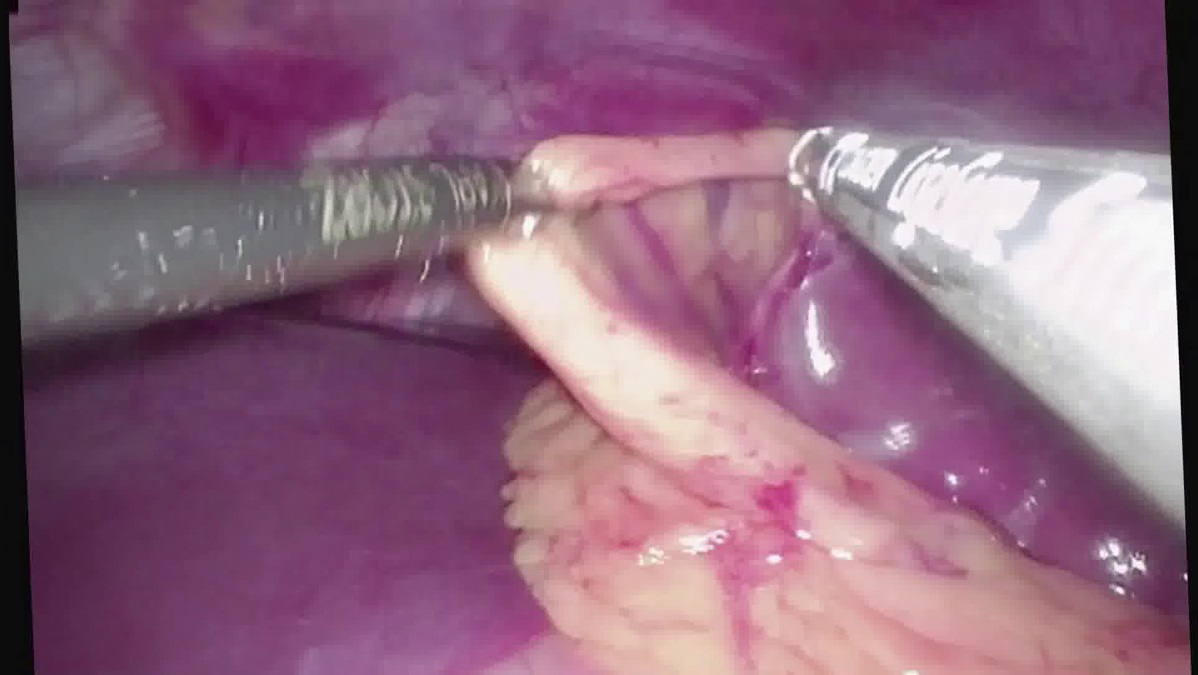
Diagnostic laparoscopy confirmed an enlarged spleen with no splenophrenic, splenorenal, or splenocolic attachments. Two accessory splenules were identified at the inferior pole of the spleen and excised. Given the size of the spleen, a peritoneal pouch was created by scoring the peritoneum above the level of the spleen and dissecting a space of adequate size where the spleen was placed. The peritoneal pouch was closed and a fat pad was utilized above the pedicle to cover the remaining peritoneal defect, ensuring the hilum remained free from compression. The patient was discharged to home on postoperative day 1 and had resolution of her abdominal pain on follow-up.
Conclusions:
Wandering spleen is a rare condition that requires a high index of suspicion for diagnosis. Laparoscopic splenopexy with the creation of a peritoneal pouch allows for appropriate fixation of the spleen, even in pediatric cases with splenomegaly.
Acknowledgment:
The source of the study is the Division of Pediatric Surgery at Penn State Milton S. Hershey Medical Center.
Author(s) have received and archived patient consent for video recording/publication in advance of video recording of the procedure
.
No competing financial interests exist.
Runtime of video: 3 mins 58 secs
Prior presentation: This video was presented at the American College of Surgeons Clinical Congress on October 25, 2023, in Boston, MA, USA.


Get full access to this article
View all access options for this article.
