Abstract
Introduction:
Congenital hyperinsulinism (CHI), or nesidioblastosis, is the most common cause of severe persistent hypoglycemia in neonates. When left untreated, CHI may cause serious brain damage and could eventually even lead to death.
1
In case of diffuse hyperinsulinism, when all beta cells are inappropriately over-secreting insulin, a near-total pancreatectomy may be indicated. With the goal of resecting 95% to 98% of the pancreas, only a small residue of pancreatic tissue between the common bile duct (CBD) and the duodenal wall is left behind.
2
To perform an adequate near-total pancreatectomy, the intrapancreatic segment of the CBD has to be safely dissected. Hereby, a feared complication is intraoperative CBD injury, associated with significant morbidity. Intraoperative injury has been reported to occur in up to 16% of open pancreatectomies involving the pancreatic head.
3,4
A laparoscopic near-total pancreatecomy is even more technically challenging, especially in the young. Therefore, to date, most near-total pancreatectomies in infants are done by traditional laparotomy. Fluorescence imaging with intravenous administration of indocyanine green (ICG) allows for clear intraoperative observation of the bile duct anatomy, which might ease the technical difficulties inherent to the near-total pancreatectomy, particularly with a laparoscopic approach.
5
This video presents a 10-month-old boy, who presented with severe persistent hypoglycemia immediately after birth. Genetic testing was performed and confirmed the diagnosis of diffuse severe CHI based on a pathogenic homozygous
Materials and Methods:
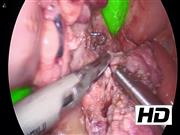
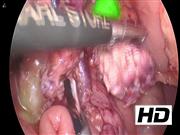
Under general anesthesia, the patient was placed in supine position. A 5 mm trocar was introduced subumbilically with two trocars aside paraumbilically and one trocar positioned in the left flank, more laterally to allow access of the upper right abdomen. First, the stomach was lifted through an earlier placed percutane endoscopic gastrostomy, placed to supply an adequate intake of carbohydrates. After transecting the right gastroepiploic vein and artery, the proximal duodenum was retracted toward the upper right quadrant through a vessel loop exiting next to the most lateral port. Then, the gastroduodenal artery was transected, after placement of clips on the side of the hepatic artery, using the harmonic scalpel. Subsequently, the uncinate process of the pancreas was dissected after the superior mesenteric vein was identified. The pancreatic head was superficially split with harmonic scalpel in such a manner that the CBD with surrounding pancreatic tissue remained intact. Then, 1 mL ICG (0.5 mg/kg) was injected intravenously. After 15 minutes of waiting, the liver appeared as well as the duodenum by drainage through the ampulla of Vater. In between, the CBD was clearly observed. Thereafter, under direct vision of the CBD, the near-total pancreatectomy was continued by dissecting pancreatic tissue from the ventral and left border of the CBD. After the dissection of the pancreatic tissue was completed, the specimen was extracted using an endobag through the subumbilical incision.
Results and Conclusions:
Approximately 5% of the pancreas remained
Runtime of video: 4 mins 2 secs

Get full access to this article
View all access options for this article.
