Abstract
Introduction:
Both endoscopic retrograde cholangiopancreatography (ERCP) and common bile duct (CBD) exploration (open or laparoscopic) are accepted management techniques for choledocholithiasis. 1 Laparoscopic cholecystectomy with preoperative or postoperative ERCP is at least a two-procedure process whereas cholecystectomy with laparoscopic common bile duct exploration (LCBDE) can provide definitive treatment in a single procedure under one anesthetic. LCBDE is associated with decreased length of stay (LOS) and cost but has equal efficacy and safety profiles as ERCP. 2 –11 Widespread adoption of LCBDE will be facilitated by systematization of the procedure and increased simplicity. Techniques commonly employed in LCBDE include vigorous flushing of the CBD, stone retrieval with Nitinol wire baskets or Fogarty balloons under fluoroscopic guidance, and use of choledochoscopy for basket or laser lithotripsy deployment. 1,12 –16 LCBDE balloon sphincteroplasty has been described in a few adult cohorts, but is not commonly utilized. 17 –19 This video describes the operative technique of balloon sphincteroplasty as an adjunct to LCBDE.
Case Presentation:
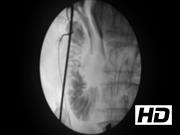
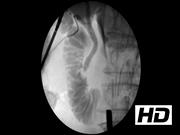
This video shows the technique for LCBDE and use of balloon sphincteroplasty in a 78-year-old male. The patient presented with right upper quadrant pain, nausea, and vomiting. His laboratories were significant for a total bilirubin of 3.0 mg/dL, AST 151 U/L, ALT 83 U/L, and WBC 10 × 103/L. A CT scan was obtained that revealed cholelithiasis with no evidence of acute cholecystitis and mild intra- and extrahepatic biliary dilation. His CBD measured 1.1 cm in size. A laparoscopic cholecystectomy with intraoperative cholangiogram and possible LCBDE was recommended. Intraoperative cholangiogram revealed a distal CBD filling defect. A 0.035″ hydrophilic guidewire was then advanced through the cholangiogram catheter into the CBD. Subsequently, a 5F balloon dilator was advanced completely into the duodenum over the guidewire. The opaque markers on the balloon assisted in positioning. The balloon was then inflated to 8 mm in diameter with a 50/50 saline–contrast mixture and gently retracted to identify the ampulla with tactile and visual feedback. The balloon was then deflated and slightly retracted so that it straddled the ampulla. After it was in the correct position, it was reinflated and held for 3 minutes to dilate the sphincter. The balloon was once again deflated and retracted to now straddle the cystic–CBD junction. It was reinflated before the completion cholangiogram to prevent flushing of debris into the proximal hepatic ducts. Contrast can be seen freely flowing into the duodenum without obstructing stones. No intraoperative or postoperative complications occurred. Postoperative laboratories revealed a normalized total bilirubin of 0.9 mg/dL. The patient was discharged home the next day.
Conclusion:
The trend over the past decade for management of choledocholithiais continues toward less LCBDE utilization in favor of ERCP despite LCBDE having equal efficacy and safety profiles with an associated decrease in hospital LOS and costs. 2 –11 An important factor in increasing adoption is to increase the simplicity of the intervention. Balloon sphincteroplasty is a straightforward and effective adjunct to LCBDE.
No competing financial interests exist.
No funding was received for creation of this study.
Runtime of video: 5 mins 35 secs

Get full access to this article
View all access options for this article.
