Abstract
Background:
An esophageal duplication is a rare but important pathogenesis of mediastinal tumor in pediatric patients. 1 It develops anywhere along the esophagus and its size can vary with diverse clinical manifestations. 2,3 Recently thoracoscopic approaches have become common even in infant cases. 3,4 We herein report a case in which thoracoscopic extirpation was performed for huge esophageal duplication derived from the posterior mediastinum.
Case Presentation:
The patient was an 11-month-old girl in whom a cystic lesion in the posterior mediastinum was detected in utero by ultrasonography. Because she was asymptomatic after birth, close follow-up was planned. During regular clinic visits, the cyst in the posterior mediastinum had grown in association with physical development. Computed tomography at 10 months of age showed a 6 × 3 cm simple cystic lesion extensively occupying the posterior mediastinum. On magnetic resonance imaging, the cyst showed low intensity on T1 imaging and high intensity on T2 imaging. The patient had no symptom at 11 months of age, but a thoracoscopic operation was planned because of the malignant potential of the growing lesion. A right-side approach was selected because of the resectability of the cystic lesion.
Operative Findings and Procedure:
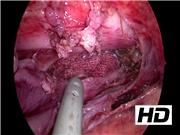
Under general anesthesia, the patient was placed in the left three-quarter prone position. A 5-mm camera port was inserted at the sixth intercostal space (ICS) of the middle axillary line using optical methods. Artificial pneumothorax was established by carbon dioxide inflation (2 L/min, 5 mm Hg), which was enough to obtain surgical view. Working ports (5 mm and 3 mm) were inserted at the fourth (operator's right hand) and eighth ICS (operator's left hand) of the anterior axillary line, respectively. The expanded cyst was easily recognized in the posterior mediastinum. To examine the cytology and to reduce the volume, the cyst was punctured and aspirated by sand balloon needle. Intraoperative cytology showed benign findings. The parietal pleura surrounding the cyst was opened by hook-type electrical cautery. The cyst wall was easily separated from the right parietal pleura by a blunt maneuver. The feeding vessels around the cyst were coagulated and divided using a vessel sealing system (LigaSure Maryland; Medtronic, Inc., Dublin, Ireland) and 3.5 mm bipolar (RoBi; KarlStorz, Tuttling, Deutschland). The medial aspect of the cyst showed severe adhesion to the contralateral parietal pleura, but blunt dissection was performed without cyst wall injury. Upper gastrointestinal endoscopy was performed at the upper esophagus as a guide to prevent injury to the esophagus and vagus nerve. After confirming the medial and upper margin of the cyst wall from the inside, the cyst was completely resected. The cyst was extracted through a 2 cm-extended camera port incision and a 10F drain was placed in the mediastinum.
Results and Conclusion:
No intraoperative or postoperative complications occurred. The postoperative course was uneventful. A pathological study revealed that the cyst included an alimentary mucosa and smooth muscle. The final diagnosis was esophageal duplication; no recurrence was recognized. Thoracoscopic extirpation of huge esophageal duplication from a one-sided approach was safe and feasible even though it extended to the contralateral side.
Acknowledgment:
We thank Brian Quinn for his comments and help with the article.
No competing financial interests exist.
Runtime of video: 4 mins 28 secs


Get full access to this article
View all access options for this article.
