Abstract
Background:
In 1976, Kluth published an atlas comprising all forms of esophageal atresia (EA). 1 We herein report a rare variant case in which thoracoscopic repair was effectively performed to treat Kluth IV1 EA combined with tracheal bronchus.
Case Presentation:
The patient was born at 40 weeks of gestation with an Apgar score of 9/9. After starting oral intake, the patient showed vomiting and respiratory distress. Coil-up sign and abdominal gas were recognized, and EA (Gross C) was suspected. Thoracoscopic repair for EA was planned.
Operative Findings and Procedure: Resection of Esophageal Membrane—
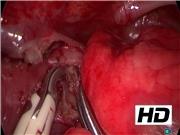
Initially, bronchofibroscopy was performed to confirm trachea–esophageal fistula (TEF). TEF was recognized 8 mm proximal to the carina at the right posterolateral side. The patient's position was then changed to the left three-quarter prone position. A camera port was inserted at the fifth intercostal space (ICS). Two working ports were inserted at the third and seventh ICSs. The azygos vein was divided using a vessel sealing system. Careful dissection of the esophagus was performed, but the esophagus showed a normal outer appearance. Membranous stenosis was, therefore, suspected. Bronchofibroscopy was performed again, and a fistula-like structure was identified as a “tracheal bronchus.” The upper esophagus was opened at the right side through a longitudinal incision. A membrane structure was recognized in the endoluminal space of the incised esophagus and resected using bipolar scissors. The longitudinal incision was transversely closed by interrupted 6-0 monofilament absorbable sutures to prevent stenosis.
Postoperative Course:
After discharge, the patient repeatedly showed atelectasis and pneumonia. Contrast esophagram showed the influx of contrast medium into the trachea. Bronchofibroscopy was, therefore, performed a third time. A TEF was recognized about 1.5 cm proximal to the carina. During the initial surgery, it was covered with an intubation tube and could not be detected. Thoracoscopic transection for the TEF was planned.
Operative Findings and Procedure: Transection of TEF—
Careful dissection of the esophagus and traction sutures of the esophagus were performed. The TEF was found in the upper mediastinum on the proximal side of the membrane-like stenosis. It was ligated with 5-0 blade absorbable sutures, Hemo-lock, and transfixing sutures and then divided using scissors.
Postoperative Course:
There were no intraoperative or postoperative complications. Contrast esophagram showed no leakage or stenosis. The patient was ultimately diagnosed with Kluth IV1 EA.
Discussion:
Kluth collected and published findings on the number and location of various types of TEFs. 1 In the study of diagnostic rigid bronchoscopy, 13.6% of EA cases had an unusual fistula, and laryngotracheal cleft was also complicated in 2.3% of cases. 2 Tracheomalacia was also reported to be complicated in 89.2% of cases under spontaneous respiration. 3 In the management of EA and TEF, the preoperative detection of other anomalies and the precise location of the TEF through rigid bronchoscopy are most important for a good outcome.
Conclusions:
Kluth IV1 EA was definitively diagnosed based on the intraoperative findings. The thoracoscopic approach was useful for the diagnosis and treatment of rare variant EA. Careful rigid bronchoscopy should be performed.
Acknowledgments:
We thank Mr. Brian Quinn for his comments and help with the article. This study was supported by a Grant-in-Aid for Scientific Research from the Japan Society for the Promotion of Science (JSPS, Nos. 26670765, 16K10466, 16K10094, 16K10095, 16K10434, 16H07090, 17K10555, 17K11514, 17K10183, and 17K11515), a Research Grant from the President's Discretionary Expenses of our University, a Research Grant from The UBE Foundation, a Research Grant from Kawano Masanori Memorial Public Interest Incorporated Foundation for Promotion of Pediatrics, a Research Grant from Tateishi Science and Technology Foundation, a Research Grant from Mitsui Life Social Welfare Foundation, and a Research Grant from The Kurata Grants of the Hitachi Global Foundation.
The authors declare no conflicts of interest in association with this study.
Runtime of video: 5 mins
Presented at the 31st Annual Congress of the Japan Society for Endoscopic Surgeons.


Get full access to this article
View all access options for this article.
