Abstract
Introduction:
Median arcuate ligament syndrome (MALS), sometimes called Dunbar syndrome, is an extremely rare condition caused by external compression of the celiac trunk and/or ganglion by an anatomically lowered median arcuate ligament (the fibrous posterior central component of the diaphragm connecting the two crura). 1 MALS is a condition usually presenting in young women, especially those between the second and fourth decades of life, though it has also been described in men. 2 Symptoms are thought to be secondary to decreased arterial flow, either because of direct compression or because of chronic ganglion overstimulation with resultant splanchnic vasoconstriction and increased postprandial demand. The condition is chronic and debilitating. Although an estimated 10%–24% of the population has an anatomically lowered median arcuate ligament, and 6.7% have asymptomatic celiac trunk stenosis, 1 only a small percentage of these individuals demonstrate associated symptoms, such as postprandial epigastric pain, nausea with or without vomiting, diarrhea, weight loss, and an epigastric bruit. Thus the condition is primarily a diagnosis of exclusion, although its identification can be augmented based on a combination of clinical presentation, computed tomography angiography (CTA), and duplex ultrasonography, 1 or papaverine infusion directly into the celiac artery with reproduction of symptoms. 3 Patients often have chronic symptoms and have undergone extensive work-up by multiple providers. Many may have developed substance dependence as a result of the chronic nature of their condition and the lack of identifiable etiology or relief. 4 Although the condition does represent a diagnosis of exclusion, duplex ultrasonography, CTA, magnetic resonance angiography, and/or gastric tonometry can all be helpful in making the diagnosis in the setting of the appropriate constellation of symptoms. Since its first identification in 1917, there have been several small case series describing a variety of approaches to its diagnosis and surgical correction. The following represents a novel approach utilizing robotic surgical techniques in conjunction with intraoperative indocyanine green (ICG) angiography; this has not been previously reported.
Case:
A 36-year-old man presented with a history of 10–12 years of episodic sharp burning epigastric pain increasing in frequency over the months just preceding his evaluation. The pain was associated with cold sweats, nausea, and vomiting and usually occurred after passage of a loose bowel movement. He stated on presentation that he usually had these episodes once or twice per year, but in the more recent months he was having it two to three times per month with worsening intensity. He denied any association with meals. He had previously undergone work-up at multiple institutions and been given the diagnosis of gastritis secondary to chronic alcoholism, although he reported sobriety for 2 years before his presentation. His medical history was significant for hypertension, gastroesophageal reflux disease, gastric ulcers, irritable bowel syndrome, no prior surgical interventions, and a history of cigarette smoking, though he had quit 5 years ago. On presentation, his abdomen was soft, nondistended, and mildly tender to deep palpation in the epigastrum, without audible abdominal bruit. He had previously undergone esophagogastroduodenoscopy and colonoscopy without aberrant findings. CTA of his abdomen and pelvis and celiac axis duplex ultrasonography were obtained 3 months before his presentation with identification of kinking of his celiac axis and hyperdynamic flow through the axis with peak systolic velocities of 297 cm/second (normal <200 cm/second). The patient was subsequently scheduled for robotic median arcuate ligament release with intraoperative ICG angiography.
Technique:
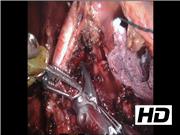
The abdomen was insufflated using a Veress needle placed at Palmer's point. A robotic 8 mm port was placed just cephalad and left of the patient's umbilicus. Under direct vision, three more 8 mm robotic ports were placed with one under each costal margin in the midclavicular line and a third at the level of the umbilical port, but in the anterior axillary line just inferior to the left costal margin. A laparoscopic subxyphoid liver retractor was placed and positioned under direct vision. The initial approach was similar to a Nissen fundoplication or hiatal hernia repair in the mobilization of the stomach and observation of the diaphragmatic crura. The pars flaccida was opened using a combination of blunt dissection and ultrasonic scalpel utilized to complete the dissection posterior to the stomach to allow for full observation of both the right and left crus. The short gastric arteries were taken down using the ultrasonic scalpel and a penrose drain passed posterior to the stomach so that it could be retracted toward the left diaphragm. Five milliliters of ICG contrast was then administered intravenously by the anesthesiologist and flushed with 5–10 mL of normal saline. 5 Using fluorescent imaging to observe the contrast as it passed through the aorta and celiac trunk, further dissection was performed between the crura, revealing a tense median arcuate ligament. This was clipped lateral on both sides of the celiac axis and then transected using an ultrasonic scalpel. During this portion of the case, further administration of ICG allowed for safe dissection of the ligament away from the axis. Immediate improvement in celiac axis flow was demonstrated by repeat ICG administration and direct observation through robotic fluorescent imaging of the splenic, common hepatic, and left gastric branches. Hemostasis was confirmed. The liver retractor was removed under direct vision. The abdomen was desufflated, the robot undocked, and the ports were removed. Operative time was 157 minutes. The patient recovered well, with improvement of his epigastric pain during the postoperative period. Postoperative CTA showed improvement in the angle of the celiac trunk and duplex ultrasonography showed normalization of the peak systolic velocity. He was discharged on postoperative day 3, tolerating a full liquid diet, ambulating, voiding, and passing flatus without difficulties. He has, unfortunately, returned to the hospital on several occasions since that time with symptoms concerning for opiate withdrawal.
Discussion:
Once diagnosed, there are several basic approaches to treatment. These include stenting of the celiac artery, open median arcuate ligament release with or without celiac ganglionectomy, median arcuate ligament release with or without celiac artery dilatation, or celiac artery decompression and reconstruction. 1 Although open approaches are the most common described, improvements in laparoscopic and robot-assisted techniques as well as increasing surgeon experience with these modalities offer an opportunity to add another option to the surgeon's armamentarium. Both robotic and laparoscopic techniques have been previously reported with good results. 6,7 The use of intraoperative angiography with ICG, which has not been previously reported, offers the ability to demonstrate immediate improvements in celiac axis flow as well as aiding in an otherwise risky dissection by clearly observing the location of the aorta and major branches while they are still concealed by other tissues. Although the use of intraoperative ICG contrast has been described on numerous occasions in the neurosurgical literature and in determining the viability of wound healing, or flap survival, there is a paucity of examples of its use in the intraperitoneal field. We describe here the manner in which it might be utilized to further minimize complications for the described surgical procedure.
No competing financial interests exist.
Runtime of video: 6 mins 47 secs
Presented at the Society for American Gastrointestinal and Endoscopic Surgeons (SAGES) Annual Meeting, March 23, 2017, Houston, TX.


Get full access to this article
View all access options for this article.
