Abstract
Introduction:
Left cardiac sympathetic denervation is a proposed treatment for patients with life-threatening ventricular arrhythmias, such as catecholaminergic polymorphic ventricular tachycardia (CPVT). This treatment is reserved for patients who remain symptomatic despite medical management with beta blockade and who have had frequent firings from their implantable cardioverter defibrillator (ICD), given reports of ICD failure, and possible negative psychological impacts of frequent firings in children. 1 –4 Unlike the procedure for hyperhidrosis, which only involves the ligation of T2 to T4 ganglia, cardiac sympathectomy also requires the partial resection of the stellate ganglion. 1 This raises the threshold for ventricular fibrillation. 5 This video shows the use of left thoracoscopic cardiac sympathectomy for ventricular arrhythmias in two patients.
Materials and Methods:
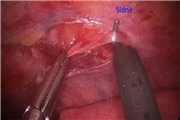
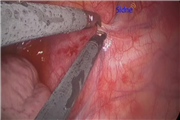
This video presents two cases of patients with refractory ventricular arrhythmias. The first case is of a 14-year-old male with CPVT and history of multiple syncopal episodes. He continued to have symptoms despite medical management with beta blockade and thus underwent an ICD placement, which resulted in frequent firings. He underwent a left thoracoscopic cardiac sympathectomy. The patient was placed in the right lateral decubitus position, and defibrillating pads were placed in the event he went into ventricular tachycardia during the procedure. Three 5-mm ports were placed: the camera port was in the fifth rib space just anterior to the scapula, and two 5-mm working ports were placed in the mid axillary line in the fourth and sixth rib space. The sympathetic chain was identified and dissected out proximally toward rib 2 and distally toward rib 5. Lidocaine was then injected into the sympathetic chain to avoid cardiac dysrhythmias during the resection. The distal sympathetic chain was then resected using electrocautery just distal to the T4 ganglion. The stellate ganglion was then identified by dissecting proximally to just above the second rib. Lidocaine was again injected into the stellate ganglion and it was resected using clips and scissors. It is important to avoid using electrocautery near the stellate ganglion as it may damage the entire ganglion and result in Horner's syndrome. A red rubber catheter was then used to evacuate the air from the chest as the lung was being reinflated. The second case is of a 13-year-old female with left ventricular hypertrophy, CPVT, and history of a previous cardiac arrest. Like the previous patient, she had persistent syncopal episodes despite beta blockade and had multiple ICD firings. She underwent the same procedure as already described.
Results:
Both patients had resolution of their ventricular arrhythmias without any further symptoms and ICD firings.
Conclusions:
Left thoracoscopic cardiac sympathectomy was used to effectively treat life-threatening cardiac arrhythmias in two of our patients. Key points of the procedure are properly identifying the stellate ganglion, which is just above the second rib, partially resecting the stellate ganglion without the use of electrocautery as it may damage the remaining segment and lead to Horner's syndrome, and also performing a T2 to T4 ganglionectomy.
Todd A. Ponsky, is on the Conmed Advisory Board. For the other authors, no competing financial interests exist.
Runtime of video: 4 mins 14 secs

Get full access to this article
View all access options for this article.
