Abstract
Introduction:
Tracheoesophageal fistula (TEF) is a common congenital anomaly of the respiratory tract, which is seen in ∼1 in 3500 live births. Typically, TEF occurs with esophageal atresia (EA) and may be associated with other congenital heart or genitourinary anomalies as part of the VACTERL or CHARGE syndromes. 1 Common complications after EA and TEF repair include esophageal stricture (35%), anastomotic leak (16%), and recurrent fistula (3%). 2
Materials and Methods:
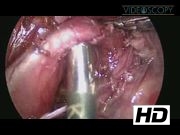
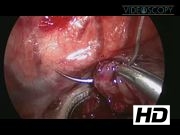
Standard TEF repair: The standard TEF repair begins by positioning the patient in a semiprone position with 40°–45° of rotation. Three ports are utilized for optimal control and observation. First, the azygous vein is identified and ligated. During dissection of the esophagus, it is crucial to avoid damaging the vagus nerve, which can be seen near the lower pouch. Often, a preoperative bronchoscopy with insertion of a guidewire can help identify the fistula for accurate ligation. Subsequently, the anesthesiologist can aid in identification of the upper pouch by inserting a red rubber catheter and pushing on it, so that a small opening can be made in the upper pouch. Finally, the lower and upper pouches are brought together in an interrupted anastomosis, beginning at the posterior layer then advancing a transanastomotic nasogastric (NG) tube before completing the anterior layer. After 5–7 days, a contrast study should be used to check for leakages before allowing oral feeds. Staged TEF repair: In this case, a 1.5 kg baby with a TEF presented in unstable condition and not fit for single stage repair. The first repair was an open procedure performed at an outside hospital and included fistula ligation with gastrostomy. In this procedure, the lower pouch was tacked onto the prevertebral fascia with Prolene suture to allow for continued growth of the lower pouch and easier identification in subsequent procedures. We returned after 6 months to finish the repair using a thoracoscopic approach. After dissecting the lower pouch from its tacking on the prevertebral fascia, the upper pouch is also dissected apart and an opening is made in it. As with the standard repair, the interrupted anastomosis of the lower and upper pouches is performed over a transanastomotic NG, beginning posteriorly and then finishing anteriorly. A staged repair may also be indicated in cases with a long gap between the upper and lower pouches. In these instances, the fistula is first ligated then given several months to hopefully elongate. The interfistula length may be measured with coronary dilators. If the vertebral distance is less than four units, a repair is possible. Larger distances require alternative approaches, such as a gastric tube or gastric pull-up. 3
Results and Conclusions:
Thoracosopic approaches are preferred over open repair because of reduced long-term musculoskeletal complications, reduced trauma to the surrounding structures, better observation and identification of the fistula, and less pain for the patient.
No competing financial interests exist.
Runtime of video: 5 mins 22 secs

Get full access to this article
View all access options for this article.
