Abstract
Introduction:
Several reports have emphasized the relative rarity of coexistence of hiatal hernia in patients with achalasia. 1 –4 Nevertheless, clinicians should be aware that esophageal disorders can coexist and may present challenges if not identified early. The esophagus should be fully investigated whenever possible to plan the most appropriate surgical technique from a range of various options. Failure to identify coexistence of achalasia in patients undergoing hiatal hernia surgery may have undesirable outcomes. 5 We assume that failure to identify hiatal hernia or predisposition to hiatal hernia in patients undergoing surgery for achalasia may have the same long-term undesirable consequence. A recent study has devised a method to measure in vivo esophageal hiatal surface area using multidetector computed tomography (MDCT) reconstruction. 6 Strong correlation between large hiatus and occurrence or predisposition to hiatal hernia has been reported. The normal size range for the hiatal surface area has been established. This methodology is potentially being used to guide decision making in antireflux surgery technique preoperatively.
Materials and Methods:
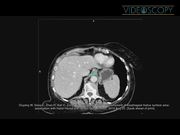
A 66-year-old female presented with achalasia. Preoperative instrumental assessment revealed megaesophagus, a narrow esophago-gastric junction with “bird-beak” appearance, poor emptying of barium. As part of preoperative assessment, thoracic computed tomography was performed to assess the severity of chronic pulmonitis developed because of the prolonged presence of achalasia and recurrent pneumonia. To assess the hiatal surface area, a double-oblique-corrected plane demonstrating the entire circumference of the esophageal hiatus was obtained using the standard technique. 6 Results showed abnormal widening of the hiatal surface area (386 mm2). Based on that, it was assumed that the patient has high predisposition to hiatal hernia. Laparoscopic Heller's myotomy, cruroplasty, and full posterior fundoplication were performed.
Results and Conclusions:
The duration of operation was 135 minutes. The postoperative period was uneventful. The patient was discharged on the fourth postoperative day. After six months of follow-up, the patient showed full relief of the symptoms. The patient gained 5 kg in weight. To our best knowledge, this is the first report on application of a method of in vivo esophageal hiatal surface area measurement using MDCT in patients with achalasia. The method is thought to be advantageous by aiding in identification of widening of the hiatal surface area preoperatively, hence providing information for the decision of most appropriate surgical technique. Little guidance exists on the most appropriate surgical technique for the achalasia associated with hiatal hernia or enlarged hiatal surface area. In our case of a female patient with achalasia associated with enlarged hiatal area (386 mm2), we performed laparoscopic Heller's myotomy, cruroplasty, and full posterior fundoplication, which resulted in permanent long-term positive results. We believe that the already mentioned technique would be appropriate for patients with achalasia associated with hiatal hernia or in isolated hiatal surface area enlargement; although cohort studies are required before any recommendations could be made. Nevertheless, we strongly advise that preoperative or intraoperative measurement of hiatal surface area using validated techniques should routinely be performed before the surgery for achalasia. 7 –9
No competing financial interests exist.
Runtime of video: 6 mins 6 secs

Get full access to this article
View all access options for this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
