Abstract
Introduction:
Type 2 diabetes mellitus (T2DM) and obesity are often associated and represent a complex health problem with debated medical management. Laparoscopic sleeve gastrectomy has gained a great consensus because of its efficacy, and no significant postoperative morbidity. In this report, we describe this relatively recent technique of bariatric surgery.
Description of the Video:
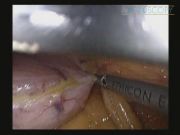
00:05—The pneumoperitoneum is performed by Veress needle in the left subcostal region. The optical trocar is positioned at ∼15 cm from the ensiform apophysis on the median. Three trocars of 12 mm were respectively placed on the left pararectal region, right, and right subcostal region, and another trocar of 5 mm was inserted in the left paraumbilical region under laparoscopic vision. 01:20—Marking is performed on the large gastric curve at 6 cm from the pylorus. From this site, there is the progressive skeletrization of the greater curvature with ultrasonic scalpel, and then the sectioning and coagulation of the vessels with release of the gastric fundus to the left diaphragmatic pillar are carried out to dissect the gastrophrenic ligament. 01:55—After placement of an orogastric probe (32F), there is a vertical sectioning and suturing of the stomach (sleeve resection) on the guide of the probe with a Echelon 60 stapler (charged green and blue) up to the His angle. 02:55—Finally, a nasogastric and an abdominal drainage in aspiration is placed. After removal of the anatomical piece, trocars are removed under vision, and the surgical mini-incisions are sutured.
Materials and Methods:
The laparoscopic procedure presented was performed in a 56-year-old man, in Obesity Class II with uncontrolled T2DM, at the Department of Digestive Surgery and Liver Unit, St. Maria Hospital, Terni, Italy.
Results and Conclusion:
At the end of 1-year follow-up, the excess weight loss was 59.2%, and the BMI decreased from 36.2 to 29.8 kg/m2. The preoperative HbA1C value was 7.5% reduced to 5.2% after 1 year from surgery without the use of medications and below the threshold defined as remission of diabetes by the American Diabetes Association. LSG is a safe bariatric technique, quick to perform, and able to greatly increasing the quality of life of patients by determining not only the achievement of a proper weight, but also the improvement in metabolic parameters until remission of T2DM. 1
The authors state that none of the authors involved in the manuscript preparation has any conflicts of interest toward the manuscript itself, neither financial nor moral conflicts. In addition, none of the authors received support in the form of grants, equipment, and/or pharmaceutical items
.
Runtime of video: 3 mins


Get full access to this article
View all access options for this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
