Abstract
Introduction:
Ischemic colitis (IC) is the most common form of bowel ischemia. One of the chronic complications of IC is stricture formation. Symptomatic ischemic strictures can be dilated by colonoscopic techniques. Colonic perforation is an uncommon complication of colonoscopy, which mandates emergent surgical intervention. This is the first report of laparoscopic colectomy for treatment of colonoscopic perforation in a patient with a segmental ischemic stricture.
Materials and Methods:
A 52-year-old man with chronic constipation underwent diagnostic colonoscopy 4 months back, which revealed a long segment of stricture with normal overlying mucosa at splenic flexure of colon. Histopathologic examination was in favor of benign pathology. After failure of medical treatments in resolving obstructive symptoms, he was scheduled for elective colonoscopic dilatation of stricture. During the procedure the patient developed severe abdominal pain. The gastroenterologist was suspicious of colonic perforation. Chest and abdominal X-rays showed free peritoneal air. Emergency surgical consultation was performed. On examination, the vital signs were stable. He had diffuse abdominal guarding and tenderness. After obtaining the informed consent, he was scheduled for emergent laparoscopic exploration under general anesthesia 2 hours after colonoscopy.
Results:
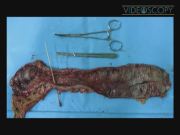
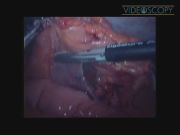
The surgeon stood at the right site of the operating table. Four ports (three 10 mm and one 12 mm) were inserted. After creation of pneumoperitoneum with the Veress needle, the first 10-mm port for the 30-degree laparoscope was inserted at umbilicus. Other working ports for hand instruments were placed at right lower, left lower, and right upper quadrants. Initial exploration revealed free intra-abdominal fluid without fecal soilage. Bowels were distended due to ileus. Working space and quality of images were limited due to guarding of abdominal muscles, distension of bowels, and presence of free fluid. The site of stricture was at proximal part of descending colon. Perforation was located at proximal part of this segment just at splenic flexure. It was necessary to perform left colectomy with removal of stricture and perforation. Left colon was mobilized through lateral to medial approach. Mesentery of left colon and its vasculatures was divided with aid of LigaSure vessel sealing system (Valleylab, Boulder, CO). Splenic flexure of colon and gastrocolic omentum were also dissected. After completion of dissection and mobilization of colon, the distal part of sigmoid was transected with laparoscopic linear stapling device (endo-GIA; Covidien, Norwalk, CT). The proximal colon was extracted through a 5-cm abdominal incision. The transverse colon was cut proximal to the stricture, and anvil of the circular stapler was fixed with purse string suture in the proximal end of colon. Then, the colon was returned back to the abdomen. The anastomosis was created with EEA circular stapler (Covidien). The anastomosis was checked with air insufflation into the rectum with the repair underwater to ensure the absence of leakage. The abdomen was thoroughly irrigated and the port sites were closed. There was no blood loss and no perioperative morbidity. Postoperative course was uneventful. Final histopathologic report was in favor of colonic stricture in the setting of previous IC.
Discussion:
Colonic perforation is a rare complication of colonoscopy that can rapidly progress to fecal peritonitis and sepsis, and may lead to death. Perforation may occur through a variety of mechanisms, including heat application at the polyp site, direct mechanical trauma from the tip of the colonoscope, lateral pressure from the side of a bowed endoscope, and pneumatic injury from over-insufflation of a stenotic area. 1 The traditional treatment of colonoscopic perforation is explorative laparotomy with primary repair or bowel resection, with or without stoma. Recently, some case reports and small series of laparoscopic repair of colonoscopic perforations have been reported. 1 –3 However, most of them have reported primary repair of colonic perforations after colonoscopic polypectomy. To my knowledge, there is no published report of laparoscopic colectomy for treatment of colonoscopic perforation in a patient with a segmental ischemic stricture. Previous reports demonstrated that early laparoscopic management of colonoscopic perforation is effective and safe. This minimally invasive approach has a low complication rate, decreases postoperative pain and the hospital stay, and makes an iatrogenic complication more acceptable to the patient. This may also reduce the related legal issues related to this iatrogenic complication of colonoscopy. 1 –3
No competing financial interests exist.
Runtime of video: 5 mins 43 secs

Get full access to this article
View all access options for this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
