Abstract


Objective:
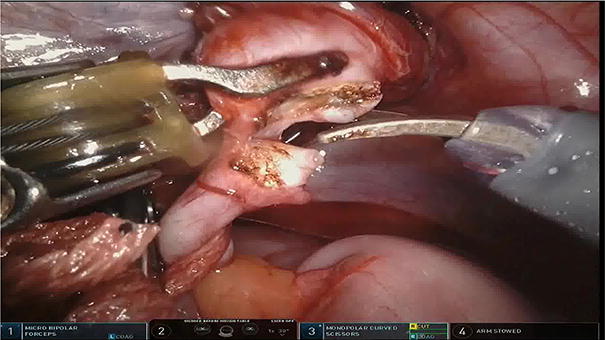
To describe the utilization of a novel surgical technique for the treatment of bilateral vesicoureteral reflux (VUR) and ureterovesical junction (UVJ) obstruction named robot-assisted laparoscopic dismembered extravesical cross-trigonal ureteral reimplantation (BI-RADECUR).
Methods:
Nine patients between the ages of 15 and 120 months who were diagnosed with bilateral VUR or obstructive megaureter (OM) underwent BI-RADECUR.
The patients were positioned in low lithotomy position, and a urethral catheter was inserted. Three 8 mm robotic ports and an assistant 10 mm laparoscopic trocar are introduced. The right and left ureters are identified and dissected. Stumps are closed utilizing PolydioxanoneUS- Ultrasound endo-loop. We tried to spare any manipulation on the dorsal–medial aspect of the distal ureter close to the UVJ in order to minimize possible injury to bladder innervation to avoid postoperative urinary retention. Excisional tapering when required was performed on a 10 cm length 8F Nelaton catheter. The ureter is closed utilizing 4-0 V-LOC™ suture. Wide transverse detrusorrhaphy approximately 5 cm in the posterior–inferior aspect of the bladder was made. Ureter–bladder anastomosis is performed utilizing interrupted 4-0 Maxon sutures. Following the completion of the lower part of the anastomosis, a JJ stent is inserted, and the anastomosis is completed. The ureter–bladder anastomosis on both sides is completed utilizing an anchoring suture at the lateral most point of the detrusor channel in order to avoid sliding of the ureter from the anti-refluxing channel and ureter kinking. Detrusor is closed utilizing 4-0 V-LOC™ suture. The first interrupted suture is placed in V fashion in order to avoid ureteral sliding. The technique that is described here provides the advantage of achieving a long tunnel mimicking the Cohen cross-trigonal ureteral reimplantation, without performing the open surgical technique and offers the potential benefits of minimally invasive surgery. Surgical technique is described, and demographic data and intra-postoperative parameters are reported.
Results:
The study included 9 patients operated between 2016 and 2022. Six patients (66%) had VUR, and the remaining 3 (44%) patients were diagnosed with OM. Median age at surgery was 33 months (IQR 16-80) and median weight was 13 kg (IQR 9.5-18) (Fig. 1). Median operative time was 120 mins (IQR 100-120). Intracorporeal excisional tapering was performed in 3 (33%) patients. Median postoperative stay was 2 days (IQR 1-3). Grade I-II Clavien–Dindo complications occurred in 2 patients. One had Grade I complication (fever), and 1 had a Grade II complication (urinary tract infection) (Fig. 2). Surgical success was achieved in 89% of cases. Urethral catheter was removed on the following day. None of the patients developed acute urinary retention.
Stents were removed 6 weeks after surgery. Follow-up US was performed at 3 and 6 months after stent removal and demonstrated significant improvement in hydronephrosis and only mild ureteral dilation. None developed UVJ obstruction or required salvage surgery. One patient with primary bilateral Grade V VUR upon surgery demonstrated recurrent Grade III reflux on one side and Grade II on the contralateral side. She underwent a successful endoscopic correction of VUR utilizing Vantris due to parent’s request (Fig. 3).
Conclusion:
Robot-assisted cross-trigonal ureteral reimplantation with intracorporeal tailoring is safe, feasible, and reproducible.
Patient Consent Statement:
Author(s) have received and archived patient consent for video recording/publication in advance of video recording of procedure.
No competing financial interests exist
.
The authors state that they have no affiliations with or involvement in any organization or entity with any financial interest or non-financial interest in the subject matter or materials discussed in this article.
Runtime of video: 5 mins 17 secs.
Demographic Data.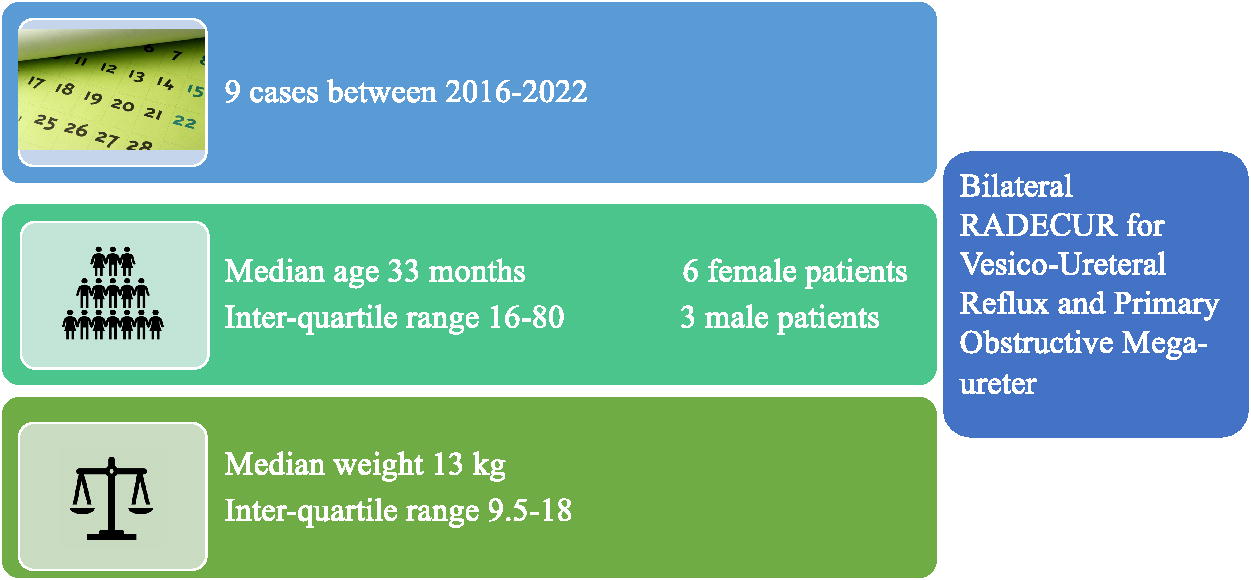
Intraoperative and Postoperative data
Intraoperative and Postoperative data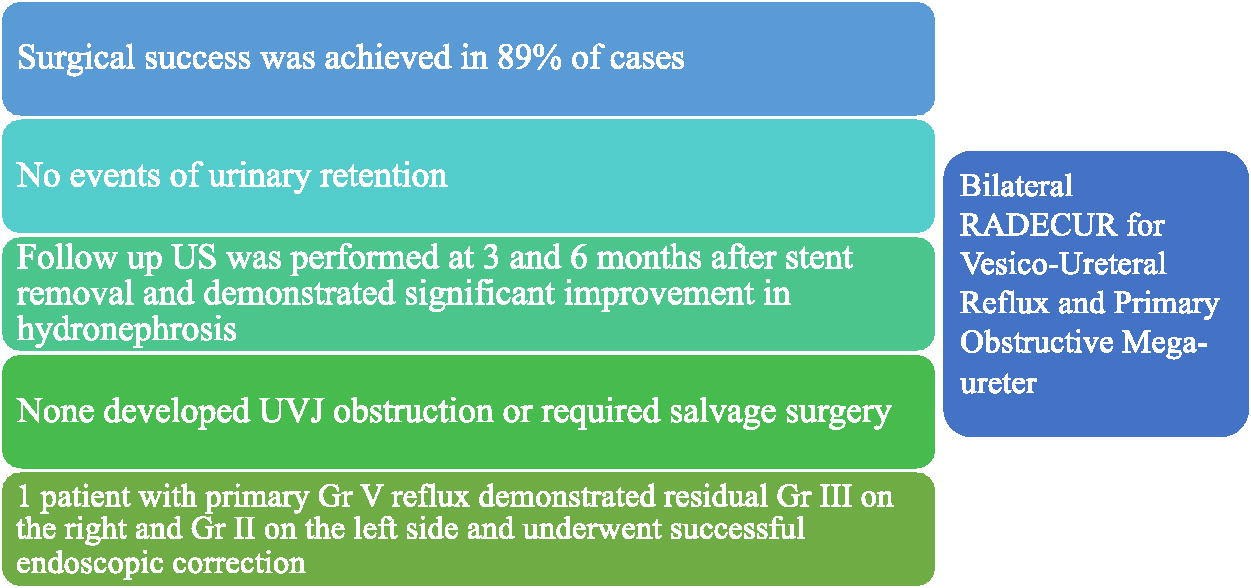
Get full access to this article
View all access options for this article.
