Abstract
Introduction:
Radical cystectomy (RC) is a complex procedure with a non-negligible morbidity. Decrease in complications may be achieved by implementation of enhanced recovery programs, but adoption of minimally invasive approaches may also contribute to it. 1 In addition, patients seem to have similar long-term oncologic outcomes and health-related quality of life. 2,3 After the increase of robot-assisted RC, there was an uptrend performing urinary diversions intracorporeally, which may provide benefits in terms of smaller incisions, reduced pain, and decreased bowel mobilization, contributing to reduced complications. 4,5 There are few reports of laparoscopic intracorporeal ileal conduit urinary diversion (ICUD). 6 –8 This is considered to be a challenging procedure, because of advanced suturing. However, because of increased costs of robotic platforms, pure laparoscopy still prevails in many countries and may be the only alternative to open surgery. Standardization of this technique could reduce surgical difficulties dramatically and provide minimally invasive approach benefits.
Objective:
To describe our step-by-step technique and provide tips and tricks for laparoscopic intracorporeal ICUD after RC.
Patients and Methods:
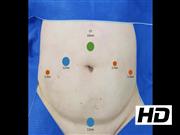
We describe a surgical technique and outcomes of all patients who underwent a standardized intracorporeal ICUD after RC in a single tertiary hospital. Surgical technique: patients are placed in Trendelenburg position and ports are inserted in a diamond configuration, with an additional assistant trocar introduced just superior to the pubic symphysis. A 15–20 cm of distal ileum is harvested. Bowel division and side-to-side anastomosis are executed with a 60 mm laparoscopic stapler through suprapubic port. Open stump is closed through pararectal port with an additional 60 mm load. A straight needle is brought through the anterior abdominal wall, passed through the distal end of ileal conduit, and then brought back to the anterior abdominal wall, inspired in “marionette technique.” 9 This stitch stabilizes bowel in a comfortable position to make ureteroileal anastomosis. Then, both ureters are opened and spatulated. Separate ureteroileal anastomosis is performed using 4.0 absorbable sutures according to the Bricker technique. Before anterior wall suture of each anastomosis, a single-J stent is inserted through the suprapubic port and grasped through the ileal conduit. Finally, stoma site is incised and a Babcock clamp is inserted under direct vision for ileal conduit traction. Stoma maturation is completed and an abdominal drain is positioned.
Results:
From 2018 to 2021, we performed a total of 20 laparoscopic radical cystectomies. A total of six patients underwent standardized intracorporeal ICUD. There were no intraoperative complications. Intracorporeal ICUD median operative time was 96 minutes (interquartile range [IQR]: 111.5–92). Median hospital stay was 7 days (IQR: 6–14). Four patients (66%) had minor complications (Clavien 1–2) within 30 days. Most frequent complication was urinary tract infection (50%). Just one patient was readmitted for intravenous antibiotics. There were no major complications (Clavien 3–5). No ileal conduit-related early complications occurred, such as anastomotic leakage, stenosis, or necrosis. Ureteroileal stenosis arose unilaterally in just one patient (8.3%).
Conclusion:
Laparoscopic intracorporeal ICUD is a challenging but feasible procedure. Standardization is crucial to minimize operative time and to achieve satisfactory outcomes. Further comparative studies with open and robotic approaches are warranted.
No competing financial interests exist.
Runtime of video: 8 mins 17 secs
Ethical Approval and Consent: Research was conducted ethically in accordance with Declaration of Helsinki. Informed consent was obtained from the patient.

Get full access to this article
View all access options for this article.
