Abstract
Introduction:
Roughly 70% of prostatectomies were accompanied by pelvic lymph node dissection (PLND) in 2010–2011. 1 PLND can provide staging information that may help further determine extent of disease and guide subsequent treatment. 2 Symptomatic lymphoceles after robot-assisted laparoscopic prostatectomy with PLND occur in 2%–15% of patients depending on the extent of the node dissection. 3 Lymphoceles can lead to significant morbidity resulting from infections and recurrence. The best treatment option for pelvic lymphoceles resulting from PLND has not been defined. Conservative management with sclerosis and percutaneous drainage is often used as an initial management strategy. Subsequent surgical excision can be challenging because of significant scarring from failed conservative attempts.
Materials and Methods:
Three prostate cancer patients treated with robot-assisted laparoscopic prostatectomy with bilateral PLND developed recurrent infected bilateral lymphoceles despite long-term antibiotics. They were referred to our institution after multiple failed attempts at sclerosis and percutaneous drainage by interventional radiology. All three elected to proceed with robot-assisted laparoscopic lymphocele excision with intraperitonealization. Standard prostatectomy port placement was used for the procedure. We have selected one of the cases to highlight our technique for robot-assisted intraperitoneal excision of the symptomatic lymphoceles.
Results:
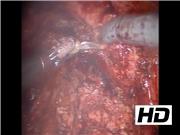
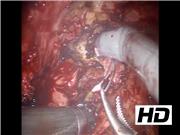
Extensive adhesions are often present from prior prostatectomy and treatment attempts. Identifying landmarks, preoperative imaging, and intraoperative ultrasound can help guide dissection. Excision of the medial lymphocele wall and surrounding fibrotic tissue is essential to prevent recurrence. Lateral wall excision and argon beam coagulation should be performed with great care to minimize the risk of damage to the iliac vessels and obturator nerve. Instillation of dye into the bladder is useful in confirming bladder integrity at the end of the case. Dye can also be injected into percutaneous drains, when present, at the beginning of the procedure to help locate and delineate the lymphocele walls, thereby facilitating complete surgical excision. This is a descriptive video of our technique that has been performed on a total of three patients. None have had a recurrence to date. Because of the rarity of this procedure, no statistical analysis was calculated.
Conclusion:
Repeated attempts at sclerosing and drainage of pelvic lymphoceles should be limited to minimize formation of scarring and fibrosis. Identification of landmarks, preoperative imaging, and intraoperative ultrasound are key for finding lymphoceles and avoiding damage to surrounding structures. Dye injection can be helpful in localizing the lymphoceles as well as confirming bladder integrity. Aggressive excision of the medial lymphocele wall is necessary to achieve adequate intraperitonealization. The internal surface of the external lymphocele wall should be cauterized to minimize the risk of recurrence. Finally, laparoscopic marsupialization is associated with low recurrence risk and may be an appropriate upfront treatment option. Transposition of omental flap into the marsupialized lymphocele may further prevent recurrence. Peritoneal flaps have been used at the time of node dissection to prevent development of symptomatic lymphoceles.
This study adhered to Institutional Review Board protocols at our institution and informed consent was obtained by all subjects included in the study.
The authors have received and archived patient consent for video recording/publication in advance of video recording of procedure.
No competing financial interests exist.
Runtime of video: 6 mins 43 secs
Video abstract presented at the 97th Annual Meeting of the South Central Section of the American Urological Association.

Get full access to this article
View all access options for this article.
