Abstract
Introduction and Objective:
Renal caliceal diverticula often present a significant management challenge for the urologist. Although not all caliceal diverticula present with symptoms, patients may experience a wide range of symptoms including persistent flank pain, recurrent infections, and even hematuria. Currently, a variety of effective management techniques are utilized for symptomatic caliceal diverticula, including ureteroscopic approaches, percutaneous approaches, and robotic/laparoscopic approaches. However, precise localization of the diverticular neck poses a significant challenge in many cases, particular when ureteroscopic localization is attempted. The diverticular neck can often be pinhole sized and, therefore, not apparent on ureteroscopy even with careful inspection. For ureteroscopy cases in which the diverticular neck is not easily observed, the “blue spritz” technique is a simple technique that enables the surgeon to localize the diverticulum using readily available colored dye agents. A minor modification that involves injection of a 50:50 mixture of methylene blue and iodine contrast allows for fluoroscopic confirmation of filling of the diverticulum, and also further accelerates the localization of the diverticulum with fluoroscopic guidance.
Materials and Methods:
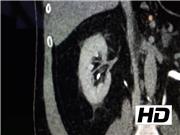
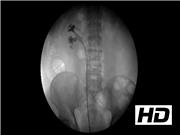
To demonstrate this technique, we have selected a 63-year-old male with a 1.8 cm symptomatic right interpolar caliceal diverticulum with milk of calcium deposits. He has not undergone prior treatment for the caliceal diverticulum, and presented complaining of chronic right flank pain. After thorough discussion regarding the ureteroscopic, percutaneous, and robotic/laparoscopic approaches, the patient elected to proceed with ureteroscopic management. A difficult-to-find diverticulum with a pinhole-sized neck became readily apparent once the modified “blue spritz” technique was employed, and a holmium laser incision of the diverticular neck was effectively performed.
Results:
This modified “blue spritz” technique has proven effective for diverticulum localization in a series of three ureteroscopy cases with a variety of diverticular sizes and locations. Two patients had milk of calcium deposits in the diverticulum, whereas the other patient did not. The mean age (57 years), diverticulum diameter (1.8 cm), operating time (52 minutes), and duration of follow-up (11 months) were noted. To date, all three patients have remained symptom free after ureteroscopic laser incision of the diverticular neck.
Conclusions:
The modified “blue spritz” technique appears to be an effective strategy for rapid ureteroscopic localization of any caliceal diverticulum in which fluid passes into the diverticulum on retrograde filling. The addition of a contrast agent to the colored dye agent enables confirmation of diverticular filling on fluoroscopy, and also facilitates more rapid localization of the diverticulum.
No competing financial interests exist.
Runtime of video: 5 mins 11 secs

Get full access to this article
View all access options for this article.
