Abstract
Introduction:
The role of minimally invasive surgery in pediatric urology has markedly expanded, but has not been traditionally applied to vesico-vaginal fistulae repairs in children. The current technique is feasible as an alternative approach and demonstrates the versatility of laparoscopy in reconstructive urology.
Materials and Methods:
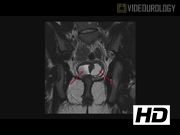
The patient is a 15-year-old postmenarchal female with uterus didelphys, bilateral hematocolpos, distal partial vaginal agenesis, and a vesico-vaginal fistula diagnosed on both clinical examination and MRI. She initially presented with urinary retention and a history of cyclical, recurrent menouria. The procedure began with cystoscopy, vaginoscopy, and bilateral ureteral catheterization. The fistula was clearly identified endoscopically. The patient then underwent laparoscopic vesico-vaginal fistula repair and repair of the distal partial vaginal agenesis with buccal mucosal vaginal reconstruction.
Results:
The patient tolerated the procedure well. There were no complications. The patient was discharged on postoperative day 2 in stable condition. In follow-up, the patient was voiding well with a well-healed buccal mucosal graft and excellent cosmetic outcome.
Conclusions:
Laparoscopic vesico-vaginal fistula repair is a safe and viable option for children with vesico-vaginal fistulae. The mobilization attained laparoscopically facilitated the vaginoplasty by minimizing the defect gap to be bridged with buccal mucosa. The procedure also avoids the morbidity associated with a larger abdominal incision. The procedure offers benefits associated with minimally invasive surgery: improved cosmesis, less pain and morbidity, and a potentially rapid recovery.
No competing financial interests exist.
Runtime of video: 5 mins 23 secs
Get full access to this article
View all access options for this article.
