Abstract
Introduction and Objective:
Symptomatic calyceal diverticula, particularly those containing stones, are simple anatomic problems that often require complex surgical solutions. Calyceal diverticula can present with intractable pain, hematuria, and recurrent infections. Techniques ranging from extracorporeal shockwave lithotripsy to open extirpative surgery have been applied to treat diverticula with varying success, although percutaneous approaches have become the primary minimally invasive therapy. However, anteriorly oriented diverticula or those that have failed percutaneous or ureteroscopic therapy present a management dilemma. Many of these complex patients are averse to another attempt at traditional management and are seeking a more definitive alternative. We present our series of four symptomatic women with complex calyceal diverticula who were managed using a novel robot-assisted laparoscopic diverticulectomy (RALD) technique.
Materials and Methods:
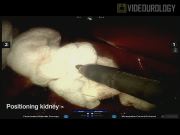
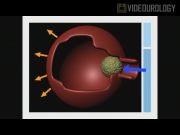
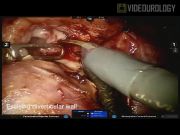
To illustrate the technique, we have selected a 22-year-old woman with a large, chronically symptomatic right upper pole posterior calyceal diverticulum. She had previously failed both ureteroscopic and percutaneous management despite being rendered stone free. She continued to have intractable pain and a large diverticular cavity remained present despite percutaneous management. Unwilling to undergo a second percutaneous approach, this patient was seeking a more definitive surgical option. The RALD technique is a modification of robot-assisted laparoscopic partial nephrectomy (RALPN) in which the diverticulum is identified by laparoscopic ultrasound and unroofed, stones are removed and the mucosa is resected in its entirety from the inside under vascular control. The ostium into the collecting system is ligated and the defect is closed hemostatically. This approach eliminates the need to resect a significant volume of normal renal parenchyma despite the endophytic nature of the diverticula.
Results:
The mean age (32 years), diverticula diameter (2.4 cm), operating time (212 minutes), blood loss (180 mL), warm ischemia time (26 minutes), length of stay (2.8 days) and duration of follow-up (7 months) were noted. Warm ischemia times were 17, 18, 28, and 39 minutes, reflecting a broad range of technical complexity. One patient had failed previous ureteroscopic management and two had failed both ureteroscopic and percutaneous approaches. The final patient had an anteriorly oriented lower pole calyceal diverticula not easily amenable to a percutaneous approach. No major complications occurred and there was no diverticula recurrence on imaging at 6 months. All patients were symptom free at their last clinic visit. Specific technical points from our full case experience are illustrated in detail in the accompanying video presentation.
Conclusions:
In our early experience, RALD appears to be effective for addressing complex symptomatic calyceal diverticula, particularly anteriorly oriented diverticula, those containing large calculi or those that have failed percutaneous and/or ureteroscopic management. Morbidity appears favorable as compared with percutaneous diverticulectomy. For surgeons facile with RALPN, the learning curve for RALD is relatively short. RALD is comparable in difficulty to robotic resection of a completely endophytic renal tumor with the caveat that finding the plane between the diverticular lining and parenchyma may be more challenging after failed percutaneous diverticular ablation. Warm ischemia times, therefore, may be slightly longer in the setting of RALD as compared with RALPN.
No competing financial interests exist.
Runtime of video: 7 mins 59 secs
Keywords
Get full access to this article
View all access options for this article.
