Abstract
Background:
Necrotizing soft tissue infections (NSTIs) are a group of rapidly progressive infections of the skin and its underlying tissue. These infections result in substantial morbidity and mortality. The focus of this study was to determine if obesity is associated with a worsened clinical outcome or prolonged hospital course for patients with NSTIs.
Patients and Methods
: We conducted a retrospective chart review of patients with NSTI presenting to a single tertiary hospital. Fat content, measured with body mass index (BMI) and abdominal fat thicknesses, including subcutaneous and visceral fat, were compared against primary and secondary outcomes of NSTIs.
Results:
We found that women had a higher mortality rate compared with men (27% vs. 15% mortality). Women also had an increased subcutaneous abdominal fat thickness (55.7 vs. 36.9 mm, p = 0.028). However, no measurements of fat, BMI, subcutaneous fat, or visceral fat differed between survivors and mortalities of NSTIs. In fact, with the exception of a higher BMI in those who developed acute kidney injury (AKI, p = 0.034), we found no correlation between increases in fat measurement and secondary outcome, including propensity to develop sepsis during hospitalization, length of hospital stay, length of intensive care stay, or antibiotic usage. Multivariable logistic regression analysis was conducted, and we found no statistically significant differences in primary or secondary outcomes.
Conclusion:
Women appear to have a higher mortality in NSTI, although the reasons for this are unclear. Obesity, as measured by BMI, subcutaneous, and visceral fat thicknesses, does not appear to be an independent risk factor.
Necrotizing soft tissue infections encompass a wide variety of infections characterized by rapidly progressive necrosis of the skin and underlying soft tissues. They can be further divided by tissue layer, such as necrotizing fasciitis when involving fascia or myositis when involving muscle, or by anatomic location, such as Fournier gangrene when present in the genitalia and perineum [1–4]. These infections are polymicrobial up to 80% of the time, with a predominance of group A Streptococcus (GAS), Staphylococcus aureus, Enterococcus, and multiple anaerobic bacterial species [2,5–7].
Necrotizing soft tissue infections (NSTIs) appear to be increasing across the United States. According to a 2014 study, an estimated 500 to 1,500 cases are reported each year in the United States [8]. A California burn center saw an increase of more than 300% in the annual NSTI incidence over an eight-year period, from 23 patients in 2000 to 72 patients in 2008 [2,9]. A recent U.S. Centers for Disease Control and Prevention (CDC) report analyzing skin and soft tissue infections (SSTI), which includes cellulitis and necrotizing fasciitis, revealed that rates were higher for those living in the southern and western United States, as well as in metropolitan areas [10]. Although the specific causes of NSTIs are still not understood completely, there is suspicion that they may be linked to an increase in community-acquired methicillin-resistant Staphylococcus aureus infections (MRSA) as well as an increase in select comorbidities, such as diabetes mellitus, obesity, immune compromised states, and vascular diseases [2,3,10–12].
Obesity is a common comorbidity in patients with NSTI as previous studies have observed [8,11]. In this exploratory, descriptive, single-center study, we hypothesized that obesity would be associated with increased mortality in NSTIs, and that gender differences in fat distribution may be associated with a higher mortality in women. By focusing on the role that gender and body habitus plays in outcomes from these infections, we hope to provide clinicians with a better way to identify patients at an increased risk of major complications or death throughout their hospital course.
Patients and Methods
After obtaining approval from our Institutional Review Board, a retrospective chart review was performed on patients with NSTI admitted to the University Medical Center (UMC) in Lubbock, Texas, between January 1, 2010 and March 31, 2018. Use of computed tomography (CT) imaging was based on clinical judgement of the emergency department physician and surgical team evaluating the patient; there is no standard protocol for its use in this scenario.
The UMC is the only American Burn Association-verified burn center servicing the surrounding western Texas and eastern New Mexico areas. As such, patients with necrotizing infections are transferred routinely from critical access hospitals in the region for higher-level care. Diagnosis of NSTI was determined using ICD-9 code 728.86. information, including age, body mass index (BMI), comorbidities, primary and secondary clinical outcomes, was collected using an encrypted data sheet.
Patients who had received an abdominal CT as part of their NSTI evaluation were included in subset analysis of abdominal fat with outcome. Two components of abdominal fat were measured, subcutaneous and visceral fat. The subcutaneous fat thickness of the abdominal wall was measured on CT at the L4/L5 lumbar vertebra as identified by the most superior aspect of iliac crest, as described previously [13,14]. Two measurements were made using the electronic medical record's measurement tool on the abdominal pannus, on either side of the vertebra. These two measurements were then averaged to obtain the value used in our statistical analysis. Visceral fat was measured from anterior peritoneum to anterior edge of L5, as previously described [15,16]. Figure 1 illustrates how these measurements were completed.
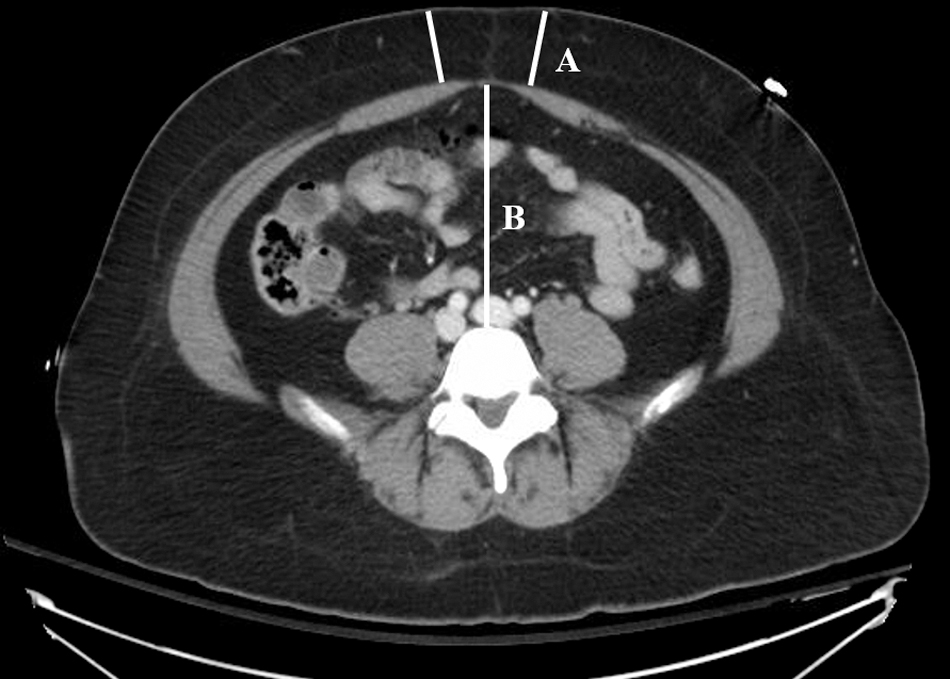
Subcutaneous and visceral fat measurement on computed tomography (CT) scan. Representative image of measurement of fat thickness at L4/L5 region. (
Statistical analysis
The demographics, clinical characteristics, and main and secondary outcomes were summarized across the comparison groups (gender and BMI groups) in descriptive statistics such as mean (standard deviation [SD], 95% confidence interval [CI]), median (interquartile range [IQR]), and count (percentage) as appropriate depending on the examined variable level of measurement. The associations among categorical parameters was tested in an unadjusted analysis using Pearson χ2 or Fisher exact tests. Independent sample t-test and Mann-Whitney U test were used in an unadjusted analysis to examine differences between the comparison groups on continuous and ordinal level parameters as as appropriate. The association among continuous variables was assessed using Spearman ρ correlation coefficient. For the adjusted analysis, a multivariable logistic regression model was fit to predict the relation between the primary outcome (mortality) and the examined obesity variables in this study (BMI, subcutaneous, and visceral fat thicknesses).
Possible confounders, total number of comorbidities, duration of antibiotics, length of hospital stay (were controlled for by building them into the logistic model, and odds ratios with 95% CI were calculated. All the predictors and covariates entered in the logistic regression model are on the continuous level of measurement. Statistical significance was set at 0.05.
Results
A total of 51 (58%) men and 37 (42%) women met selection criteria and were included in the study. Patient demographics are provided in Table 1 and 2. Of these 88 patients, all had BMI information, but only 42 received abdominal CT on admission, and thus only those 42 patients were included in the visceral and subcutaneous fat thickness analyses. The average patient in our study was age 48.8 (95% CI 45.5–52.1) years with an average BMI of 35.7 (95% CI 32.6–38.9). The majority of the study cohort was Caucasian (58%), followed by Hispanic (39%), and black (2%). The most common site for the NSTI was in the lower extremity (39%) followed by the upper extremity (22%). Infections confined to the trunk shared similar frequency, with 19% on the perineum, 15% on the abdomen, and 14% on the buttocks. The average number of comorbidities in the patient cohort was two with an IQR of 1–3.
Cohort Summary: Male versus Female
χ2 test.
Fisher exact test.
Independent sample t-test.
Mann-Whitney U test.
Hemoglobin A1c < 7%.
Hemoblogin A1c ≥7%.
SD = standard deviation; IQR = interquartile range; CHF = congestive heart failure; COPD = chronic obstructive pulmonary disease; CAD = coronary artery disease; LOS = length of hospital stay; ICU = intensive care unit.
All data reflect unadjusted analysis.
Cohort Summary: Obese versus Not Obese
χ2 test.
Fisher exact test.
Independent sample t-test.
Mann-Whitney U test.
Hemoglobin A1c < 7%.
Hemoblogin A1c ≥7%.
SD = standard deviation; IQR = interquartile range; CHF = congestive heart failure; COPD = chronic obstructive pulmonary disease; CAD = coronary artery disease; LOS = length of hospital stay; ICU = intensive care unit.
All data reflect unadjusted analysis. Overweight/obese is defined as BMI >25.
The pre-existing medical conditions most commonly identified among the patients were hypertension (55%), smoking (43% current smokers and 6% past smokers), and diabetes mellitus (62%), with 38% considered uncontrolled with a hemoglobin A1c ≥ 7% and 24% considered controlled with an hemoglobin A1c < 7%. Other identified comorbidities were pre-existing renal failure (13%), chronic obstructive pulmonary disease (11%), coronary artery disease (11%), congestive heart failure (10%), and alcohol abuse (2%). The demographics were similar to those of previous studies [2,17,18].
We found women had a worse outcome compared with men. Women suffered nearly double the mortality rate as men (27.2% vs. 15.7%), although the results were not statistically significant. The cohort of women had an increased average BMI compared with men, which was not statistically significant (37.2 and 33.2, respectively, p = 0.087). Women had statistically increased subcutaneous fat thickness on CT scans compared with men (average of 55.7 mm and 36.9 mm, respectively, p = 0.032). Women and men did not differ in visceral fat thickness (average of 143.1 mm and 138.9 mm, respectively, p = 0.77).
We then wanted to determine if this increased fat content mattered in survival from NSTI. Fat measurements, using BMI, subcutaneous fat, or visceral fat measurements did not differ among the clinical outcomes of survival or death. The average BMI of patients who died was 34.3 kg/m2 (95% CI 32.6–39.4 kg/m2) compared to a BMI of 36.0 kg/m2 (95% CI 27.1–41.5 kg/m2, p = 0.65) in survivors. When looking at subcutaneous fat thickness, we found that those who died had an average of 42.5 mm (95% CI 21.8–63.2 mm) of umbilical fat compared 45.8 mm (95% CI 35.7–55.9 mm, p = 0.79) in survivors. Results for visceral fat thickness were similar: 139 mm (95% CI 125.3–153.3 mm) in survivors compared with 146 mm (95% CI 95.0–196.11, p = 0.7241) in mortalities. To ensure that this negative result was not simply because of a lack of normal weight individuals in our study, we also looked at whether our normal weight patients carried a different mortality risk. We found that that normal weight (BMI <25 kg/m2, n = 25) patients actually had a higher mortality rate compared with overweight patients (n = 63), 25% and 19% mortality, respectively, although results were not significant. Overall, fat content did not differ based on the primary outcome of survival versus mortality.
Conversely, BMI showed a statistically significant impact on the development of an acute kidney injury (AKI) during hospitalization, with an average BMI of 40.2 kg/m2 in those who developed AKI compared with 33.6 kg/m2 in those who did not (p < 0.05). Body mass index did not impact the development of sepsis (p = 0.76). Subcutaneous fat content did not differ with the development of either AKI or sepsis during hospitalization (p = 0.41 and p = 0.34, respectively). Similarly, visceral fat content also did not differ between with and without AKI or sepsis event (p = 0.8283 and p = 0.399, respectively)
When comparing fat content with secondary outcomes, we found no correlation (Table 3). There was no correlation between hospital length of stay, intensive care unit (ICU) length of stay, number of days patients received antibiotic agents for their infections, or the number of comorbidities compared with BMI and abdominal fat measurements. None of these secondary outcomes correlated with either BMI or abdominal fat measurements from CT scans (R2 value range, 0.0033–0.1667).
Fat Measurements Do Not Correlate with Secondary Measurements (R 2 values)
BMI = body mass index; LOS = length of stay; ICU = intensive care unit.
All predictors in the multivariable logistic regression model were not significant. Table 4 shows the multivariable logistic regression results with odds rations and 95% CI.
Multivariable Logistic Regression Show No Significance in Secondary Outcomes
B = estimated logistic regression coefficient; SE = standard error; df = degrees of freedom; Wald = Wald χ2 statistic; OR = odds ratio; CI = confidence interval; BMI = body mass index.
Discussion
In this study, we expanded on the observation that women have a worse outcome after an NSTI compared with men [19,20]. We found that women had nearly twice the mortality rate of men (27.2% vs. 15.7%). Although not statistically significant, this awareness bears clinical significance.
Because obesity has long been thought of as a comorbidity in infectious processes [21,22], and obesity has proven to be detrimental to women's health [23], we wanted to see if increased fat content could account for this increased mortality in women. However, BMI has been criticized as an unreliable estimation of fat content in the body. Thus, in addition to BMI, we also looked at both subcutaneous and visceral fat thicknesses on CT scans in our study, and this has been shown to be a more accurate approximation of total fat content [13–16]. This is the first study to utilize these tools to determine if obesity is a factor in NSTI clinical outcome.
We first confirmed that in our cohort, women did indeed have an increased fat content in the abdominal region in comparison with men. However, we found no difference in BMI or either of our abdominal fat measurements between survivors and non-survivors (primary clinical outcome). When analyzing secondary outcomes, we found that an increased BMI was associated with a statistically significant increased propensity toward development of AKI, which is consistent with previous reports [24,25]. However, analysis based on abdominal fat thickness did not reflect this finding. Subsequently, we found that neither BMI nor abdominal fat thickness was correlated with any secondary clinical outcomes, including hospital lengths of stay (LOS), intensive care unit LOS, and length of antibiotic use. Multivariable logistic regression was conducted to confirm these findings. Although surprising, this is not the first report of a lack of relation between obesity and post-surgical infection [26,27].
The major limitation of this study was the small sample size. This is an exploratory-descriptive single center study. Obtaining a larger sample size is difficult for a single-center study because of the rarity of NSTIs [28]. A multicenter study with a larger sample size is required to be more decisive about the trends and generalizations in the target population.
If obesity does not explain the observation that women with NSTIs have an increased mortality, further investigation into other plausible explanations is warranted. We are interested in wound locations and the microbes that are associated with the wounds from specific locations (such as perineum and buttock regions where gut microbes can easily infect the wound) and if there are differences between men and women in this respect. Expanding our sample size would also be helpful in further dissecting differences between survival and mortality. A deeper understanding into the cause of increased mortality in women with NSTIs will prove crucial in attempts to provide more effective and targeted treatment to patients with NSTI.
Conclusion
Necrotizing soft tissue infections remain a serious surgical emergency because of increasing incidence over the last several years and the high associated morbidity and mortality. Although patients with comorbidities seem to be affected by NSTIs more often than patients without chronic medical conditions, we did not find one condition or comorbidity to be a statistically significant factor in NSTIs. Overall, our study revealed that mortality in women was nearly twice that of men and that women had more subcutaneous fat compared with men. Neither BMI nor abdominal fat content influenced NSTI outcomes. Future studies with larger sample sizes are needed to confirm and expand on our findings. In addition, exploration into the impact of body location and the microbiology of NSTIs is needed to further understand factors that may be impacting clinical outcomes.
Footnotes
Acknowledgments
The authors wish to thank the Clinical Research Institute at Texas Tech University Health Sciences Center for help with IRB approval and data analysis. We also thank the Texas Tech University Health Sciences Center Burn Center of Research Excellence for stimulating meeting discussions, from which projects such as this arise.
Funding Information
No funding was received for this article.
Author Disclosure Statement
The authors have no conflicts of interest to disclose.
