Abstract
Background:
Communication and interpersonal skills are essential medical components of oncology patient care. Patients and families rely on physicians for treatment, expertise, guidance, hope, meaning, and compassion throughout a life-threatening illness. A provider's inability to empathize with patients is linked to physician-related fatigue and burnout. Because oncology training programs focus on teaching evidence-based medicine and clinical acumen, little time may be dedicated to professional development and acquisition of interactive skills. Traditional communication courses typically include two components: formal, knowledge-based learning skills, which are gained from didactic lectures, and role-playing, which usually occurs in small groups. We report the implementation of a novel longitudinal communication curriculum for trainees in Oncology.
Materials and Methods:
At a single-center institution, an innovative communication curriculum titled “REFLECT” (Respect, Empathy, Facilitate Effective Communication, Listen, Elicit Information, Compassion, and Teach Others) was implemented for radiation oncology residents and medical oncology fellows to improve and refine physician/patient interactions. All oncology specialty residents and fellows were eligible to participate in this communication curriculum. The curriculum emphasized a reflective process to guide trainees through challenging scenarios.
Results:
Since October 2018, this comprehensive course consisted of quarterly (four hour) workshops comprising assigned reading, knowledge assessments, didactic lectures, expert guest lecturers, standardized patient simulations, role-playing, patient/expert panels, coaching, reflective writing, and debriefing/feedback sessions. The curriculum provided longitudinal communication training integrated with the learners' daily physician/patient encounters rather than occasional isolated experiences. Fifteen workshops have been completed. Each focused on navigating challenging situations with patients, loved ones, or colleagues.
Conclusions:
Future directions of the curriculum will entail improving the communication skills of oncology trainees and gathering communication improvement data to assess the program's success formally.
Background
Physicians have a critical and multifaceted role in patient and family interactions. Elements discussed include diagnosis, prognosis, management options, goals of therapy, and toxicity. 1 In addition, they must deliver clear medical information, navigate patient and family emotional reactions, and talk openly with patients about end of life when necessary. Although physicians face challenging encounters and clinical experiences daily, they may lack the appropriate affective and interpersonal communication skills and empathy to be successful in the clinical arena. Medical education is an active and transformative progression of professional identity development, which can be strengthened by reflection.2,3 When learners see behaviors or values that differ or contradict what is taught within a formal curriculum, reflection can promote more profound understanding, continuous learning, and personal growth. Medical reflective writing has been utilized to encourage critical and organized thought of various moral, ethical, and social contexts in patient care. 4 This reflective process can enhance physicians' abilities to evaluate patients and allow caregivers to connect with the human condition, improving empathy and communication skills. 5
Because oncology training programs focus on teaching evidence-based medicine and clinical acumen, little time is dedicated to professional development and acquisition of interactive skills. Therefore, communication courses may enhance a physician's bedside manner. Communication courses typically include two components: formal, knowledge-based learning skills from didactic lectures and role-playing, usually in small groups. 6 Traditionally, clinical skills are developed through peer/expert observations. 7 To date, courses have been developed to teach oncology learners communication skills, focusing on challenging conversations. For instance, Oncotalk is a communication course focusing on prognostication and delivering bad news. 8 However, this sporadic type of learning is limited by several factors. Abbreviated communication courses are often limited in scope and disconnected from situational learning. Contrary to these common learning courses and seminars, the REFLECT curriculum creates a framework for multiple skills to be incorporated into memory through repetition and recalled into clinical practice. We report on implementing the REFLECT communication curriculum for radiation oncology residents and medical oncology fellows at a single institution.
Materials and Methods
The authors implemented an innovative, concurrent, but separate communication curriculum for radiation oncology residents in 2018. Given their interest, the program was expanded to include medical oncology fellows. The curriculum is titled REFLECT, which stands for Respect, Empathy, Facilitate Effective Communication, Listen, Elicit Information, Compassion, and Teach Others (Fig. 1). Involved radiation oncologists and medical oncologists chose workshop topics to cover various clinical scenarios an oncologist may encounter. The primary goal of this program was to blend aspects of palliative medicine into oncology training. In addition, the REFLECT curriculum uses reflective processes to strengthen a trainee's comfort with challenging scenarios.2,3 The Wald and Reis “REFLECT ‘best practice’ rubric (Reflection Evaluation For Learners' Enhanced Competencies Tool) was used as a guide for creating this novel communication curriculum. 9
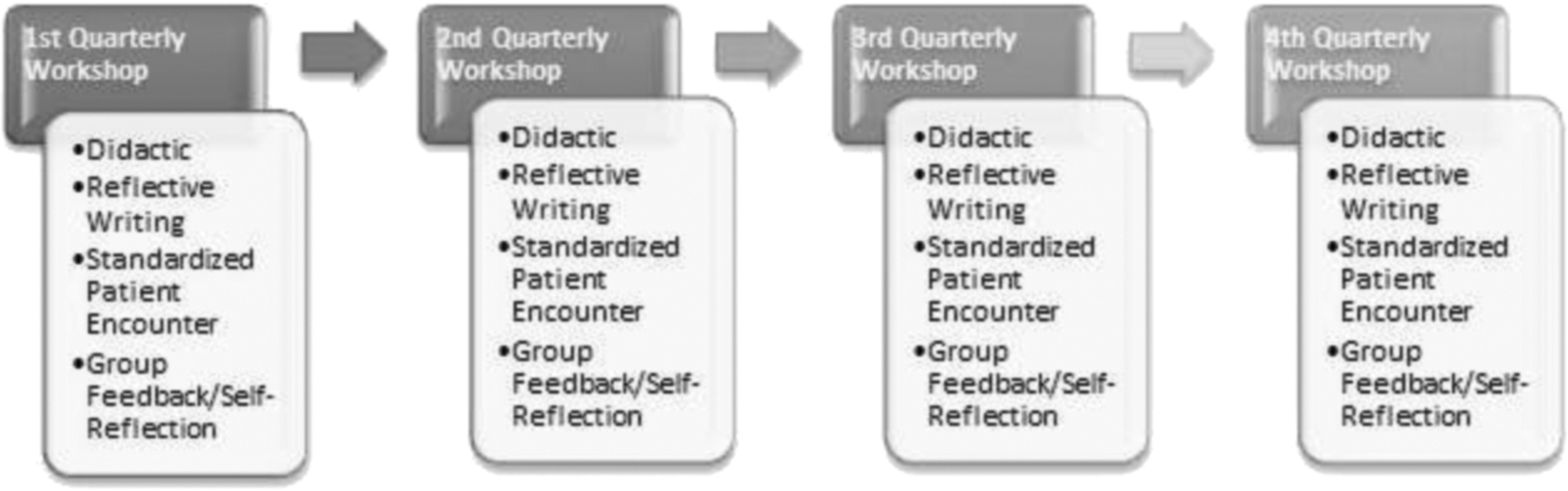
REFLECT Curriculum Design consisting of quarterly workshops. REFLECT, Respect, Empathy, Facilitate Effective Communication, Listen, Elicit Information, Compassion, and Teach Others.
All new oncology specialty residents and fellows were eligible to participate in this communication curriculum. As part of the future goals of the education curriculum, the authors sought to design studies that would evaluate the communication skills of trainees participating in the program. To proceed with studying the impact of the curriculum, The Mayo Clinic Institutional Review Board approved this prospective trial.
Results
This curriculum consisted of (1) comprehensive quarterly (four hour) workshops, including regular Standardized Patient (SP) simulations and feedback, and (2) longitudinal curriculum participation throughout the continuum of the oncology training program. This approach would facilitate opportunities for growth, clinical analysis, and new communication proficiency. Reflections on learners' encounters and professional development were expected to be continuous rather than isolated occurrences.
Learner-directed workshops included didactic lectures (1–1.5 hours), reflective writing exercises (30 minutes), simulated encounters with SPs (30 minutes), debriefing discussions with multiple source feedback on their patient/physician interactions from the patient/actor, peers, and mentors (1–1.5 hours). A radiation oncologist delivered didactic lectures with board certification in palliative medicine and pediatrics. Learners completed reflective exercises (30 minutes) titled “The Critical Incident” and “The High-Stakes Conversation” on meaningful clinical encounters about the relevant workshop topic. Small group reviews were performed to provide reference frameworks for the learners to identify patterns of communication that they would like to continue or abandon.
Since October 2018, there have been ∼15 workshop sessions, primarily focusing on communication skills important for oncologists. The following topics were covered: prognostication; children and adolescents with cancer; managing conflict with a colleague; patients receiving mixed messages; communication and delivery of bad news; delivering bad news- the medical error; opioid diversion; honoring patients' cultural and religious preferences in the oncology setting; and communicating with the angry oncology patient (Table 1). Topics such as delivering bad news and prognostication have been repeated, so trainees complete these sessions at least once during their training.
REFLECT Curriculum Workshop Topics
To evaluate the effectiveness of this communication curriculum, Likert scale surveys were distributed to participating trainees and faculty oncologists to analyze their perception of the program and its impact on improving trainees' communication skills. 10 Future directions include incorporating communication assessment tools to evaluate trainees' performances during workshops. The Communication and Interpersonal Rubric will assess six competencies: Respect, Professionalism and Demeanor, Self-reflection and Self-awareness, Communication, Organization and Reliability, and Giving and Receiving Feedback. The SECURE framework will be implemented to assess communication interactions to monitor the development of a resident and fellow's communication and interpersonal skills on a longitudinal basis. 11 The Emotional and Social Competence Inventory (ESCI) is a validated survey instrument that will be administered at the end of each year to formally assess the development of emotional intelligence (EI) throughout the trajectory of learners' medical education. 12 A thematic analysis of “The Critical Incident” and “The High-Stakes Conversation” will be performed.
Discussion
The American Society of Clinical Oncology (ASCO) highlighted that oncologists may have significant deficiencies in communicating with cancer patients and their loved ones regarding their diagnosis, prognosis, and treatment. 13 The authors desired to build a curriculum exposing trainees to highly complex scenarios to improve their communication skills. Our REFLECT curriculum is unique in that it is structured to be longitudinal for each resident or fellow. Other well-known communication courses, such as Oncotalk, are much shorter in duration. 8 An advantage of the REFLECT curriculum is the exposure of oncology trainees to challenging situations concurrently with their training when they acquire the most knowledge about how to best care for cancer patients.
Several factors have limited the research goals of this novel communication curriculum. The initial requirement for each trainee to sign written informed consent before formal statistical analysis delayed the formal assessment of their communication skills. Gathering written informed consent was highly challenging, especially during the COVID-19 pandemic. While the curriculum was able to continue during the pandemic, social distancing decreased learner interactions and engagement in the curriculum. As a result, attendance decreased during this period. Through working with the IRB, it has been determined that trainees provide verbal consent to be included in future studies if they participate in the communication workshops. Future studies will include trainees who participated in at least one workshop. The following steps will evaluate the importance and qualitative analysis of the curriculum's preliminary findings for future improvements as learners participate in quarterly workshops based on oncology-relevant topics. We plan to assess the presence of communication, interpersonal skills, and other competencies as the learners participate in the longitudinal curriculum. In addition, we will perform thematic analyses of multiple sequential narratives obtained throughout each learner's training course.
Our first research study of the REFLECT curriculum was a Likert scale study completed by the trainee and faculty to provide their perceptions of the REFLECT curriculum. To be included in this study, trainees needed to participate in at least one workshop. Similarly, faculty needed to observe at least one workshop. 10 In general, trainees and faculty had positive perceptions of the curriculum, but the faculty felt the communication curriculum was more impactful than the trainees. 10 Faculty may perceive a more positive impact of the curriculum as they have more experience handling challenging and complex situations where they feel the communication curriculum may have benefited their training. However, some trainees felt the curriculum was not as beneficial to their training. 10
In conclusion, the REFLECT curriculum is a novel communication curriculum incorporated into radiation oncology and medical oncology training programs. This curriculum provides an all-encompassing approach to expose trainees to various clinical scenarios so they are well prepared to navigate challenging discussions with patients and their loved ones. We plan to perform future studies to determine whether the REFLECT curriculum improves physician interpersonal communication skills.
Funding Information
No funding was received for this article.
Footnotes
Author Disclosure Statement
No competing financial interests exist.
