Abstract
Background:
Many countries have introduced a compulsory use of community masks for certain public areas during the SARS-CoV-2 pandemic. Different manufacturers offer reusable community masks in large quantities. The efficacy of these masks, however, is unknown.
Method:
We tested available community masks of major manufactures and determined the filtration efficacy using radioactive aerosol particles as well as air resistance with a vacuum measurement.
Results:
Filtration efficacy of the tested reusable community masks ranged from 34.9% ± 1.25% to 88.7% ± 1.18%. Air resistance ranged from 4.3 ± 0.06 to 122.4 ± 0.12 Pa/cm2. There was a good correlation between filtration efficacy and air resistance (Pearson correlation 0.938, p < 0.0001).
Conclusions:
Filtration efficacy and air resistance differ significantly between the different community masks, but the two measurements correlate well with each other within the entire test series. For optimal protection, one should select a rather airtight mask. When selecting a mask, the highest level of tolerable air resistance can be used as a selection criterion.
Introduction
Sars-CoV-2
Methods
Reusable (washable) textile community masks from manufacturers who stated that they produce large quantities of masks (>10,000/month) were examined. One mask made from nonreusable FFP fleece was included into the comparative measurements.
The community masks examined and their manufacturer's details are shown in Table 1.
Characteristics of the Investigated Masks
Examination of air resistance
DIN EN 14683: 2019-10 requires a pressure difference of <40 Pa/cm2 for the breathability of medical masks when an air flow of 8 L/min is passed over an area of 4.9 cm2 of the test membrane. We reproduced the experimental setup described in detail in DIN EN 14683: 2019-10. A pneumotachograph (SOMNOmedics, Randersacker, Germany) was connected on one side to a 4.9 cm2 measuring clamping device. On the other side of the clamping device, a pressure sensor (SEN 633; SOMNOmedics) was connected as well as an adjustable suction pump (Fina VAC B 800; Medap, Lenzkirch, Germany). Pressure and flow values were transferred to the local sleep laboratory network through WLAN (SomnoScreen Plus RC easy; SOMNOmedics) and displayed and analyzed by means of the sleep laboratory software (DOMINO® Software Package; SOMNOmedics). After clamping the respective mask cloth of the respective community mask, the negative pressure was titrated manually to achieve a flow of 133 mL/s (corresponding to 8 L/min). A total of three different masks were measured per brand.
Examination of filtration efficacy
We examined the filtration efficacy using radioactive particles. For this purpose, isotonic saline (0.9%) with 150 MBq 99mTc-diethylenetriamine pentaacetate (DTPA) per mL was nebulized with a Pari LC Sprint Star nebulizer (Pari, Starnberg, Germany) inside an airtight plastic box (Iris 70 L, model no. 135455; IRIS Ohyama, Sendai, Japan) (Fig. 1).

After a nebulization time of 20 seconds, the particles were homogeneously distributed and dried for 30 seconds using two fans installed inside the box (Fig. 1C). Water from the particles evaporates within a few seconds (<5 seconds at a relative humidity of 50% and <10 seconds at a relative humidity of 90%).(18) The MMAD of sodium chloride particles emitted from the Pari LC Sprint Star nebulizer is 2.8 μm with a geometric standard deviation of 2 μm. The drying (evaporation) process described earlier thus will result in a particle spectrum of 0.6 ± 0.4 MMAD. The box contains a clamping device for the mask cloth (Fig. 1C) corresponding to DIN EN 14683: 2019-10 with an area of 49 cm2 and a second unfiltered reference port. The test box was provided with a total of four 22 mm ventilation hose adapters (ports), which were sealed airtight into the front of the box (Fig. 1B, C). Port 1 is used to connect the Pari nebulizer. Port 2 was connected on the inside to the output of the clamping device and port 3 was connected on the inside to the unfiltered reference connection. From the outside, ports 2 and 3 were ventilated with a two-chamber artificial lung (dual adult test lung model 5600i; Michigan Instruments, Kentwood, MI; Fig. 1A), whose chambers were blocked and thus moved synchronously. Port 4 was only equipped with a filter from the outside and serves for free air circulation during the ventilation of ports 2 and 3. After aerosol nebulization and the evaporation process was completed, the artificial lungs were actuated a total of 10 times with 1 L per chamber to ventilate port 2 (stretched mask cloth) and 3 (unfiltered reference).
To collect the radioactive aerosols, two particle-tight filters (Iso-Gard No. 19212; Teleflex Medical GmbH, Fellbach, Germany) were used at ports 2 and 3 between the box and the artificial lungs. The radioactivity of the filters at ports 2 and 3 were determined using a gamma camera (ECAM Scintron; Medical Imaging Electronics GmbH, Seth, Germany). The background activity was subtracted from the filter activity, the ratio of the measured net counts from ports 2 and 3 corresponds to the filtration efficacy of the mask cloth that was clamped in each case. For each of the community masks listed in Table 1, were examined three different masks.
Statistics
We used the Shapiro–Wilk test to check for normal distribution and Levene's test for equality of variances. For multiple comparison we used analysis of variance. For pairwise comparisons we used a nonpaired two-sided t-test with Bonferroni adjustment for multiple comparisons. A p < 0.05 was considered significant. SPSS (IBM, Armonk, New York) version 26 was used for statistical analysis.
Data sharing policy
The complete data set of all measurements is available on the Mendeley data sharing platform (https://data.mendeley.com/datasets/p7djxzttzc/1).
Results
Filtration efficacy and air resistance are shown in Table 2.
Measurements
Filtration efficacy (%) and air resistance, mean ± SD.
Figure 2 shows differences in the filtration efficacy of the different community masks.
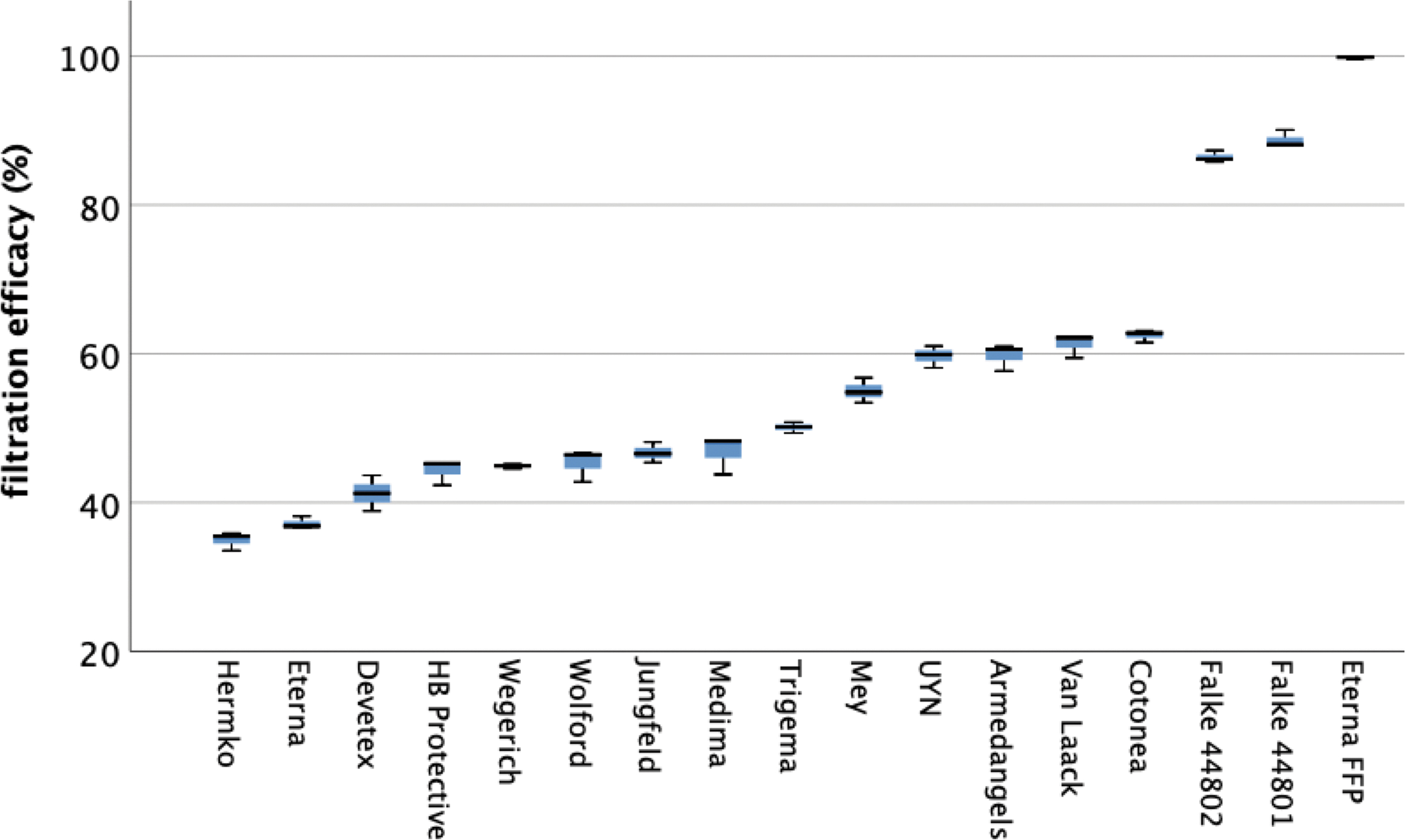
Box plot of the measured filtration efficacy. Statistics are shown in Table 3.
p-Values and Confidence Intervals
p-Values and CI for pairwise comparisons.
CI, confidence interval.
Figure 3 shows the relationship between filtration efficacy and air resistance.
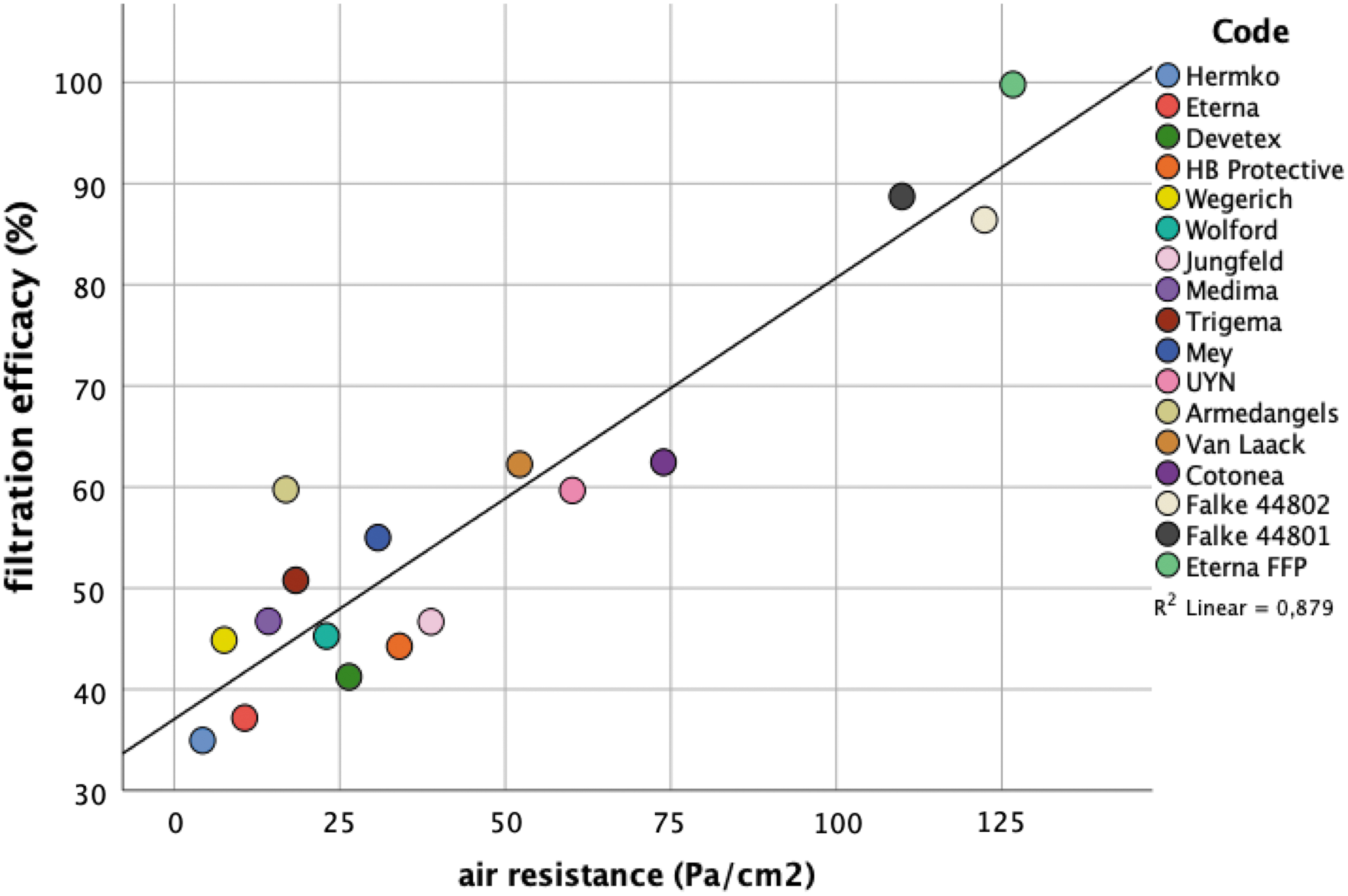
Filtration efficacy in % versus air resistance in Pascal/cm2.
Filtration efficacy and air resistance correlate closely (correlation according to Pearson 0.938. p < 0.0001).
Discussion
According to the certification requirements of DIN 14683: 2019-10, none of the tested community masks met the certification requirements (filtration efficacy >99% and air resistance <40 Pa/cm2). Since we used smaller particles as required by the DIN 14683: 2019-10 norm with direct detection of penetrated particles instead of bacterial culture growth, our setup is more rigorous and rather comparable with the DIN EN 149 or NIOSH (42 CFR Part 84) as described in the introduction of this article. However, we felt it was important to use smaller particles that remain airborne for longer periods since these particles are becoming more and more the focus of virus transmission. The filtration efficacy differs more than twofold, the air resistance even by the factor 20. Overall, one can see a very good correlation between filtration efficacy and air resistance. When it comes to filtration efficacy, the number of layers of material does not necessarily seem to be important (Table 1), but rather the quality of the fabric. Davies et al. examined various textile fabrics and nonwoven fabrics and found a wide range of measured filtration efficacies.(19) A recently published study showed that especially the weave density of a fabric influences the filtration efficacy.(20) For cotton fabrics this density is determined by the number of threads per inch (TPI). In the latter study, a cotton fabric with 80 TPI had a filtration efficacy of 14%, a cotton fabric with 600 TPI, in contrast, had a filtration efficacy of 98.4%.(20) In the case of multilayer fabrics, however, friction between the different layers can generate electrostatic forces, that may positively affect filtration efficacy.(21)
The optimal filter material has, on the one hand, a pore characteristic that prevents the passage of small aerosol particles; on the other hand, the sum of the pore cross section must be large enough to keep the air resistance low. Fulfilling these two requirements in accordance with DIN 14683: 2019-10 is very unlikely to be achieved without the effect of electrostatic forces in the filter membrane.(22) The filter effects of electrostatically charged membranes are reduced during use, whereas the air resistance remains constant. This phenomenon is best explained by a decrease in the electrostatic filter effects.(23) In particular, however, increasing moisture seems to reduce the electrostatic effects.(24,25)
The latter arises from the exhaled air and of course from the cleaning process with water. That is why membranes with electrostatic properties are deactivated and become ineffective by washing processes and thus are inapplicable for reusable masks.
The direct filter performance of the mask cloth is primarily responsible for the third-party protection component of a mask. It prevents the exhaled aerosol from spreading toward an opposite person. For self-protection, the tightness of the mask on the facial skin plays a decisive role. Investigations could show that a leak at the edge of the mask can reduce the filtration efficacy by up to 60%.(20) Mathematical models to assess the likely effectiveness of facemasks on the reproduction number (R) have highlighted the importance of the filtration efficacy.(26)
The third-party and self-contamination risk increases with the working life of a protective mask(27,28); therefore, a regular change or a regular cleaning is mandatory. It is assumed that the moisture in the mask cloth as well as the contamination rate of the mask with airborne pathogens increases significantly with longer use of the masks. Blachere et al. called surgical masks and respirators a “personal bioaerosol sampler.”(29) Infectious particles from the mask surface could be further spread by contact or re-aerosolization causing self-infection or infection of others.(27–29)
With regard to the change intervals and hygienic preparation, it is advisable not to exceed a total wearing time of 6 hours.(27) The mask should then be disinfected. Disinfectant preparation can be carried out, for example, by washing at >90°C in the washing machine or by boiling the mask for at least 5 minutes. Machine washing in low-temperature programs should be avoided due to the considerable risk of contamination.(30) After using the masks and after washing, care should also be taken to ensure that they are completely dry and protected against contamination.
Limitations
There is a huge variety of commercially produced community masks on the market and we were only able to test a small sample. However, we selected manufacturers who claimed to be able to produce large quantities. Owing to shipping restrictions during the corona pandemic our test sample was mainly restricted to brands from the country of the authors.
However, we are convinced that the general principles we explored can be applied to masks of other brands as well. Surface charge is usually not present in liquid (water-based) aerosols. However, we did not use a discharger and cannot fully exclude that filtration efficacy could have been influenced by electrostatic properties of the mask cloth. We used a particle spectrum of 0.6 ± 0.4 μm MMAD. The use of even smaller particles could have resulted in lower filtration efficacies of the community masks we tested.
Conclusion
For community masks a high filtration efficacy goes along with high air resistance and vice versa. In general, the filtration efficacy should be chosen as high as possible, taking into account the tolerance of the air resistance by the wearer. Air resistance of community mask, however, can be substantially higher as allowed for surgical masks.
Further research should focus on the development of reusable mask with electrostatic properties and cleaning procedures that conserve these properties.
Authors' Contributions
D.D. and J.K. designed the study setup and the experiments. L.M., D.P., and D.D. conducted the experiments. L.M. and D.P. extracted and collected the data. D.D. and J.K. analyzed the data. D.D. and F.G. drafted the article. All authors have read the article and agree to the publication.
Footnotes
Author Disclosure Statement
The authors declare they have no competing financial interests.
Funding Information
No funding was received for this article.
Reviewed by:
Gerhard Scheuch
Jens Hohlfield
