Abstract
As countries face public health emergencies, building public health capacity to prevent, detect, and respond to threats is a priority. In recent years, national public health institutes (NPHIs) have emerged to play a critical role in strengthening public health systems and to accelerate and achieve implementation of the International Health Regulations (IHR 2005). NPHIs are science-based government institutions that provide national leadership and expertise for the country's efforts to protect and improve health. Providing a Legal Framework for a National Public Health Institute is a recently released Africa CDC publication intended to support NPHI development throughout Africa. Here we present a legal mapping analysis of sampled legal domains for 5 countries, using the “Menu of Considerations for an NPHI Legal Framework.” The analysis delineates the types of legal authorities countries may use to establish or enhance NPHIs and demonstrates how legal mapping can be used to review legal instruments for NPHIs. It also demonstrates variability among legal approaches countries take to establish and enable public health functions for NPHIs. This article examines how the legal framework and menu of considerations can help countries understand the nuances around creating and implementing the laws that will govern their organizations and how countries can better engage stakeholders to identify or address potential areas for opportunity where law may be used as a tool to strengthen public health infrastructure.
With countries increasingly facing disease threats that transcend borders, 196 countries have agreed to implement the International Health Regulations (IHR, 2005). 1 Additionally, in 2014 the United States and several other countries initiated the Global Health Security Agenda (GHSA) to spur progress toward full IHR implementation. 2 The Joint External Evaluation (JEE) tool was developed and adopted by the World Health Organization (WHO) to help countries identify gaps and measure progress toward meeting full IHR implementation. 3 Law and policy issues are included throughout the JEE, underscoring the impact that law and policy can have on improving global health security and public health capacity. 3 As countries seek to improve capacities measured by the JEE, strengthening legal authorities can be used in multiple ways to enhance compliance with IHR obligations. 4 In particular, the national, policy, and financing capacity section of the JEE specifies the role legal frameworks can play in enabling IHR implementation. 5 While none of the 19 technical areas in the JEE tool expressly assesses the functions of national public health institutes (NPHIs), the institutes can provide a centralized platform for implementation across technical areas.
National public health institutes have emerged as playing a critical role in coordinating, developing, and strengthening public health capacities; helping countries achieve IHR implementation; and improving population health.6,7 As science-based government organizations, 8 NPHIs often serve as the focal points for efforts to protect, strengthen, and improve health, catalyzing responses to key public health challenges.9,10 Typical NPHI functions with direct implications for health security include public health laboratory and surveillance systems, emergency preparedness and response, public health workforce development, and research in public health. In addition, NPHIs often lead in developing One Health* approaches to surveillance, disease prevention, and emergency response and can also bridge the gap between clinical and public health systems.2,10,11
In 2017, the African Union created the Africa Centres for Disease Control and Prevention (Africa CDC) to support public health throughout the continent. Africa CDC has prioritized the development of strong NPHIs in all African countries and has developed guidance for countries. This includes Providing a Legal Framework for a National Public Health Institute, 12 a guidance document that includes the “Menu of Considerations for an NPHI Legal Framework.” This framework was developed in 2019 as a joint effort of the International Association of National Public Health Institutes (IANPHI), the US Centers for Disease Control and Prevention (US CDC), Public Health England, and African NPHI directors from Ethiopia, Guinea Bissau, Liberia, Mozambique, Nigeria, and South Africa.9,12 These documents underscore that development of a legal instrument that clearly defines what an NPHI will do and how it will operate within the government's structure is an important step in clarifying the NPHI's mission, governance, reporting structure, leadership, and finance and will contribute to success. 12
The legal process used to establish or restructure an NPHI varies greatly from country to country and therefore requires deliberate steps to ensure sustainability of an NPHI in the health system. Thus, the NPHI Legal Framework provides information and perspectives for countries seeking to enable their NPHIs with legal authorities. Based on in-depth consultations with stakeholders and a thorough review and analysis of existing public health laws related to NPHIs, NPHI strategic guidance documents, and legal literature,
12
the NPHI Legal Framework includes 7 core legal domains:
. Establishment: Outlines legal character and organizational identity of the NPHI I. Functions: Specifies the work to be carried out by an NPHI II. Leadership: Characterizes the leadership structure of an NPHI V. Oversight and Advisory Boards: Relates to establishment, function, operation, and membership . Accountability and Reporting: Provides a legal basis for reporting and oversight within a government's structure I. Financial Resources and Their Use: Authorizes funds and certain aspects related to their use II. Effective Date: States when the law becomes effective and any necessary preconditions
To identify these legal domains, global public health literature was analyzed and technical guidance and input from subject matter experts were sought to further refine the domains. Each domain contains legal attributes, with 140 legal attributes across all domains. The domains and attributes together provide a framework to assist in characterizing NPHI legal authorities—both the existing legal landscape and opportunities to use law as a tool to strengthen public health infrastructure, including further supporting IHR compliance. 5 In the analysis below, we provide an example of how using a legal framework can assist with systematically mapping a country's laws to identify potential gaps and provide opportunities where law may be used as a tool to strengthen public health infrastructure.
Methods
Global public health law † and policy experts from US CDC, assisted by IANPHI, conducted an initial scan of national NPHI laws ‡ enacted through April 15, 2019. Researchers selected for analysis NPHI legal instruments from 5 African countries—Ethiopia,14,15 Guinea-Bissau, 16 Liberia, 17 Mozambique,18,19 and Nigeria20,21—representative of different geographic regions and legal systems from the African continent. Copies of laws were obtained from IANPHI's online database, including translated copies of laws from Guinea-Bissau and Mozambique. Only national laws were analyzed using the NPHI Legal Framework; subnational laws, international laws, policies, national strategic plans, and other guidance documents were not included in the scope of the analyses. Researchers used legal epidemiologic methodologies5,22 to systematically review and code these national laws for the presence or absence of all legal domains and attributes included in the NPHI Legal Framework. Each of 3 reviewers independently coded laws for up to 2 countries, and then coders collectively reviewed and validated codes to ensure interrater agreement was achieved. Quality control measures were implemented to ensure coding integrity.
Analysis
While an analysis of all domains and attributes was completed, the discussion presented here focuses on domains I, II, III, IV, and V, which relate to the legal character of the NPHI, functions of the NPHI, leadership structure, accountability, and reporting. Additional details for all domains and attributes are included in the appendix (see Supplemental material at https://www.liebertpub.com/doi/suppl/10.1089/hs.2019.0093/).
Legal Character of the NPHI
Domain I, “The legal instrument establishes the NPHI,” includes attributes related to both the creation and legal identity of the NPHI (Table 1). All countries included in this review used legal authority to establish the NPHI. For example, in Mozambique, the NPHI is “endowed with legal personality, with administrative and technical-scientific autonomy.”18,19 In Ethiopia, the NPHI is an “autonomous federal government office” that has its “own legal personality.” 14 Liberia's NPHI is an “autonomous agency of the government,” 17 and Guinea-Bissau's has its own “juridical personality, endowed with technical, administrative, financial, and patrimonial autonomy.” 16 Lastly, Nigeria's NPHI is enabled as “a body corporate with perpetual succession.” 20
Legal Coding for Domain I: The Legal Instrument Establishes the NPHI
All 5 NPHIs are authorized as parastatal entities, although the definition of parastatal and the implications for oversight and use of ministry systems (eg, for hiring and finances) vary across countries. The review showed significant diversity in autonomy and, in particular, reporting to and oversight by ministries of health. Laws for Mozambique, Ethiopia, Guinea-Bissau, Liberia, and Nigeria codify relationships between the NPHIs and ministries of health or other government entities. For example, in Nigeria, the “Centre shall submit annual costed work plans relating to its functions to the Minister for approval.” 20 Liberia's law requires “proper coordination” and “sectoral reporting accountability to the Ministry of Health.” 17 Mozambique's Ministry of Health has “guardianship” of the NPHI, which includes power to inspect the structure of the NPHI and authorize and approve annual reports, programs, bodies, and activity plans. 18
Legal authorities for all 5 countries articulate public health functions and scope of duties for the NPHI. For example, Ethiopia's law provides a list of 21 specific duties, with particular emphasis on the NPHI's role in conducting public health research, 14 while Liberia's law includes broader categories, such as development and sustainability of the public health workforce, surveillance and laboratory capacity, environmental and occupational health structures, and coordinated public health and medical research. 15 Likewise, while Mozambique's law includes core “attributions” and “competencies” 16 to authorize functions and operations for the NPHI, an organic statute subsequent to the law specifies a regulatory process to clarify the public health functions of the NPHI. 17
Public Health Functions of the NPHI
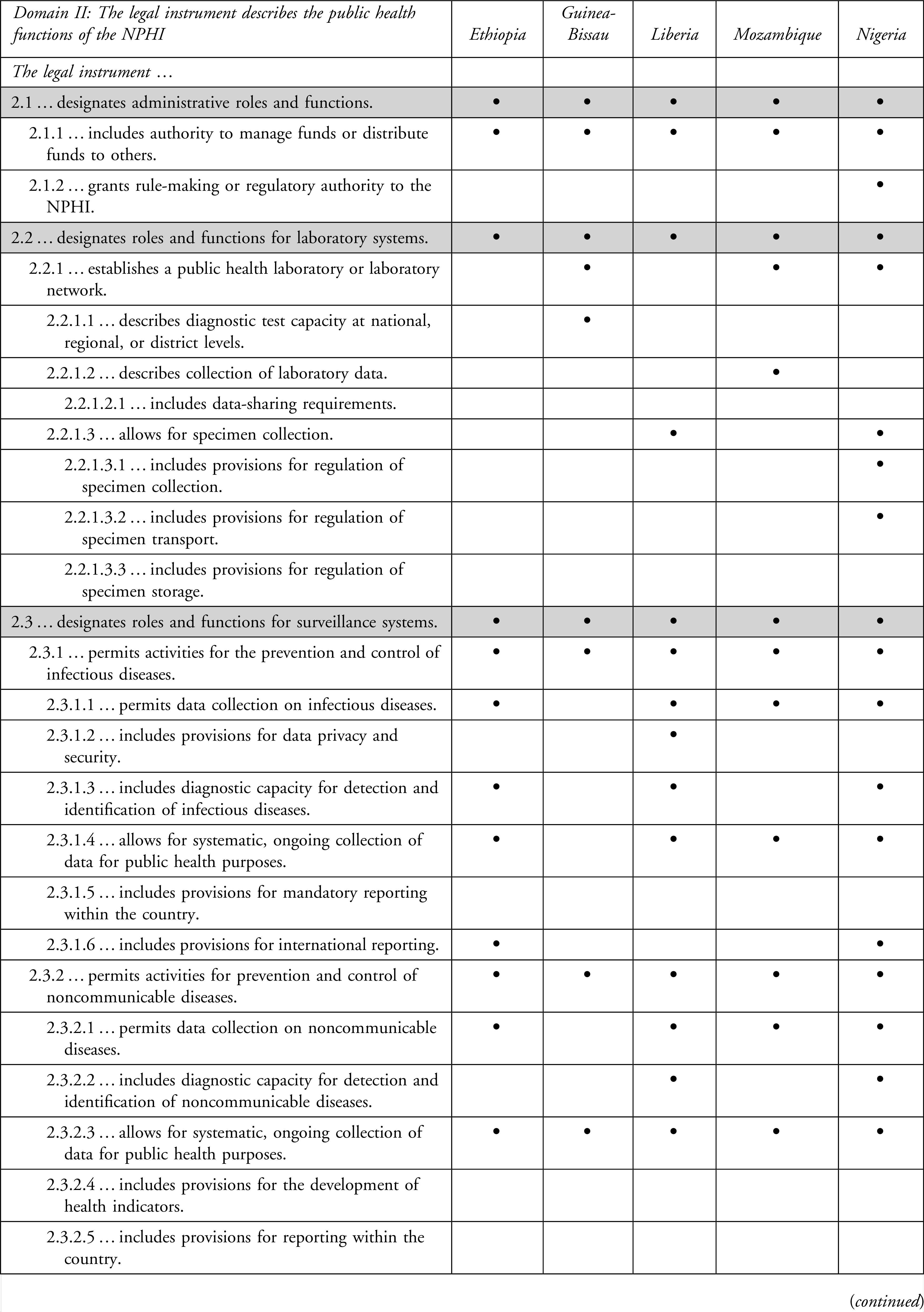
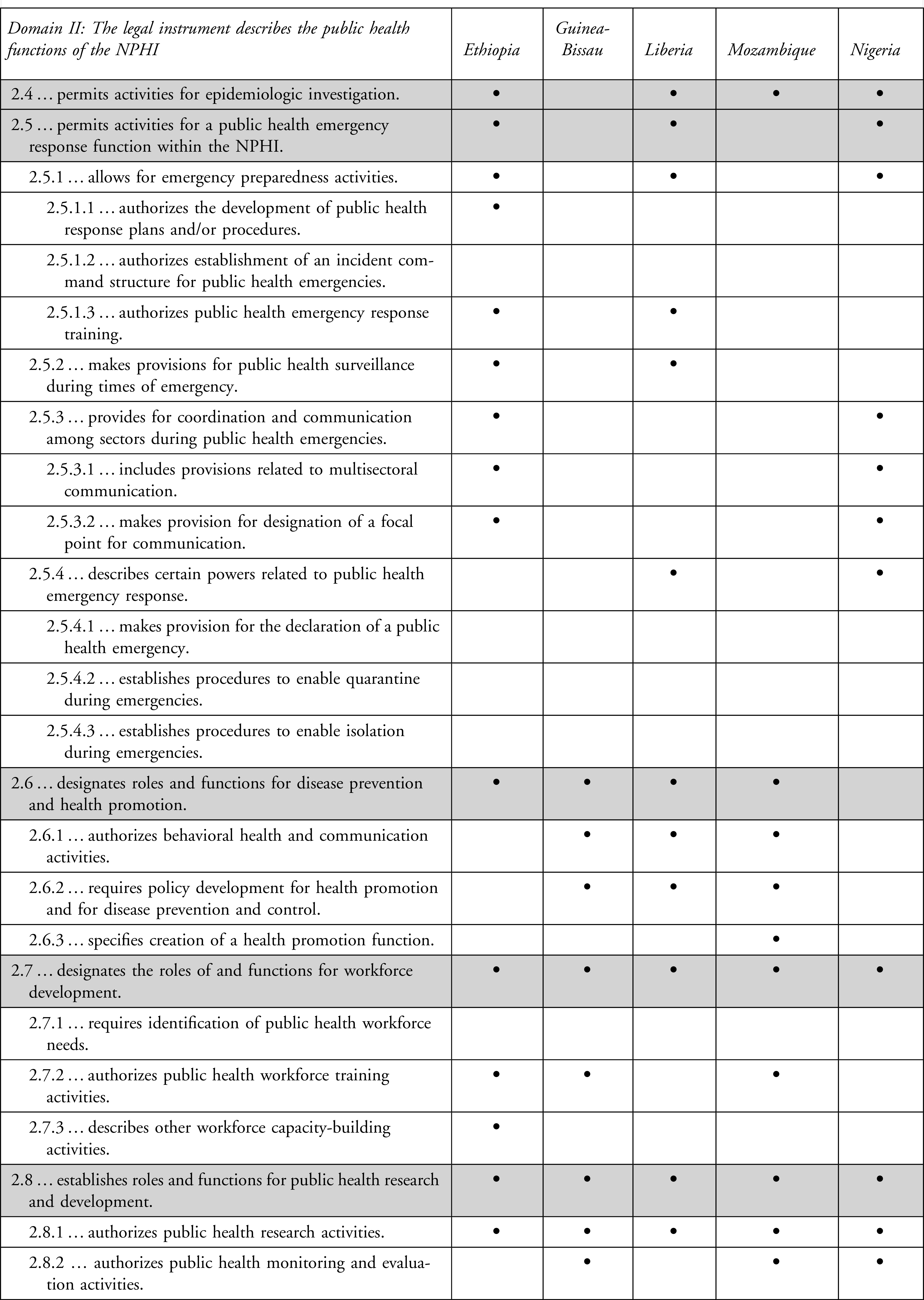
Domain II includes specific functions, including public health functions that may be legally authorized for NPHIs (Table 2). All 5 countries reviewed include authorization for the following functions: (1) administrative, (2) laboratory and (3) surveillance systems, (4) disease prevention and promotion, (5) workforce development, and (6) health research and development. Ethiopia, Liberia, and Nigeria also authorize public health emergency response.
Legal Coding for Domain II: The Legal Instrument Describes the Core Public Health Functions of the NPHI
In Ethiopia, the NPHI is directed to “design strategies, issue guidelines, develop preparedness and response plans, build capacity, establish and implement coordination and collaboration frameworks, conduct public health vulnerability assessment and risk analysis, and provide public health support to prevent and mitigate public health emergencies.” 14 This also includes authorization to conduct “… on site investigation when deemed necessary, verify outbreaks, issue alerts, provide warning and disseminate information to the concerned organizations, mobilize or cause the mobilization of resources, and support the response activities carried out. …” 14 Ethiopia also requires that there be a focal point for communication to “implement international health regulations on grave public health emergencies having implications of international crisis.” 14
Nigeria has expressly included language dedicating their NPHI as the IHR focal point. 20 Moreover, in Liberia, in addition to supporting “the health response and provid[ing] recommendations to government on control measures for disease outbreaks and mitigating health risks and hazards,” 17 the NPHI is also authorized to “recommend the declaration of public health emergency and disease outbreaks based on available public health data.” 17
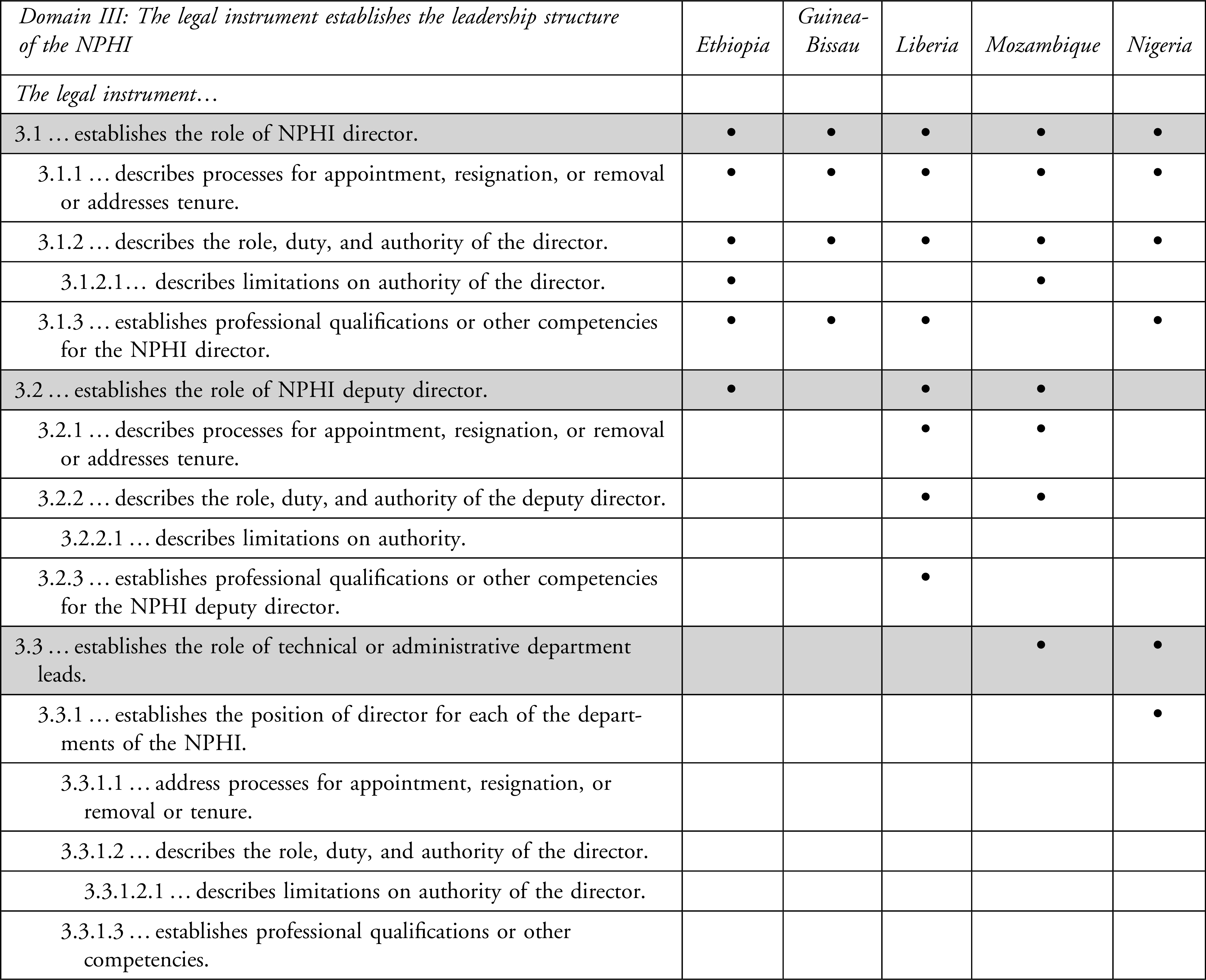
Leadership of the NPHI
Domain III describes laws related to leadership roles in the NPHI (Table 3). All 5 countries authorize an NPHI director and include legal requirements for appointment, removal, and tenure. For instance, in Mozambique, the director is “appointed by the Prime Minister, on the proposal of the Minister overseeing the area of Health.”18,19 In Liberia the “President shall, upon the recommendations of the Board of Directors, appoint the Director General.” 17
Legal Coding for Domain III: The Legal Instrument Describes the Leadership Structure for the NPHI
Laws in Ethiopia, Nigeria, Liberia, and Guinea-Bissau include qualifications or other competencies for the NPHI director. For example, in Guinea-Bissau, the NPHI director must be selected “among doctorates in medicine or related fields.” 16 Nigeria goes further, mandating that the director “shall be a health professional with at least 15 years post graduate qualification experience in medicine or public health.” 20 Only Ethiopia and Mozambique include language describing limitations on authority for the NPHI director. For example, in Mozambique, the director general shall “define the general direction of management and direct the activities of the Instituto Nacional de Saude (INS), with the vision of realizing its attributions, reporting to the Minister [of Health].” 18 In Ethiopia, the director shall, among other mandates, “… prepare a workplan and submit a budget to the Ministry of Health (d) expend resources according to the Ministry approved budget.” 14
Accountability and Reporting
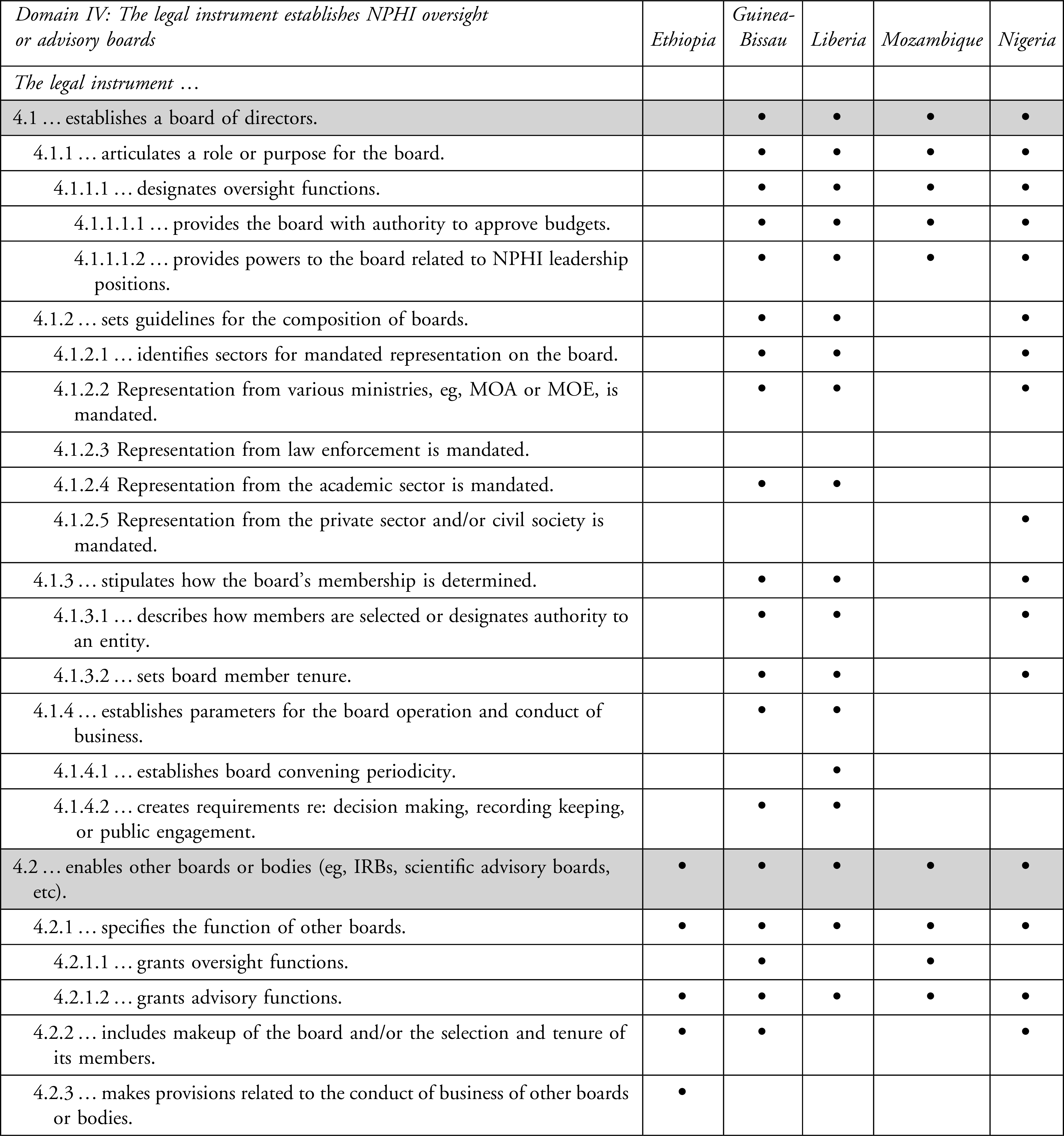
Domain IV, “The legal instrument establishes oversight or advisory boards,” and Domain V, “The legal instrument establishes accountability and reporting mechanisms,” include attributes related to oversight and accountability for NPHIs (Tables 4 and 5). Analysis of NPHI laws shows that all 5 countries have legal provisions establishing NPHI oversight or advisory boards. Four countries (Guinea-Bissau, Liberia, Mozambique, and Nigeria) have laws establishing a board of directors, further articulating a purpose or role for the board and designating oversight functions. For example, in both Guinea-Bissau and Liberia, the board of directors has oversight authority to approve or authorize budgets.16,17
Legal Coding for Domain IV: The Legal Instrument Establishes NPHI Oversight or Advisory Boards
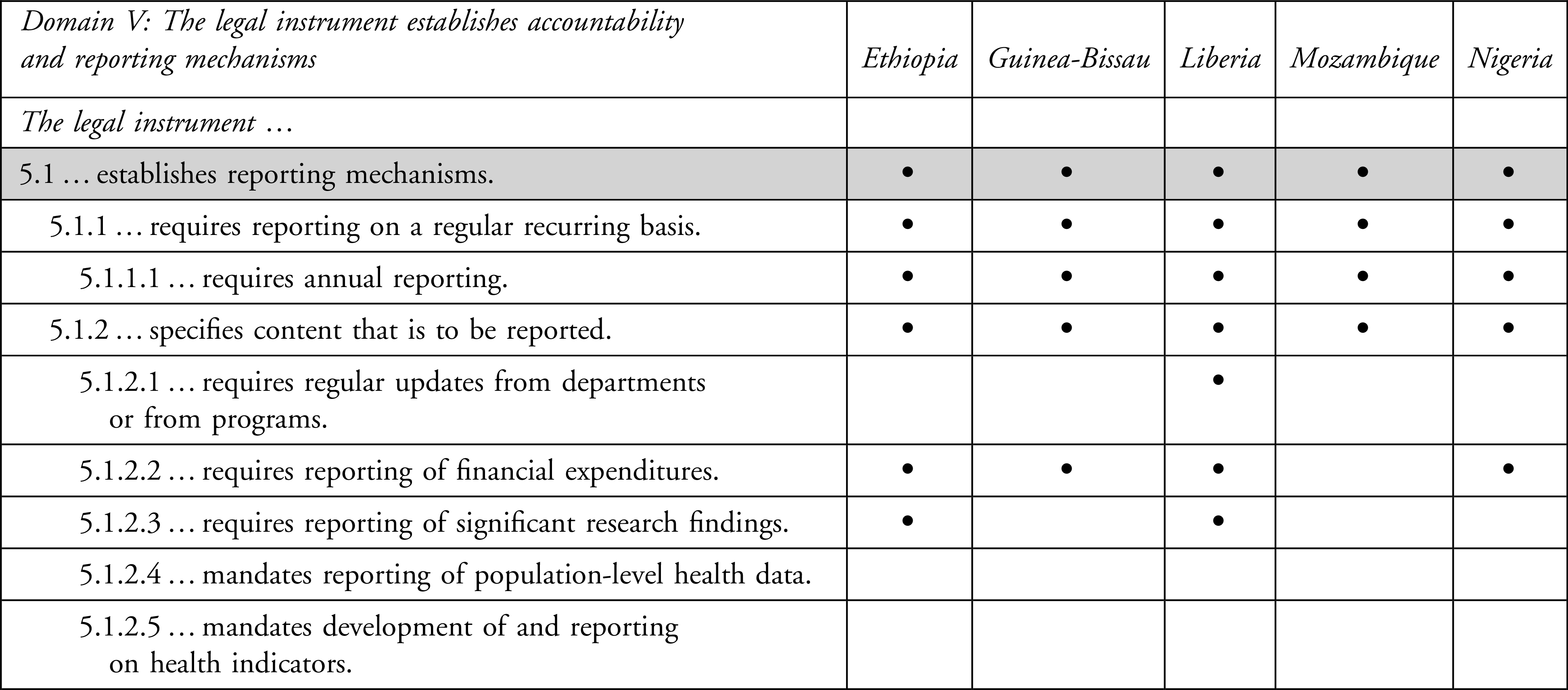
Legal Coding for Domain V: The Legal Instrument Establishes Accountability and Reporting Mechanisms
Laws for Mozambique, Ethiopia, Guinea-Bissau, Liberia, and Nigeria codify relationships between the NPHI and the ministry of health or other government entities under Domain I. The reporting mechanisms reviewed under Domain V lay out additional requirements for accountability and reporting under the law. While all 5 countries require annual reporting, they vary on the content required to be reported and the recipient of the report. For example, in Liberia, the “Director General shall submit quarterly and annually a report consisting of financial and programmatic information to the Board for onward submission to the President and Legislature.” 17 In Liberia, the minister may request the director to submit reports “from time to time on specific issues, programs, or periods.” 17 By comparison, the director in Ethiopia must “prepare and submit to the Ministry [of Health] the annual work program and budget of the institute and … (f) prepare and submit to the Ministry [of Health] the performance and financial reports of the Institute.” 14 While only Ethiopia and Liberia require reporting of significant research findings, 4 countries (Liberia, Ethiopia, Guinea-Bissau, and Nigeria) require reporting on financial expenditures.
Discussion
With the increased attention to the key role NPHIs can play in global health security and the emphasis on NPHIs by the Africa CDC, 23 there is a need for tools that help establish or strengthen NPHIs. The NPHI Legal Framework and the approach to analysis presented here are such tools. By laying out a detailed menu of considerations, the NPHI Legal Framework provides a basis for countries to establish NPHI laws and for other countries to identify gaps and opportunities in the law. 12 Because of the role NPHIs play in the overall strengthening of the public health systems, description and designation of functions helps establish the range of allowable competencies to help achieve NPHI goals and can make clearer who has the authority to act during public health emergencies. In addition, the law can articulate the legal character of the organization and how it fits into the overall government structure and can establish certain technical requirements for those that lead NPHIs.
Just as NPHIs vary widely in structure, public health functions, and attributes, the mechanisms used to establish NPHIs and the content of their laws vary. 12 For example, while Mozambique, Liberia, Guinea-Bissau, Ethiopia, and Nigeria establish parastatal NPHI structures, this is not the case for all NPHIs. Even among the countries reviewed that chose to establish parastatal structures, the review showed significant diversity related to autonomy and the NPHIs' relationship to the ministry of health. For example, some countries have chosen to maintain significant institutional ties to the ministry of health, while others do not directly require such direct institutional linkages.18,19 In Mozambique, the NPHI is under the direct tutelage of the ministry of health, and the minister maintains the authority to approve and authorize INS rules, annual reports, and activity plans.18,19 On the other hand, Liberia only requires the NPHI to maintain sectoral reporting accountability and sharing of scientific information reports with the ministry of health. 17
Because of the role NPHIs play in the overall strengthening of public health systems, description and designation of functions in the law help to establish public health roles for the NPHI that have a high priority. Therefore, the role of a legal instrument is largely to clarify and formally establish these roles, responsibilities, and relationships. Many NPHIs play a critical role in supporting key public health functions such as surveillance, outbreak preparedness and response, laboratory quality assurance, and public health research, among other functions. Given the variability in structure for NPHIs, the designation of specific functions can also serve as a blueprint for mapping which activities fall under the purview of the NPHI and what authorities reside elsewhere. This is particularly important for ensuring multisectoral and cross-sectoral collaboration in order to avoid duplication of efforts or any potential conflict of law. For example, as seen in Domain II, depending on the NPHI's role, surveillance and data-sharing functions may need to specify the collaborative relationships with sister institutes, government agencies, international organizations, universities, nongovernmental organizations, and professional societies. Other countries may use the designated functions to specify special authorities, such as authorizing the NPHI to engage in emergency preparedness activities, to designate and clarify what specific responsibilities rest with the NPHI for emergency operations. In particular, as countries develop new or enhance existing NPHI structures, the NPHI legal framework can serve as a valuable tool for addressing potential conflict of authorities that could be faced as new entities are developed and expanded.
Lastly, strong NPHI authorities can be used to help catalyze country activities toward achieving greater IHR compliance and can be used to ensure an increased coordination and cooperation both nationally and internationally toward prevention and control of disease. 11 Given the role of law in the overall capacity development process, including as measured by the JEE, countries may consider review of NPHI legal authorities to determine if gaps exist and whether addressing legal gaps will demonstrate capacity development progress as measured through the JEE.3,5 Moreover, the JEE highlights that, even if national legal systems do not require revised legislation to implement health system changes, revisions may still be a “more efficient, effective or beneficial manner” for implementation of health system interventions. 3
Conclusion
A strong legislative and regulatory framework can assist countries in building support for further public health capacity development, including establishment of sustainable norms to support IHR core capacities. 24 The JEE's national legislation, policy, and financing capacity area specifically underscores the role of law and policy by calling on nations to support and enable IHR implementation with a legal framework. 2 Given the increased effort by countries to meet these core capacities, the legal framework and menu of considerations for NPHIs provides a standardized tool to review existing authorities. As additional countries strive to develop new NPHIs or strengthen existing ones, the legal framework and menu of considerations provides stakeholders with a resource to enhance activities to clarify, establish, or enhance the legal foundation for the NPHI. 12 The legal framework and menu of considerations can provide stakeholders with a structured approach to conducting legal mapping of existing laws to identify where additional laws could help strengthen the public health infrastructure and support the continuity of the NPHI structure over time. 12 Given the variability in legal approaches used to establish and enable NPHIs, the legal framework and menu of considerations provides a roadmap to review and identify areas of opportunity to strengthen NPHI laws, while also providing flexibility for country-specific determinations.
Footnotes
Acknowledgments
The authors would like to acknowledge the collaboration, support, and contributions provided by ministries of health and other key partners from the Africa Centres for Disease Control and Prevention, Emory University School of Law, Guinea Bissau National Institute of Public Health, the International Association of National Public Health Institutes, Mozambique Instituto Nacional de Saude, National Public Health Institute of Liberia, Nigeria Centre for Disease Control, Public Health England, South Africa National Institute of Communicable Diseases, and the US Centers for Disease Control and Prevention on the development of the NPHI framework and subsequent legal framework tools.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.